Vocal cord dysfunction involves inappropriate vocal cord motion that produces partial airway obstruction. Patients may present with respiratory distress that is often mistakenly diagnosed as asthma. Exercise, psychological conditions, airborne irritants, rhinosinusitis, gastroesophageal reflux disease, or use of certain medications may trigger vocal cord dysfunction. The differential diagnosis includes asthma, angioedema, vocal cord tumors, and vocal cord paralysis. Pulmonary function testing with a flow-volume loop and flexible laryngoscopy are valuable diagnostic tests for confirming vocal cord dysfunction. Treatment of acute episodes includes reassurance, breathing instruction, and use of a helium and oxygen mixture (heliox). Long-term management strategies include treatment for symptom triggers and speech therapy.
Vocal cord dysfunction is a syndrome in which inappropriate vocal cord motion produces partial airway obstruction, leading to subjective respiratory distress. When a person breathes normally, the vocal cords move away from the midline during inspiration and only slightly toward the midline during expiration.1 However, in patients with vocal cord dysfunction, the vocal cords move toward the midline during inspiration or expiration, which creates varying degrees of obstruction.2 Vocal cord dysfunction has numerous labels in the literature, including paradoxical vocal cord dysfunction,3 paradoxical vocal fold motion,4 and factitious asthma.5
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Exercise-induced vocal cord dysfunction should be strongly considered in patients diagnosed with exercise-induced asthma who respond poorly to usual treatment. | C | 7, 8 |
| Pulmonary function testing with a flow-volume loop is useful in confirming a diagnosis of vocal cord dysfunction. | C | 2, 22–25 |
| Reassurance and breathing instruction may resolve an acute episode of vocal cord dysfunction. | C | 27 |
| Pretreatment with inhaled ipratropium (Atrovent) may be a helpful adjunct in patients with exercise-induced vocal cord dysfunction. | C | 8 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Clinical Presentation
Vocal cord dysfunction occurs more often in women than in men, and is common in persons 20 to 40 years of age.2,6,7 However, studies have identified vocal cord dysfunction in adolescents and in children as young as eight years.8
Patients with vocal cord dysfunction typically present with recurrent episodes of subjective respiratory distress that are associated with inspiratory stridor, cough, choking sensations, and throat tightness.3 The presence of wheezing can indicate an asthma exacerbation, but is commonly a mistaken description of the stridor characteristic of vocal cord dysfunction.9,10 In one study, 59 percent of patients with vocal cord dysfunction had been previously diagnosed with asthma.8 Most patients with vocal cord dysfunction have intermittent and relatively mild symptoms, although some patients may have prolonged and severe symptoms.
Laryngospasm, a subtype of vocal cord dysfunction, is a brief involuntary spasm of the vocal cords that often produces aphonia and acute respiratory distress. Laryngospasm is a common complication of anesthesia.11 Another variation of vocal cord dysfunction is spasmodic dysphonia, which causes hoarseness and strained vocalization when the abnormal vocal cord motion occurs during speech.12
Differential Diagnoses
The primary diagnosis to consider in patients with respiratory distress or wheezing is asthma. Vocal cord dysfunction is often misdiagnosed as asthma, and a considerable subset of patients with vocal cord dysfunction also have asthma, making the diagnosis more difficult.2,8 A careful patient history may help to differentiate between the two conditions. Unlike asthma, vocal cord dysfunction causes more difficulty with inspiration than expiration, and is commonly associated with a sensation of throat tightness or choking. However, further testing, including pulmonary function testing and laryngoscopy, is usually required to make the diagnosis.13 Additional conditions in the differential diagnosis of vocal cord dysfunction are listed in Table 1.
Table 1. Differential Diagnosis of Vocal Cord Dysfunction
| Anaphylaxis |
| Angioedema |
| Asthma |
| Epiglottitis |
| Hypoparathyroidism |
| Laryngomalacia (in adults) |
| Laryngotracheobronchitis (croup) |
| Presence of foreign body |
| Tracheal stenosis |
| Vocal cord paralysis |
| Vocal cord tumors or polyps |
Precipitating Factors
Vocal cord dysfunction is associated with a variety of precipitating factors, but no clear unifying pathophysiology has been identified.
EXERCISE
Exercise is a common cause of vocal cord dysfunction. Exercise-induced vocal cord dysfunction is often misdiagnosed as exercise-induced asthma.8 It should be strongly considered in patients with dyspnea on exertion who have been diagnosed with exercise-induced asthma, particularly if they respond poorly to usual treatment with bronchodilators.7
PSYCHOLOGICAL CONDITIONS
Studies have reported associations between vocal cord dysfunction and multiple psychological conditions, including posttraumatic stress disorder, anxiety, depression, and panic attack.14 Anxiety disorders appear to be particularly common in adolescent patients with vocal cord dysfunction.15 However, associated depression and anxiety may also be consequences of persistent respiratory symptoms, rather than causes.16
IRRITANTS
Exposure to environmental and occupational irritants has been found to precipitate respiratory symptoms consistent with vocal cord dysfunction. Common airborne irritants associated with vocal cord dysfunction include ammonia, dust, smoke, soldering fumes, and cleaning chemicals. Studies have shown a clear temporal relationship between exposure and onset of symptoms.17
RHINOSINUSITIS
Postnasal drip associated with rhinosinusitis has been linked to airway hyperresponsiveness.18 A high prevalence of rhinosinusitis in patients with vocal cord dysfunction and case reports of resolution of vocal cord dysfunction symptoms with treatment suggest that rhinosinusitis may play a role in some patients.17
GASTROESOPHOGEAL REFLUX DISEASE
Gastroesophageal reflux disease (GERD) has been implicated in triggering vocal cord dysfunction.19 In some studies, a high prevalence of GERD was identified in patients with vocal cord dysfunction20; however, treatment of GERD was only effective in decreasing vocal cord dysfunction in some patients.
MEDICATION USE
Neuroleptic drugs, specifically phenothiazines, may cause transient vocal cord dysfunction. This appears to be a focal dystonic reaction and is associated with extra-pyramidal signs, such as torticollis.21
Diagnostic Approaches
The most valuable diagnostic tests for vocal cord dysfunction are pulmonary function testing with a flow-volume loop and flexible laryngoscopy. Other testing, such as measurement of arterial blood gases, may be useful in ruling out other possible diagnoses.
PULMONARY FUNCTION TESTING
Pulmonary function testing with a flow-volume loop is the most commonly used diagnostic test to confirm vocal cord dysfunction. In the flow-volume loop, it is typical for the expiratory loop to be normal and the inspiratory loop to be flattened, which is consistent with an extrathoracic upper airway obstruction (Figure 1). This pattern is characteristic of patients when they are symptomatic.22 Even when asymptomatic, some patients with vocal cord dysfunction will demonstrate inspiratory loop flattening.2 Exercise flow-volume loops, performed in conjunction with exercise testing, may be useful in identifying patients with exercise-induced vocal cord dysfunction.23
Figure 1.
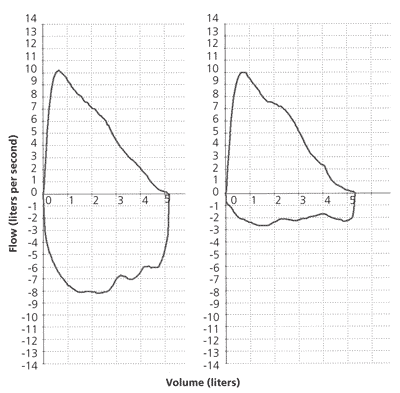
Flow-volume loop. (Left) Normal expiratory and inspiratory loop. (Right) Normal expiratory loop with flattening of the inspiratory loop, consistent with vocal cord dysfunction.
Pulmonary function testing is particularly useful in differentiating vocal cord dysfunction from asthma because bronchospasm produces an impaired expiratory loop that is different from that seen in vocal cord dysfunction.24 In cases with an unclear etiology, or if concurrent asthma and vocal cord dysfunction are suspected, methacholine challenge testing may help to clarify the diagnosis.25
FLEXIBLE LARYNGOSCOPY
Flexible laryngoscopy is considered the diagnostic standard for vocal cord dysfunction. Direct observation of abnormal vocal cord movement toward the midline during inspiration or expiration confirms the diagnosis. Most patients with symptomatic vocal cord dysfunction will demonstrate the abnormal movement, and more than one half of patients who are asymptomatic will be diagnosed.2,26 Stimulating asymptomatic patients with panting, deep breathing, phonating, or exercising may increase the sensitivity of the test.2,6
Treatment
SHORT-TERM
Patients with vocal cord dysfunction may present with acute respiratory distress in the emergency department or outpatient setting.10 After other causes have been ruled out, vocal cord dysfunction can be treated with a variety of interventions (Table 2).
Reassurance and breathing instruction may resolve an acute episode of vocal cord dysfunction. Published case reports suggest that having the patient breathe rapidly and shallowly (i.e., pant) can result in immediate resolution of symptoms.27 Additional breathing maneuvers include diaphragmatic breathing, breathing through the nose, breathing through a straw, pursed-lip breathing, and exhaling with a hissing sound.
Administering a helium and oxygen mixture (heliox) reduces airway resistance and may result in rapid improvement in patients with acute vocal cord dysfunction. A trial of heliox may be appropriate because of its relatively low cost and minimal adverse effects, although this has been reported in only one case series.28,29
Table 2. Short- and Long-term Management of Vocal Cord Dysfunction
| Short-term |
| Reassure patient |
| Instruct patient in breathing behaviors, including panting, diaphragmatic breathing, breathing through the nose or a straw, pursed-lip breathing, and exhaling with a hissing sound |
| Consider a trial of helium and oxygen (heliox) in patients with persistent or severe vocal cord dysfunction |
| Long-term |
| Avoid known triggers, such as smoke, airborne irritants, or certain medications |
| Treat underlying conditions, including anxiety, depression, gastroesophageal reflux disease, and rhinosinusitis |
| Consider a trial of inhaled ipratropium (Atrovent) in patients with exercise-induced symptoms |
| Referral for speech therapy is indicated in patients with unresolved symptoms |
| Long-term tracheostomy may be appropriate in severe, resistant cases |
LONG-TERM
Management of chronic vocal cord dysfunction (Table 2) begins with treatment or elimination of precipitating factors, including GERD, rhinosinusitis, psychological conditions, airborne irritants, and certain medications.
Speech therapy is the mainstay of long-term management. Therapy that incorporates a variety of techniques, including relaxed-throat breathing, has been shown to improve symptoms of vocal cord dysfunction and reduce recurrences.8,30
Anticholinergics may be a helpful adjunct in patients with exercise-induced vocal cord dysfunction. In a series of six patients receiving pretreatment with inhaled ipratropium (Atrovent), all patients reported improvement of symptoms.8 In severe, resistant cases of vocal cord dysfunction, treatment with long-term tracheostomy has been reported.31

