The goals of the well-child examination in school-aged children (kindergarten through early adolescence) are promoting health, detecting disease, and counseling to prevent injury and future health problems. A complete history should address any concerns from the patient and family and screen for lifestyle habits, including diet, physical activity, daily screen time (e.g., television, computer, video games), hours of sleep per night, dental care, and safety habits. School performance can be used for developmental surveillance. A full physical examination should be performed; however, the U.S. Preventive Services Task Force recommends against routine scoliosis screening and testicular examination. Children should be screened for obesity, which is defined as a body mass index at or above the 95th percentile for age and sex, and resources for comprehensive, intensive behavioral interventions should be provided to children with obesity. Although the evidence is mixed regarding screening for hypertension before 18 years of age, many experts recommend checking blood pressure annually beginning at three years of age. The American Academy of Pediatrics recommends vision and hearing screening annually or every two years in school-aged children. There is insufficient evidence to recommend screening for dyslipidemia in children of any age, or screening for depression before 12 years of age. All children should receive at least 400 IU of vitamin D daily, with higher doses indicated in children with vitamin D deficiency. Children who live in areas with inadequate fluoride in the water (less than 0.6 ppm) should receive a daily fluoride supplement. Age-appropriate immunizations should be given, as well as any missed immunizations.
The goals of the well-child examination in school-aged children (kindergarten through early adolescence) are promoting health, detecting disease, and counseling to prevent injury and future health problems. It is also an opportunity for family physicians to stay connected with children and their parents and to build a medical home for families. In a recent survey of pediatricians, 85 percent of respondents reported that lack of time is the main limitation to providing preventive care.1 Because of these time constraints, health maintenance visits should focus on screening and counseling interventions that are evidence-based and that have a major impact on morbidity. This article, part I of a two-part series, focuses on history, physical examination, screening, and immunization recommendations for health maintenance in school-aged children. Part II discusses counseling recommendations.2
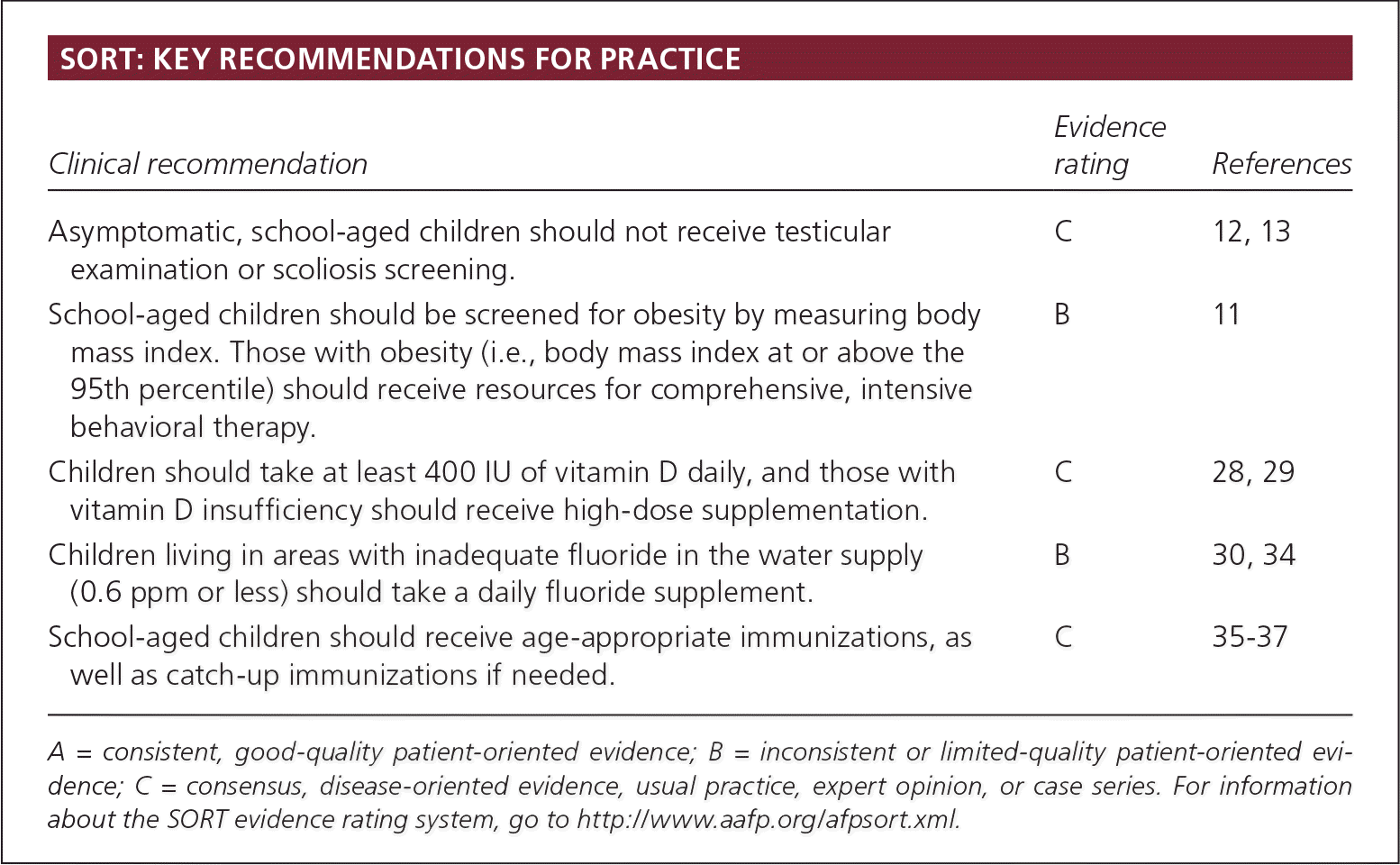
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Asymptomatic, school-aged children should not receive testicular examination or scoliosis screening. | C | 12, 13 |
| School-aged children should be screened for obesity by measuring body mass index. Those with obesity (i.e., body mass index at or above the 95th percentile) should receive resources for comprehensive, intensive behavioral therapy. | B | 11 |
| Children should take at least 400 IU of vitamin D daily, and those with vitamin D insufficiency should receive high-dose supplementation. | C | 28, 29 |
| Children living in areas with inadequate fluoride in the water supply (0.6 ppm or less) should take a daily fluoride supplement. | B | 30, 34 |
| School-aged children should receive age-appropriate immunizations, as well as catch-up immunizations if needed. | C | 35–37 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
History
During a well-child examination of a school-aged child, the history should include screening questions and address any concerns raised by the child or parents. The patient's medical and surgical history, medications, allergies, and family history should be briefly reviewed. Social history can be particularly important in this age group. Living situation and lifestyle habits, including diet, physical activity, daily screen time (e.g., television, computer, video games), hours of sleep per night, and dental care practices should be assessed. Physicians should also inquire about safety habits, such as use of protective sports equipment (e.g., helmets), seat belt use, and the presence of firearms in the home.
Because there are many topics to cover during a well-child visit, physicians should consider giving a questionnaire to the family to complete before the visit. By screening for topics most relevant to the specific child, the physician can maximize the impact of the time spent with the patient.
Developmental Surveillance
Although formal developmental screening is not recommended beyond the toddler years, family physicians can monitor continued development by inquiring about school performance.3 If the patient is struggling in school, referral for formal testing for learning disabilities should be considered. Symptoms of attention-deficit/hyperactivity disorder often present in school-aged children as the complexity of schoolwork increases. Problems with vision or hearing may impact success in the classroom. School performance may also be affected if the child is experiencing stress at home or in school.4
Physical Examination
A full physical examination should be performed during any health maintenance visit, and is required in a well-child examination for insurance billing. However, one study has shown that physical examination in an asymptomatic, school-aged child will find a new abnormality in less than 4 percent of patients, and most of these abnormalities are not clinically significant.5 Few specific examination elements have been validated as having a positive or negative health effect. Because more than 1 million abused children are identified annually in the United States, physicians should remain alert for signs of abuse.6,7
Screening Tests
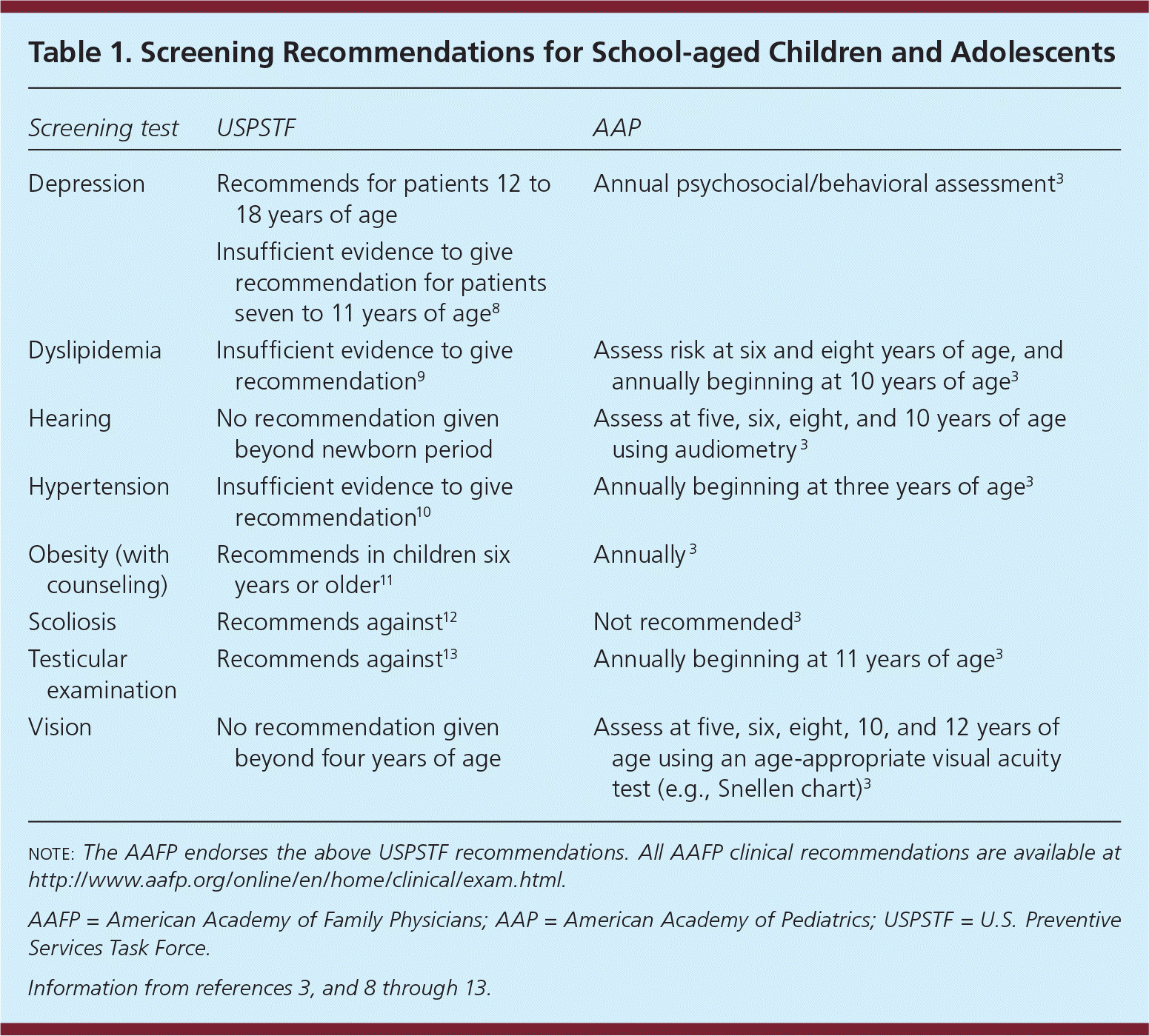
Screening recommendations for school-aged children from the American Academy of Pediatrics (AAP) and the U.S. Preventive Services Task Force (USPSTF) are listed in Table 1.3,8–13 The USPSTF recommends against scoliosis screening and testicular examination in asymptomatic patients because these tests have been found to be more harmful than beneficial in these patients.12,13
Table 1. Screening Recommendations for School-aged Children and Adolescents
| Screening test | USPSTF | AAP |
|---|---|---|
| Depression | Recommends for patients 12 to 18 years of age | Annual psychosocial/behavioral assessment3 |
| Insufficient evidence to give recommendation for patients seven to 11 years of age 8 | ||
| Dyslipidemia | Insufficient evidence to give recommendation9 | Assess risk at six and eight years of age, and annually beginning at 10 years of age3 |
| Hearing | No recommendation given beyond newborn period | Assess at five, six, eight, and 10 years of age using audiometry 3 |
| Hypertension | Insufficient evidence to give recommendation10 | Annually beginning at three years of age3 |
| Obesity (with counseling) | Recommends in children six years or older11 | Annually3 |
| Scoliosis | Recommends against12 | Not recommended3 |
| Testicular examination | Recommends against13 | Annually beginning at 11 years of age3 |
| Vision | No recommendation given beyond four years of age | Assess at five, six, eight, 10, and 12 years of age using an age-appropriate visual acuity test (e.g., Snellen chart)3 |
note: The AAFP endorses the above USPSTF recommendations. All AAFP clinical recommendations are available at https://www.aafp.org/patient-care/clinical-recommendations/a-z.html.
AAFP = American Academy of Family Physicians; AAP = American Academy of Pediatrics; USPSTF = U.S. Preventive Services Task Force.
OVERWEIGHT AND OBESITY
Rates of childhood overweight and obesity have been steadily increasing over the past three decades. The USPSTF recommends measuring body mass index (BMI) in children beginning at six years of age.11 Overweight is defined as a BMI at or above the 85th percentile for age and sex, and obesity as a BMI at or above the 95th percentile.14 In the United States, 17 percent of children are considered overweight or obese.15 Children with obesity should be offered resources for comprehensive, intensive behavioral therapy.11
HYPERTENSION
Routine blood pressure measurement beginning at three years of age has been a longstanding recommendation from the AAP.3 Blood pressure standards for children are based on sex, age, and height. The U.S. Department of Health and Human Services provides tables of these standards at http://www.nhlbi.nih.gov/guidelines/hypertension/child_tbl.htm. Normal blood pressure in children is defined as that lower than the 90th percentile, prehypertension as the 90th to 95th percentile, and hypertension as at or above the 95th percentile.16 The National High Blood Pressure Education Program has published recommendations for the management and workup in children and adolescents with blood pressure abnormalities.16 The American Academy of Family Physicians (AAFP) has found insufficient evidence to recommend universal blood pressure screening before 18 years of age.10
HEARING AND VISION
The AAP recommends routine vision testing at five, six, eight, 10, and 12 years of age using an age-appropriate visual acuity test, such as the Snellen chart, with a risk assessment at other well-child visits.3 Referral for formal optometry evaluation is recommended for children with visual acuity less than 20/40. The AAP does not have a formal policy on hearing screening, but the Bright Futures Steering Committee recommends screening for hearing loss at five, six, eight, and 10 years of age using audiometry, with a risk assessment at other well-child visits.3 Although the USPSTF recommends vision screening for children younger than five years17 and hearing screening for infants,18 no recommendations are provided for older children.
DYSLIPIDEMIA
The AAP recommends assessing for risk of dyslipidemia at six and eight years of age, and annually beginning at 10 years of age.3 The AAFP and the USPSTF have found insufficient evidence to support routine screening for dyslipidemia in children.9,19 There is good evidence that children with lipid disorders are at risk of continued problems in adulthood. However, one study has shown that only 50 percent of these children will have abnormal cholesterol levels in adulthood, and there is no evidence that diagnosis and treatment in childhood improves long-term primary outcomes.20
DEPRESSION
Major depressive disorder can be a debilitating mental health condition in children and adolescents. The prevalence of current or recent depression is 3 percent in children and increases to 6 percent in adolescents.21 Children and adolescents with major depressive disorder have increased risk of poor school performance and social functioning, early pregnancy, physical illness, and substance abuse.22,23 There is good evidence to support screening adolescents 12 to 18 years of age for depression when systems are in place to ensure accurate diagnosis, psychotherapy, and follow-up.8 Less data are available regarding children seven to 11 years of age, and the USPSTF has concluded that there is insufficient evidence to recommend for or against routine depression screening in this age group.8 Younger children may not be able to communicate a depressed mood; therefore, physicians should consider a depression diagnosis in children presenting with vague somatic symptoms, irritability, or impaired attention.24 The Children's Depression Inventory and Reynolds Child Depression Scale are appropriate screening tools for school-aged children.25,26
Supplements
VITAMIN D
Inadequate vitamin D levels have been associated with a wide range of conditions, such as type 1 diabetes mellitus and osteoporosis. 27 Studies have shown that up to 50 percent of children are vitamin D deficient, and many more have insufficient levels.25 The AAP recommends 400 IU of vitamin D daily for all children.28 However, many experts believe that this dose is inadequate, particularly for those living in northern climates or who have little sun exposure. In children older than one year whose vitamin D levels are insufficient or deficient, experts recommend supplementation with 5,000 IU of vitamin D daily until levels have normalized.29 There are no clear guidelines for screening for vitamin D deficiency in children. If a child is screened, the most appropriate test is 25-hydroxyvitamin D. A vitamin D level greater than 30 ng per mL (74.88 nmol per L) is considered adequate.
FLUORIDE
Children six months to 16 years of age living in areas with inadequate fluoride in the water supply (0.6 ppm or less) should be counseled on fluoride supplementation (Table 230–33 ) to prevent dental caries.30,34
Table 2. Recommended Dietary Fluoride Supplementation in School-aged Children and Adolescents
Immunizations
Immunizations remain a cornerstone of health maintenance, and the AAFP strongly recommends immunizing children and adolescents. 35 The Centers for Disease Control and Prevention's Advisory Committee on Immunization Practices, in conjunction with the AAFP and AAP, has released the 2011 Child and Adolescent Immunization Schedules.36
There are two sets of immunizations recommended for school-aged children. The first set should be administered at four to six years of age, and the second at 11 or 12 years of age. In addition to these primary vaccines, the influenza virus vaccine is recommended annually for all children older than six months. Certain high-risk groups may need additional vaccines.36 At every well-child visit, the immunization record should be reviewed to ensure that catch-up immunizations are not needed. 37
Nationally, there is a high level of vaccine completion for the four- to six-year-old vaccines, with most states achieving an immunization rate of greater than 95 percent.38 Completion rates for vaccines recommended in early adolescence are significantly less, with approximately 40 percent of patients receiving the tetanus toxoid, reduced diphtheria toxoid, and acellular pertussis (Tdap) vaccine and meningococcal vaccine, and less than 20 percent completing the human papillomavirus vaccine series.39 There is significant regional and local variation in immunization rates, and physicians should adopt strategies to increase immunization completion in their patients.


