The differential diagnosis of left lower-quadrant pain includes gastrointestinal, gynecologic, and renal/ureteric pathology. Imaging is helpful in evaluating left lower-quadrant pain, and is generally guided by the clinical presentation. Acute sigmoid diverticulitis should be suspected when the clinical triad of left lower-quadrant pain, fever, and leukocytosis is present. The severity of disease varies from mild pericolonic and peridiverticular inflammation to severe inflammatory changes with complications such as perforation, peritonitis, or abscess or fistula formation. Computed tomography is the preferred test in evaluating clinically suspected diverticulitis. It is used to evaluate the severity and extent of disease and to identify complications, but it also may diagnose other causes of left lower-quadrant pain that can mimic diverticulitis. Magnetic resonance imaging can be used to assess left lower-quadrant pain. It has superior resolution of soft tissues and does not expose the patient to ionizing radiation, but it is expensive and requires more time to perform. Transabdominal ultrasonography with graded compression is another effective technique but is limited by its high operator dependency and technical difficulties in scanning patients who are obese. Pelvic ultrasonography is the preferred imaging modality in women of childbearing age. Radiography with contrast enema is less sensitive than computed tomography in diagnosing diverticulitis and is seldom used.
Acute sigmoid diverticulitis, a complication of colonic diverticulosis, is the most common cause of acute left lower-quadrant pain in adults. Diverticulosis occurs in 5 to 10 percent of persons by 45 years of age, and in up to 80 percent by 80 years of age.1 Although most persons with diverticulosis never have symptoms, diverticulitis occurs in 10 to 20 percent of persons with this condition,2 and recurrent diverticulitis occurs in approximately 25 percent of these patients.3 The severity ranges from mild to severe, which can result in perforation with peritonitis and abscess or fistula formation. The severity of the initial attack is an excellent predictor of the likelihood of recurrence.4 Mild cases of diverticulitis can be treated medically. More severe cases may require emergent surgery as a result of complications.5
Acute sigmoid diverticulitis should be suspected in patients with the clinical triad of left lower-quadrant pain, fever, and leukocytosis. Additional diagnostic considerations include, but are not limited to, other gastrointestinal pathology, obstetric and gynecologic pathology, and renal or ureteric colic (Table 1). This article reviews the most appropriate imaging studies in adults presenting with left lower-quadrant pain, according to the American College of Radiology (ACR) Appropriateness Criteria (Table 2).6
Table 1. Differential Diagnosis of Left Lower-Quadrant Pain
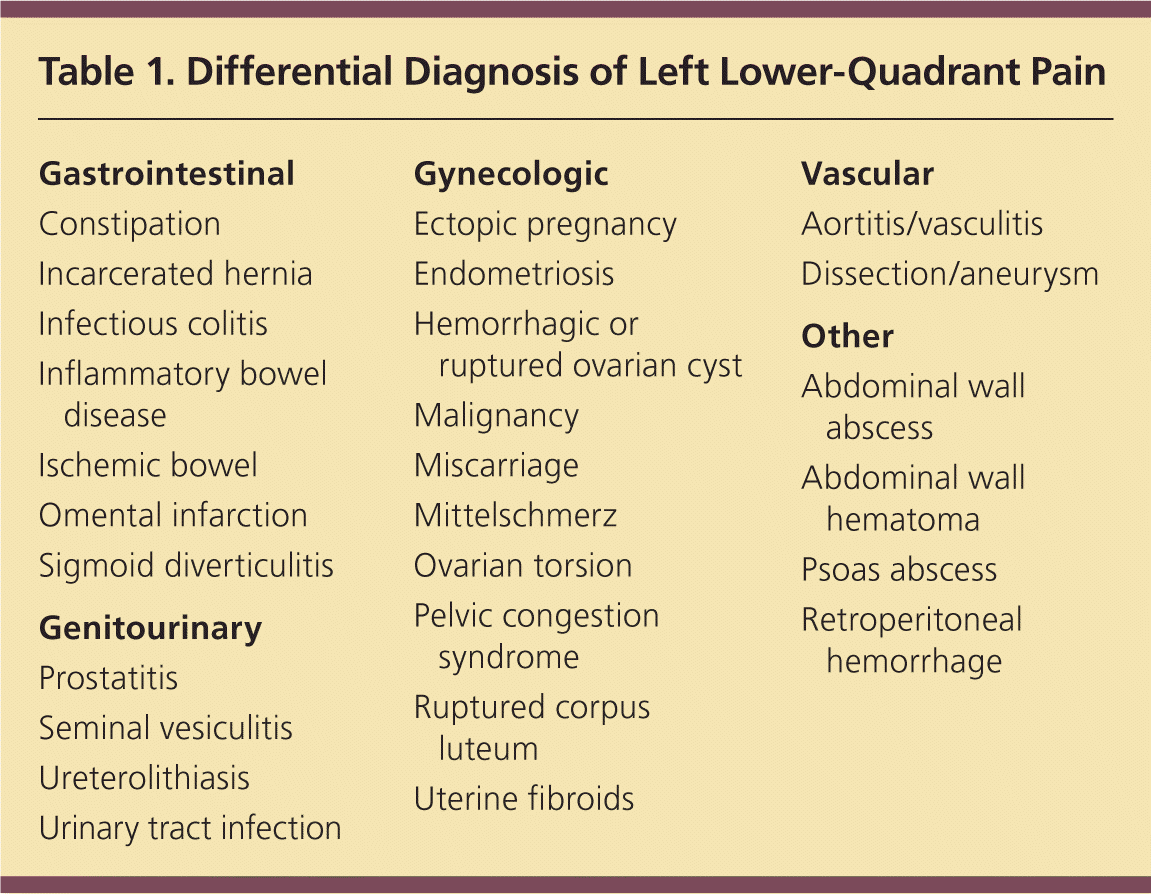
| Gastrointestinal |
| Constipation |
| Incarcerated hernia |
| Infectious colitis |
| Inflammatory bowel disease |
| Ischemic bowel |
| Omental infarction |
| Sigmoid diverticulitis |
| Genitourinary |
| Prostatitis |
| Seminal vesiculitis |
| Ureterolithiasis |
| Urinary tract infection |
| Gynecologic |
| Ectopic pregnancy |
| Endometriosis |
| Hemorrhagic or ruptured ovarian cyst |
| Malignancy |
| Miscarriage |
| Mittelschmerz |
| Ovarian torsion |
| Pelvic congestion syndrome |
| Ruptured corpus luteum |
| Uterine fibroids |
| Vascular |
| Aortitis/vasculitis |
| Dissection/aneurysm |
| Other |
| Abdominal wall abscess |
| Abdominal wall hematoma |
| Psoas abscess |
| Retroperitoneal hemorrhage |
Table 2. American College of Radiology Appropriateness Criteria for Left Lower-Quadrant Pain in Older Patients with Suspected Diverticulitis
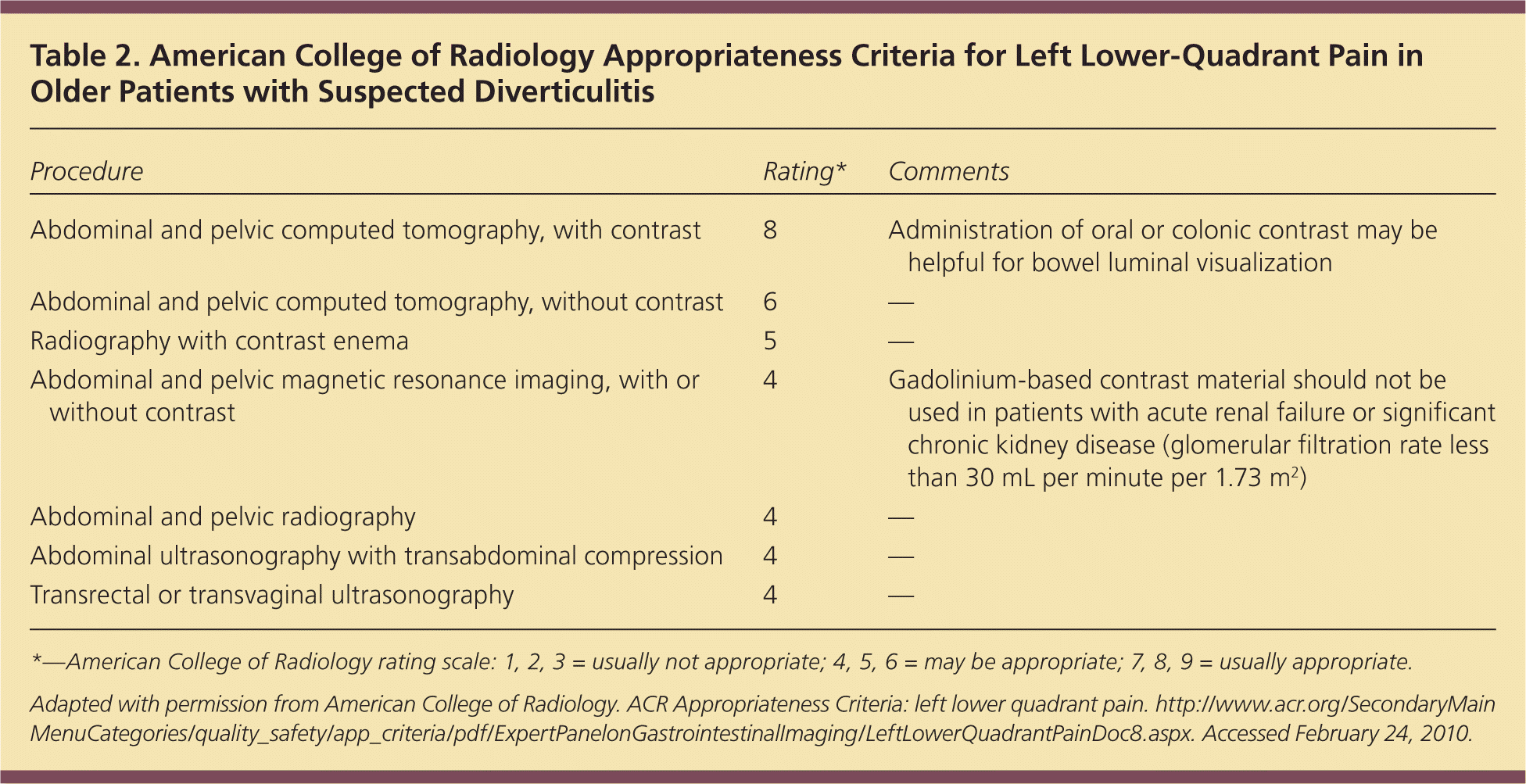
| Procedure | Rating* | Comments |
|---|---|---|
| Abdominal and pelvic computed tomography, with contrast | 8 | Administration of oral or colonic contrast may be helpful for bowel luminal visualization |
| Abdominal and pelvic computed tomography, without contrast | 6 | — |
| Radiography with contrast enema | 5 | — |
| Abdominal and pelvic magnetic resonance imaging, with or without contrast | 4 | Gadolinium-based contrast material should not be used in patients with acute renal failure or significant chronic kidney disease (glomerular filtration rate less than 30 mL per minute per 1.73 m2) |
| Abdominal and pelvic radiography | 4 | — |
| Abdominal ultrasonography with transabdominal compression | 4 | — |
| Transrectal or transvaginal ultrasonography | 4 | — |
*—American College of Radiology rating scale: 1, 2, 3 = usually not appropriate; 4, 5, 6 = may be appropriate; 7, 8, 9 = usually appropriate.
Adapted with permission from American College of Radiology. ACR Appropriateness Criteria: left lower quadrant pain. http://www.acr.org/SecondaryMainMenuCategories/quality_safety/app_criteria/pdf/ExpertPanelonGastrointestinalImaging/LeftLowerQuadrantPainDoc8.aspx. Accessed February 24, 2010.
Illustrative Cases
CASE 1
A 64-year-old man presents with left lower-quadrant pain that has progressively worsened over the past three days. Axial contrast-enhanced computed tomography (CT) shows multiple diverticula in the sigmoid colon, with stranding of the adjacent fat (Figure 1A). A coronal reformatted image shows the offending diverticulum (Figure 1B). The patient is treated conservatively with antibiotics.
Figure 1.
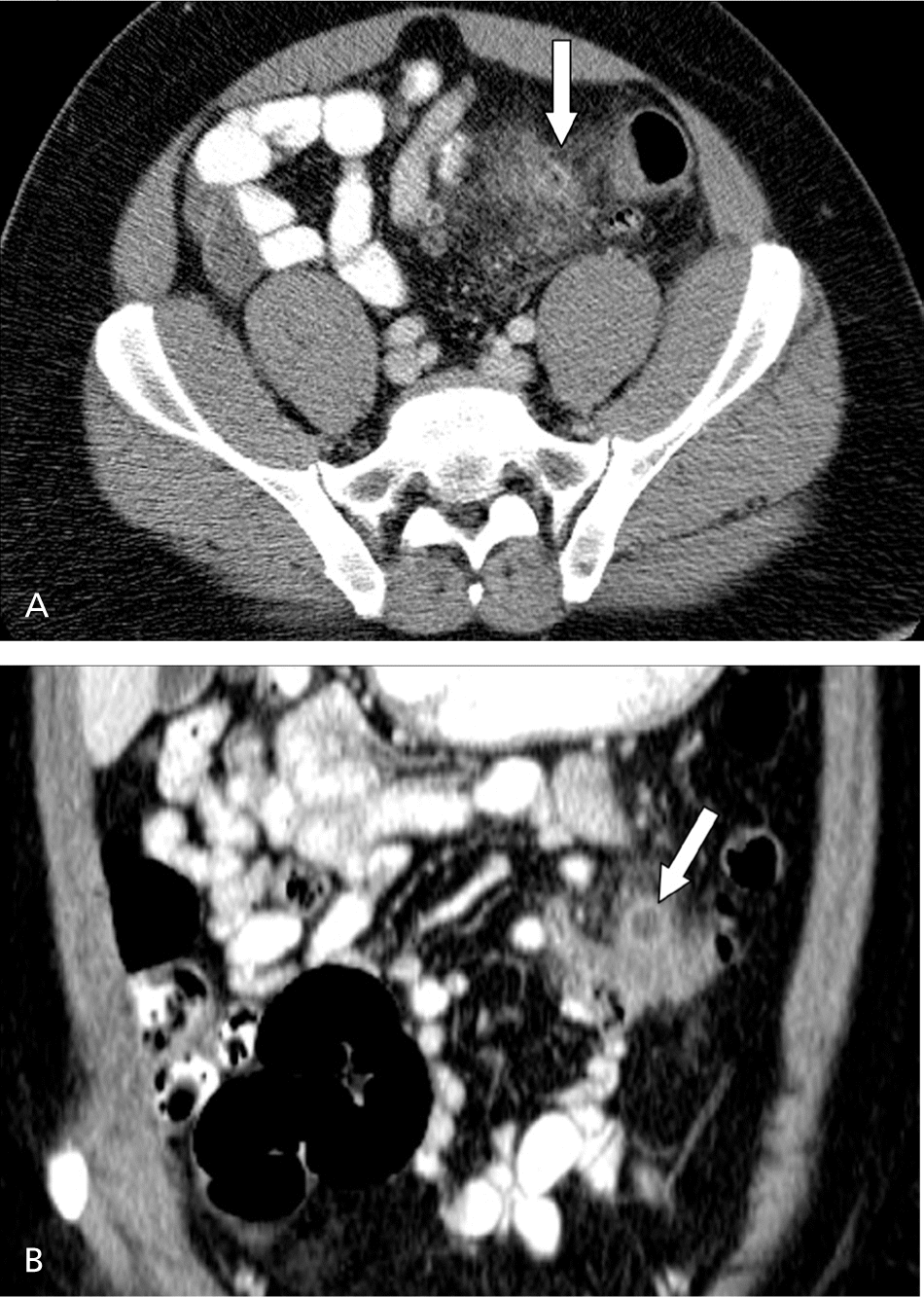
(A) Contrast-enhanced axial computed tomography scan shows stranding of the fat adjacent to the sigmoid colon, with scattered colonic diverticula (arrow). (B)Coronal reformatted image shows the offending diverticulum at the epicenter of the inflammatory changes (arrow).
CASE 2
A 44-year-old man who was recently treated conservatively for diverticulitis presents with recurrent left lower-quadrant pain and fever. Contrast-enhanced CT shows a rim-enhancing gas and fluid collection adjacent to the sigmoid colon, which is consistent with a diverticular abscess (Figure 2). Multiple sigmoid diverticula, colonic wall thickening, and pericolonic fat stranding are also present. The abscess is drained percutaneously.
Figure 2.
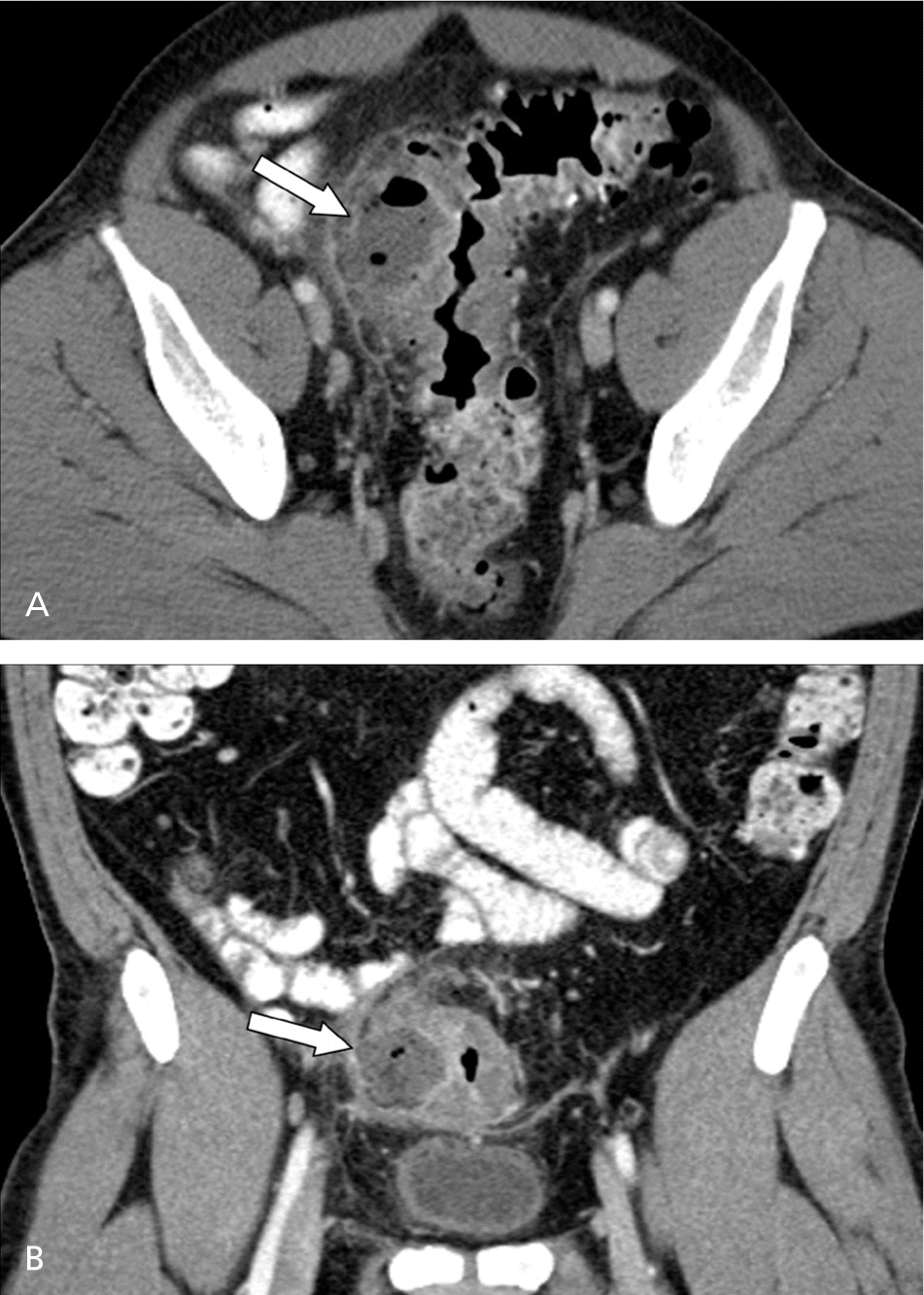
(A) Contrast-enhanced axial computed tomography scan shows pericolonic rim-enhancing gas and fluid collection consistent with a diverticular abscess (arrow). Note the stranding to the surrounding fat and the adjacent colonic wall thickening. (B) Coronal reformatted image further depicts the diverticular abscess (arrow).
CASE 3
A 76-year-old man with recurrent sigmoid diverticulitis presents with left lower-quadrant pain and fever. Contrast-enhanced CT shows a diverticular fistula communicating with an abscess (Figure 3). Rectal contrast delineates the fistula tract. The patient undergoes a sigmoidectomy.
Figure 3.
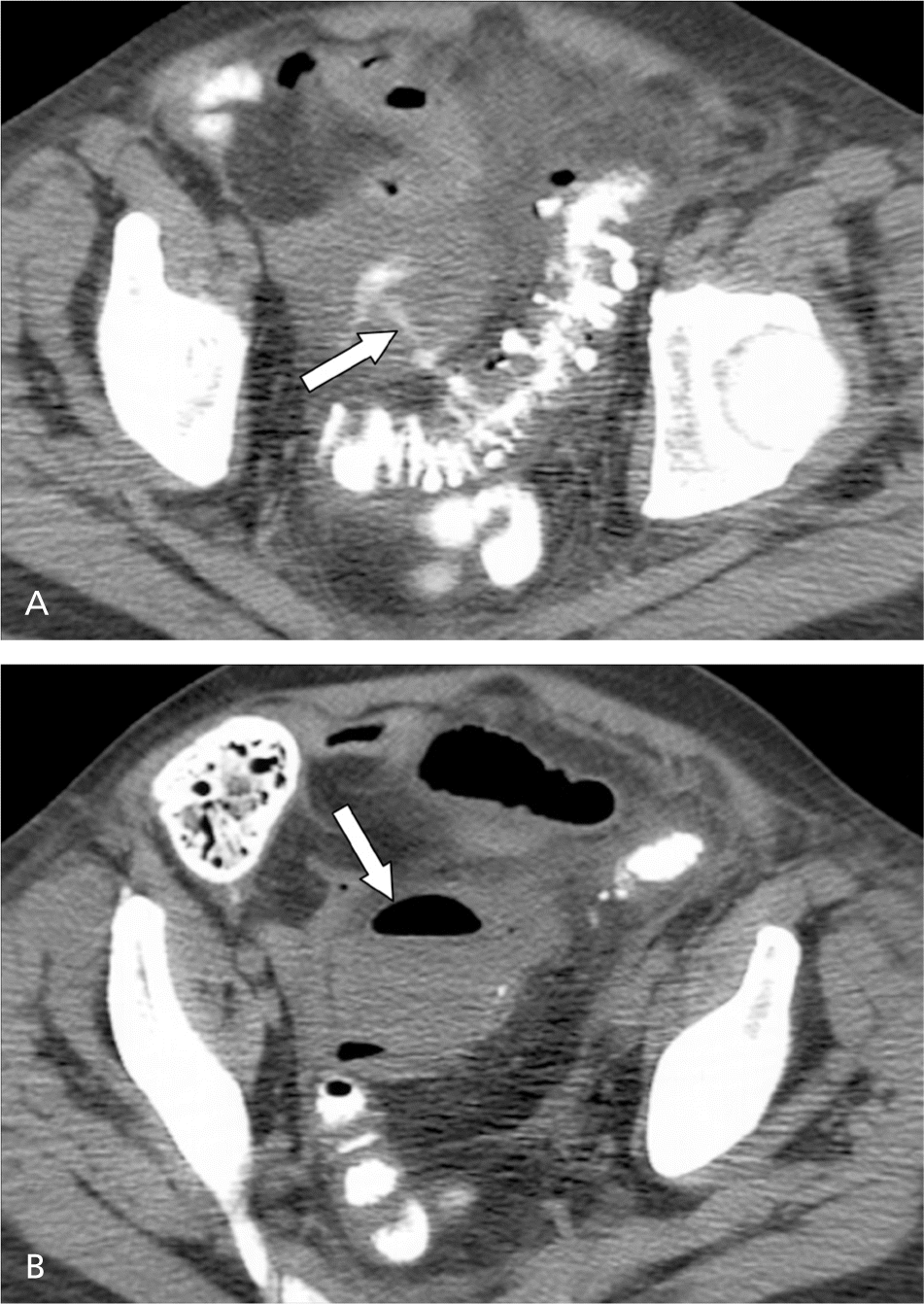
(A) Contrast-enhanced axial computed tomography scan shows contrast material extending into a diverticular abscess via a fistula tract (arrow). Multiple sigmoid diverticula and free fluid in the pelvis are also present. (B) Axial image obtained just inferior to the fistula tract shows the full extent of the associated diverticular abscess, which contains an air-fluid level (arrow).
Radiologic Evaluation
Imaging of patients with lower-quadrant pain should be guided by the clinical scenario. The differential diagnosis should be considered, and any additional relevant information should be obtained to guide clinical management. Imaging may not be necessary in patients with the classic triad of left lower-quadrant pain, fever, and leukocytosis, and in whom uncomplicated diverticulitis is suspected. Imaging also may not be necessary in patients with a history of diverticulitis who present with relatively mild clinical symptoms of recurrent disease. However, imaging often plays a definitive role in evaluating left lower-quadrant pain of unclear etiology.
COMPUTED TOMOGRAHPY
CT is the preferred imaging modality in patients with clinically suspected diverticulitis.7 However, it should be used judiciously in female patients of childbearing age in whom gynecologic etiologies have been clinically or sonographically excluded. CT allows for diagnosis of other causes of left lower-quadrant pain that may mimic diverticulitis, which is important in directing appropriate medical management. The ACR Appropriateness Criteria specifies CT as the most appropriate imaging test for patients with acute, severe left lower-quadrant pain with or without fever; for patients with chronic, intermittent, or low-grade left lower-quadrant pain; and for patients who are obese with left lower-quadrant pain.6
CT has reported sensitivity and specificity as high as 100 percent in diagnosing sigmoid diverticulitis.8 Additionally, CT is rapid, widely available, and highly reproducible.9 It has a key role in determining the extent and severity of disease, and in assessing for complications such as colonic perforation and abscess and fistula formation. CT can be used to guide percutaneous drainage when abscesses are present, and it is particularly helpful when an abscess is located deep in the pelvis or is surrounded by vital structures. CT also helps determine the severity of disease to facilitate selection of patients for medical versus surgical treatment.10–16
The most common CT findings in patients with acute diverticulitis are pericolonic fat stranding, bowel wall thickening, and diverticula. Additional findings may include free fluid, free air, fascial thickening, an inflamed diverticulum, or the arrowhead sign (i.e., an arrowhead-shaped configuration of contrast material found at the orifice of the inflamed diverticulum7).17 Muscular hypertrophy also may occur as a response to longstanding elevated intraluminal pressures resulting from the underlying pathophysiology of diverticulosis; it has a reported specificity of 98 percent for diverticulitis.17
Bowel opacification optimizes the sensitivity and specificity of CT for the diagnosis of diverticulitis.18 Adequate bowel opacification can be achieved with oral or rectal administration of contrast. Rectal administration has been advocated for optimal colonic distention, which increases the accuracy of CT in detecting diverticulitis.18 It also eliminates the delay required for oral contrast to reach the distal colon. Although rectal administration is typically not necessary to diagnose diverticulitis, it can be useful in some cases. The diagnosis of diverticulitis can usually be made without the administration of intravenous contrast. However, intravenous contrast increases the ability of CT to evaluate for complications, and it is helpful in identifying alternative diagnoses.
In the acute setting, perforated colon cancer can be difficult to distinguish from diverticulitis on CT in some patients. The presence of pericolonic lymphadenopathy on CT has been shown to be a strong predictor of colon cancer rather than diverticulitis.19
Although CT is the preferred imaging test in patients with suspected diverticulitis, it should be used judiciously because it exposes the patient to ionizing radiation. However, one review concluded that the risk of radiation-induced malignancy is small and is typically justified by medical need in symptomatic patients.20
MAGNETIC RESONANCE IMAGING
Preliminary studies show that magnetic resonance imaging (MRI) has diagnostic potential in evaluating for diverticulitis,21,22 although its practicality is still evolving. Advantages of MRI over CT include a lack of ionizing radiation and superior resolution of soft tissues. Disadvantages include longer scan times, greater susceptibility to motion artifact, higher cost, and decreased availability.
In patients with colonic diverticulitis, MRI findings may include pericolonic fat stranding, bowel wall thickening, and diverticula.21 MRI readily shows abscess or fistula formation secondary to diverticulitis.
The use of gadolinium-enhanced MRI may be limited in patients with renal disease because the U.S Food and Drug Administration has issued a boxed warning recommending that gadolinium-based contrast material be avoided in patients with acute renal failure or significant chronic kidney disease (glomerular filtration rate less than 30 mL per minute per 1.73 m2).
ULTRASONOGRAPHY
Transabdominal ultrasonography using graded compression is effective in evaluating for suspected diverticulitis,23,24 but it is not widely used in the acute clinical setting. Ultrasound findings in patients with diverticulitis include a thickened loop of bowel with a target-like appearance.
One review found limited evidence to support the use of ultrasonography as the preferred diagnostic test in patients with suspected diverticulitis.25 A meta-analysis of six studies of ultrasonography and eight studies of CT showed that there is no statistically significant difference between modalities in diagnosing acute diverticulitis, and that both can be used as an initial diagnostic tool.26 However, CT may be more likely to identify alternative causes of abdominal pain. Ultrasonography may be difficult to perform in patients who are obese and requires technical expertise for interpretation, and the graded compression technique may be uncomfortable in patients with acute abdominal pain. Consequently, there has not been widespread use of ultrasonography for the diagnosis of diverticulitis in the United States.
Transvaginal and transabdominal pelvic ultrasonography is the preferred imaging technique in women of childbearing age to assess for gynecologic conditions such as ectopic pregnancy and pelvic inflammatory disease.6
RADIOGRAPHY WITH CONTRAST ENEMA
Before the advent of CT, radiography with contrast enemas was the primary diagnostic tool in evaluating for diverticulitis. CT has higher sensitivity and specificity than this technique.27 Radiography shows the secondary effects of inflammation in the colon and does not show pericolonic inflammation, abscesses, or extracolonic pathology.
Because diverticulitis can be difficult to distinguish from colon cancer on CT in the acute setting, radiography with contrast enemas may be helpful as a follow-up study to exclude an underlying colonic neoplasm, especially if colonoscopy cannot be performed because of strictures.

