An 89-year-old woman presented with an ulcerated lesion on the vulva. It was very itchy, but not painful, and had been present for over one year with no significant change to the lesion or surrounding skin. There was no discharge from the lesion, and the patient did not report fever. She had not been sexually active for more than 15 years before the lesion appeared, and had only one partner before that. She had no relevant medical history. Examination revealed a 1 cm × 0.5 cm erythematous, ulcerated area on the left labia majora (Figures 1 and 2).
Figure 1.
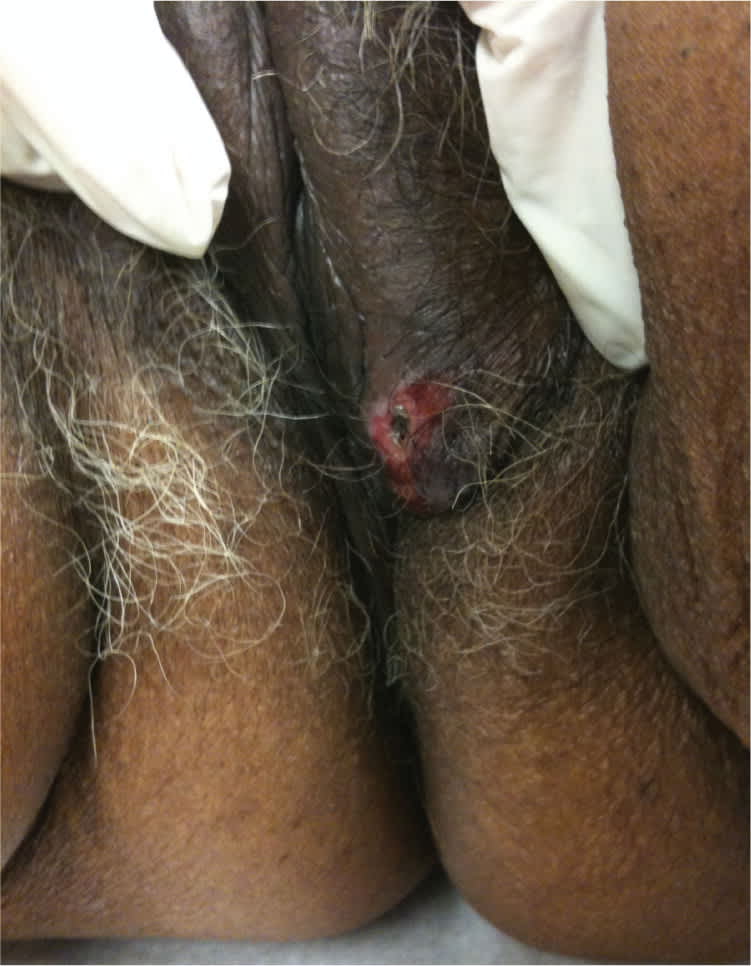
Figure 2.
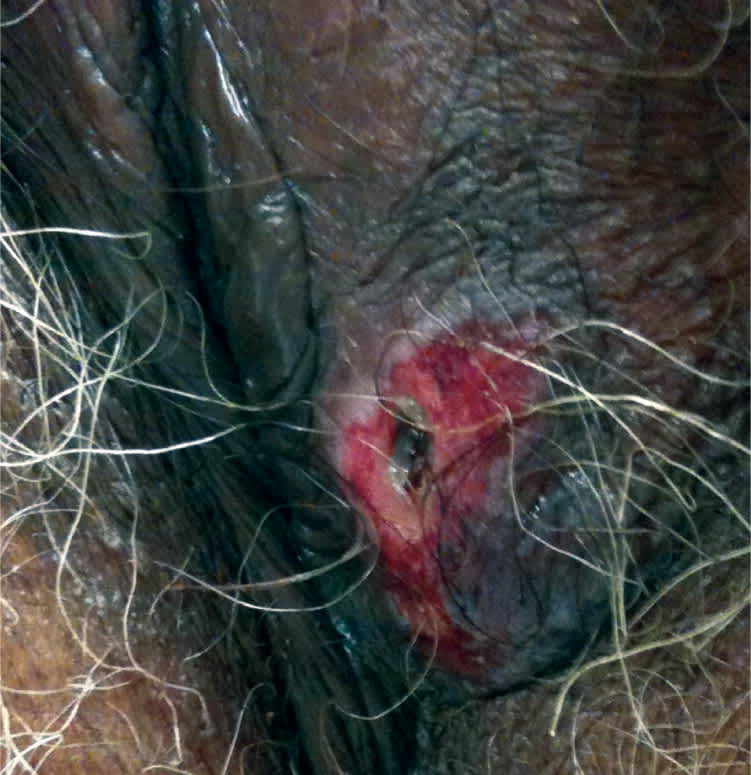
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Basal cell carcinoma.
B. Lichen sclerosus.
C. Melanoma.
D. Squamous cell carcinoma.
E. Syphilis.
Discussion
The correct answer is D: squamous cell carcinoma. Biopsy confirmed the diagnosis of basaloid squamous carcinoma, a type of squamous cell carcinoma. More than 90 percent of vulvar malignancies are squamous cell carcinomas.1 Vulvar squamous cell carcinoma typically presents as a unifocal plaque, ulcer, or mass on the labia majora1 and is most common in postmenopausal white women.1,2 Patients often report a pruritic area that becomes a red, nonhealing wound.1 Vulvar bleeding, discharge, dysuria, and enlarged lymph nodes are less common symptoms.1,3 Many patients are asymptomatic at the time of diagnosis. The signs and symptoms of vulvar malignancies are similar, so it is essential to biopsy all lesions to establish a diagnosis.
Squamous cell carcinoma is strongly associated with human papillomavirus types 16 and 33 or chronic inflammation from an autoimmune process.1,4 Human papillomavirus is responsible for approximately 60 percent of vulvar cancers.1,4 Risk factors for vulvar cancers include smoking, vulvar dystrophy (lichen sclerosus), vulvar or cervical intraepithelial neoplasia, immunodeficiency syndromes, history of cervical cancer, and Northern European ancestry.1,4
Treatment options for squamous cell carcinoma include surgical excision, radiation therapy, and chemotherapy. Each of the treatments may be used alone or in combination, depending on the stage of the lesion.1,3 The prognosis is determined by the size of the lesion, lymph node involvement, and presence or absence of distant metastasis. Squamous cell carcinoma that is found early, before it spreads into deeper tissues, has a 90 percent cure rate.1,3
Basal cell carcinoma tends to affect the face, but comprises approximately 2 percent of vulvar cancers.2 It may present as a locally invasive rodent, or Jacob, ulcer with rolled edges and a central ulceration. The lesions may be pigmented or pearly gray and typically have a granular appearance.
Lichen sclerosus is an eruption of pruritic, white, atrophic papules and plaques that usually occur in postmenopausal women. The lesions are either discrete or confluent and contain a central depression.
Melanoma is the second most common vulvar malignancy, accounting for 5 to 10 percent of primary vulvar neoplasms.1,2 The disease predominantly affects non-Hispanic white, postmenopausal women.2 Melanomas often present as a mass or nodule with bleeding, discharge, dysuria, and pain.2 The disease rarely affects genitalia, but lesions are more common on the clitoris or the labia minora. Melanomas are usually pigmented, although amelanotic lesions occur. Melanoma rarely presents as an ulcer.
Syphilis is an infectious disease caused by Treponema pallidum that is transmitted via direct sexual contact. A chancre, which develops after an incubation period of 12 to 30 days, starts as a painless papule or an area of infiltration that is a dull red color and hard. The center then erodes and becomes ulcerated. Unlike a squamous cell carcinoma lesion, this chancre will heal slowly over four to six weeks followed by a generalized rash.
Summary Table
| Condition | Characteristics |
|---|---|
| Basal cell carcinoma | Locally invasive rodent, or Jacob, ulcer with rolled edges and central ulceration; pigmented or pearly gray with granular appearance; tends to affect the face |
| Lichen sclerosus | Pruritic, white, atrophic papules and plaques; discrete or confluent with central depression |
| Melanoma | Mass or nodule with bleeding, discharge, dysuria, and pain; usually pigmented; rarely affects genitalia, but more common on clitoris or labia minora |
| Squamous cell carcinoma | Unifocal plaque, ulcer, or mass; pruritic area becomes red, nonhealing wound |
| Syphilis | Chancre appears as painless papule or area of infiltration that is a dull red color and hard, then center erodes and becomes ulcerated; chancre heals on its own, followed by a generalized rash |

