Am Fam Physician. 2010;82(6):665-666
Author disclosure: Nothing to disclose.
Conjunctivitis causes irritation, itching, foreign body sensation, and watering or discharge of the eye.
Most cases in adults are probably due to viral infection, but children are more likely to develop bacterial conjunctivitis than viral forms. The main bacterial pathogens are Staphylococcus species in adults, and Haemophilus influenzae, Streptococcus pneumoniae, and Moraxella catarrhalis in children.
A bacterial cause is more likely if there is gluing of the eyelids and no itching.
Contact lens wearers may be more likely to develop gram-negative infections. Bacterial keratitis occurs in up to 30 out of 100,000 contact lens wearers.
Gonococcal ophthalmia neonatorum can occur in up to 10 percent of infants exposed to gonorrheal exudate during delivery, despite prophylaxis, and can be associated with bacteremia and meningitis.
Otitis media can occur in 25 percent of children with H. influenzae conjunctivitis, and meningitis can develop in 18 percent of persons with meningococcal conjunctivitis. Conjunctivitis resolves spontaneously without treatment within two to five days in more than one half of persons, but infectious complications rarely occur.
Topical antibiotics may speed up clinical and microbiological cure of bacterial conjunctivitis, but the benefit is small.
In persons with suspected, but not confirmed, bacterial conjunctivitis, empiric treatment with topical antibiotics may be beneficial. However, this benefit is marginal, so it is advisable to suggest that patients take antibiotics only if symptoms do not resolve after one to two days.
Clinical and microbiological cure rates are increased in the first week in persons with culture-positive bacterial conjunctivitis, but there is no good evidence of a longer-term benefit from topical antibiotics.
Adverse effects of topical antibiotics are mild, but their effect on bacterial resistance is unknown.
Parenteral antibiotics may cure gonococcal ophthalmia neonatorum, although we do not know whether they are beneficial in children in developed countries because we only found studies from Africa. Neonates usually require investigation for concomitant infections and complications.
We do not know whether ocular decongestants, saline, or warm compresses are beneficial in persons with suspected or confirmed bacterial or gonococcal conjunctivitis.
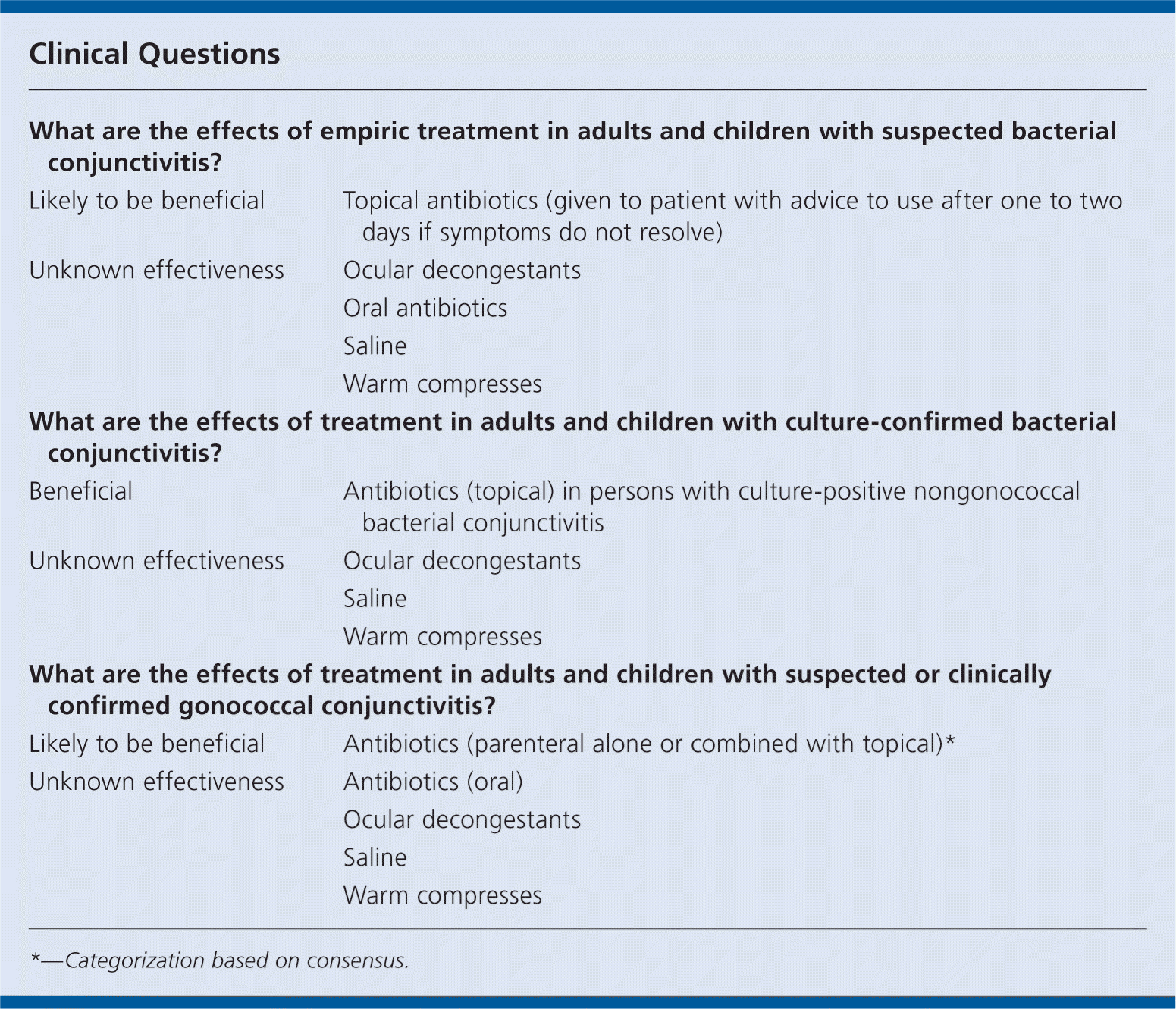
| What are the effects of empiric treatment in adults and children with suspected bacterial conjunctivitis? | |
| Likely to be beneficial | Topical antibiotics (given to patient with advice to use after one to two days if symptoms do not resolve) |
| Unknown effectiveness | Ocular decongestants |
| Oral antibiotics | |
| Saline | |
| Warm compresses | |
| What are the effects of treatment in adults and children with culture-confirmed bacterial conjunctivitis? | |
| Beneficial | Antibiotics (topical) in persons with culture-positive nongonococcal bacterial conjunctivitis |
| Unknown effectiveness | Ocular decongestants |
| Saline | |
| Warm compresses | |
| What are the effects of treatment in adults and children with suspected or clinically confirmed gonococcal conjunctivitis? | |
| Likely to be beneficial | Antibiotics (parenteral alone or combined with topical)* |
| Unknown effectiveness | Antibiotics (oral) |
| Ocular decongestants | |
| Saline | |
| Warm compresses | |
Definition
Conjunctivitis is any inflammation of the conjunctiva, generally characterized by irritation, itching, foreign body sensation, and watering or discharge. Treatment is often based on clinical suspicion that the conjunctivitis is bacterial, without waiting for the results of microbiological tests. Therefore, in this review, we have distinguished the effects of empiric treatment from effects of treatment in persons with culture-positive bacterial conjunctivitis. Bacterial conjunctivitis in contact lens wearers is of particular concern because of the risk of bacterial keratitis—an infection of the cornea accompanying acute or subacute corneal trauma. Bacterial keratitis is more difficult to treat than conjunctivitis and can threaten vision. Conjunctivitis caused by Neisseria gonorrhoeae—referred to as ophthalmia neonatorum—is primarily a disease of neonates that is caused by exposure of the neonatal conjunctivae to the cervicovaginal exudate of infected women during delivery.
Incidence and Prevalence
We found no good evidence on the incidence or prevalence of bacterial conjunctivitis. Bacterial keratitis is estimated to occur in 10 to 30 out of 100,000 contact lens wearers. Gonococcal ophthalmia neonatorum occurs in up to 10 percent of infants who received antibiotic prophylaxis after delivery to mothers with gonorrhea infection, and in 2 to 48 percent of exposed infants without prophylaxis.
Etiology
Conjunctivitis may be infectious (causes include bacteria and viruses) or allergic. In adults, bacterial conjunctivitis is less common than viral conjunctivitis, although estimates vary widely (viral conjunctivitis has been reported to account for 8 to 75 percent of acute conjunctivitis). Staphylococcus species are the most common pathogens for bacterial conjunctivitis in adults, followed by S. pneumoniae and H. influenzae. In children, bacterial conjunctivitis is more common than the viral form, and is mainly caused by H. influenzae, S. pneumoniae, and M. catarrhalis. One prospective study (428 children from southern Israel with a clinical diagnosis of conjunctivitis) found that in 55 percent of the children, conjunctivitis was caused by S. pneumoniae, H. influenzae, or M. catarrhalis. Narrative reviews suggest that the causative agents of bacterial conjunctivitis and keratitis in contact lens wearers are usually gram-negative bacteria (such as Pseudomonas aeruginosa), but may include all of the above agents. Acanthamoeba infections can be particularly difficult to diagnose and treat, and are most common in contact lens wearers.
Prognosis
Bacterial conjunctivitis is usually self-limiting. One systematic review (search date of 2004) found clinical cure or significant improvement with placebo within two to five days in 65 percent of persons. Some organisms cause corneal or systemic complications, or both. Otitis media may develop in 25 percent of children with H. influenzae conjunctivitis, and systemic meningitis may complicate primary meningococcal conjunctivitis in 18 percent of persons. Untreated gonococcal ophthalmia neonatorum can cause corneal ulceration, perforation of the globe, and panophthalmitis. Investigations to detect concomitant infections, gonococcal bacteriemia, and meningitis are often required, as well as admission to the hospital for parenteral treatment of the eye infection.