Primary care physicians often prescribe contraceptives to women of reproductive age with comorbidities. Novel delivery systems (e.g., contraceptive patch, contraceptive ring, single-rod implantable device) may change traditional risk and benefit profiles in women with comorbidities. Effective contraceptive counseling requires an understanding of a woman's preferences and medical history, as well as the risks, benefits, adverse effects, and contraindications of each method. Noncontraceptive benefits of combined hormonal contraceptives, such as oral contraceptive pills, include regulated menses, decreased dysmenorrhea, and diminished premenstrual dysphoric disorder. Oral contraceptive pills may be used safely in women with a range of medical conditions, including well-controlled hypertension, uncomplicated diabetes mellitus, depression, and uncomplicated valvular heart disease. However, women older than 35 years who smoke should avoid oral contraceptive pills. Contraceptives containing estrogen, which can increase thrombotic risk, should be avoided in women with a history of venous thromboembolism, stroke, cardiovascular disease, or peripheral vascular disease. Progestin-only contraceptives are recommended for women with contraindications to estrogen. Depo-Provera, a long-acting injectable contraceptive, may be preferred in women with sickle cell disease because it reduces the frequency of painful crises. Because of the interaction between antiepileptics and oral contraceptive pills, Depo-Provera may also be considered in women with epilepsy. Implanon, the single-rod implantable contraceptive device, may reduce symptoms of dysmenorrhea. Mirena, the levonorgestrelcontaining intrauterine contraceptive system, is an option for women with menorrhagia, endometriosis, or chronic pelvic pain.
Nearly one half of all pregnancies in the United States are unplanned.1 An unintended pregnancy can have serious health consequences in women with chronic medical conditions. Certain diseases can be worsened by pregnancy or are associated with adverse outcomes.2 Moreover, medications used to treat many chronic conditions are potentially teratogenic.3
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| OCPs may be considered in healthy, nonsmoking women older than 35 years if there are no other contraindications to combined hormonal contraceptives. | C | 6, 9, 35, 36 |
| OCPs may be considered in women who have migraine headaches without aura if they do not have focal neurologic symptoms, do not smoke, are younger than 35 years, and are otherwise healthy. | C | 6, 9, 44, 45 |
| OCPs appear to be safe in women with stable or inactive systemic lupus erythematosus who do not have antiphospholipid antibodies. | C | 6, 8, 9 |
| Injectable long-acting progestin (depot medroxyprogesterone acetate [Depo-Provera]) is an appropriate contraceptive option for women with sickle cell disease and has been shown to reduce painful crises. | C | 58, 59 |
| Injectable long-acting progestin is associated with a loss in bone mineral density; however, the length of use does not need to be restricted because the loss is reversible with discontinuation. | C | 6, 9, 66–70 |
| The single-rod implantable contraceptive device (Implanon) may be used to decrease symptoms of dysmenorrhea. | C | 72, 73 |
OCP = oral contraceptive pill.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Despite this, women with comorbidities may not receive adequate counseling on contraceptive methods. For example, in a study at an urban epilepsy center, 50 percent of women experienced unplanned pregnancies.4 Almost 17 percent of these women were taking antiepileptic drugs that reduce the effectiveness of hormonal contraceptives. Additionally, women with diabetes mellitus rarely receive contraceptive counseling during ambulatory visits,5 even though poor preconception glycemic control can be associated with adverse outcomes.2
In 2006, the American College of Obstetricians and Gynecologists (ACOG) published guidelines for the use of hormonal contraceptives in women with comorbidities.6 Since its publication, new contraceptive products have been approved by the U.S. Food and Drug Administration, and new data about the risks of the contraceptive patch (Ortho Evra) and the long-acting injectable progestin, depot medroxyprogesterone acetate (Depo-Provera), have emerged.
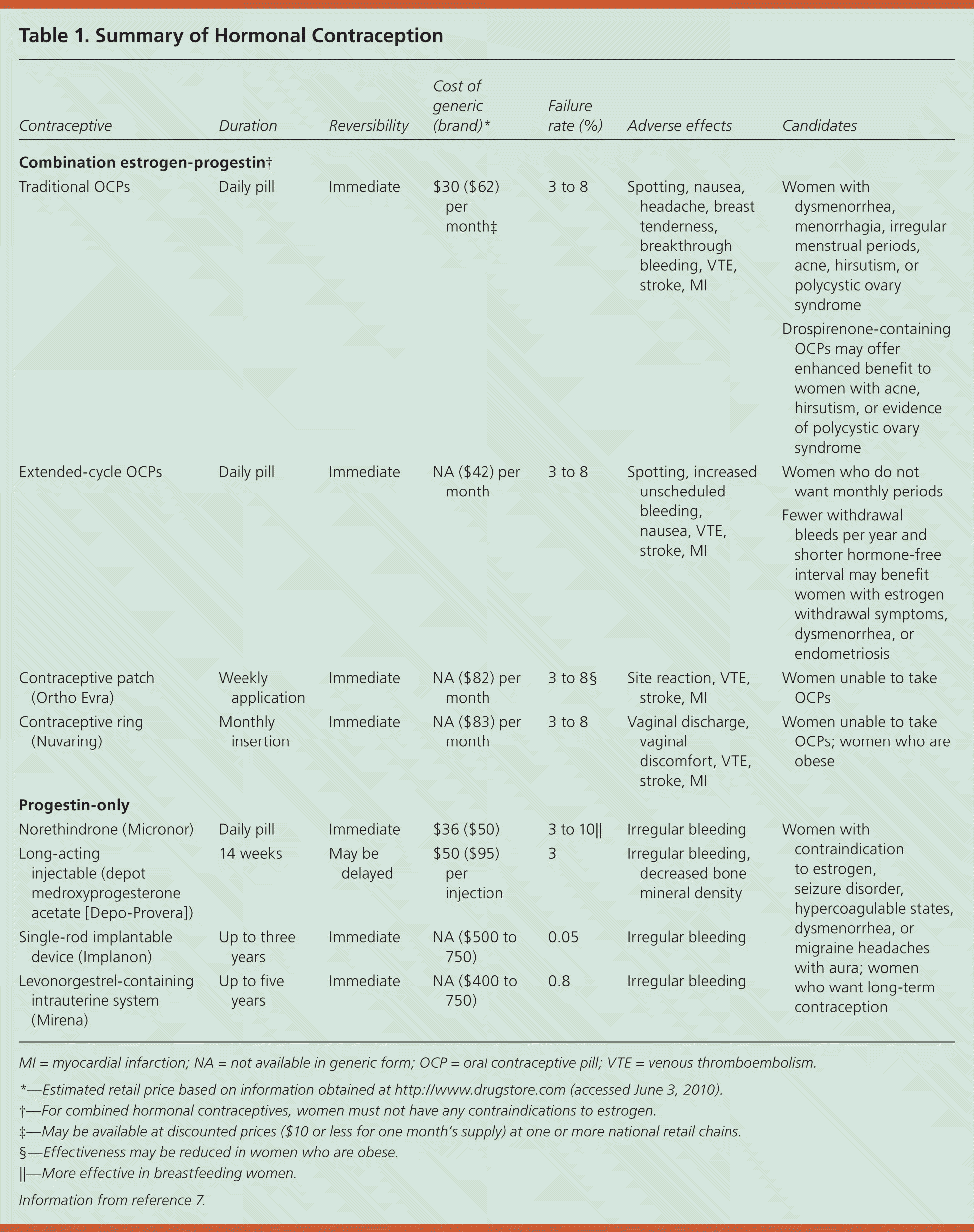
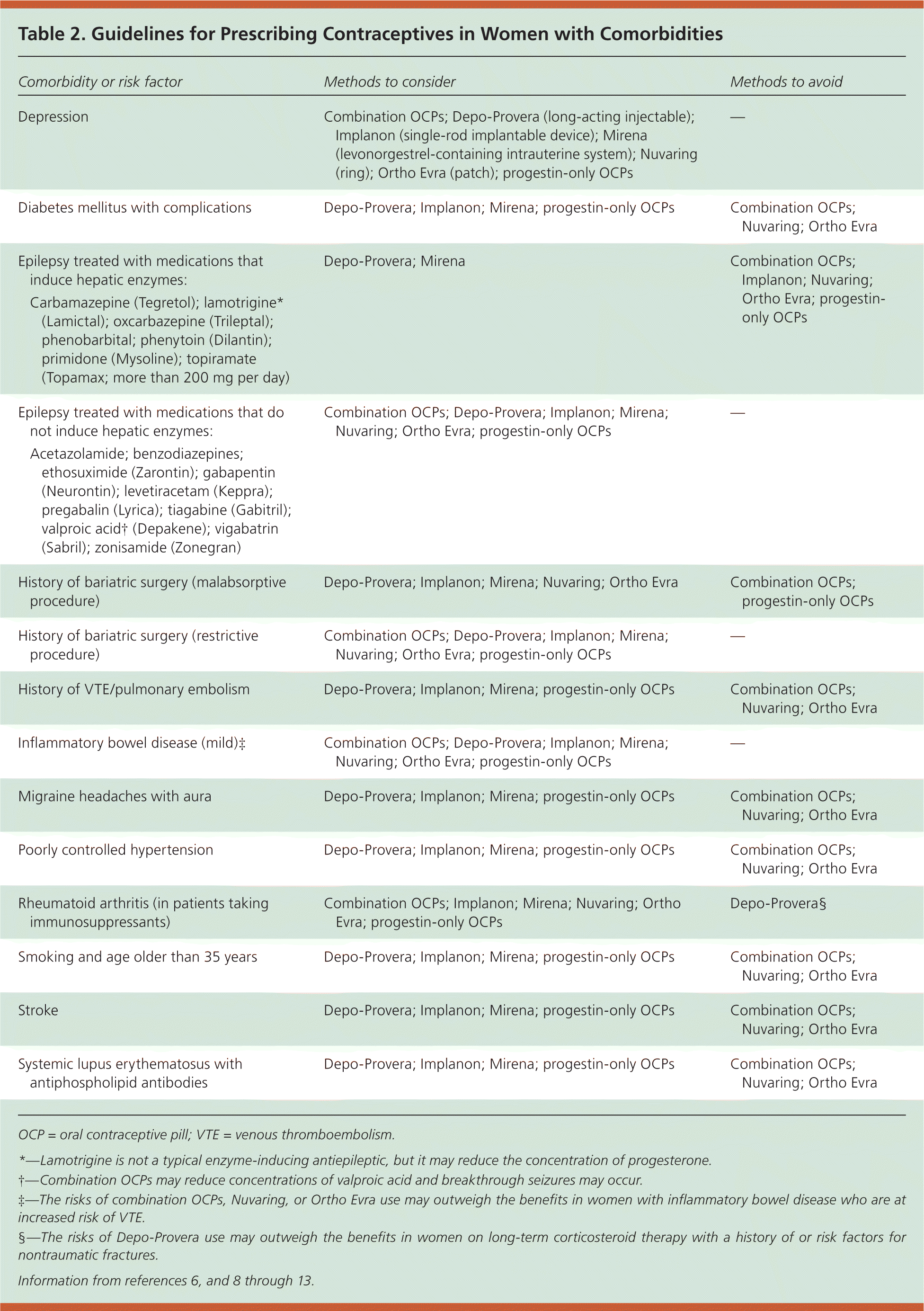
[ corrected] Although women of reproductive age with comorbidities may prefer, or be more appropriate for, nonpharmacologic family planning options, such as fertility awareness-based methods or barrier contraceptives, this article focuses on the prescription of hormonal contraceptives. Understanding the indications, benefits, and risks of these products, as well as patient preferences, will help physicians match patients with the contraceptive method best for them. Table 1 provides a summary of hormonal contraceptive options.7 Table 2 lists contraceptive methods to consider and those to avoid in women with comorbidities.6,8–13
Table 1. Summary of Hormonal Contraception
| Contraceptive | Duration | Reversibility | Cost of generic (brand)* | Failure rate (%) | Adverse effects | Candidates |
|---|---|---|---|---|---|---|
| Combination estrogen-progestin† | ||||||
| Traditional OCPs | Daily pill | Immediate | $30 ($62) per month‡ | 3 to 8 | Spotting, nausea, headache, breast tenderness, breakthrough bleeding, VTE, stroke, MI | Women with dysmenorrhea, menorrhagia, irregular menstrual periods, acne, hirsutism, or polycystic ovary syndrome |
| Drospirenone-containing OCPs may offer enhanced benefit to women with acne, hirsutism, or evidence of polycystic ovary syndrome | ||||||
| Extended-cycle OCPs | Daily pill | Immediate | NA ($42) per month | 3 to 8 | Spotting, increased unscheduled bleeding, nausea, VTE, stroke, MI | Women who do not want monthly periods |
| Fewer withdrawal bleeds per year and shorter hormone-free interval may benefit women with estrogen withdrawal symptoms, dysmenorrhea, or endometriosis | ||||||
| Contraceptive patch (Ortho Evra) | Weekly application | Immediate | NA ($82) per month | 3 to 8§ | Site reaction, VTE, stroke, MI | Women unable to take OCPs |
| Contraceptive ring (Nuvaring) | Monthly insertion | Immediate | NA ($83) per month | 3 to 8 | Vaginal discharge, vaginal discomfort, VTE, stroke, MI | Women unable to take OCPs; women who are obese |
| Progestin-only | ||||||
| Norethindrone (Micronor) [ | Daily pill | Immediate | $36 ($50) | 3 to 10|| | Irregular bleeding | Women with contraindication to estrogen, seizure disorder, hypercoagulable states, dysmenorrhea, or migraine headaches with aura; women who want long-term contraception |
| Long-acting injectable (depot medroxyprogesterone acetate [Depo-Provera]) | 14 weeks | May be delayed | $50 ($95) per injection | 3 | Irregular bleeding, decreased bone mineral density | |
| Single-rod implantable device (Implanon) | Up to three years | Immediate | NA ($500 to 750) | 0.05 | Irregular bleeding | |
| Levonorgestrel-containing intrauterine system (Mirena) | Up to five years | Immediate | NA ($400 to 750) | 0.8 | Irregular bleeding | |
MI = myocardial infarction; NA = not available in generic form; OCP = oral contraceptive pill; VTE = venous thromboembolism.
*—Estimated retail price based on information obtained at http://www.drugstore.com (accessed June 3, 2010).
†—For combined hormonal contraceptives, women must not have any contraindications to estrogen.
‡—May be available at discounted prices ($10 or less for one month's supply) at one or more national retail chains.
§—Effectiveness may be reduced in women who are obese.
||—More effective in breastfeeding women.
Information from reference 7.
Table 2. Guidelines for Prescribing Contraceptives in Women with Comorbidities
| Comorbidity or risk factor | Methods to consider | Methods to avoid | |
|---|---|---|---|
| Depression | Combination OCPs; Depo-Provera (long-acting injectable); Implanon (single-rod implantable device); Mirena (levonorgestrel-containing intrauterine system); Nuvaring (ring); Ortho Evra (patch); progestin-only OCPs | — | |
| Diabetes mellitus with complications | Depo-Provera; Implanon; Mirena; progestin-only OCPs | Combination OCPs; Nuvaring; Ortho Evra | |
| Epilepsy treated with medications that induce hepatic enzymes: | Depo-Provera; Mirena | Combination OCPs; Implanon; Nuvaring; Ortho Evra; progestin-only OCPs | |
| Carbamazepine (Tegretol); lamotrigine* (Lamictal); oxcarbazepine (Trileptal); phenobarbital; phenytoin (Dilantin); primidone (Mysoline); topiramate (Topamax; more than 200 mg per day) | |||
| Epilepsy treated with medications that do not induce hepatic enzymes: | Combination OCPs; Depo-Provera; Implanon; Mirena; Nuvaring; Ortho Evra; progestin-only OCPs | — | |
| Acetazolamide; benzodiazepines; ethosuximide (Zarontin); gabapentin (Neurontin); levetiracetam (Keppra); pregabalin (Lyrica); tiagabine (Gabitril); valproic acid† (Depakene); vigabatrin (Sabril); zonisamide (Zonegran) | |||
| History of bariatric surgery (malabsorptive procedure) | Depo-Provera; Implanon; Mirena; Nuvaring; Ortho Evra | Combination OCPs; progestin-only OCPs | |
| History of bariatric surgery (restrictive procedure) | Combination OCPs; Depo-Provera; Implanon; Mirena; Nuvaring; Ortho Evra; progestin-only OCPs | — | |
| History of VTE/pulmonary embolism | Depo-Provera; Implanon; Mirena; progestin-only OCPs | Combination OCPs; Nuvaring; Ortho Evra | |
| Inflammatory bowel disease (mild)‡ | Combination OCPs; Depo-Provera; Implanon; Mirena; Nuvaring; Ortho Evra; progestin-only OCPs | — | |
| Migraine headaches with aura | Depo-Provera; Implanon; Mirena; progestin-only OCPs | Combination OCPs; Nuvaring; Ortho Evra | |
| Poorly controlled hypertension | Depo-Provera; Implanon; Mirena; progestin-only OCPs | Combination OCPs; Nuvaring; Ortho Evra | |
| Rheumatoid arthritis (in patients taking immunosuppressants) | Combination OCPs; Implanon; Mirena; Nuvaring; Ortho Evra; progestin-only OCPs | Depo-Provera§ | |
| Smoking and age older than 35 years | Depo-Provera; Implanon; Mirena; progestin-only OCPs | Combination OCPs; Nuvaring; Ortho Evra | |
| Stroke | Depo-Provera; Implanon; Mirena; progestin-only OCPs | Combination OCPs; Nuvaring; Ortho Evra | |
| Systemic lupus erythematosus with antiphospholipid antibodies | Depo-Provera; Implanon; Mirena; progestin-only OCPs | Combination OCPs; Nuvaring; Ortho Evra | |
OCP = oral contraceptive pill; VTE = venous thromboembolism.
*—Lamotrigine is not a typical enzyme-inducing antiepileptic, but it may reduce the concentration of progesterone.
†—Combination OCPs may reduce concentrations of valproic acid and breakthrough seizures may occur.
‡—The risks of combination OCPs, Nuvaring, or Ortho Evra use may outweigh the benefits in women with inflammatory bowel disease who are at increased risk of VTE.
§—The risks of Depo-Provera use may outweigh the benefits in women on long-term corticosteroid therapy with a history of or risk factors for nontraumatic fractures.
Combined Hormonal Contraceptives
Oral contraceptive pills (OCPs) have been widely used in the United States for decades because of the contraceptive and noncontraceptive benefits of combined hormonal contraceptives. Many women want the noncontraceptive benefits of combined hormonal contraceptives, such as regulated menses, decreased dysmenorrhea, and diminished premenstrual dysphoric disorder. However, combined hormonal contraceptives are not appropriate for every patient. Before prescribing OCPs, physicians should obtain a complete medical history to determine whether OCPs may benefit patients or put them at increased risk of adverse events, such as stroke or venous thromboembolism (VTE). Most contraindications to OCPs can be ruled out during the history. Although a pelvic examination is not necessary before prescribing combined hormonal contraceptives,14 a focused physical examination that includes blood pressure measurement and evaluation for signs of hyperandrogenism, such as hirsutism or acne, may guide the contraceptive decision.
The noncontraceptive benefits of OCPs, as well as the established cardiovascular risks and common adverse effects, have been discussed elsewhere.15,16 Some risks of OCPs may be enhanced and some benefits may be negated in women with comorbidities. For example, OCPs containing 35 mcg of estrogen or less are optimal in most women to reduce the risks and adverse effects of estrogen. However, women with seizure disorders are an exception. The World Health Organization (WHO) recommends that women taking antiepileptic medications not be prescribed OCPs containing less than 30 mcg of estrogen because certain anticonvulsants can decrease the effectiveness of combined hormonal contraceptives.9
Many contraindications to combined hormonal contraceptives are caused by the estrogen component. Although the estrogen schedule may differ depending on the delivery (i.e., oral, transdermal, or intravaginal), the risks and benefits are grouped together in the WHO's updated 2009 medical eligibility criteria for contraceptive use.9 Several extended-cycle OCPs that shorten or eliminate the hormone-free interval have been developed to better manage common menstrual symptoms (e.g., headaches, tiredness, bloating, excessive bleeding, menstrual pain), as well as to improve OCP compliance through better symptom management.17–33 However, a systematic review of extended-cycle versus traditional 28-day–cycle OCPs found similar effectiveness and safety, and no difference in adherence.24 For the purpose of this article, unless otherwise stated, the risks and benefits of traditional OCPs can be extrapolated to extended-cycle OCPs, the contraceptive patch, and the contraceptive ring (Nuvaring).
Combined hormonal contraceptives can be used safely in women with a range of medical conditions, including well-controlled hypertension, uncomplicated diabetes, depression, uncomplicated valvular heart disease, migraine headaches without aura, systemic lupus erythematosus without antiphospholipid antibodies, human immunodeficiency virus (HIV) infection, thyroid disease, anemia, and uncomplicated liver disease.6,9
Table 3 lists selected contraindications to combined hormonal contraceptives.6,8,9,34 The contraindications in the WHO medical eligibility criteria for OCPs differ from those in the Physicians' Desk Reference34; according to the WHO, women who have systemic lupus erythematosus with antiphospholipid antibodies or unknown antibody results should avoid using combined hormonal contraceptives.9 Instead of listing contraindications, ACOG designates patients in whom progestin-only methods may be appropriate, such as in women older than 35 years who smoke or are obese.6
Table 3. Selected Contraindications to Combined Hormonal Contraceptives

| Carcinoma of the breast (known or suspected) or personal history of breast cancer |
| Carcinoma of the endometrium or other known or suspected estrogen-dependent neoplasia |
| Cerebral vascular or coronary artery disease (current or history of) |
| Cholestatic jaundice of pregnancy or jaundice with previous oral contraceptive pill use |
| Combination of smoking and age older than 35 years |
| Diabetes mellitus with complications |
| Headaches with focal neurologic symptoms |
| Hepatic adenomas or carcinoma |
| Hepatocellular disease (acute or chronic) with abnormal liver function |
| Hypersensitivity to any component in oral contraceptive pills |
| Major surgery with prolonged immobilization |
| Pregnancy (known or suspected) |
| Severe hypertension |
| Stroke |
| Systemic lupus erythematosus with antiphospholipid antibodies |
| Undiagnosed abnormal genital bleeding |
| Valvular heart disease with complications |
| Venous thromboembolism, thrombophlebitis, or thromboembolic disorders (acute or history of) |
AGE
Combined hormonal contraceptives are generally safe in healthy women older than 35 years who do not smoke, provided that there are no other contraindications.6 Data from U.S. trials suggest that stroke and myocardial infarction risks for OCP users compared with nonusers are similar in younger and older nonsmoking women.35,36
HYPERTENSION
Many risks of combined hormonal contraceptives, such as VTE and, less commonly, myocardial infarction or stroke, are related to the effects of estrogen on the cardiovascular system. These risks are increased in women older than 35 years who smoke. OCPs have been shown to elevate systolic and diastolic blood pressures by about 8 and 6 mm Hg, respectively.37 Caution should be used in women with elevated blood pressures, especially those older than 35 years. Guidelines from the WHO and ACOG suggest that the risks of OCPs outweigh the benefits in patients with poorly controlled hypertension.6,9
The risks of myocardial infarction and stroke in women with medically controlled hypertension who use OCPs are not known. However, ACOG and WHO guidelines recommend a trial of OCPs in women with well-controlled hypertension who are otherwise healthy and who do not have other contraindications to combined hormonal contraceptives. 6,9 Drospirenone-containing hormone combinations have been shown to modestly lower systolic and diastolic blood pressures in postmenopausal women,38–40 but these effects have not been shown in women of reproductive age. A third-generation OCP or progestin-only contraceptives may lower cardiovascular risk in women with hypertension.41–43 The relative risk of myocardial infarction and stroke remains high in women with hypertension who use OCPs and smoke, or who have uncontrolled diabetes or hypercholesterolemia. Progestin-only methods may be more appropriate in these women.6,44,45
DIABETES
ACOG recommends that the use of OCPs in women with diabetes be limited to women younger than 35 years who do not smoke; are otherwise healthy; and show no evidence of hypertension, nephropathy, retinopathy, or other vascular disease.6
MIGRAINE HEADACHES
There does not appear to be an increased risk of stroke in healthy, nonsmoking women taking OCPs containing 35 mcg of estrogen or less.6 However, migraine headaches with aura have been associated with up to a twofold increased risk of stroke in otherwise healthy women taking OCPs.46,47 Smoking further increases this risk.46
For this reason, migraine headache with aura is a contraindication to combined hormonal contraceptives. Stroke risk is not increased in patients with migraine without aura; therefore, combined hormonal contraceptives is not contraindicated unless the patient has other major risk factors for stroke (e.g., smoking, hypertension, diabetes) or unless the patient's headaches are exacerbated when OCPs are started.6,9,47 In general, OCPs may be cautiously considered in women who have migraine headaches if they do not have focal neurologic symptoms (such as aura), do not smoke, are younger than 35 years, and are otherwise healthy.6,9,44,45
OBESITY
Obesity can complicate the choice of contraceptives for several reasons. For example, data suggest that certain OCPs and the contraceptive patch may have limited effectiveness in women who are obese.48,49 Additionally, obesity is an independent risk factor for cardiovascular disease and VTE, and exposure to excess estrogen in these women may further increase their risk.49,50 The WHO considers the benefits of OCPs in this population to be greater than the harms,9 although ACOG suggests that a progestin-only method may be safer.6 Weight has not been shown to change the effectiveness of the contraceptive ring51 or extended-cycle OCPs.28 If the decision is made to prescribe OCPs to a patient who is obese, the physician should assess for comorbidities that would preclude her from using OCPs, such as severe hypertension or uncontrolled diabetes.
VENOUS THROMBOEMBOLISM
Although OCPs can increase the risk of VTE in all users, risk is especially high in women with a history of VTE, women with antiphospholipid antibodies, or women who are undergoing major surgery with an anticipated period of prolonged immobilization.9 The risk of VTE may also be higher in women who use OCPs that contain specific third-generation progestins, such as desogestrel and gestodene.52–54 There have been conflicting data about an increased risk of VTE in women who use the contraceptive patch; the risk may be slightly increased or equivalent to the risk of VTE in women who use OCPs.55–57 Although there are no recommendations to alter prescribing habits at this time, these risks should be balanced with the risk of pregnancy and pregnancy-related complications.
SYSTEMIC LUPUS ERYTHEMATOSUS
Use of OCPs in women with stable or inactive systemic lupus erythematosus does not appear to increase mild or severe flare-ups.8 If vascular disease, nephritis, or antiphospholipid antibodies are present, progestin-only methods are more appropriate.6
Progestin-Only Methods
LONG-ACTING INJECTABLE CONTRACEPTIVE
Depo-Provera is a highly effective, injectable, progestinonly contraceptive that is safe in women with a contraindication to estrogen (e.g., a history of cardiovascular disease, stroke, VTE, peripheral vascular disease).2,6 Women with sickle cell disease may note a decrease in sickling or painful crises with Depo-Provera use.58,59 Certain antiepileptic drugs (e.g., carbamazepine [Tegretol], oxcarbazepine [Trileptal], phenobarbital, phenytoin [Dilantin], topiramate [Topamax]) induce hepatic metabolism of estrogen and progestin, potentially leading to contraceptive failure in women taking OCPs.10 Conversely, lamotrigine (Lamictal) levels are reduced in patients taking OCPs, which may lead to an increase in seizures.11,60 Depo-Provera is effective in women taking enzyme-inducing antiepileptics, although there are some recommendations that the injection frequency be increased to every 10 weeks.10,11 Additionally, progestins may decrease seizure frequency.61
Data are conflicting regarding the effects of Depo-Provera on depression.62,63 ACOG has concluded that Depo-Provera does not worsen depressive symptoms.6 Depo-Provera reduces serum estradiol levels, which can adversely affect bone health.64 In 2004, the U.S. Food and Drug Administration issued a boxed warning associating
Depo-Provera use with loss of bone mineral density, and recommended that its use be limited to less than two years.65 In 2006, a seven-year, prospective matched cohort study in young women showed that those who used Depo-Provera had substantial bone mineral density loss, but the loss was reversible with discontinuation of use.66 Systematic reviews in 2006 and 2008 reached the same conclusion about the reversibility of bone mineral density loss.67,68
The WHO has recommended that there be no restriction on the use of Depo-Provera in women 18 to 45 years of age, and that the benefits likely outweigh the harms in women outside that age group.69 Physicians should counsel patients about the risk of bone mineral density loss, but reassure them about reversibility with discontinuation. No evidence exists to support routine bone mineral density assessment in women who use Depo-Provera.6,70
SINGLE-ROD IMPLANTABLE CONTRACEPTIVE DEVICE
The single-rod implantable contraceptive device containing etonogestrel (Implanon) is inserted subdermally in the upper arm and remains active for three years.71 It has been available for more than 10 years, but has been widely marketed in the United States only since 2007. Insertion and removal of the implant requires specific training by the manufacturer.
Implanon has been shown to be beneficial in women with dysmenorrhea. One study found that it is associated with a decrease in symptoms in 80 percent of women.72 ACOG has suggested that the contraceptive implant may be used for dysmenorrhea.73
WHO guidelines consider Implanon to be a contraceptive option in women with a history of hypertension, diabetes, VTE, cardiovascular disease or stroke, migraine headaches (with or without aura), seizure disorder, sickle cell disease, or HIV infection.9
LEVONORGESTREL-CONTAINING INTRAUTERINE CONTRACEPTIVE SYSTEM
The levonorgestrel-containing intrauterine contraceptive system (Mirena) has been reviewed previously,74 but is another option for women with contraindications to estrogen who want long-term contraception.6,9 It may be considered specifically in women with menorrhagia, endometriosis, or chronic pelvic pain.74

