A six-month-old boy presented with a nonhealing diaper rash. His parents first noticed the rash in the inguinal folds two months earlier. The rash persisted despite diligent treatment with barrier creams and antifungal ointment. The patient developed a fever and increased fussiness, although he continued to maintain adequate oral intake.
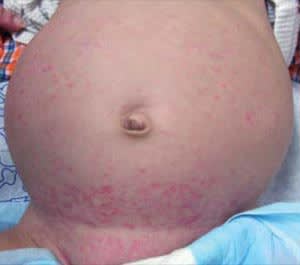
The physical examination revealed red, seborrhea-like eruptions on the diaper area and lower abdomen (see accompanying figure), as well as a scaling dermatitis of the scalp, axilla, and postauricular area. Abdominal distension with marked hepatosplenomegaly and bilateral inguinal lymphadenopathy was noted.
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Candidiasis.
B. Congenital syphilis.
C. Langerhans cell histiocytosis.
D. Perianal streptococcal infection.
E. Seborrheic dermatitis.
Discussion
The answer is C: Langerhans cell histiocytosis. Langerhans cell histiocytosis is a group of idiopathic disorders characterized by the proliferation of histiocytes, which consist of specialized dendritic cells, monocytes, and eosinophils.1 The three classic clinical presentations are eosinophilic granuloma (solitary lytic lesion of bone), Hand-Schüller-Christian disease (triad of lytic skull lesions, diabetes insipidus, and exophthalmos), and Letterer-Siwe disease (purpuric rash and systemic disease involving the lungs, liver, and bone marrow).
The diagnosis is based on a biopsy of the lesion. The presence of CD1a and S-100 surface markers, and characteristic racquet-shaped bodies in the cytoplasm (Birbeck granules) is confirmatory.2 Prognosis for patients with single-system disease is generally excellent, with treatment consisting of observation or organ-specific interventions. Multisystem disease is often treated with combination chemotherapy, with a five-year survival rate of up to 94.4 percent.3 All patients should receive long-term follow-up because the clinical course is variable and sequelae are common.
Candidiasis and irritant diaper dermatitis account for most diaper rashes. Candidiasis leads to beefy red erythema on the buttocks, lower abdomen, and thighs with pinpoint pustulovesicular satellite lesions involving the intertriginous areas. Candidal dermatitis is associated with antecedent antibiotic use, oral thrush, and maternal candidal nipple infection. Candidiasis infection should be suspected if diaper dermatitis persists for more than three days.4 A potassium hydroxide preparation showing budding yeast and pseudohyphae confirms the diagnosis.
Although congenital syphilis may have a similar clinical presentation to Langerhans cell histiocytosis, syphilis typically appears as a maculopapular rash of the groin area with associated involvement of the palms and soles. With a congenital infection, the rash may be vesicular with formation of bullae that subsequently desquamate. Additional signs of early congenital syphilis include snuff les, jaundice, hemolytic anemia, osteochondritis, and failure to thrive. Signs of late disease include Hutchinson teeth, saddle nose, saber shins, hearing impairment, hydrocephalus, and mental retardation.
Perianal streptococcal infection appears as a bright red, sharply demarcated rash that is associated with perianal itching, rectal pain, and blood-streaked stools. The condition may be mistaken for irritant or candidal diaper dermatitis, but the rash will not improve if treated as such. Perianal streptococcal infection is caused by group A beta-hemolytic streptococci and usually affects children between six months and 10 years of age. The disease readily responds to antibiotics; however, relapses may occur, necessitating a repeat antibiotic regimen.5
Seborrheic dermatitis appears as well-circumscribed, greasy scaling over red, inflamed skin. The condition should be strongly suspected if the rash involves the scalp, eyebrows, ears, and axilla. Seborrheic dermatitis is benign and usually resolves by six months of age. Infants presenting with generalized seborrheic dermatitis, diarrhea, and failure to thrive should be evaluated for complement C5 immunodeficiency.6
Summary Table
| Condition | Characteristics |
|---|---|
| Candidiasis | Beefy red erythema on the buttocks, lower abdomen, and thighs; pinpoint pustulovesicular satellite lesions involving the intertriginous areas |
| Congenital syphilis | Maculopapular rash in the groin area with associated involvement of the palms and soles; associated with hepatosplenomegaly and anemia |
| Langerhans cell histiocytosis | Severe and chronic; hemorrhagic, seborrhea-like eruptions; multisystem disease associated with hepatosplenomegaly; skin biopsy positive for S-100 and CD1a surface markers |
| Perianal streptococcal infection | Bright red, sharply demarcated rash associated with perianal itching, rectal pain, and blood-streaked stools |
| Seborrheic dermatitis | Well-circumscribed, greasy scaling over red, inflamed skin; associated with dermatitis of the scalp, eyebrows, ears, and axilla |

