An 82-year-old woman presented to the emergency department with right-sided leg pain and paresthesias that had lasted for five days. The patient had been bedridden for several years because of dementia.
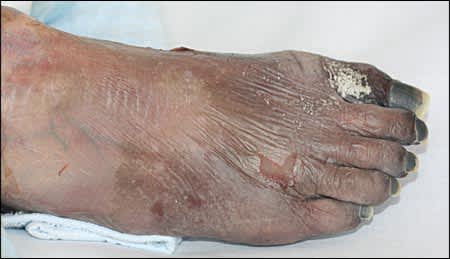
Examination revealed diffusely scattered cyanosis on the foot (see accompanying figure), ankle, and calf, but sparing the knee. Peripheral pulses, including popliteal, posterior tibial, and dorsal pedis, were absent on the affected side.
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Blue toe syndrome.
B. Buerger disease.
C. Diabetic gangrene.
D. Diffuse acute limb ischemia.
E. Postthrombotic syndrome.
Discussion
The answer is D: diffuse acute limb ischemia. Diffuse acute limb ischemia is caused by a sudden decrease in limb perfusion that threatens limb viability within two weeks of the acute event. The condition is called critical limb ischemia when symptoms last for more than two weeks.1
Skin examination typically shows a cool, pale extremity with delayed capillary refill. The level of occlusion is generally one joint above the line of demarcation between the normal and ischemic areas. The classic symptoms of large artery occlusion are described as the five Ps: pain, paleness, pallor, paresthesia, and paralysis. Irreversible damage occurs within six hours of ischemia. When arterial occlusion occurs in the setting of well-developed collateral circulation, the symptoms may be less remarkable (e.g., intolerance to ambulation, modest pain, paresthesia). Limb ischemia is more common in lower extremities than in upper extremities. Diagnosis can be made using arterial Doppler evaluation and angiography. Angiography is confirmatory and demonstrates the location and severity of the obstruction.2
Acute limb ischemia is usually caused by embolic events, and therefore warrants investigation for an embolic source. Most embolic events are of cardiac or large artery origin. Cardiac disorders that can cause embolism include atrial fibrillation, myocardial infarction, and ventricular aneurysm. Atherosclerosis, or aneurysm of the aorta and other large arteries, is another embolic source of embolism. Although less common, a venous thrombus may enter systemic circulation through a patent foramen ovale or other septal defect.2 Arterial thrombosis may occur in atheromatous, aneurysmal, or traumatized vessels.
Treatment of embolism includes prompt initiation of heparin to prevent propagation of the clot,1 followed by intra-arterial thrombolytic therapy with urokinase or surgical intervention (embolectomy or a bypass procedure). Nonviable tissue requires debridement, and amputation if necessary.3 Delayed amputation increases the risk of infection, myoglobinuria, acute renal failure, and hyperkalemia. After successful limb salvage, continuous anticoagulation with heparin followed by oral warfarin (Coumadin) is recommended to prevent recurrence.2
Blue toe syndrome is an acute embolic event at the digital artery that leads to sudden, painful cyanosis in the toe despite strong pedal pulse and a warm foot.4 This condition is analogous to transient ischemic attack in the central nervous system and leads to an impending ischemic event.
Buerger disease is inflammation of distal arteries and veins causing ischemic pain and ulceration. Pathology shows inflammation of vessels; however, atherosclerosis is typically absent. Risk factors include Asian descent and cigarette smoking.2
Diabetic gangrene manifests as a nonhealing ulcer, typically on the toe. It is caused by the combination of arterial atherosclerosis and peripheral nerve damage. Diabetic gangrene typically develops after long-standing diabetes mellitus with multiple foot infections.
Postthrombotic syndrome is a common complication of deep venous thrombosis. Typical features include pain, swelling, and heaviness; a stasis ulcer may develop.5
Summary Table
| Condition | Characteristics |
|---|---|
| Blue toe syndrome | Acrocyanosis with strong pedal pulse and warm foot |
| Buerger disease | Small and medium vessel vasculitis causing ischemic pain and ulceration; more common in smokers and persons of Asian descent |
| Diabetic gangrene | Nonhealing ulcer, typically in persons with long-standing history of diabetes mellitus and multiple foot infections |
| Diffuse acute limb ischemia | Progressive pain, paleness, pallor, paresthesia, and paralysis |
| Postthrombotic syndrome | Pain, swelling, and heaviness; stasis ulcer may develop |

