A 53-year-old man presented to the emergency department with diplopia, left-sided ptosis, unsteady gait, headache, and left eye pain that had persisted for four days. He had a history of poorly controlled hypertension and type 2 diabetes mellitus, and had undergone surgery for right optic tumor resection 30 years earlier.
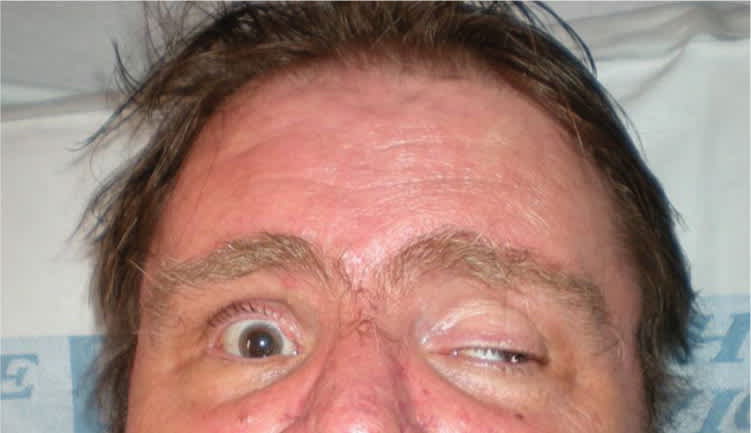
The patient's blood pressure was 148/72 mm Hg at presentation. Physical examination revealed partial ptosis and inferolateral deviation of the left eye (see accompanying figure), and the patient was unable to move his eye past midline. Extraocular muscles of the right eye were intact, and bilateral vision was 20/20. The left pupil was 3 mm and reactive to light. The remainder of the neurologic examination, including cerebellar and Romberg testing, was unremarkable.
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Aneurysm of the posterior communicating artery.
B. Diabetic third nerve palsy.
C. Myasthenia gravis.
D. Orbital myositis.
E. Vertebrobasilar occlusion.
Discussion
The answer is B: diabetic third nerve palsy. The third cranial nerve innervates the levator palpebrae and four extraocular muscles. Third nerve palsy typically manifests as diplopia and ptosis. The pupil may be unaffected.1 Diabetic third nerve palsy is a disease caused by microvascular infarction of the blood supply to the oculomotor cranial nerve. The infarction initially occurs in the smallest vessels that are supplying the interior portion of the third nerve. This results in a pupil-sparing presentation because the superficial parasympathetic nerve fibers are unaffected.
Microvascular ischemia from diabetes is the most common etiology of third nerve palsy. The pupil-sparing presentation in an older patient with other vascular risk factors, such as hypertension or diabetes, is diagnostic. Magnetic resonance imaging should be performed if the diagnosis is unclear or if symptoms persist.2 Treatment is aimed at the underlying etiology and includes anti-platelet therapy and control of diabetes and blood pressure. Most patients recover within weeks to months, although deficits that are present at six months are usually permanent.
An aneurysm of the posterior communicating artery can compress the oculomotor nerve, leading to third nerve palsy. The parasympathetic fibers to the pupil travel outside of the third nerve; therefore, compression by this type of aneurysm typically impairs pupil constriction.3
Myasthenia gravis is characterized by autoimmune destruction of postsynaptic acetylcholine receptors. The condition manifests as weakness and fatigue of skeletal muscles; smaller muscles are affected first. Myasthenia can also present as a pupil-sparing third nerve palsy with ptosis. Application of ice for two minutes will typically relieve ptosis, which differentiates it from ischemic palsies.4
Orbital myositis is the inflammation of at least one extraocular muscle. Patients present with acute orbital pain and diplopia, and often have elements of conjunctivitis. The pupil is spared. Orbital myositis is diagnosed by neuroimaging, and can be ruled out by the absence of focal or diffuse extraocular lesions. The condition is treated with corticosteroids.5
Vertebrobasilar occlusion, also known as posterior circulation ischemia, can cause ischemia in various locations. Stenosis or occlusion typically occurs in the aortic arch, neck, or intracranial arteries. The oculomotor nucleus, located in the midbrain, can be affected if the blood supply to the midbrain is decreased.6 Patients may also present with nausea, vertigo, and other cranial nerve or neurologic deficits. Because the levator palpebrae are innervated by a single central subnucleus, a nuclear lesion would cause bilateral ptosis.
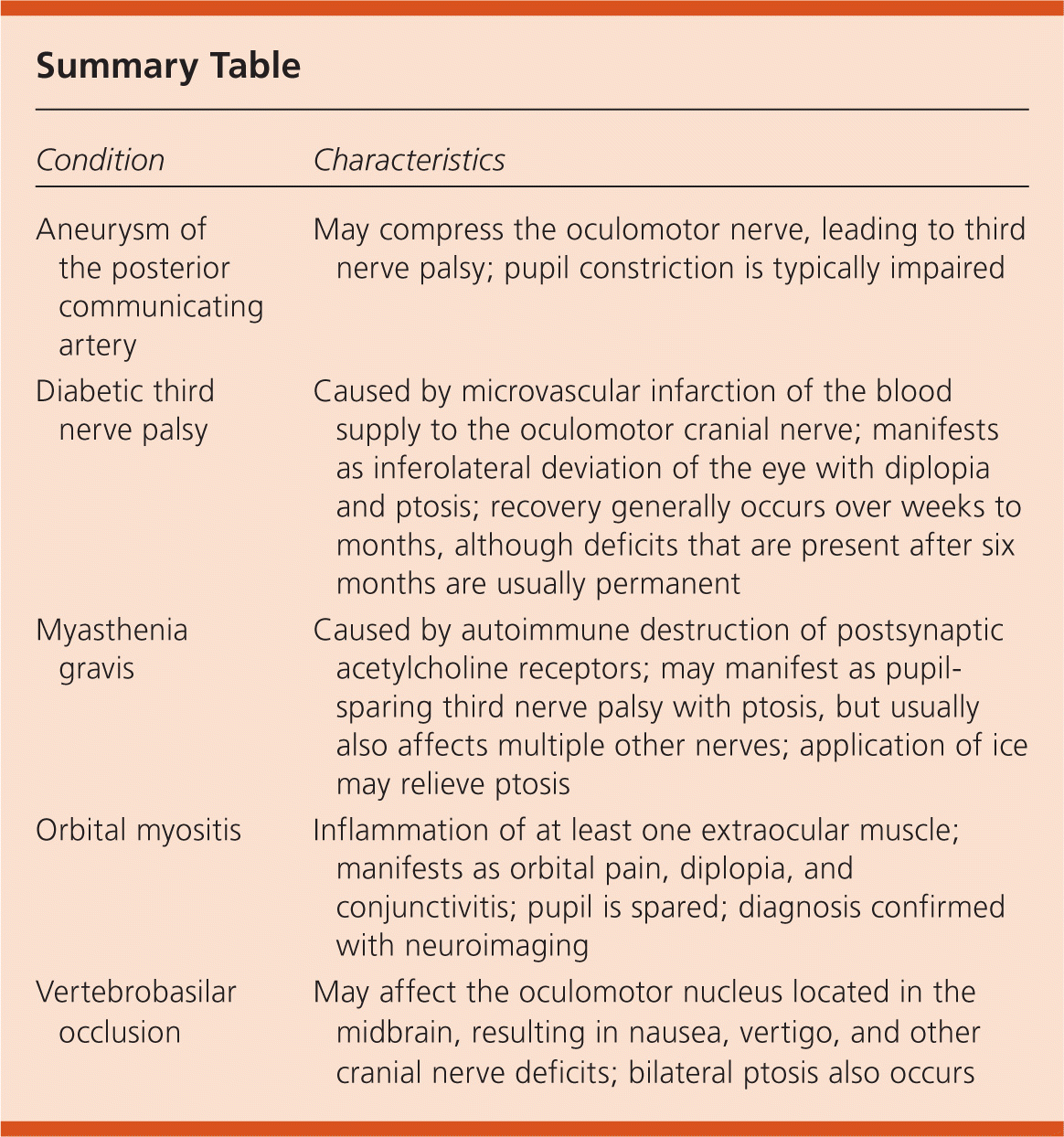
Summary Table
| Condition | Characteristics |
|---|---|
| Aneurysm of the posterior communicating artery | May compress the oculomotor nerve, leading to third nerve palsy; pupil constriction is typically impaired |
| Diabetic third nerve palsy | Caused by microvascular infarction of the blood supply to the oculomotor cranial nerve; manifests as inferolateral deviation of the eye with diplopia and ptosis; recovery generally occurs over weeks to months, although deficits that are present after six months are usually permanent |
| Myasthenia gravis | Caused by autoimmune destruction of postsynaptic acetylcholine receptors; may manifest as pupil-sparing third nerve palsy with ptosis, but usually also affects multiple other nerves; application of ice may relieve ptosis |
| Orbital myositis | Inflammation of at least one extraocular muscle; manifests as orbital pain, diplopia, and conjunctivitis; pupil is spared; diagnosis confirmed with neuroimaging |
| Vertebrobasilar occlusion | May affect the oculomotor nucleus located in the midbrain, resulting in nausea, vertigo, and other cranial nerve deficits; bilateral ptosis also occurs |

