A 13-year-old girl presented with a pruritic rash on her foot. The rash appeared between her toes several days earlier and had spread over the dorsum of her foot (Figures 1 and 2). The rash was erythematous, serpiginous, and raised with clear, fluid-filled vesicles measuring 2 mm. The patient had no history of similar episodes. She did not have fever, contact with sick persons, or recent travel. None of her family members had symptoms. She had recently moved to rural northeast Florida.
Figure 1.
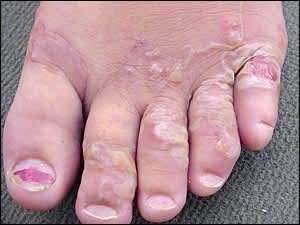
Figure 2.
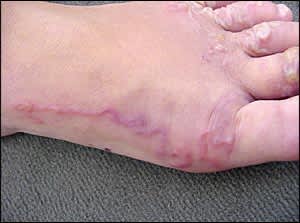
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Cutaneous larva migrans.
B. Erythema migrans of Lyme borreliosis.
C. Impetigo.
D. Scabies.
E. Tinea pedis.
Discussion
The answer is A: cutaneous larva migrans. Cutaneous larva migrans (also called creeping eruptions or sand-worm disease) typically occurs after exposure to moist, sandy areas that have been contaminated with dog or cat feces. Patients present with an intensely pruritic, erythematous rash with a serpiginous pattern. The rash may be accompanied by small vesicles. The most commonly affected areas are those directly exposed to the contaminated soil, such as hands, feet, and buttocks. The lesion tract may advance as much as 1 to 2 cm per day.1
Secondary bacterial infection often occurs because of intense pruritus and poor hand hygiene. Systemic signs may include peripheral eosinophilia.1
Although many types of hookworm can cause cutaneous larva migrans, Ancylostoma braziliense is the most common cause in the southern United States, Central and South America, and the Caribbean.2 Larvae enter the skin through fissures, sweat glands, or follicles, causing a tingling sensation.3 The larva may begin creeping immediately or may be dormant for weeks to months.2 Because the larvae cannot penetrate the dermis, the infestation is self-limited.
Treatment consists of anthelmintics, such as thiabendazole, albendazole (Albenza), mebendazole, and ivermectin (Stromectol).1 Typically, the pruritus resolves 24 to 48 hours after treatment, with resolution of the lesion after one week.2
Erythema migrans is classically described as a bull'seye lesion with expanding erythema and central clearing, although this presentation is rarely noted.4 The nonpruritic lesion usually appears on the axilla, on the inguinal region, behind the knees, or at the belt line.4
Impetigo begins as small vesicles that develop into pustules. A serpiginous pattern is not typical. The pustules rupture with the characteristic golden honey–colored exudate.5 Impetigo is caused by staphylococcal and streptococcal infections.
Scabies appear as tiny papules and vesicles with black dots, which are the mites themselves.6 The pleomorphic lesions are intensely pruritic and may consist of linear, curved burrows that are pale pink and raised.6 Usually, multiple family members have symptoms.
Tinea pedis typically leads to fissuring, maceration, and dry scaling interdigitally or in a moccasin-like pattern on the soles and edges of the foot.7 Tinea pedis may appear as vesicles or pustules that generally occur on the soles.7 The condition is caused by a fungal infection.
Summary Table
| Condition | Characteristics |
|---|---|
| Cutaneous larva migrans | History of exposure to sand contaminated with dog or cat feces; pruritic rash commonly appears on hands, feet, or buttocks; erythematous rash with serpiginous pattern |
| Erythema migrans of Lyme borreliosis | Bull's-eye lesion; nonpruritic rash usually appears on the axilla, in the inguinal region, behind the knees, or at the belt line; history of tick bites |
| Impetigo | Nonpruritic rash with vesicles and pustules; golden honey–colored exudates; staphylococcal or streptococcal infection |
| Scabies | Household contacts are usually infected; tiny papules and vesicles with black dots in interdigital spaces; burrows may be present; pruritic |
| Tinea pedis | Fissuring, maceration, and dry scaling interdigitally or in a moccasin-like pattern; fungal infection; pruritic |

