A 15-year-old boy presented with a diffuse rash that began on his lower extremities and rapidly progressed over the previous two weeks to his upper extremities, chest, and back. A basic metabolic panel and complete blood count were unremarkable. Topical steroids were ineffective. The rash was associated with mild muscle aches, joint pain, and one day of emesis.
On physical examination, the patient was nontoxic and had no fever. Skin examination revealed multiple, diffuse, nonblanching purpura scattered on the distal lower extremities, lower abdomen, lower back, and distal upper extremities (Figure 1). In addition, there were several areas of coalescence with a few scattered vesicles that varied in level of progression (Figure 2). Urine dipstick testing was unremarkable.
Figure 1.
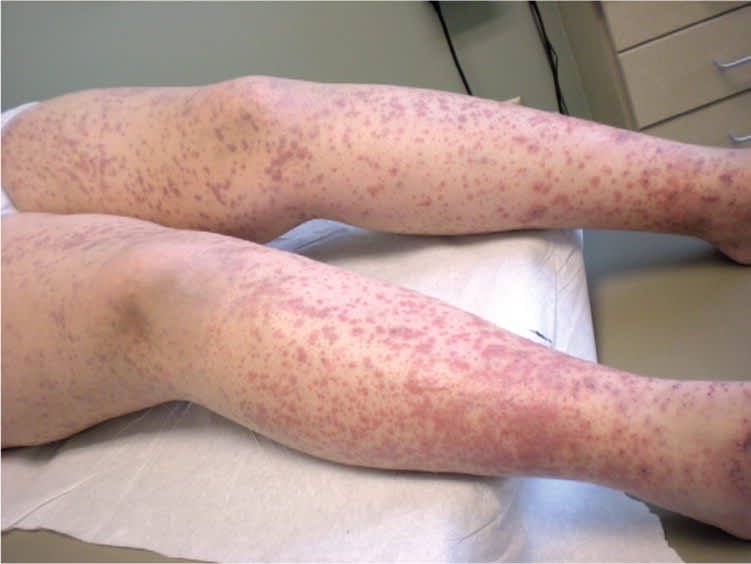
Figure 2.
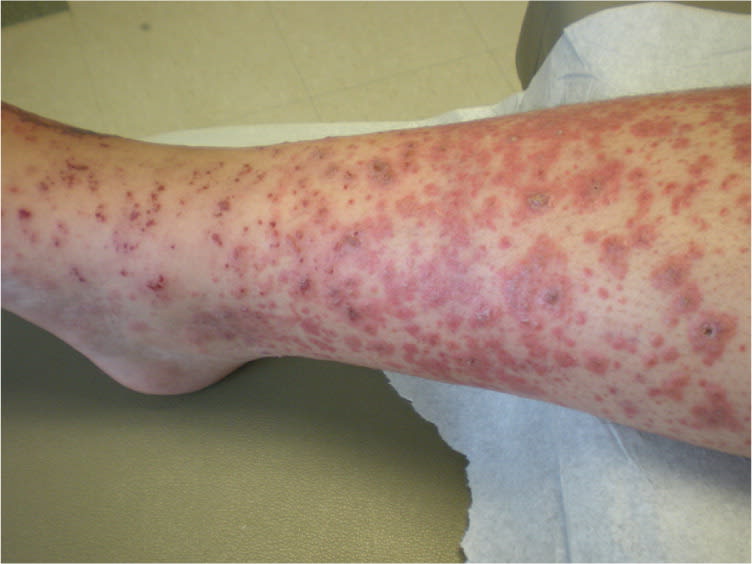
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Contact dermatitis.
B. Henoch-Schönlein purpura.
C. Idiopathic thrombocytopenic purpura.
D. Meningococcemia.
E. Rocky Mountain spotted fever.
Discussion
The answer is B: Henoch-Schönlein purpura. Henoch-Schönlein purpura is the most common systemic vasculitis of childhood.1 The disease is characterized by a tetrad of clinical manifestations, including palpable purpura without thrombocytopenia or coagulopathy, arthritis and arthralgias, abdominal pain, and renal disease. The rash often begins with erythematous, macular, or urticarial wheals that coalesce into ecchymosis, petechiae, and palpable purpura.2 The purpura are typically located on pressure-dependent areas, often in a symmetric distribution.
Henoch-Schönlein purpura is less common in adults, often occurring between three and 15 years of age. The condition appears primarily in the fall, winter, and spring, but rarely in the summer. Approximately 50 percent of cases are preceded by an upper respiratory infection, particularly streptococcal pharyngitis3; however, the underlying cause is unknown. Henoch-Schönlein purpura is an immune complex–mediated vasculitis associated with immunoglobulin A (IgA) deposition in small vessels. The diagnosis is clinical but may be confirmed with skin or renal biopsies, which demonstrate leukocytoclastic vasculitis with a predominance of IgA deposition. The clinical manifestations may develop over days to weeks and may vary in order of presentation.
Henoch-Schönlein purpura is usually self-limited. Treatment includes supportive care and symptomatic therapy for arthralgias, abdominal pain, and skin irritation. Acetaminophen and nonsteroidal anti-inf lammatory drugs are the mainstays of treatment. Hospitalization may be required in patients who cannot maintain hydration and in those with severe abdominal pain, gastrointestinal bleeding, mental status changes, or renal disease. Early, aggressive oral prednisone is recommended for patients with severe renal involvement.1
Contact dermatitis is characterized by pruritic papules and vesicles on an erythematous base that typically do not coalesce.4 A causative exposure typically can be identified, such as poison ivy or nickel, and distribution of the rash is usually related to exposure.
Idiopathic thrombocytopenic purpura is characterized by nonpalpable petechiae, which occur mostly in areas that are subject to pressure, such as the lower extremities, belt line, and buttocks.5 The lesions do not coalesce. The condition is associated with thrombocytopenia and coagulopathy.
Meningococcemia is a severe systemic infection that usually causes fever and malaise. The condition can occur at any age.4 The rash appears as petechiae, purpura, and ecchymosis. Patients often have neurologic symptoms (e.g., mental status changes) at presentation.
Rocky Mountain spotted fever is a rickettsial infection that appears as a classic blanching, maculopapular eruption on the wrists and ankles, then spreads centripetally to involve the trunk and extremities.6
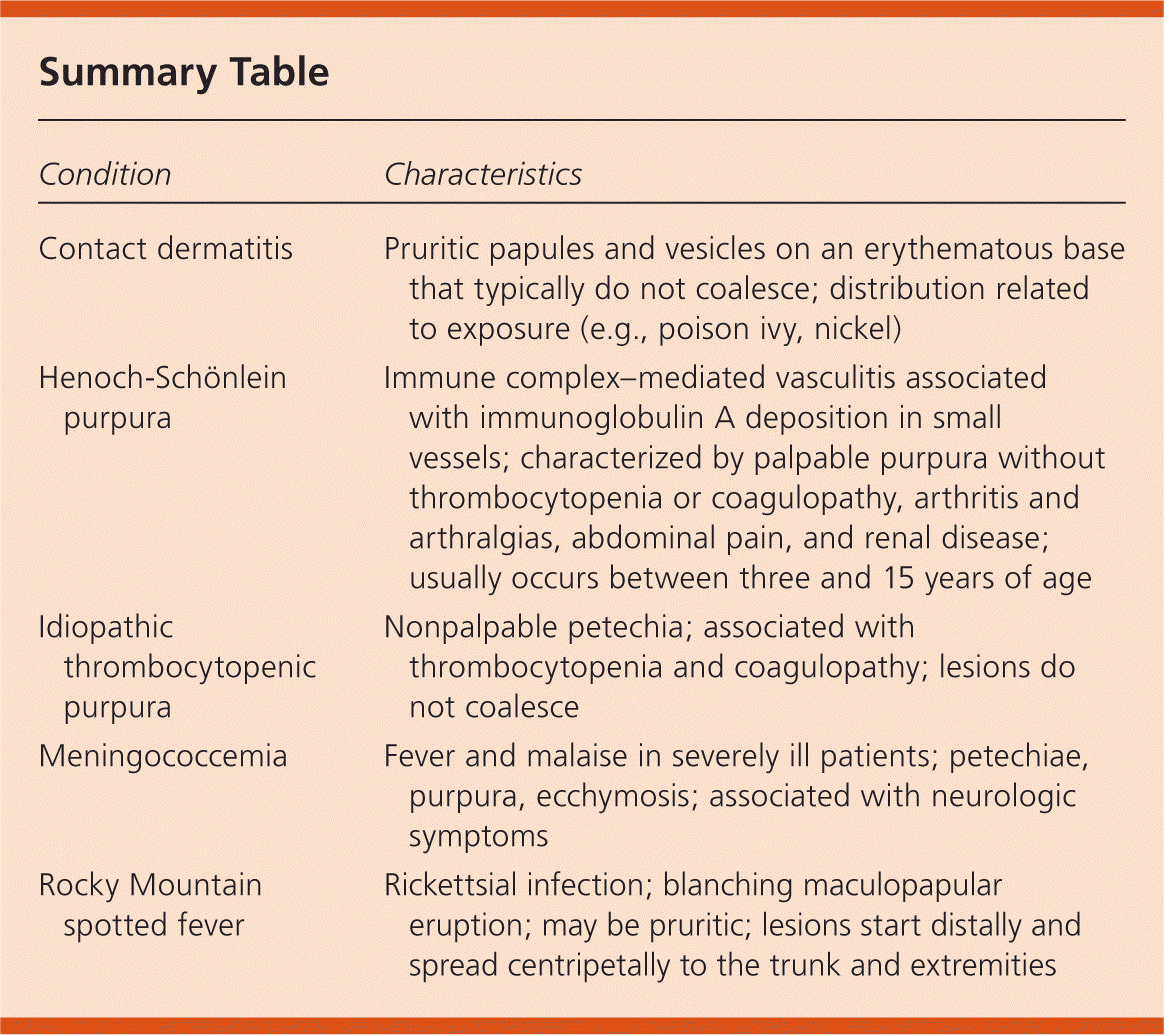
Summary Table
| Condition | Characteristics |
|---|---|
| Contact dermatitis | Pruritic papules and vesicles on an erythematous base that typically do not coalesce; distribution related to exposure (e.g., poison ivy, nickel) |
| Henoch-Schönlein purpura | Immune complex–mediated vasculitis associated with immunoglobulin A deposition in small vessels; characterized by palpable purpura without thrombocytopenia or coagulopathy, arthritis and arthralgias, abdominal pain, and renal disease; usually occurs between three and 15 years of age |
| Idiopathic thrombocytopenic purpura | Nonpalpable petechia; associated with thrombocytopenia and coagulopathy; lesions do not coalesce |
| Meningococcemia | Fever and malaise in severely ill patients; petechiae, purpura, ecchymosis; associated with neurologic symptoms |
| Rocky Mountain spotted fever | Rickettsial infection; blanching maculopapular eruption; may be pruritic; lesions start distally and spread centripetally to the trunk and extremities |

