A six-year-old girl presented with a rash on her right arm that her mother first noticed one month earlier. The rash began on her shoulder and grew distally down her arm in a linear pattern (Figure 1). It measured 1 cm × 35 cm and was hypopigmented and papular (Figure 2). The rash was nonpruritic. Application of antibiotic ointment and hydrating lotion had no effect. The patient was otherwise healthy, and her vaccinations were up to date. There were no other rashes on the patient or her family members, and there had been no change in her environment or exposures.
Figure 1.
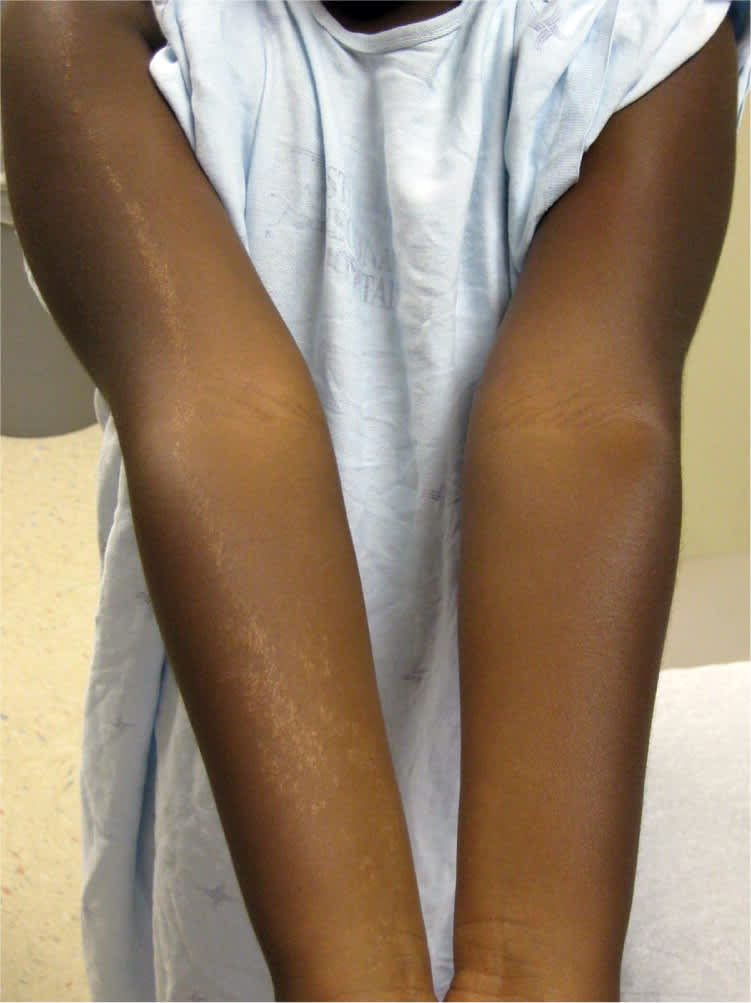
Figure 2.

Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Lichen planus.
B. Lichen striatus.
C. Psoriasis.
D. Tinea corporis.
Discussion
The answer is B: lichen striatus. Lichen striatus is an asymptomatic, papular rash with a sudden onset (full disease develops within weeks). The eruptions usually appear as a linear rash that expands distally down the extremities, but rarely can appear on the trunk or face. They are usually 2 mm to 2 cm in width, and the length can vary from a few centimeters to the entire length of a limb. Few cases of multiple bands have been reported.1 The rash occurs most often in childhood and is seldom reported in adults.2 It typically resolves without intervention within two years.2 Nail involvement is rare, but when it occurs it affects a single nail. Nail changes (e.g., ridging, splitting, fraying, onycholysis) can be observed before, during, or after the skin eruption.3
Lichen striatus occurs along the Blaschko lines (a linear and sometimes curved pattern of skin lesions on the body following the lines of embryogenesis), suggesting a somatic mutation in the keratinocytes.1 Microscopic findings include epidermal hyperkeratosis and focal parakeratosis in the epidermis. The CD8 cell infiltrate surrounds the sweat glands, a finding that distinguishes lichen striatus from lichen planus.2
Lichen planus manifests as pruritic, shiny, flat, violaceous papules that may have Wickham striae (a white, lacelike pattern on the surface). The condition usually occurs in middle-aged adults and may have a short or chronic course. The rash typically affects the mouth, extremities, or trunk. Involvement of the buccal mucosa is common, occurring in up to 70 percent of patients.4 Lichen planus can also affect the nails, causing ridging. It can be associated with immunosuppression, especially from hepatitis C.
Psoriasis is a chronic skin condition causing plaques with silver scale surrounded by erythema, usually occurring on the elbows, knees, and lower back. It is thought to be an immune-mediated disease and is associated with inflammatory bowel disease. The typical age of onset is biphasic, with the first peak between 20 and 30 years of age, and the second peak between 50 and 60 years of age.5 Arthritis or nail changes can develop.
Tinea corporis is a fungal infection that presents as a mildly pruritic, round, scaly patch. It extends centrifugally and has a raised, erythematous border with central clearing. This annular rash can be found on any body part. Diagnosis is confirmed with a potassium hydroxide preparation or fungal culture. Outbreaks can occur as a result of skin-to-skin contact.6
Summary Table
| Condition | Characteristics |
|---|---|
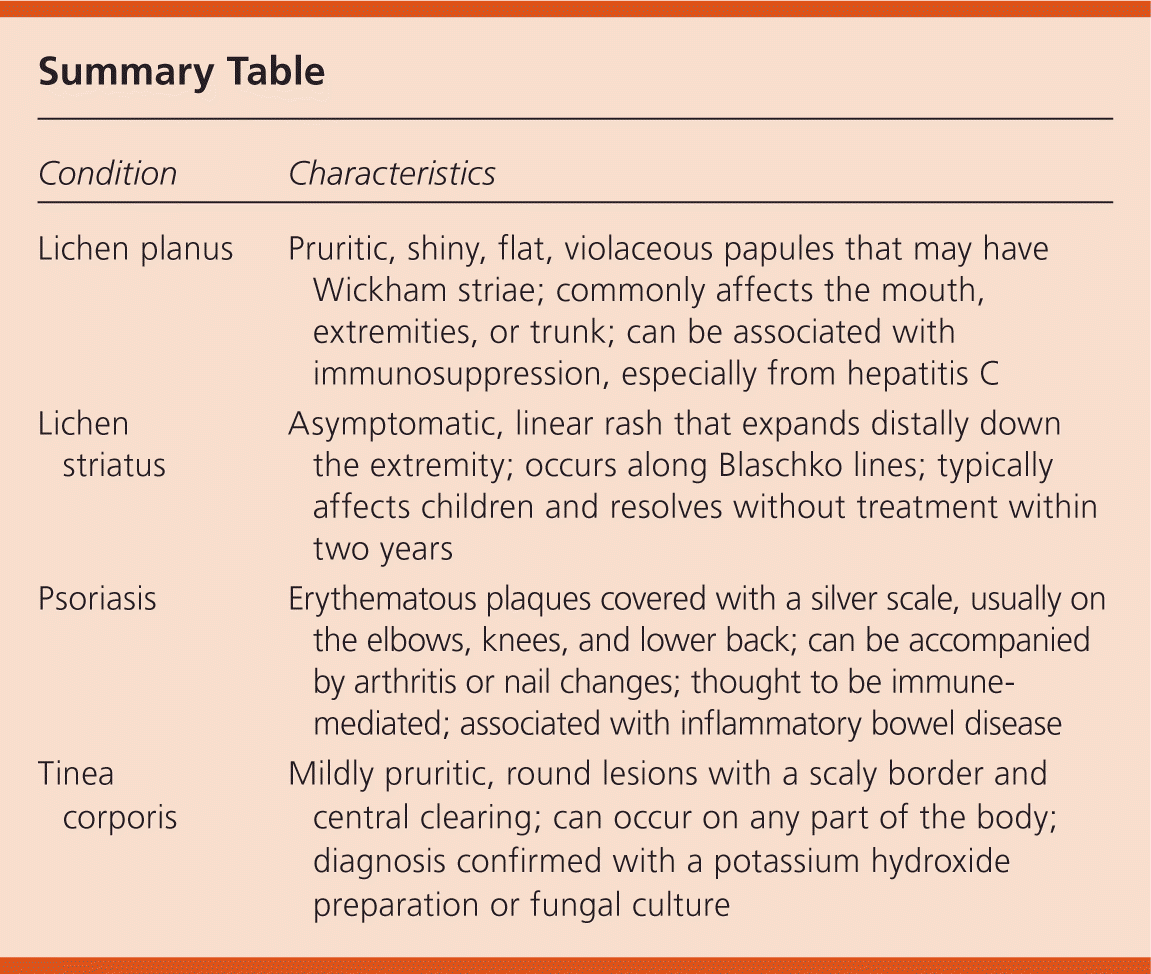
| Lichen planus | Pruritic, shiny, flat, violaceous papules that may have Wickham striae; commonly affects the mouth, extremities, or trunk; can be associated with immunosuppression, especially from hepatitis C |
| Lichen striatus | Asymptomatic, linear rash that expands distally down the extremity; occurs along Blaschko lines; typically affects children and resolves without treatment within two years |
| Psoriasis | Erythematous plaques covered with a silver scale, usually on the elbows, knees, and lower back; can be accompanied by arthritis or nail changes; thought to be immune-mediated; associated with inflammatory bowel disease |
| Tinea corporis | Mildly pruritic, round lesions with a scaly border and central clearing; can occur on any part of the body; diagnosis confirmed with a potassium hydroxide preparation or fungal culture |

