Am Fam Physician. 2010;81(6):745-748
Patient information: See related handout on vitamin D in children, written by the authors of this article.
Author disclosure: Nothing to disclose.
Vitamin D deficiency in children can have adverse health consequences, such as growth failure and rickets. In 2008, the American Academy of Pediatrics increased its recommended daily intake of vitamin D in infants, children, and adolescents to 400 IU. Infants who are breastfed and children and adolescents who consume less than 1 L of vitamin D–fortified milk per day will likely need supplementation to reach 400 IU of vitamin D per day. This recommendation is based on expert opinion and recent clinical trials measuring biomarkers of vitamin D status. It is also based on the precedent of preventing and treating rickets with 400 IU of vitamin D. In addition to dietary sources, exposure to ultraviolet B sunlight provides children and adults with additional vitamin D. Although the American Academy of Pediatrics recommends keeping infants out of direct sunlight, decreased sunlight exposure may increase children's risk of vitamin D deficiency. No randomized controlled trials assessing patient-oriented outcomes have been performed on universal vitamin D supplementation. However, vitamin D may reduce the risk of certain infections and chronic diseases. Physicians should help parents choose the appropriate vitamin D supplement for their child.
Vitamin D deficiency in children has been linked to adverse effects, such as growth failure and rickets. Although vitamin D is available in several foods and drinks, recent estimates suggest the prevalence of vitamin D deficiency among infants, children, and adolescents is between 12 and 24 percent.1,2 Infants who are breastfed appear to be at higher risk of vitamin D deficiency. Family physicians should understand current recommendations for vitamin D supplementation, and be prepared to educate parents about breastfeeding, sun precautions, and nutrition throughout childhood and adolescence.
Vitamin D in Health and Disease
Vitamin D plays several important roles in the metabolism and absorption of other minerals in the body. Vitamin D is essential for facilitating calcium metabolism and bone mineralization; is beneficial for phosphate and magnesium metabolism; and stimulates protein expression in the intestinal wall to promote calcium absorption. Low levels of vitamin D lead to the release of parathyroid hormone, which causes calcium mobilization from the bone. Over time, excessive bone resorption can lead to rickets.
Adequate levels of vitamin D may also help reduce the risk of autoimmune conditions,3,4 infection,5 and type 2 diabetes.6 Evidence from observational studies supports the role of vitamin D supplementation in reducing the risk of type 1 diabetes in infants and children.7 Although observational studies suggest that vitamin D may be protective against some cancers,8 a randomized controlled trial of calcium and vitamin D supplementation in 36,282 women did not find a protective effect against breast cancer.9
Guidelines for Vitamin D Intake
In 2003, the American Academy of Pediatrics (AAP) published a guideline recommending that all children older than two months receive 200 IU of supplemental vitamin D daily.10 This expert consensus statement was supported by studies of breastfed infants in the United States, Norway, and China and suggested that infants who ingest 100 or 200 IU of supplemental vitamin D daily were less likely to develop rickets.11 Since then, there have been concerns that these dosages may be insufficient. These concerns are supported by studies showing that vitamin D deficiency can occur early in life12; that serum 25-hydroxyvitamin D concentrations tend to be lower in breastfed infants13; and that 400 IU of vitamin D supplementation in these infants maintains higher concentrations of 25-hydroxyvitamin D.14 In addition, studies have shown that adolescents consume insufficient levels of dietary vitamin D 15,16 and that supplementation increases 25-hydroxyvitamin D levels and bone mineral density.17
| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
| Infants ingesting less than 1 L (33.8 fl oz) of formula per day, as well as all breastfed or partially breastfed infants, should receive 400 IU of supplemental vitamin D daily. | C | 13, 19, 20 | Based on disease-oriented evidence and expert opinion |
| Children and adolescents consuming less than 1 L of vitamin D–fortified milk per day should receive 400 IU of supplemental vitamin D daily. | C | 21, 22 | Based on disease-oriented evidence and case series |
| Limiting sunlight exposure may predispose children to vitamin D deficiency. | C | 23, 25–27 | Based on disease-oriented evidence and expert opinion |
| The best available biomarker of vitamin D status is serum 25-hydroxyvitamin D levels. | C | 28, 29 | Based on consensus and disease-oriented evidence |
| Children at increased risk of vitamin D deficiency may require higher dosages of supplemental vitamin D. | C | 32–34 | Based on disease-oriented evidence and expert opinion |
Consequently, the AAP issued an updated recommendation in 2008 that all infants, children, and adolescents receive a minimum of 400 IU of vitamin D daily through diet or supplements.18 Infants who are formula-fed exclusively will most likely have an adequate level of vitamin D. Infants who are breastfed or partially breastfed, as well as children and adolescents who consume less than 1 L (33.8 fl oz) of vitamin D–fortified milk per day, should receive 400 IU of supplemental vitamin D daily.13,19–22
Despite these recommendations, there are no studies showing that universal supplementation improves patient-oriented outcomes, such as the reversal of lethargy, irritability, and growth failure, attributed to vitamin D deficiency. Only indirect evidence supports the contention that 400 IU of supplemental vitamin D daily prevents and treats rickets.14 Prospective studies focusing on patient-oriented outcomes, rather than biomarkers, are needed before the actual clinical impact of supplemental vitamin D will be understood.
Vitamin D and Sunlight
In addition to dietary sources, children and adults obtain vitamin D through exposure to ultraviolet B sunlight. As little as 10 to 15 minutes of direct sunlight can generate 10,000 to 20,000 IU of vitamin D. Many factors influence vitamin D synthesis, such as skin pigmentation, latitude, and amount of skin exposed, making it difficult to assess how much vitamin D will be converted from sunlight exposure. Infants and children who have darker pigmentation require five to 10 times the length of sunlight exposure to reach the same levels of 25-hydroxyvitamin D when compared with children who have lighter pigmentation.23 However, the AAP recommends that infants younger than six months be kept out of direct sunlight.24 Although the goal of limiting sunlight exposure is to minimize the risk of skin cancer, it may also predispose children to vitamin D deficiency.25–27 Because the safe level of sunlight exposure needed for vitamin D conversion is unknown, increasing vitamin D supplementation is a reasonable alternative.
Complications of Vitamin D Deficiency
Risk factors for vitamin D deficiency are summarized in Table 1. Physicians should confirm suspicion of vitamin D deficiency by measuring levels of 25-hydroxyvitamin D, which is the best available biomarker for checking vitamin D status.28,29 Vitamin D deficiency in adults is defined as 25-hydroxyvitamin D levels of less than 20 ng per mL (50 nmol per L), although this varies among studies.30 There is no set level of 25-hydroxyvitamin D to confirm vitamin D deficiency in infants, children, and adolescents. Although no set level has been established for children and adolescents, recent studies have used less than 15 to 20 ng per mL (37.44 to 50 nmol per L) as a cutoff for vitamin D deficiency in these age groups.
| Anticonvulsant medication therapy |
| Chronic diseases associated with fat malabsorption |
| Darker skin pigmentation |
| Exclusive breastfeeding without vitamin D supplementation |
| Insufficient sunlight exposure |
| Low maternal vitamin D levels (risk factor for infants) |
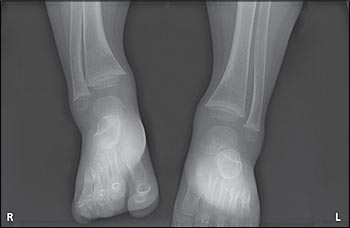
Patients with severe cases of rickets may present with growth failure, hypocalcemic seizures, decreased bone mass, and characteristic bone changes or fractures (Figure 1). Nonspecific symptoms, such as irritability, lethargy, and developmental delay, may be less obvious. In a case-control study of children hospitalized for acute illnesses, investigators found an increased rate of admissions for lower respiratory tract infections among those with rickets.31
Supplementation Options
Vitamin D3, known as cholecalciferol, is the preferred form of vitamin D for supplementation. Children with certain conditions, such as fat malabsorption, and those who require long-term use of seizure medications may need higher dosages of vitamin D because of increased risk of deficiency.32–34 Monitoring 25-hydroxyvitamin D levels every three months, and parathyroid hormone levels and bone-mineral status every six months, is recommended for these children.
Vitamin D deficiency during pregnancy may increase the risk of abnormal fetal growth and bone development, but further studies are needed before high-dose supplementation in pregnant women can be universally recommended.35
No evidence suggests that daily supplementation of 400 IU of vitamin D is toxic. Physicians should provide patients with detailed administration instructions to avoid accidental overdose. Vitamin D3 drops, which are preferable for infants, are available in formulations of 400, 1,000, and 2,000 IU per drop. Varying amounts of vitamin D3 are available within formulations of the same brand. Chewable and gummy vitamins for older children contain 200 or 400 IU of vitamin D, but may vary by formulation from the same manufacturer. Physicians may prefer to recommend one brand and formulation for each age group to ensure that patients reach a daily dosage of 400 IU (Tables 2 and 3).
| Brand | Vitamin D per serving (IU) | Serving size |
|---|---|---|
| Carlson Baby D Drops | 400 | 1 drop |
| Enfamil Poly-Vi-Sol Multivitamin Supplement Drops | 400 | 1 mL |
| Enfamil Tri-Vi-Sol Vitamins A, C & D with Iron | 400 | 1 mL |
| Sunlight Vitamins Just D infant vitamin drops | 400 | 1 mL |
| Twinlab Infant Care Multivitamin Drops with DHA | 400 | 1 mL |
| Brand | Vitamin D per serving (IU) | Serving size | |
|---|---|---|---|
| Centrum Kids Complete Multivitamins, chewable tablets | 400 | One tablet for children four years and older (1/2 tablet for children two and three years of age) | |
| Disney Gummies Children's Multivitamin | 200 | Two gummies for children two years and older | |
| Flintstones Children's Complete Multivitamin, chewable tablets | 400 | One tablet for children four years and older (1/2 tablet for children two and three years of age) | |
| Flintstones Gummies with Calcium & Vitamin D, multivitamin | 400 | Two gummies for children four years and older (one gummy for children two and three years of age) | |
| Li'l Critters Gummy Vites Kids Multivitamin | 240 | Two gummies for children two years and older | |
| Sundown Spider-man Complete Children's Gummies | 200 | Two gummies for children two years and older | |