to the editor: Sebaceous cell carcinoma of the eyelid is the fourth most common malignancy in the periocular region in the United States (basal cell carcinoma, squamous cell carcinoma, and melanoma are the leading three causes) and the second most common malignancy in China (basal cell carcinoma is the leading cause).1,2 Diagnosis and therapy tend to be delayed because sebaceous carcinoma is often mistaken for benign entities such as chalazion, conjunctivitis, or blepharitis.3
A 74-year-old woman presented to her ophthalmologist with conjunctival erythema and slight tenderness of her upper eyelid. She was diagnosed with conjunctivitis and prescribed erythromycin 0.5% ophthalmic ointment. At her one-month follow-up visit, she continued to have erythema and had also developed a small tender papule. A diagnosis of chalazion was made, and the patient was instructed to continue her antibiotic ointment and to apply warm compresses four times daily to the eye. At her two-month follow-up visit, the papule had enlarged to a 2-cm nodule (see accompanying figure). An excisional biopsy was performed, and pathology was consistent with a poorly differentiated invasive sebaceous carcinoma. Workup for metastases was negative. The patient underwent Mohs micrographic surgery for tumor extirpation. Oculoplastic reconstruction was performed with a tarsoconjunctival flap from the right lower lid and a free right retroauricular skin graft repair. She remained disease free at nine months.
Figure.
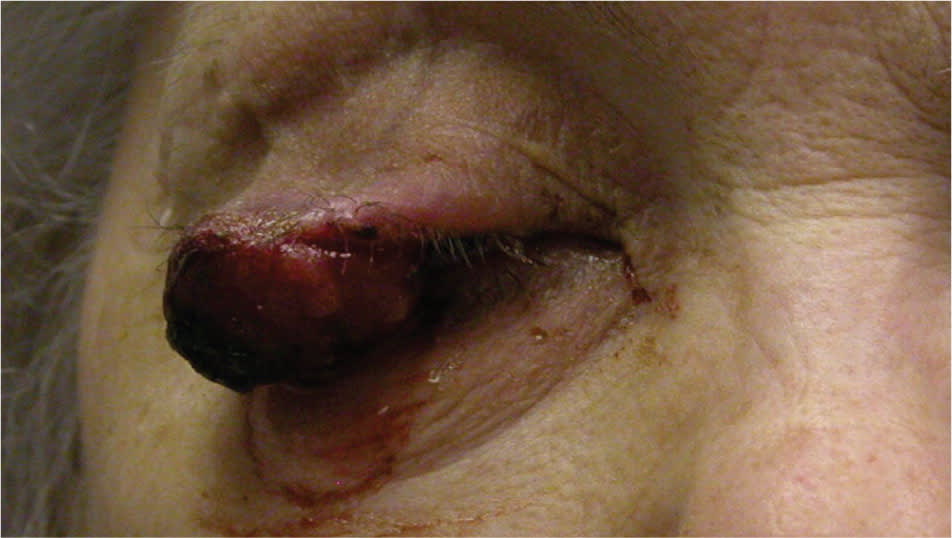
Sebaceous cell carcinoma nodule on the upper right eyelid.
The etiology of sebaceous gland carcinoma is idiopathic. It rarely occurs in childhood, with the highest frequency occurring in persons 60 to 79 years of age.4 An association has been established between sebaceous carcinoma and Muir-Torre syndrome, which combines at least one sebaceous neoplasm (i.e., sebaceous adenoma, sebaceous epithelioma, or sebaceous carcinoma) and at least one visceral malignancy (usually gastrointestinal or genitourinary carcinomas).5 Evaluation for Muir-Torre syndrome includes a rectal examination, colonoscopy or barium enema, and a first-morning urine sample for cytologic analysis.6
The diagnosis of sebaceous carcinoma should be considered in cases of persistence of conjunctivitis or chalazion despite appropriate therapeutic interventions.

