Cardiovascular disease (CVD) is the leading cause of death in adults, accounting for one out of every 2.8 deaths in the United States.1 Daily use of low-dose (75 to 325 mg) aspirin as a secondary preventive measure reduces all-cause mortality by 18 percent, and subsequent myocardial infarctions by 30 percent in persons with known CVD.2,3 Aspirin use prevents CVD by inhibiting cyclooxygenase, which blocks the formation of thromboxane A2 and thus disrupts platelet aggregation and prevents vasoconstriction.4 The American Heart Association recommends that daily aspirin be used indefinitely in all patients with known CVD, unless contraindicated, for secondary prevention.5
There is interest in and controversy over daily use of aspirin for primary prevention of CVD in persons who have yet to demonstrate clinical evidence of CVD. Several major randomized clinical trials and subsequent meta-analyses involving more than 96,000 participants have demonstrated that daily aspirin use in persons at moderate to high risk of CVD can reduce the risk of a first-time CVD event by at least 28 percent.6,7 However, recent studies have questioned whether the benefits of daily aspirin for primary cardioprevention outweigh the risks of gastrointestinal (GI) and intracerebral hemorrhage.8,9 In addition, a recent randomized controlled trial involving 39,876 relatively healthy women 45 years and older suggested that daily aspirin therapy may not decrease the risk of acute myocardial infarction in women, although there was a 17 percent decreased risk of stroke.10 Currently, two large, international randomized controlled trials (n > 10,000) are investigating the benefit of daily aspirin therapy for primary cardioprevention in select populations: the ASCEND trial (a study of cardiovascular events in diabetes) and the ASPREE trial (aspirin in reducing events in the elderly). Results from these trials should be available within the next five years.
After critically analyzing the evidence of potential benefits and harms of aspirin therapy, the U.S. Preventive Services Task Force (USPSTF) reaffirmed and clarified its position in 2009, concluding that aspirin is effective for primary CVD prevention.11 Aspirin should be recommended when benefits outweigh risks. The USPSTF found good evidence that aspirin use decreases myocardial infarctions in men 45 to 79 years of age, and strokes in women 55 to 79 years of age who are at increased risk of, but have not yet experienced, these events. Compared with its 2002 recommendation,6 the USPSTF's 2009 recommendation differentiates CVD risk by age group and sex, complicating physicians' task of determining patients' CVD risk. Physicians must now consider the 10-year myocardial infarction risk for men and 10-year stroke risk for women.
Aspirin therapy should be considered in men with a 10-year CVD risk of at least 4 percent in those 45 to 59 years of age, 9 percent in those 60 to 69 years of age, and 12 percent in those 70 to 79 years of age. Aspirin therapy should be considered in women with a 10-year stroke risk of at least 3 percent in those 50 to 59 years of age, 8 percent in those 60 to 69 years of age, and 11 percent in those 70 to 79 years of age. Several online calculators are available to help physicians determine these risks (Table 1). To assist physicians in better identifying patients who potentially would benefit from aspirin therapy, the American College of Preventive Medicine is studying the use of a patient-friendly decision table.
Table 1. Online Cardiovascular Risk Calculators
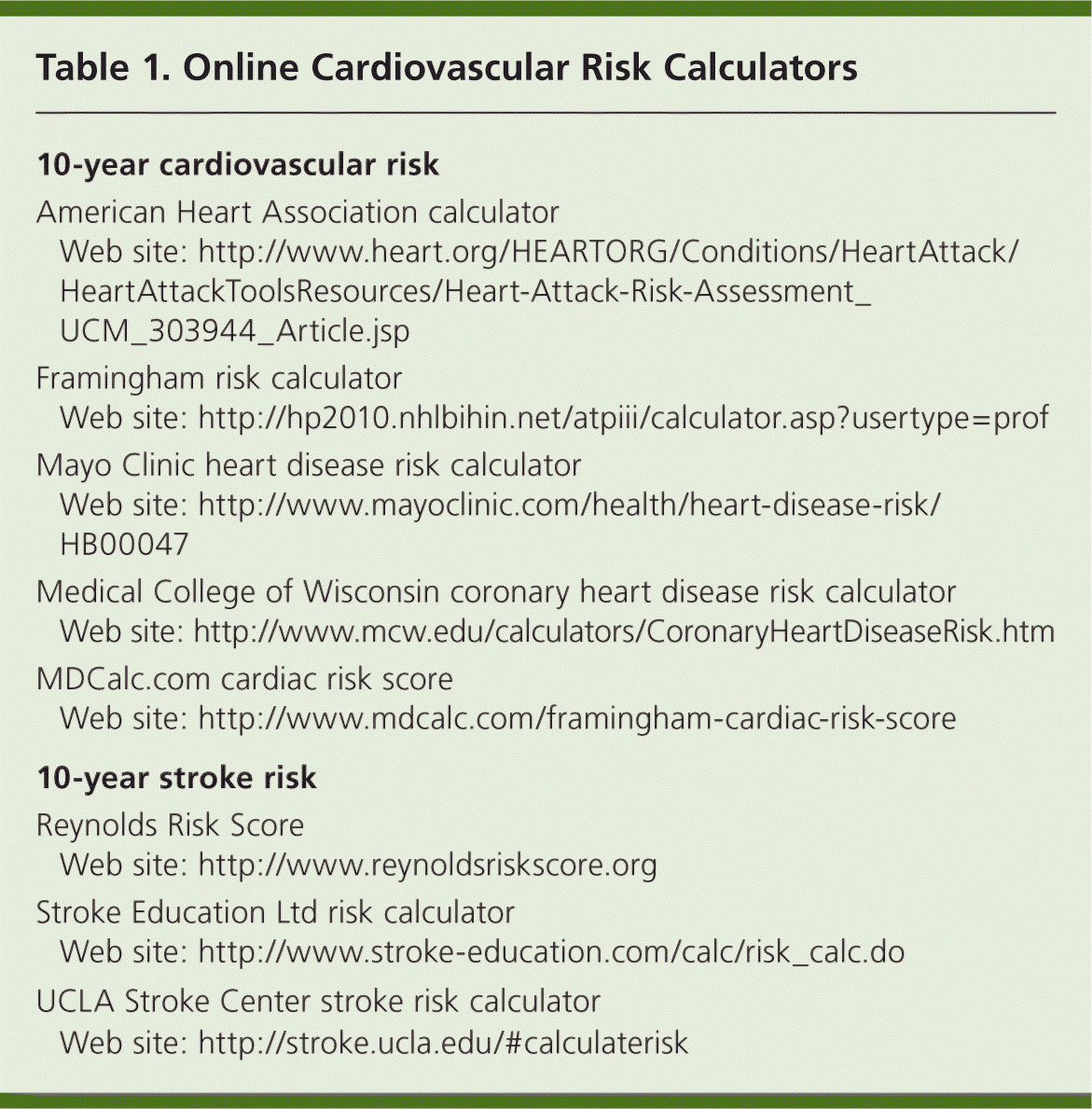
| 10-year cardiovascular risk | |
| American Heart Association calculator | |
| Web site: http://www.heart.org/HEARTORG/Conditions/HeartAttack/HeartAttackToolsResources/Heart-Attack-Risk-Assessment_UCM_303944_Article.jsp | |
| Framingham risk calculator | |
| Web site: http://hp2010.nhlbihin.net/atpiii/calculator.asp?usertype=prof | |
| Mayo Clinic heart disease risk calculator | |
| Web site: http://www.mayoclinic.com/health/heart-disease-risk/HB00047 | |
| Medical College of Wisconsin coronary heart disease risk calculator | |
| Web site: http://www.mcw.edu/calculators/CoronaryHeartDiseaseRisk.htm | |
| MDCalc.com cardiac risk score | |
| Web site: http://www.mdcalc.com/framingham-cardiac-risk-score | |
| 10-year stroke risk | |
| Reynolds Risk Score | |
| Web site: http://www.reynoldsriskscore.org | |
| Stroke Education Ltd risk calculator | |
| Web site: http://www.stroke-education.com/calc/risk_calc.do | |
| UCLA Stroke Center stroke risk calculator | |
| Web site: http://stroke.ucla.edu/#calculaterisk | |
When advising aspirin use, the USPSTF recommends considering the risk of GI bleeding. The most widely recognized adverse effect of aspirin therapy is a modestly increased risk of GI bleeding; 769 persons need to be treated with aspirin to cause one additional major bleeding episode annually.12 Aspirin-induced GI toxicity appears to be dose-dependent; higher aspirin doses increase the risk of bleeding.13 It appears that in most persons, low-dose aspirin (81 mg) is best. Increasing the dose to 325 mg does not increase the effectiveness, but does increase the risk of GI bleeding.14
Aspirin for primary cardioprevention should be avoided in persons who have had a GI or cerebral bleeding episode, and in those who are at risk of bleeding problems (e.g., bleeding disorder, severe liver disease, thrombocytopenia, concomitant anticoagulant therapy). For persons with an aspirin- induced bleeding ulcer, aspirin use in combination with a proton pump inhibitor may be safely restarted after the ulcer has healed.15 A randomized controlled trial found that in those taking low-dose aspirin who had GI bleeding, continuous aspirin therapy may increase the risk of recurrent GI bleeding, but potentially reduces cardiovascular and cerebrovascular mortality rates.16 Eradication of Helicobacter pylori decreases the risk of recurrent GI bleeding in those taking low-dose aspirin.15 Enteric-coated or buffered aspirin does not decrease the risk of GI toxicity.17 A list of absolute and relative contraindications to aspirin therapy is presented in Table 2.
Table 2. Contraindications to Aspirin Therapy

| Absolute contraindications |
| Active peptic ulcer |
| Aspirin allergy or intolerance |
| Bleeding disorders (e.g., hemophilia, von Willebrand disease) |
| History of recent gastrointestinal bleeding |
| History of recent intracranial bleeding |
| Renal failure |
| Severe liver disease |
| Thrombocytopenia |
| Relative contraindications |
| Age younger than 21 years (increased risk of Reye syndrome) |
| Concurrent use of anticoagulation therapy |
| Concurrent use of nonsteroidal anti-inflammatory drugs |
| Poorly controlled hypertension (risk of intracranial bleeding) |
As with any medication, the key to aspirin therapy for CVD prevention is appropriate use. A study evaluating 24 clinical preventive services considered effective by the USPSTF found that advising at-risk adults to consider taking daily aspirin was the most cost-effective preventive measure available for physicians.18 If 90 percent of those who should be taking aspirin were doing so, it is estimated that an additional 45,000 lives would be saved each year. Despite this benefit, less than one-half of those who should be taking aspirin regularly are actually taking it.19 Although not reported, there are also persons taking daily aspirin for primary cardioprevention in whom the benefit is negligible or the risk is high. These persons should be cautioned against this practice until the benefit outweighs the risk.
The factor most strongly associated with appropriate aspirin use is a conversation between the patient and physician.20 The National Committee for Quality Assurance has proposed that health plans measure their members' use of aspirin, as well as the extent to which physicians discuss aspirin use with their patients. Determining patients' CVD risk and discussing appropriate aspirin use with them should be a priority for all family physicians.

