Up to 11.3 percent of girls and 3.6 percent of boys will have a urinary tract infection (UTI) by 16 years of age, and recurrence of infection is common.
- Vesicoureteric reflux is identified in up to 40 percent of children being evaluated for a first UTI, and it is a risk factor for, but weak predictor of, renal scarring.
- Renal parenchymal defects occur in 5 to 15 percent of children within one to two years of their first presentation with UTI, and it is associated with increased risks of progressive renal damage. The risk of parenchymal defects probably diminishes over time.
There is consensus that antibiotics are beneficial in children with UTI compared with no treatment, although few studies have been done to confirm this.
- Shorter courses (two to four days) of initial intravenous antibiotics seem as effective as longer courses (seven to 14 days) at curing infections, preventing recurrence of infection, and preventing renal parenchymal defects in children with acute pyelonephritis.
- Oral antibiotics may be as effective as intravenous antibiotics at treating UTI (including pyelonephritis) and preventing complications.
- Single-dose or single-day courses of oral antibiotics may be less effective than longer courses of oral antibiotics at treating UTI in children.
- Shorter courses (two to four days) of oral antibiotics seem as effective as longer courses at treating UTI in children without acute pyelonephritis or known renal tract abnormalities and may be associated with fewer adverse effects.
- We do not know whether immediate empiric antibiotic treatment is more effective at preventing renal parenchymal defects compared with treatment delayed for 24 hours.
- Immediate treatment may reduce the risk of renal parenchymal defects compared with treatment delayed for more than four days. Prophylactic antibiotics probably do not reduce the risk of recurrent UTI and can cause adverse effects.
- Immunotherapy, used in addition to prophylactic antibiotics, may reduce recurrence of UTI, but studies have been small.
Surgical correction of moderate to severe vesicoureteric reflux may be no more effective than medical management in preventing UTI recurrence or complications and increases morbidity associated with surgery.
- Children with minor functional anomalies do not seem to develop renal parenchymal defects, and therefore may not benefit from surgery for minor functional anomalies.
Clinical Questions
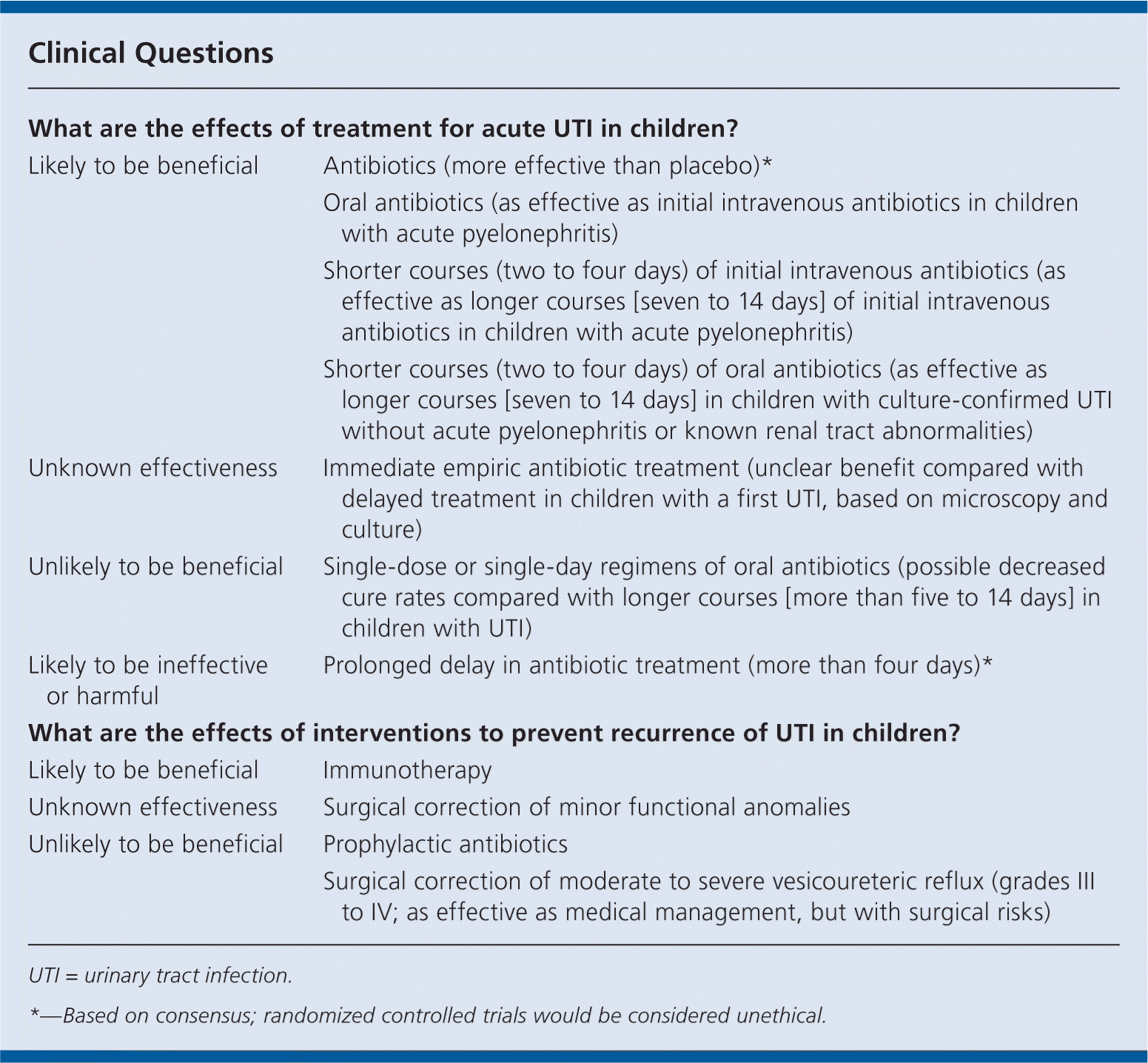
| What are the effects of treatment for acute UTI in children? | |
| Likely to be beneficial | Antibiotics (more effective than placebo)* |
| Oral antibiotics (as effective as initial intravenous antibiotics in children with acute pyelonephritis) | |
| Shorter courses (two to four days) of initial intravenous antibiotics (as effective as longer courses [seven to 14 days] of initial intravenous antibiotics in children with acute pyelonephritis) | |
| Shorter courses (two to four days) of oral antibiotics (as effective as longer courses [seven to 14 days] in children with culture-confirmed UTI without acute pyelonephritis or known renal tract abnormalities) | |
| Unknown effectiveness | Immediate empiric antibiotic treatment (unclear benefit compared with delayed treatment in children with a first UTI, based on microscopy and culture) |
| Unlikely to be beneficial | Single-dose or single-day regimens of oral antibiotics (possible decreased cure rates compared with longer courses [more than five to 14 days] in children with UTI) |
| Likely to be ineffective or harmful | Prolonged delay in antibiotic treatment (more than four days)* |
| What are the effects of interventions to prevent recurrence of UTI in children? | |
| Likely to be beneficial | Immunotherapy |
| Unknown effectiveness | Surgical correction of minor functional anomalies |
| Unlikely to be beneficial | Prophylactic antibiotics |
| Surgical correction of moderate to severe vesicoureteric reflux (grades III to IV; as effective as medical management, but with surgical risks) | |
UTI = urinary tract infection.
*—Based on consensus; randomized controlled trials would be considered unethical.
Definition
UTI is defined by the presence of a pure growth of more than 105 colony-forming units of bacteria per mL of urine. Lower counts of bacteria may be clinically important, especially in boys and in specimens obtained by urinary catheter. Any growth of typical urinary pathogens is considered clinically important if obtained by suprapubic aspiration. In practice, three age ranges are usually considered on the basis of differential risk and different approaches to management: children younger than one year; young children (ages one to four, five, or seven years, depending on the information source); and older children (up to 12 to 16 years of age). Recurrent UTI is defined as a further infection by a new organism. Relapsing UTI is defined as a further infection with the same organism.
Incidence and Prevalence
Boys are more susceptible to UTI than girls before six months of age; thereafter, the incidence is substantially higher in girls than in boys. Estimates of the true incidence of UTI depend on rates of diagnosis and investigation. Observational studies have found that in Sweden, UTIs are diagnosed in at least 2.2 percent of boys and 2.1 percent of girls by two years of age and in 7.8 percent of girls and 1.7 percent of boys by seven years of age; and in the United Kingdom, UTIs are diagnosed in 11.3 percent of girls and 3.6 percent of boys by 16 years of age.
Etiology
The normal urinary tract is sterile. Contamination by bowel flora may result in urinary infection if a virulent organism is involved or if the child is immunosuppressed. In neonates, infection may originate from other sources. Escherichia coli accounts for about 75 percent of all pathogens. Proteus is more common in boys (one study found that proteus caused 33 percent of UTI infections in boys one to 16 years of age, compared with 0 percent of UTI infections in girls of the same age). Obstructive anomalies are found in up to 4 percent and vesicoureteric reflux in 8 to 40 percent of children being evaluated for their first UTI. Although vesicoureteric reflux is a major risk factor for adverse outcome, other factors, some of which have not yet been identified, are also important.
Family history: Vesicoureteric reflux runs in families. In one review article, the incidence of reflux in siblings ranged from 26 percent (a cohort of asymptomatic siblings) to 86 percent (siblings with a history of UTI) compared with a rate of less than 1 percent in the general population. Although some gene variants seem more common in children who have renal damage, no clear link has yet been established between specific genes and an adverse outcome. Local or systemic immune problems are also likely to be factors in the development of UTI.
Prognosis
Recurrence: A study in the United Kingdom found that 78 percent of girls and 71 percent of boys presenting with UTI within the first year of life experienced recurrence, and that 45 percent of girls and 39 percent of boys presenting after their first year of life developed further infections.
Vesicoureteric reflux: In a longitudinal study, 84 percent of children (572 children with UTI and vesicoureteric reflux) had spontaneous resolution during medical follow-up at five to 15 years of age.
Renal parenchymal defects: A systematic review of imaging in childhood UTI suggested that renal parenchymal defects (assessed with intravenous pyelogram or dimercaptosuccinic acid [DMSA] scan) occurs in 5 to 15 percent of children within one to two years of their first diagnosed UTI. Between 32 and 70 percent of these parenchymal defects were noted at the time of initial assessment, suggesting a high level of preexisting scarring, perhaps caused by previously unrecognized infection. This percentage did not substantially change, despite an increasing referral rate, during the three years studied. One meta-analysis of 12 cohort studies (537 children admitted to hospital for UTI, 1,062 kidneys) found that 36 percent of all kidneys had parenchymal defects on DMSA scintigraphy, and that 59 percent of children with vesicoureteric reflux on micturating cystourethrography had at least one scarred kidney (pooled positive likelihood ratio = 1.96; 95% confidence interval [CI], 1.51 to 2.54; pooled negative likelihood ratio = 0.71; 95% CI, 0.58 to 0.85). However, there was evidence of heterogeneity in likelihood ratios among studies. The authors concluded that vesicoureteric reflux is a weak predictor of renal damage in children admitted to the hospital. A retrospective population-based study in the United Kingdom suggested that 4.3 percent of boys and 4.7 percent of girls develop parenchymal defects (assessed using DMSA scans after their first referral for UTI).
New or progressive renal parenchymal defects and recurrent UTI: The systematic review reported on four studies that provided at least two years' follow-up. New renal parenchymal defects developed in 1.6 to 23 percent of children, and existing renal parenchymal defects progressed in 6 to 34 percent of children. It is unclear whether figures for new parenchymal defects included any children without previous scarring. The highest rates of renal parenchymal defects were associated with the highest rates of recurrent UTI. A further study showed that in children five years or older, abnormal DMSA scans were noted in 64 out of 118 children (55 percent) presenting with recurrent UTI, whereas 7 out of 44 (15 percent) who presented with a first UTI had renal parenchymal defects (odds ratio for recurrences causing renal parenchymal defects = 6.3; 95% CI, 2.6 to 15.2).
However, recurrent UTI may be less important as a risk factor for renal parenchymal defects in older children. One study showed that in children with initially normal scans at three or four years of age, five out of 176 children (3 percent) who were three years of age at presentation and 0 out of 179 children (0 percent) who were four years of age at presentation had developed renal parenchymal defects two to 11 years later. Of those children who developed renal parenchymal defects, four out of five (80 percent) had a definite history of recurrent UTI, with at least three episodes in all cases (odds ratio for recurrences causing renal parenchymal defects = 11.5; 95% CI, 1.3 to 106.1). Another study (287 children with severe vesicoureteric reflux treated either medically or surgically for any UTI) used serial DMSA scintigraphy to evaluate the risk of renal parenchymal defects over five years. It found that children younger than two years were at a greater risk of renal parenchymal defects than older children, regardless of treatment for the infection (deterioration in DMSA scan over five years: 21 out of 86 [24 percent] for younger children versus 27 out of 201 [13 percent] for older children; relative risk = 1.82; 95% CI, 1.09 to 3.03).
It is likely that children who present when older and have renal parenchymal defects have had at least one previous UTI that was undiagnosed. Many children seem to lose their susceptibility to renal damage with age.
Consequences for longer term: One long-term follow-up study in the United Kingdom found that children with renal parenchymal defects and vesicoureteric reflux at presentation, or with just one of these followed by documented UTI, were associated with an increased risk of progressive renal damage compared with children presenting without these features (relative risk of progressive renal damage = 17; 95% CI, 2.5 to 118). Persistent renal parenchymal defects may be associated with future complications, such as poor renal growth, recurrent adult pyelonephritis, impaired glomerular function, early hypertension, and end-stage renal failure. A combination of recurrent UTI, severe vesicoureteric reflux, and the presence of renal parenchymal defects at first presentation is associated with the worst prognosis.

