
Am Fam Physician. 2009;80(12):1483-1484
Author disclosure: Nothing to disclose.
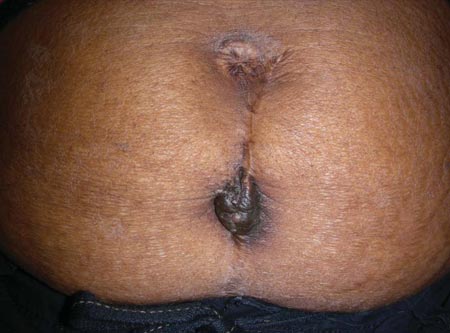
A 24-year-old woman presented with a tender mass in the midline of her lower abdomen that had been slowly enlarging for one year. The lesion became more painful and bled during menses. She had had two cesarean deliveries, but no other notable medical or surgical history. Review of systems and medication history was unremarkable.
Physical examination revealed a midline vertical scar with a 5.5-cm, dark brown, firm, fixed nodule (see accompanying figure). On palpation, the nodule appeared to be firmly adhered to deeper structures.
Question
Discussion
The answer is A: cutaneous endometrioma. Endometriosis is defined as endometrial tissue located outside of the uterine cavity. When this tissue takes the form of a tumor, it is known as an endometrioma.1,2 Computed tomography of the patient's abdomen and pelvis showed a 2.5-cm mass within the subcutaneous fat, without involvement of the peritoneal cavity or bowel.
A cutaneous endometrioma typically appears as an intermittently painful, tender, enlarging, deep red to violaceous, multilobulated, cystic mass. The pain usually occurs during menses.3,4 The lesions are located in surgical scars after procedures such as hysterectomy,5 cesarean delivery,5–8 amniocentesis, episiotomy, and tubal ligation.2–4,9
A biopsy of the lesion confirms the diagnosis. The histology consists of poorly circumscribed, nodular collections of endometrial glands in various phases of development surrounded by stroma and inflammation in the dermal and subcutaneous layers.3,4,6 Occasionally, these tumors also involve the fascia.
With the increasing number of hysterectomies and cesarean deliveries, the incidence of endometriomas is likely to increase.9 Endometriomas may present as early as three months after surgery and as late as 10 years after surgery, with the median time being two to three years postsurgery.3–5 Wide local excision is the preferred treatment.5 Medical therapies such as oral contraceptives, stanozolol (no longer available in the United States), or gonadotropin-releasing hormone analogues may lead to temporary benefits, but are associated with a high recurrence rate.7,10
Cutaneous sarcoidosis may be part of a systemic granulomatous disease that usually affects middle-aged black women. The condition has a range of cutaneous presentations, including patches, plaques, and nodules. However, the lesions typically are not painful and do not bleed. The most common presentation is a reddish-brown nodule in a previous scar.
Direct hernias often do not cause overlying cutaneous change. Typically, they are diagnosed by palpation because they are more prominent with increased abdominal pressure and may be reduced with external pressure. Patients should be referred for elective surgical repair.
Keloids are common, benign neoplasms consisting of increased fibroblasts and collagen that may occur after a trauma or surgical procedure. They typically present in the months following a trauma or procedure, as the wound heals. Although keloids may be painful, the pain usually is not associated with menses, and the lesions do not bleed.
A suture granuloma essentially is a foreign body reaction to suture remaining in the tissue after surgery. It is generally a tender, erythematous nodule that occurs several days to weeks after surgery. A suture granuloma is treated with intralesional steroids or excision.
| Condition | Characteristics |
|---|---|
| Cutaneous endometrioma | Intermittent pain, typically during menses; tender, enlarging, deep red to violaceous, multilobulated, cystic mass |
| Cutaneous sarcoidosis | A range of cutaneous presentations, including patches, plaques, and nodules; most commonly appears as a reddish-brown nodule in a previous scar |
| Direct hernia | Usually no overlying cutaneous change; typically has greater prominence with increased abdominal pressure and is diagnosed by palpation |
| Keloid | Usually appears in the months following a trauma or surgery, as the site heals; occasionally tender or painful |
| Suture granuloma | Tender, erythematous nodule occurring several days to weeks after surgery |
