A 49-year-old man presented with a growth in the middle of his chest that appeared about one year earlier. He became concerned when it started growing more rapidly over the previous six to eight months. It caused some discomfort, but was not acutely painful or pruritic. He did not recall any signs of inflammation, such as redness, warmth, or drainage, and stated that there were no other such lesions on his body. The patient history was unremarkable except for smoking one pack of cigarettes per day and drinking a six-pack of beer on the weekends. He was not taking any medications and had no allergies.
Physical examination revealed a 3.1-in (7.9-cm) lesion located in the upper epigastrium. It had neovascularization on the surface, was soft (but not fluctuant), was flesh colored, and was not movable (Figures 1 and 2).
Figure 1.
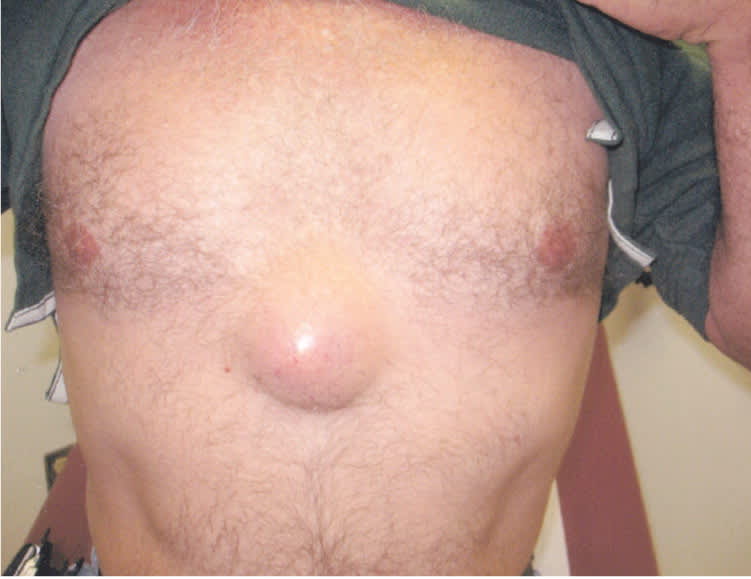
Figure 2.
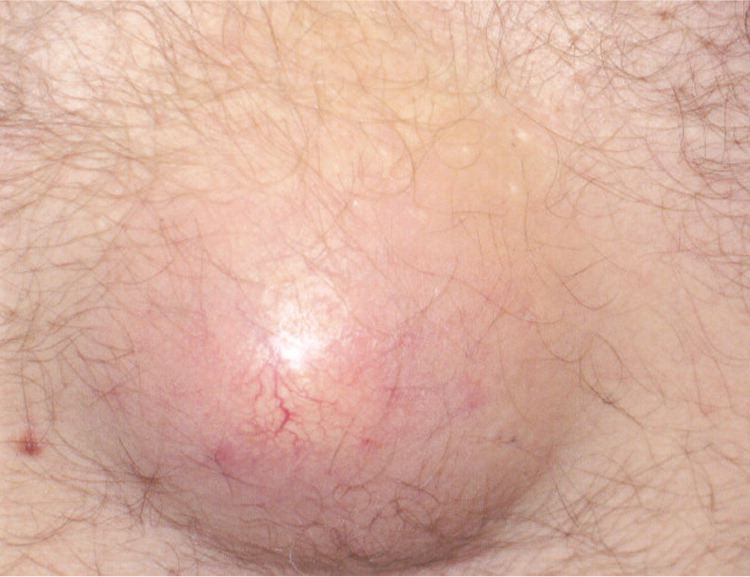
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Lipoma.
B. Neurofibroma.
C. Sarcoma.
D. Sebaceous cyst.
E. Skin metastasis.
Discussion
The correct answer is D: sebaceous cyst. Ultrasonography showed a solid mass with well-defined borders and interspersed areas of echogenicity, limited blood flow within the mass, and possible neoplasia. The lesion was surgically removed, and pathology confirmed it to be a large sebaceous cyst.
Sebaceous cysts are closed sacs in the epidermis that form when keratin blocks a sebaceous gland.1–3 Sebum buildup leads to a yellowish material that resembles cottage cheese and can have a foul odor when expressed. Sebaceous cysts can occur on any part of the body, most commonly on hairy areas. They can be caused by trauma, swollen hair follicles, or high testosterone levels, but are most often idiopathic. Some persons seem to be predisposed to them. The cyst begins as a soft nodule in the skin, which can enlarge over time. Many of these cysts resolve without treatment, but some become infected and need treatment such as medication, incision and drainage, excision, and heat. They can recur after surgical removal.
Lipomas are common, benign, fatty tumors that can appear on virtually any body surface.2,4 They typically occur in middle-aged adults. Lipomas are soft, flesh-colored, usually slow growing, rarely painful, and easily removed. They usually do not undergo malignant transformation to liposarcomas. Surgical excision is the treatment, and most lipomas will not recur after removal.
Neurofibromas are relatively uncommon and slow-growing tumors that arise from peripheral nerve sheaths.1,2,5 They most often occur in patients with neurofibromatosis, an inherited disorder usually heralded by café au lait spots. However, neurofibromas can occur sporadically in persons who do not have neurofibromatosis. As they enlarge, they may cause electric shock–like sensations. The treatment is surgical excision, which is often risky because of nerve involvement.
Sarcomas are uncommon, malignant, soft tissue tumors that originate from fat, muscle, subcutaneous or connective tissue, or bone.4,6 They can appear anywhere on the body, but most often on the arms and legs. Liposarcomas (malignant fatty tumors) often occur on the thigh, behind the knee, and on the retroperitoneum. Sarcomas are most common in persons between 50 and 65 years of age. They are resistant to chemotherapy. Treatment is surgical excision and sometimes radiation.
Skin metastases can occur from almost any type of primary tumor, but most commonly from melanoma and cancers of the breast, lung, colon, ovary, nasal sinus, and oropharynx.1,7 Metastases typically appear suddenly and are painful. They are firm, rubbery, and sometimes discolored. The chest is a common location, especially if the primary tumor is located in the lung. Treatment is of the primary cancer, but skin metastases can be diminished by laser, liquid nitrogen, excision, or intralesional chemotherapy.
Summary Table
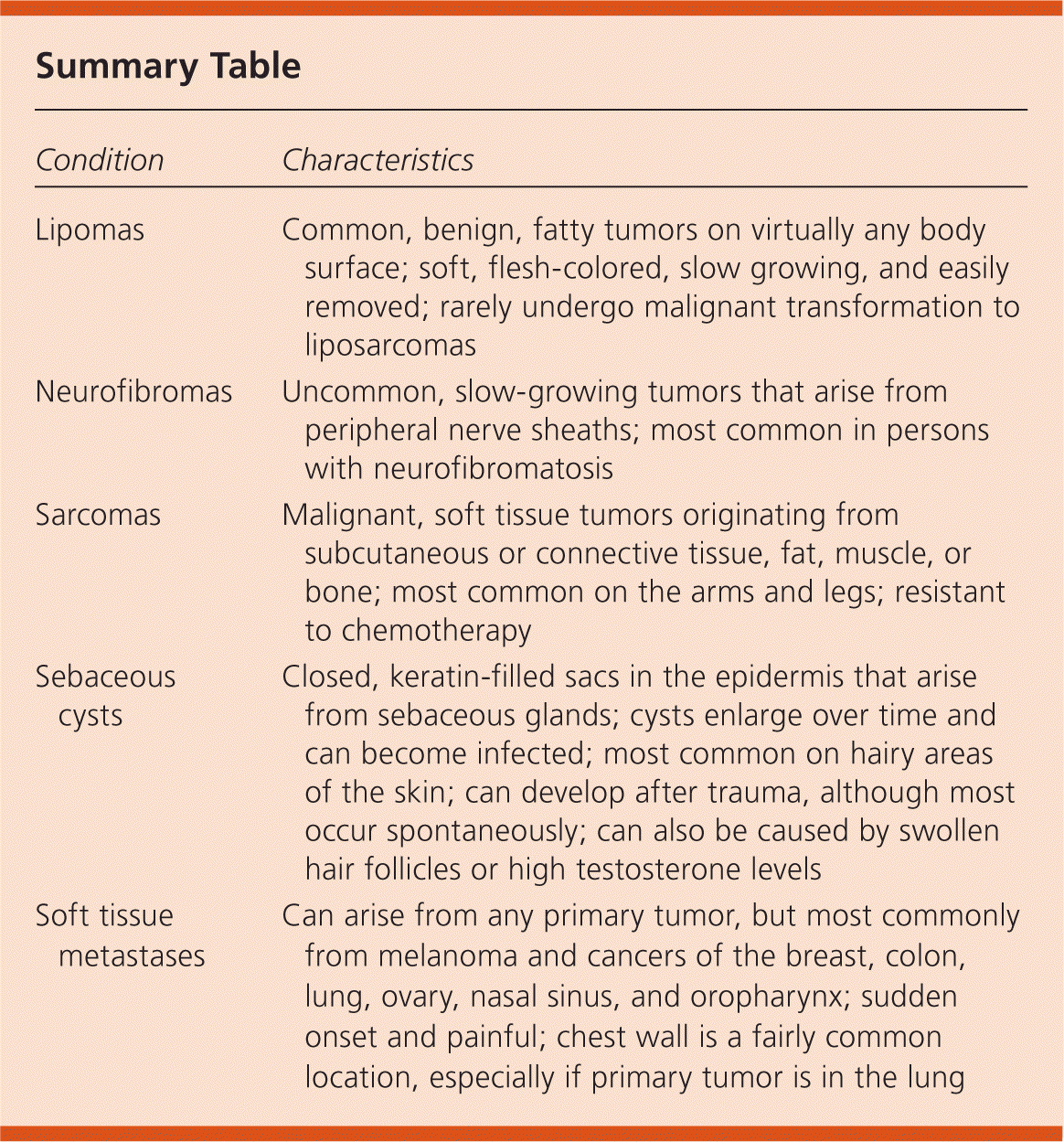
| Condition | Characteristics |
|---|---|
| Lipomas | Common, benign, fatty tumors on virtually any body surface; soft, flesh-colored, slow growing, and easily removed; rarely undergo malignant transformation to liposarcomas |
| Neurofibromas | Uncommon, slow-growing tumors that arise from peripheral nerve sheaths; most common in persons with neurofibromatosis |
| Sarcomas | Malignant, soft tissue tumors originating from subcutaneous or connective tissue, fat, muscle, or bone; most common on the arms and legs; resistant to chemotherapy |
| Sebaceous cysts | Closed, keratin-filled sacs in the epidermis that arise from sebaceous glands; cysts enlarge over time and can become infected; most common on hairy areas of the skin; can develop after trauma, although most occur spontaneously; can also be caused by swollen hair follicles or high testosterone levels |
| Soft tissue metastases | Can arise from any primary tumor, but most commonly from melanoma and cancers of the breast, colon, lung, ovary, nasal sinus, and oropharynx; sudden onset and painful; chest wall is a fairly common location, especially if primary tumor is in the lung |

