A 44-year-old woman was admitted to the hospital for severe pain localized to her lower extremities. She had a history of diabetes mellitus and end-stage renal disease requiring hemodialysis. On the sixth day of hospitalization, she developed tender, flat, hyperpigmented, violaceous plaques with irregular borders on her buttocks and thighs (Figure 1). Laboratory results included the following: ionized calcium level of 4.28 mg per dL (1.07 mmol per L), phosphorus level of 5.9 mg per dL (1.91 mmol per L), parathyroid hormone level of 483 pg per mL (483 ng per L), protein C activity of 41 percent, and protein S activity of 325 percent. The plaques increased in size, followed by blistering and sloughing of the skin (Figure 2). Skin biopsy showed focal necrosis of the deep dermis, microthrombi, and calcification of the vessel walls.
Figure 1.
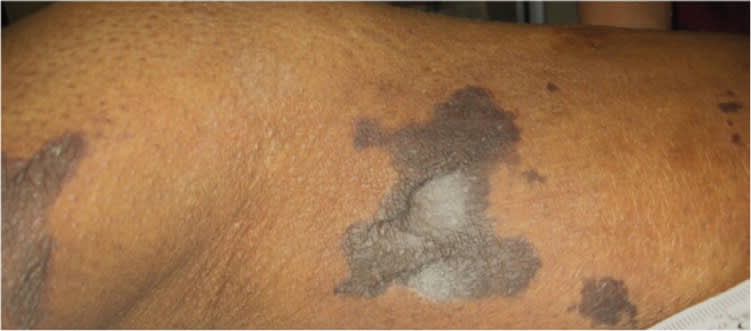
Figure 2.
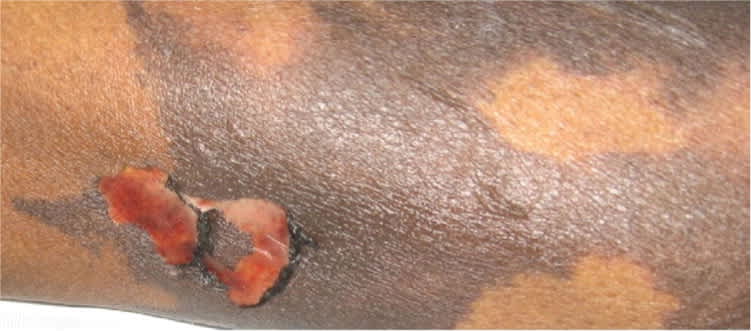
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Calcific uremic arteriolopathy.
B. Necrotizing vasculitis.
C. Nephrogenic systemic fibrosis.
D. Peripheral arterial disease.
E. Skin necrosis from warfarin (Coumadin) therapy.
Discussion
The correct answer is A: calcific uremic arteriolopathy. Calcific uremic arteriolopathy, also known as calciphylaxis, is characterized by small vessel calcification and cutaneous necrosis. The condition occurs primarily in patients with end-stage renal disease who are on dialysis or who have recently received a renal transplant. It has also been reported in patients with primary hyperparathyroidism, alcoholic cirrhosis, or breast carcinoma treated with chemotherapy.1 The prevalence is approximately 4 percent among patients on dialysis.2 The mortality rate can be as high as 80 percent1,3 and is often due to secondary infection of ulcers and sepsis.
The pathogenesis of calcific uremic arteriolopathy is unclear, but hyperparathyroidism, vitamin D supplementation, hyperphosphatemia, hypercalcemia, and abnormalities of coagulation may be related.4 Clinically, calcific uremic arteriolopathy is suggested by painful skin lesions that progress quickly into necrotic, nonhealing ulcers. There are no specific laboratory tests, but laboratory findings, especially increased levels of calcium, phosphorus, and parathyroid hormone, in the presence of suspicious lesions may suggest the diagnosis. Histopathology reveals calcification of the vessel walls and sebaceous gland necrosis. Treatment includes correcting calcium and phosphorus levels,5 hemodialysis, wound debridement, hyperbaric oxygen therapy, and antibiotics. Parathyroidectomy may be required if hyperparathyroidism does not respond to medical management.
Necrotizing vasculitis occurs in patients with collagen vascular disease, inflammatory bowel disease, or malignancy. The lesions are usually pruritic and painful and are often preceded by fever, arthralgia, and malaise.
Nephrogenic systemic fibrosis occurs in patients with underlying renal disease. The lesions are typically erythematous papules that coalesce into erythematous to brawny plaques. The involved skin becomes thickened and woody in texture. Skin biopsy is essential for diagnosis.
Peripheral arterial disease can cause ulcers and necrosis. Peripheral pulses are absent, and bilateral necrosis is possible. Ulcers typically occur on the toes, heels, and anterior shin, whereas the trunk and upper extremities usually are not involved.
Skin necrosis from warfarin therapy usually develops in a distinct pattern three to six days after therapy is initiated and regresses after the therapy is discontinued. Necrosis occurs in areas with significant underlying subcutaneous fat tissue. The rash is painful, and petechiae develop within 24 to 48 hours, progress to hemorrhagic bullae, and quickly change into full-blown necrotic eschar.
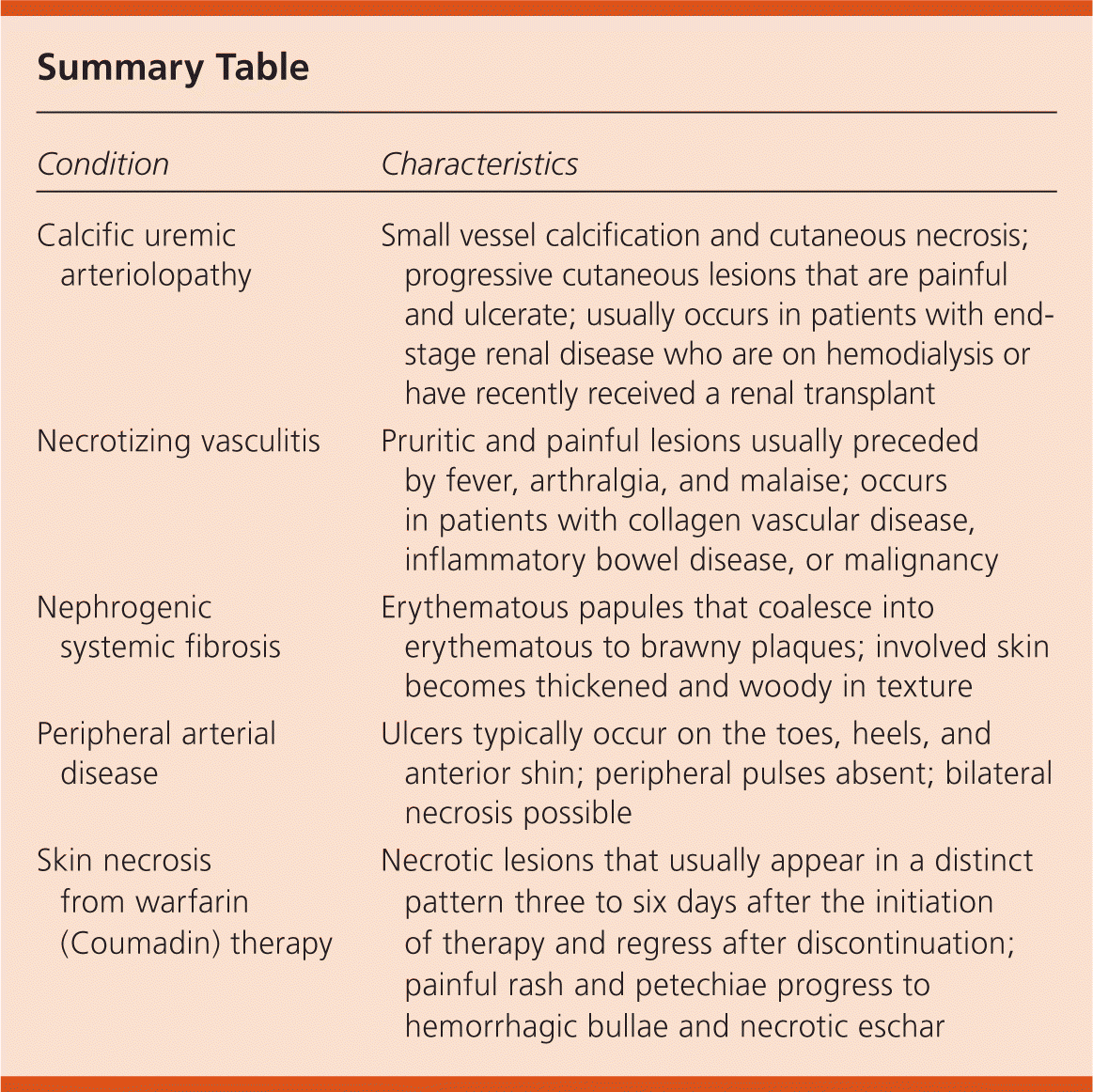
Summary Table
| Condition | Characteristics |
|---|---|
| Calcific uremic arteriolopathy | Small vessel calcification and cutaneous necrosis; progressive cutaneous lesions that are painful and ulcerate; usually occurs in patients with end-stage renal disease who are on hemodialysis or have recently received a renal transplant |
| Necrotizing vasculitis | Pruritic and painful lesions usually preceded by fever, arthralgia, and malaise; occurs in patients with collagen vascular disease, inflammatory bowel disease, or malignancy |
| Nephrogenic systemic fibrosis | Erythematous papules that coalesce into erythematous to brawny plaques; involved skin becomes thickened and woody in texture |
| Peripheral arterial disease | Ulcers typically occur on the toes, heels, and anterior shin; peripheral pulses absent; bilateral necrosis possible |
| Skin necrosis from warfarin (Coumadin) therapy | Necrotic lesions that usually appear in a distinct pattern three to six days after the initiation of therapy and regress after discontinuation; painful rash and petechiae progress to hemorrhagic bullae and necrotic eschar |

