Acute pyelonephritis is a common bacterial infection of the renal pelvis and kidney most often seen in young adult women. History and physical examination are the most useful tools for diagnosis. Most patients have fever, although it may be absent early in the illness. Flank pain is nearly universal, and its absence should raise suspicion of an alternative diagnosis. A positive urinalysis confirms the diagnosis in patients with a compatible history and physical examination. Urine culture should be obtained in all patients to guide antibiotic therapy if the patient does not respond to initial empiric antibiotic regimens. Escherichia coli is the most common pathogen in acute pyelonephritis, and in the past decade, there has been an increasing rate of E. coli resistance to extended-spectrum beta-lactam antibiotics. Imaging, usually with contrast-enhanced computed tomography, is not necessary unless there is no improvement in the patient's symptoms or if there is symptom recurrence after initial improvement. Outpatient treatment is appropriate for most patients. Inpatient therapy is recommended for patients who have severe illness or in whom a complication is suspected. Practice guidelines recommend oral fluoroquinolones as initial outpatient therapy if the rate of fluoroquinolone resistance in the community is 10 percent or less. If the resistance rate exceeds 10 percent, an initial intravenous dose of ceftriaxone or gentamicin should be given, followed by an oral fluoroquinolone regimen. Oral beta-lactam antibiotics and trimethoprim/sulfamethoxazole are generally inappropriate for outpatient therapy because of high resistance rates. Several antibiotic regimens can be used for inpatient treatment, including fluoroquinolones, aminoglycosides, and cephalosporins.
Acute pyelonephritis is one of the most common serious bacterial infections in young adult women. Because of the frequency and severity of the infection, physicians must be familiar with approaches to effective management. This includes making an accurate diagnosis, deciding between inpatient and outpatient management, and selecting an appropriate antimicrobial regimen that is consistent with expert guidelines and local susceptibility data.
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | Reference |
|---|---|---|
| A urine culture and antimicrobial susceptibility testing should be performed in women with suspected acute pyelonephritis. Initial empiric therapy should be selected based on the likely infecting uropathogen and local antibiotic sensitivity patterns. | C | 15 |
| Treatment options for women with acute pyelonephritis not requiring hospitalization include 500 mg of oral ciprofloxacin (Cipro) twice per day for seven days; 1,000 mg of extended-release ciprofloxacin once per day for seven days; or 750 mg of levofloxacin (Levaquin) once per day for five days. These options are appropriate in areas where the prevalence of resistance to fluoroquinolones does not exceed 10 percent. | C | 15 |
| Oral trimethoprim/sulfamethoxazole (Bactrim, Septra) at a dosage of 160 mg/800 mg twice per day for 14 days is an appropriate treatment choice for women with acute pyelonephritis if the uropathogen is known to be susceptible. | C | 15 |
| Initial treatment of women with acute pyelonephritis who require hospitalization should include an intravenous antimicrobial regimen, such as a fluoroquinolone, an aminoglycoside (with or without ampicillin), an extended-spectrum cephalosporin or penicillin (with or without an aminoglycoside), or a carbapenem.* | C | 15 |
*—The choice of agents should be based on local resistance data, and the regimen should be tailored based on susceptibility results.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Epidemiology
By definition, acute pyelonephritis is an infection of the renal pelvis and kidney that usually results from ascent of a bacterial pathogen up the ureters from the bladder to the kidneys. It is estimated that acute pyelonephritis accounts for approximately 250,000 office visits and 200,000 hospital admissions each year in the United States, and approximately 11 hospitalizations per 10,000 Canadian women each year.1–3 The incidence of acute pyelonephritis is highest in otherwise healthy women 15 to 29 years of age, followed by infants and older persons.4 Although acute pyelonephritis also occurs in men, children, and pregnant women, these groups account for only a small percentage of cases. Accordingly, this review focuses on diagnosis and treatment of acute pyelonephritis in nonpregnant women.
MICROBIOLOGY
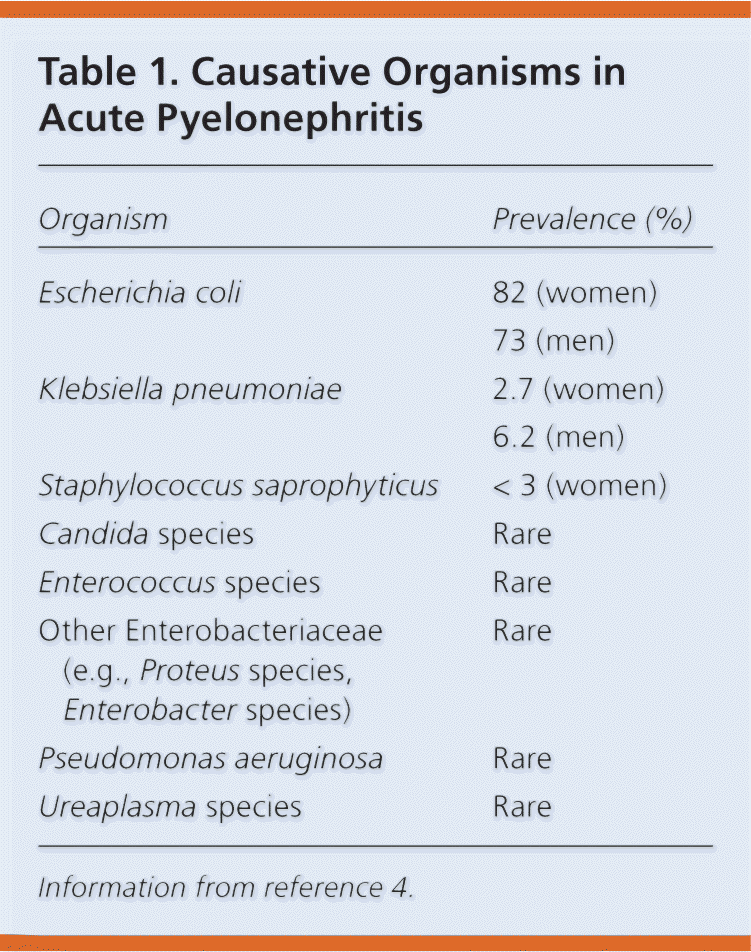
In 80 percent of acute pyelonephritis cases, Escherichia coli is the responsible pathogen in women, although it is not as common in older persons.5 After E. coli, less common causative organisms include other Enterobacteriaceae, Pseudomonas aeruginosa, group B streptococci, and enterococci. The spectrum of pathogens involved in acute pyelonephritis is similar to that of cystitis but with a lower frequency of Staphylococcus saprophyticus (Table 14).
Table 1. Causative Organisms in Acute Pyelonephritis
| Organism | Prevalence (%) |
|---|---|
| Escherichia coli | 82 (women) |
| 73 (men) | |
| Klebsiella pneumoniae | 2.7 (women) |
| 6.2 (men) | |
| Staphylococcus saprophyticus | < 3 (women) |
| Candida species | Rare |
| Enterococcus species | Rare |
| Other Enterobacteriaceae (e.g., Proteus species, Enterobacter species) | Rare |
| Pseudomonas aeruginosa | Rare |
| Ureaplasma species | Rare |
Information from reference 4.
ANTIBIOTIC RESISTANCE
During the previous decade, community-acquired bacteria (particularly E. coli) that produce extended-spectrum beta-lactamases have emerged as a cause of acute pyelonephritis worldwide. The most common risk factors for contracting these uropathogens include visits to health care centers, recent use of antimicrobial agents (particularly cephalosporins and fluoroquinolones), older age, and presence of comorbid conditions, such as diabetes mellitus and recurrent urinary tract infections (UTIs).6–9
RISK FACTORS
Risk factors for acute pyelonephritis in nonpregnant women include sexual intercourse three or more times per week during the previous 30 days, UTIs in the previous 12 months, diabetes, stress incontinence in the previous 30 days, a new sex partner in the previous year, recent spermicide use, and a history of UTIs in the patient's mother.4,5,10 Older women, women who are menopausal or pregnant, and women who have preexisting urinary tract structural abnormalities or obstructions have a higher risk of UTI, but not necessarily of acute pyelonephritis.5,6
COMPLICATED VS. UNCOMPLICATED ACUTE PYELONEPHRITIS
Uncomplicated acute pyelonephritis typically occurs in healthy, young women without structural or functional urinary tract abnormalities and without relevant comorbidities. Complicated acute pyelonephritis occurs in patients with a structurally or functionally abnormal genitourinary tract, or a predisposing medical condition. Compared with uncomplicated acute pyelonephritis, complicated acute pyelonephritis is characterized by a broader spectrum of clinical presentations, a wider variety of infecting organisms (including a greater likelihood of antimicrobial resistance), and a greater risk of progression to a complication, such as intrarenal or perinephric abscess or emphysematous pyelonephritis.11
Clinical Diagnosis
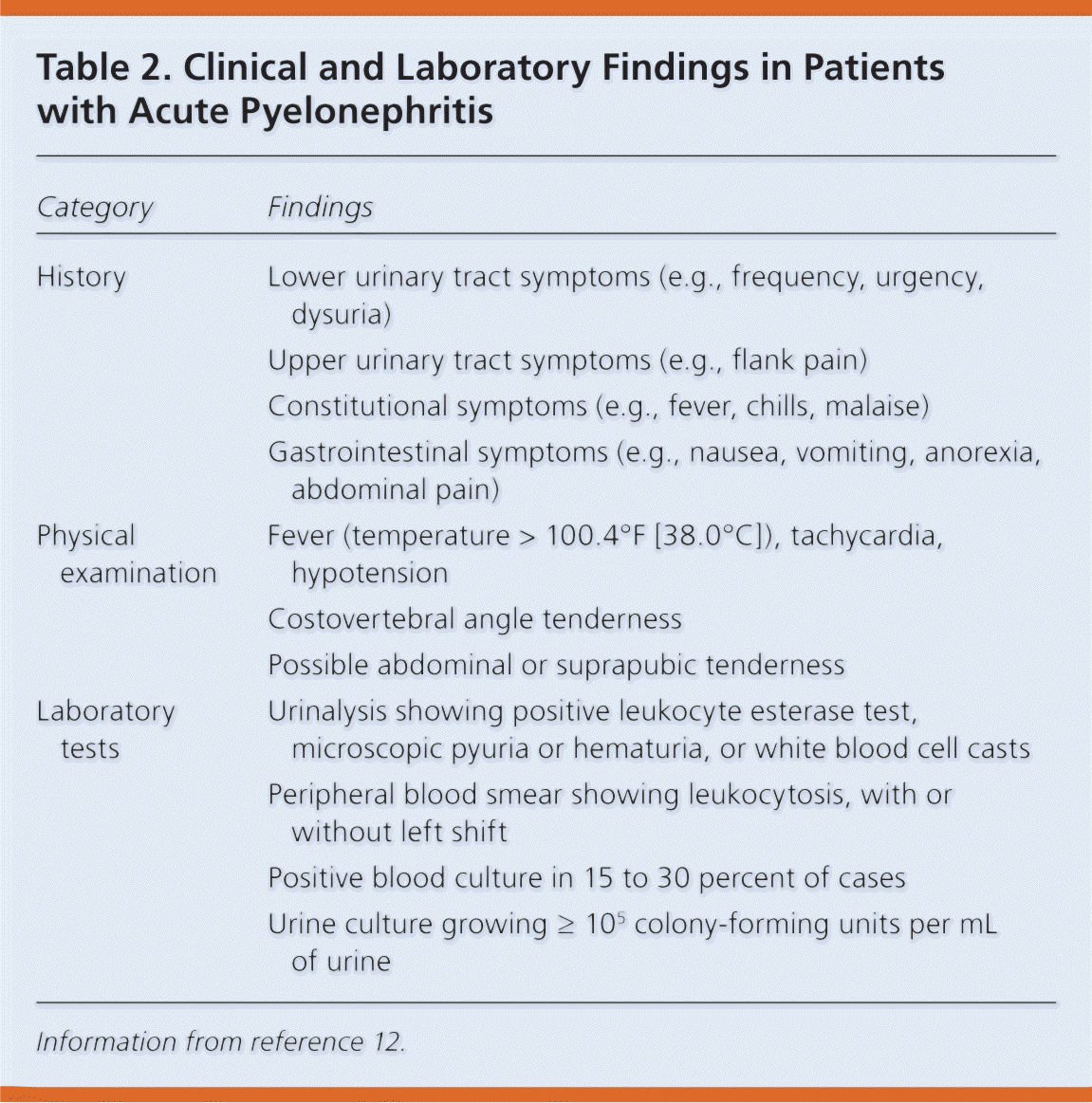
History and physical examination are the most helpful tools for diagnosing acute pyelonephritis (Table 212 ). Physicians should consider acute pyelonephritis in women presenting with lower urinary tract symptoms (e.g., urinary frequency, urgency, dysuria) accompanied by fever, nausea, vomiting, or flank pain. Flank pain is nearly universal in patients with acute pyelonephritis; its absence should raise suspicion of an alternative diagnosis. On physical examination, the key finding is tenderness to palpation of the costovertebral angle. Patients with nephrolithiasis and ureterolithiasis, which also cause flank pain, do not usually present with costovertebral angle tenderness.
Table 2. Clinical and Laboratory Findings in Patients with Acute Pyelonephritis
| Category | Findings |
|---|---|
| History | Lower urinary tract symptoms (e.g., frequency, urgency, dysuria) |
| Upper urinary tract symptoms (e.g., flank pain) | |
| Constitutional symptoms (e.g., fever, chills, malaise) | |
| Gastrointestinal symptoms (e.g., nausea, vomiting, anorexia, abdominal pain) | |
| Physical examination | Fever (temperature > 100.4°F [38.0°C]), tachycardia, hypotension |
| Costovertebral angle tenderness | |
| Possible abdominal or suprapubic tenderness | |
| Laboratory tests | Urinalysis showing positive leukocyte esterase test, microscopic pyuria or hematuria, or white blood cell casts |
| Peripheral blood smear showing leukocytosis, with or without left shift | |
| Positive blood culture in 15 to 30 percent of cases | |
| Urine culture growing ≥ 105 colony-forming units per mL of urine |
Information from reference 12.
Fever greater than 100.4°F (38.0°C) is characteristic of acute pyelonephritis, but it may be absent in persons with early or mild cases. Fever may also be absent in frail, older persons or in immunocompromised persons, who also may not exhibit other classic manifestations of acute pyelonephritis.
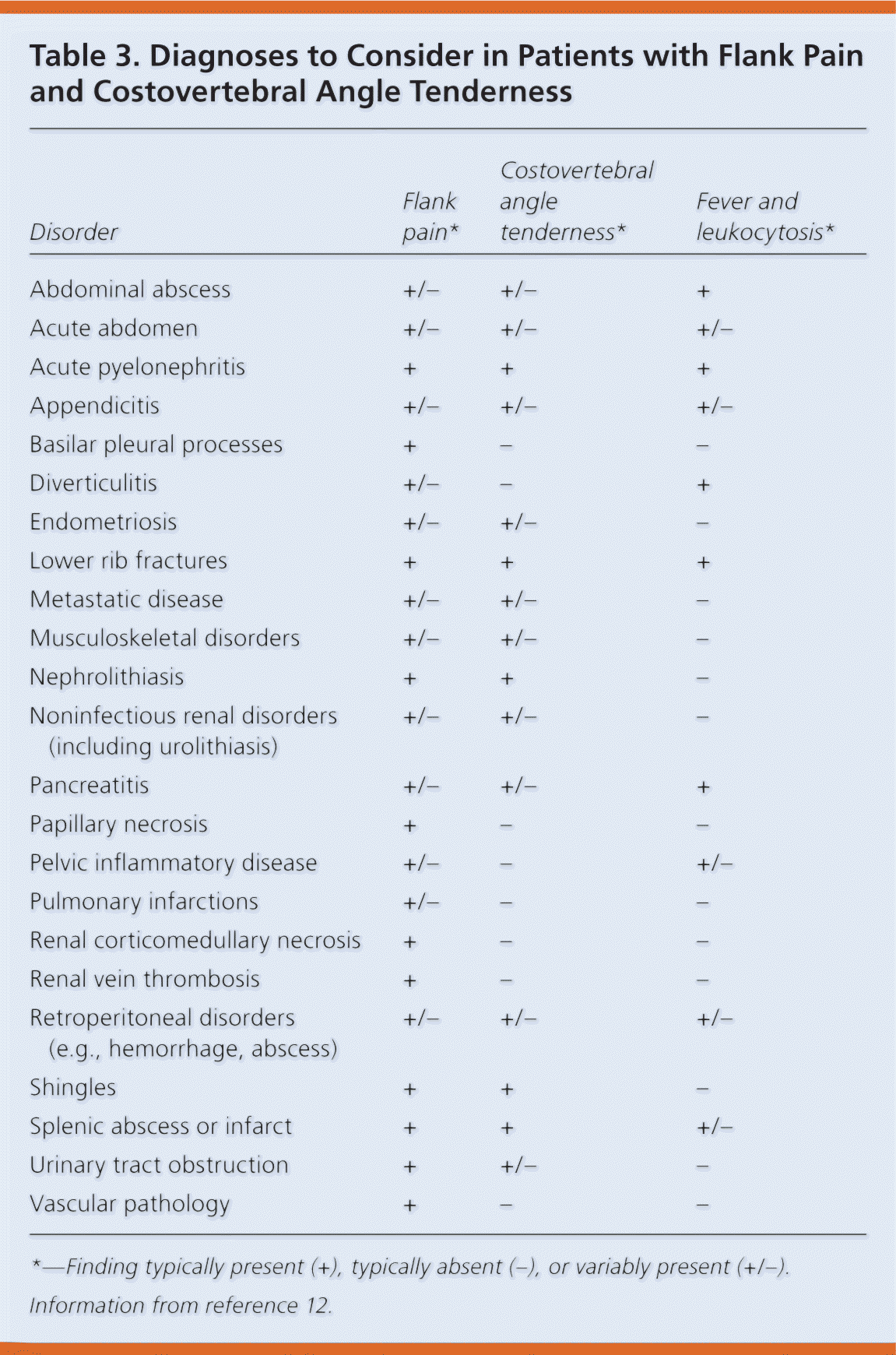
Physicians should consider other disorders that may arise from or mimic acute pyelonephritis (Table 312 ). Intrarenal and perinephric abscesses, which usually are complications of acute pyelonephritis, are more common than emphysematous pyelonephritis, which is a necrotizing infection that produces intraparenchymal gas within the kidney that is identifiable by renal imaging.13 This disorder occurs most often in older women with diabetes. Additional complications of acute pyelonephritis that may benefit from urologic or infectious disease subspecialty consultation are listed in Table 4.
Table 3. Diagnoses to Consider in Patients with Flank Pain and Costovertebral Angle Tenderness
| Disorder | Flank pain* | Costovertebral angle tenderness* | Fever and leukocytosis* |
|---|---|---|---|
| Abdominal abscess | +/− | +/− | + |
| Acute abdomen | +/− | +/− | +/− |
| Acute pyelonephritis | + | + | + |
| Appendicitis | +/− | +/− | +/− |
| Basilar pleural processes | + | − | − |
| Diverticulitis | +/− | − | + |
| Endometriosis | +/− | +/− | − |
| Lower rib fractures | + | + | + |
| Metastatic disease | +/− | +/− | − |
| Musculoskeletal disorders | +/− | +/− | − |
| Nephrolithiasis | + | + | − |
| Noninfectious renal disorders (including urolithiasis) | +/− | +/− | − |
| Pancreatitis | +/− | +/− | + |
| Papillary necrosis | + | − | − |
| Pelvic inflammatory disease | +/− | − | +/− |
| Pulmonary infarctions | +/− | − | − |
| Renal corticomedullary necrosis | + | − | − |
| Renal vein thrombosis | + | − | − |
| Retroperitoneal disorders (e.g., hemorrhage, abscess) | +/− | +/− | +/− |
| Shingles | + | + | − |
| Splenic abscess or infarct | + | + | +/− |
| Urinary tract obstruction | + | +/− | − |
| Vascular pathology | + | − | − |
*—Finding typically present (+), typically absent (−), or variably present (+/−).
Information from reference 12.
Table 4. Complications of Acute Pyelonephritis That May Benefit from Subspecialty Consultation

| Complication | Relevant diagnostic test | Relevant subspecialty |
|---|---|---|
| Catheter-associated bacteremia | Blood cultures, antimicrobial susceptibility testing | Infectious diseases |
| Emphysematous pyelonephritis | Urinary tract imaging | Infectious diseases, interventional radiology, urology |
| Extensively drug-resistant organism | Blood and urine cultures, antimicrobial susceptibility testing | Infectious diseases |
| Perinephric or intrarenal abscess | Urinary tract imaging | Interventional radiology, urology |
| Urinary obstruction | Urinary tract imaging | Interventional radiology, urology |
Previous antibiotic treatment, although not diagnostically relevant, is important to consider when choosing a treatment regimen. For this reason, it should be included in the patient history when considering acute pyelonephritis.
Inpatient vs. Outpatient Treatment
Most cases of uncomplicated acute pyelonephritis can be managed in the outpatient setting. However, patients who appear ill may have severe pyelonephritis or a complication of acute pyelonephritis and should be considered for hospitalization and further evaluation (Table 514 ). The possibility of urinary obstruction or an alternative diagnosis should be considered in these patients.
Table 5. Considerations for Hospitalization in Patients with Acute Pyelonephritis

| Comorbid conditions (e.g., renal dysfunction, urologic disorders, diabetes mellitus, advanced liver or cardiac disease) |
| Hemodynamic instability* |
| Male sex |
| Metabolic derangement (e.g., renal dysfunction, acidosis) |
| Pregnancy |
| Severe flank or abdominal pain |
| Toxic appearance |
| Unable to take liquids by mouth |
| Very high fever (> 103°F [39.4°C]) |
*—Physicians must be alert for the presence of severe sepsis and septic shock, which require urgent specialized management that is beyond the scope of this review.
Information from reference 14.
Diagnostic Tests
URINALYSIS
Urine dipstick testing, microscopic urinalysis, or both are commonly used in diagnosing UTI, including acute pyelonephritis. Most women with acute pyelonephritis have marked pyuria or a positive leukocyte esterase test, which often is accompanied by microscopic hematuria or a positive heme dipstick test. In contrast, gross hematuria is rare in patients with acute pyelonephritis and is more common in patients with acute uncomplicated cystitis. The presence of white blood cell casts indicates renal-origin pyuria, supporting the diagnosis of acute pyelonephritis, but casts are not often seen.
URINE CULTURE
All patients with suspected acute pyelonephritis should have a urine culture and antimicrobial susceptibility testing to guide possible adjustment of the initial antimicrobial regimen (if there is no improvement) and selection of step-down oral therapy for patients treated initially with intravenous therapy.15
A midstream urine specimen after proper cleansing of the vulva is often recommended. Several studies, however, found no significant differences in the number of contaminated or unreliable culture results when voided urine specimens were collected with or without preparatory cleansing.16–18 Obtaining a urine sample by catheterization is unnecessary. Studies have shown no differences in colony counts or organisms between samples collected by catheterization versus midstream voiding.17,18
More than 95 percent of women with uncomplicated acute pyelonephritis will have greater than 105 colony-forming units of a single gram-negative organism per mL of urine.19 Urine Gram stain, if available, may aid in the choice of empiric antimicrobial therapy pending culture results. If gram-positive cocci are observed, Enterococcus species or S. saprophyticus may be the causative organism.20
Posttreatment urinalysis and urine culture are unnecessary in patients who are asymptomatic after therapy. However, repeat urine culture is advised if symptoms do not improve substantially within two to three days of initiation of therapy, or if symptoms recur within two weeks of treatment. These patients should also undergo urinary tract imaging.
IMAGING
Most women with acute pyelonephritis do not need imaging studies unless symptoms do not improve or there is a recurrence.21 The purpose of imaging is to identify an underlying structural abnormality, such as occult obstruction from a stone or an abscess 21,22 (Figure 123). Although renal ultrasonography and magnetic resonance imaging are sometimes used, computed tomography with contrast media is considered the imaging modality of choice for nonpregnant women.
Figure 1.
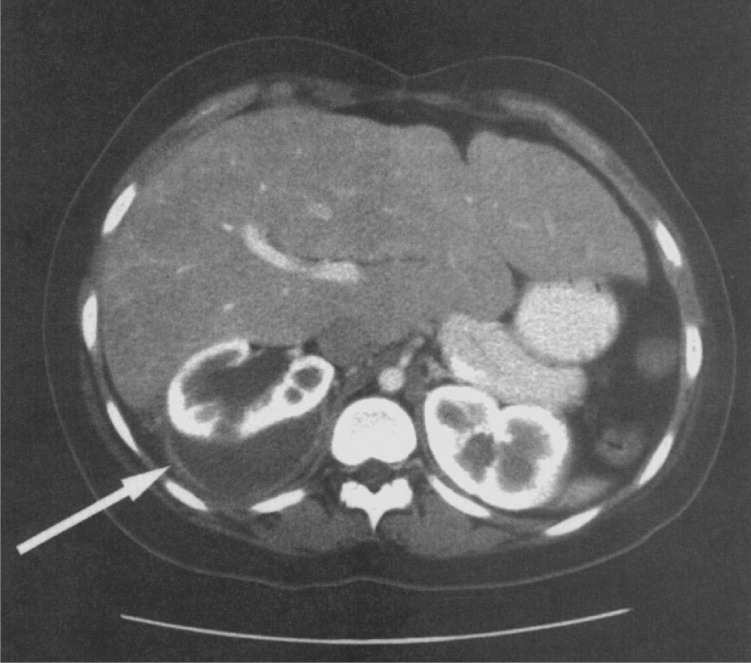
Abdominal computed tomography with intravenous contrast media in a patient with acute pyelonephritis demonstrates a large right perinephric abscess (crescentic low-density collection identified by arrow).
Reprinted with permission from Tanagho E. Radiography of urological infections. In: Tanagho EA, McAninch JW, eds. Smith's General Urology. New York, NY: McGraw-Hill; 2008:525.
Because of the risk of contrast nephropathy, caution is needed when administering contrast media to patients taking metformin (Glucophage) or to those with renal insufficiency. However, patients with acute pyelonephritis and an acutely elevated baseline serum creatinine level may sometimes warrant computed tomography imaging as part of the evaluation to look for obstruction.24
BLOOD CULTURES
Blood cultures are commonly obtained from patients with acute pyelonephritis who are ill enough to warrant hospital admission, although they may not routinely be necessary in patients with uncomplicated acute pyelonephritis.25,26 Approximately 15 to 30 percent of patients with acute pyelonephritis are found to be bacteremic; older persons and those with complicated acute pyelonephritis are more likely to have bacteremia and sepsis.26–28
Because urine culture yields a causative organism in almost all cases of acute pyelonephritis, a positive blood culture is diagnostically redundant. However, blood cultures may be the only method of identifying the causative organism in cases of suspected acute pyelonephritis that turn out to be another disorder, such as endometritis, intraabdominal or psoas abscess, or cholangitis.
There is no evidence that patients with a positive blood culture should be treated differently from those with negative blood cultures with respect to agent, route, or duration of antimicrobial therapy; hospital admission; or length of hospital stay (if admitted to the hospital).
OTHER DIAGNOSTIC TESTS
The baseline evaluation of acute pyelonephritis should include a basic metabolic panel, most importantly to assess renal function. If the diagnosis is not clear, other laboratory tests (e.g., lipase, transaminase, and beta subunit of human chorionic gonadotropin levels) may be appropriate to clarify the differential diagnosis.
Choice of Antibiotics
In 2010, the Infectious Diseases Society of America updated its 1999 guidelines on the treatment of acute uncomplicated cystitis and pyelonephritis in women.15 The guidelines include recommendations for antimicrobial regimens in patients with acute pyelonephritis.
When choosing an antibiotic, physicians should consider the effectiveness, risk of adverse effects, and resistance rates in the local community. Regardless of which antibiotic is chosen for initial empiric therapy, the regimen should be revised as necessary after urine culture susceptibility results are available.
OUTPATIENT REGIMENS
Fluoroquinolones are the preferred empiric antimicrobial class in communities where the local prevalence of resistance of community-acquired E. coli is 10 percent or less. Although not all clinical microbiology laboratories serving outpatient medical practices provide reports on the source of specimens tested for antibiotic resistance (i.e., community-acquired versus hospital-acquired), physicians should consider contacting their local laboratory to obtain the best available susceptibility data.
If the prevalence of fluoroquinolone resistance among relevant organisms does not exceed 10 percent, patients not requiring hospitalization can be treated with oral ciprofloxacin (Cipro; 500 mg twice per day for seven days), or a once-daily oral fluoroquinolone, such as ciprofloxacin (1,000 mg, extended-release, for seven days) or levofloxacin (Levaquin; 750 mg for five days).15 These can be given with or without an initial intravenous dose of the corresponding agent (e.g., 400 mg ciprofloxacin or 500 mg levofloxacin). An initial intravenous dose is appropriate in patients experiencing nausea or vomiting. Table 6 summarizes outpatient treatment options for nonpregnant women with acute pyelonephritis.15
Table 6. Outpatient Treatment Options for Nonpregnant Women with Acute Pyelonephritis

| Drug class | Antibiotic | Dosage |
|---|---|---|
| Fluoroquinolones* | Ciprofloxacin† (Cipro) | 500 mg orally, twice per day for seven days |
| Ciprofloxacin, extended-release‡ | 1,000 mg orally, once per day for seven days | |
| Levofloxacin‡ (Levaquin) | 750 mg orally, once per day for five days | |
| Folate inhibitors§ | Trimethoprim/sulfamethoxazole† (Bactrim, Septra) | 160 mg/800 mg orally, twice per day for 14 days |
*—Use when prevalence of fluoroquinolone resistance among Escherichia coli isolates is known to be 10 percent or less. If resistance prevalence exceeds 10 percent, see inpatient recommendations in Table 7.
†—There is good evidence for use from at least one properly randomized controlled trial.
‡—There is moderate evidence for use from at least one well-designed clinical trial, without randomization; from cohort or case-control analytic studies (preferably from more than one center); from multiple time-series; or from dramatic results from uncontrolled experiments.
§—Use if pathogen is known to be susceptible to trimethoprim/sulfamethoxazole. If susceptibility profile is unknown, see inpatient recommendations in Table 7.
Information from reference 15.
Because of the generally high prevalence of resistance to oral betalactam antibiotics and trimethoprim/sulfamethoxazole (Bactrim, Septra), these agents usually are reserved for cases where susceptibility results for the urine isolate are known and indicate likely activity.15 However, additional factors (e.g., allergy history, potential drug-drug interactions, drug availability) may require the empiric use of an oral beta-lactam antibiotic or trimethoprim/sulfamethoxazole before susceptibility is known. In such cases, a long-acting, broad-spectrum parenteral drug such as ceftriaxone (Rocephin; 1 g) or gentamicin (5 mg per kg) should be given concurrently as a one-time dose or longer to cover for possible resistance until sensitivities of the organism are known. Likewise, if the local fluoroquinolone resistance prevalence in E. coli exceeds 10 percent, an initial intravenous dose of ceftriaxone or gentamicin is recommended, followed by an oral fluoroquinolone regimen.
INPATIENT REGIMENS
For women with acute pyelonephritis who require hospitalization, initial intravenous antimicrobial therapy is recommended (Table 7).15 Options include a fluoroquinolone, an aminoglycoside (with or without ampicillin), an extended-spectrum cephalosporin or penicillin (with or without an aminoglycoside), or a carbapenem.15 Pregnant women with acute pyelonephritis should be hospitalized and treated initially with a second-or third-generation cephalosporin, and then assessed to determine whether further treatment as an outpatient is appropriate.29,30
Table 7. Initial and Step-Down Inpatient Treatment Options for Nonpregnant Women with Acute Pyelonephritis
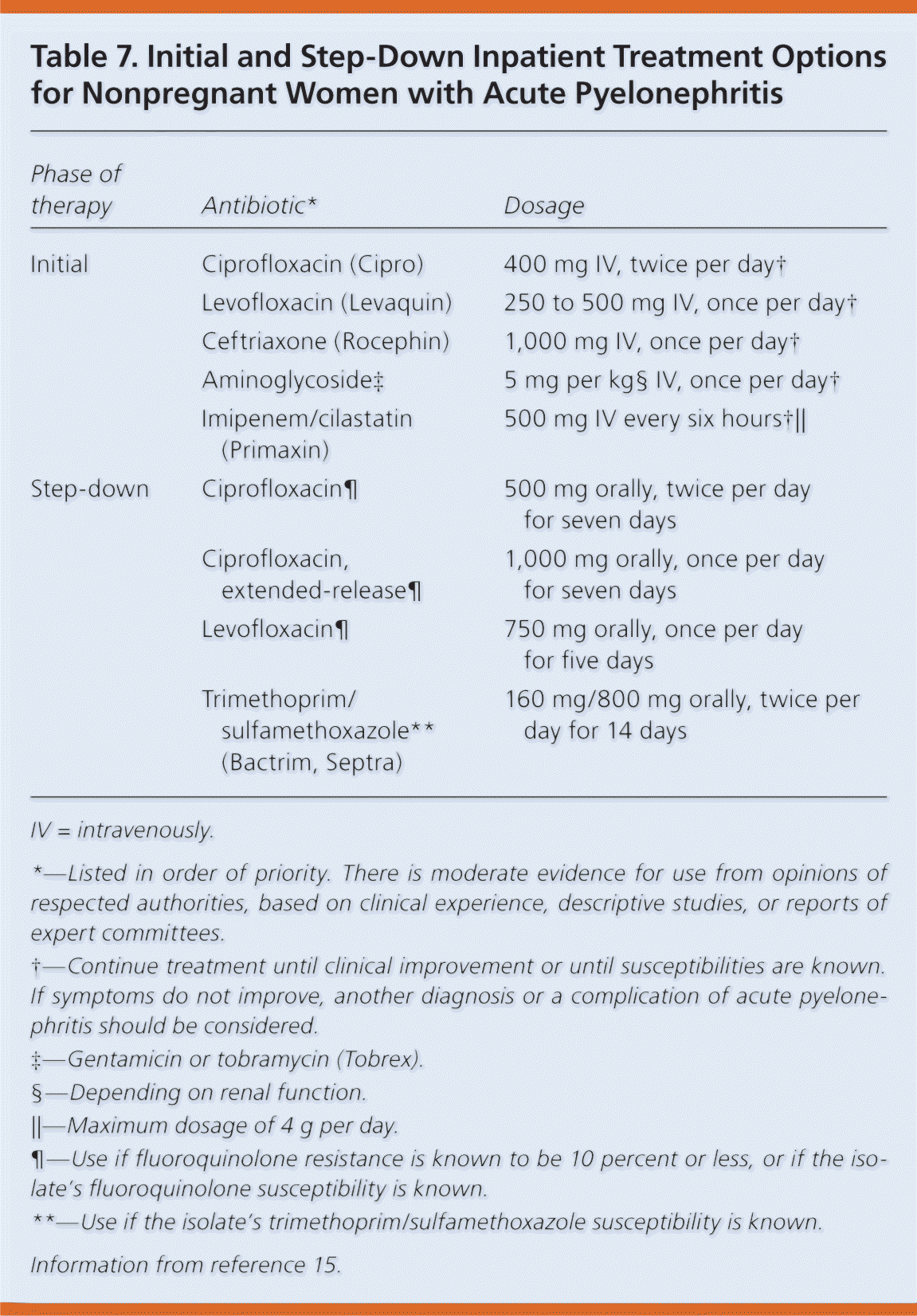
| Phase of therapy | Antibiotic* | Dosage |
|---|---|---|
| Initial | Ciprofloxacin (Cipro) | 400 mg IV, twice per day† |
| Levofloxacin (Levaquin) | 250 to 500 mg IV, once per day† | |
| Ceftriaxone (Rocephin) | 1,000 mg IV, once per day† | |
| Aminoglycoside‡ | 5 mg per kg§ IV, once per day† | |
| Imipenem/cilastatin (Primaxin) | 500 mg IV every six hours†∥ | |
| Step-down | Ciprofloxacin¶ | 500 mg orally, twice per day for seven days |
| Ciprofloxacin, extended-release¶ | 1,000 mg orally, once per day for seven days | |
| Levofloxacin¶ | 750 mg orally, once per day for five days | |
| Trimethoprim/sulfamethoxazole** (Bactrim, Septra) | 160 mg/800 mg orally, twice per day for 14 days |
IV = intravenously.
*—Listed in order of priority. There is moderate evidence for use from opinions of respected authorities, based on clinical experience, descriptive studies, or reports of expert committees.
†—Continue treatment until clinical improvement or until susceptibilities are known. If symptoms do not improve, another diagnosis or a complication of acute pyelonephritis should be considered.
‡—Gentamicin or tobramycin (Tobrex).
§—Depending on renal function.
∥—Maximum dosage of 4 g per day.
¶—Use if fluoroquinolone resistance is known to be 10 percent or less, or if the isolate's fluoroquinolone susceptibility is known.
**—Use if the isolate's trimethoprim/sulfamethoxazole susceptibility is known.
Information from reference 15.
Monitoring Response to Therapy
Therapy with appropriate empiric antibiotics should produce improvement within 48 to 72 hours. If the patient does not improve as expected (i.e., no progressive reduction in, or resolution of, the local and systemic signs and symptoms that led to the diagnosis), strong consideration should be given to a complication of acute pyelonephritis or an alternative diagnosis, and appropriate additional testing should be performed.

