Am Fam Physician. 2011;84(6):705-709
| Guideline source: American College of Obstetricians and Gynecologists (ACOG) |
| Evidence rating system used? Yes |
| Literature search described? Yes |
| Published source:Obstetrics & Gynecology, April 2011 |
| Available at: http://journals.lww.com/greenjournal/Citation/2011/04000/Practice_Bulletin_No_119_Female_Sexual.38.aspx |
Sexual dysfunction is common in U.S. women but is underdiagnosed and undertreated, partly because patients are not likely to discuss it with their physician unless they are asked. In addition to patients' reluctance to initiate a conversation about sex, obstacles for physicians include a lack of adequate training and confidence, a perception that there are few treatment options, inadequate time to obtain a sexual history, and underestimation of the prevalence of sexual dysfunction.
Initial Approach to the Patient
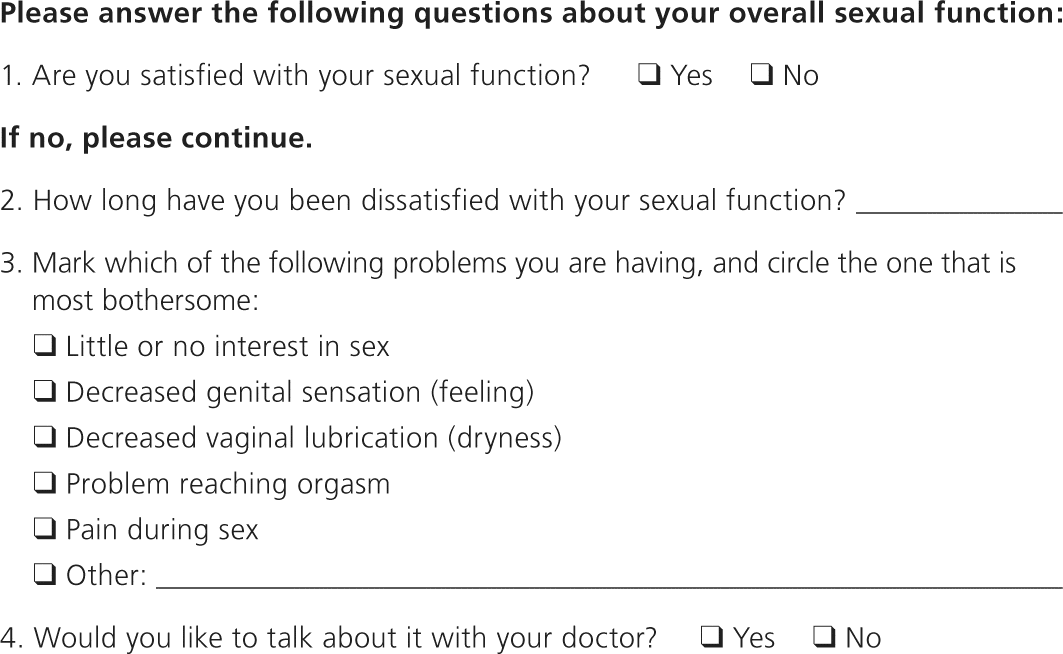
A caring and compassionate physician who is comfortable discussing sex, who knows the patient and has seen her before, and who seems concerned about her sexual health is one with whom patients will feel most comfortable discussing sex. A thorough sexual history should be obtained using a brief set of questions or a screening questionnaire (Figure 1). The patient's medical, surgical, social, and psychiatric history also should be obtained, and information about the use of prescription and over-the-counter medications should be elicited. After the initial evaluation, treatment can be initiated or a referral can be made to a marriage counselor or sex therapist, depending on the training and comfort level of the physician.
Types of Sexual Dysfunction
Sexual dysfunction in women includes several conditions that are characterized by loss of sexual desire, impaired arousal, inability to achieve orgasm, or pain during sex. A diagnosis should be made when symptoms cause distress or interpersonal problems.
HYPOACTIVE SEXUAL DESIRE DISORDER
Hypoactive sexual desire disorder (i.e., persistent or recurrent deficiency or absence of sexual desire or receptivity to sexual activity) is the most common sexual dysfunction in women, with an estimated prevalence between 5.4 and 13.6 percent. The disorder peaks in women 40 to 60 years of age and in those who have undergone surgical menopause. In this age group, it may be situational, such as in depression or chronic disease (e.g., endocrine disorders with adrenal insufficiency), or it may be associated with medication use. However, it is more often an isolated event. In younger women, this disorder is often associated with situational circumstances, such as dysfunctional relationships, chronic disease, depression, gynecologic disorders, and use of certain medications (e.g., selective serotonin reuptake inhibitors [SSRIs], oral contraceptives, corticosteroids).
Treatment of hypoactive sexual desire disorder consists of psychotherapy and antidepressants for patients who have associated anxiety. Transdermal testosterone is also effective for short-term therapy; however, there is little evidence to support long-term use (longer than six months). Monitoring androgen levels before or during treatment has not been proven useful.
FEMALE SEXUAL AROUSAL DISORDER
Female sexual arousal disorder (i.e., inability to complete sexual activity with adequate lubrication) occurs in approximately 5 percent of U.S. women. It often affects women with gynecologic or chronic medical conditions and those who are taking certain medications (especially SSRIs). The disorder typically resolves when the underlying condition is treated or the medication is adjusted.
FEMALE ORGASMIC DISORDER
Female orgasmic disorder (i.e., persistent or recurrent delay in or absence of orgasm after a normal excitement phase) occurs in 3.4 to 5.8 percent of U.S. women. It can be either primary (i.e., patient has never achieved orgasm) or secondary (i.e., resulting from another sexual dysfunction, typically hypoactive sexual desire disorder). Primary orgasmic disorder may be genetic and is often associated with a history of trauma or abuse. It typically does not resolve without treatment. Psychotherapy and couples counseling may be helpful for women with primary orgasmic disorder associated with abuse. There is no effective therapy for unexplained primary orgasmic disorder in which the patient has never achieved orgasm, even through masturbation. Secondary orgasmic disorder typically resolves with treatment of the primary dysfunction. Adjunctive education on masturbation techniques may be helpful.
SEXUAL PAIN DISORDERS
Vaginismus (i.e., recurrent or persistent involuntary spasm of the muscles of the outer one-third of the vagina that interferes with sex) occurs in 1 to 6 percent of women. It is common in women with hypoactive sexual desire disorder and in those with sexual aversion; these disorders often have the same situational and psychosocial causes, and resolve with treatment of those causes. In other women, vaginismus is associated with gynecologic disorders, chronic medical conditions, and the use of certain medications, and resolves with treatment or adjustment of medications. The most effective treatment is a combination of cognitive and behavioral psychotherapy known as systematic desensitization. Patients are taught deep muscle relaxation techniques, which they use while dilators of increasing diameter are gradually inserted into the vagina. The goal is to desensitize the patient to her fear that vaginal penetration will be painful, and give her a sense of control so that vaginal muscle contractions are no longer an automatic response to penetration. If treatment is ineffective, the patient may benefit from referral for pelvic floor physical therapy.
Dyspareunia (i.e., recurrent or persistent genital pain associated with sex and not caused exclusively by lack of lubrication or by vaginismus) is a common problem in postmenopausal women, among whom the prevalence is approximately 8 to 22 percent. Pain on vaginal entry may reflect provoked vestibulodynia, inadequate lubrication, or vaginismus. Physical examination will reproduce the pain when the vulva or vagina is touched with a cotton swab or when a finger is inserted into the vagina. Pain may worsen over time because of arousal disorders and loss of desire.
Hysterectomy and Menopause
The main indications for hysterectomy are uterine leiomyomas, menstrual disorders, uterine prolapse, and endometriosis—all of which can lead to decreased sexual function. In addition to concerns about the risks of surgery, many women worry about their sexual function after the procedure. Prospective studies evaluating the effect of hysterectomy on postoperative sexual function have not shown a difference between total and subtotal hysterectomy.
Estrogen affects sexual performance through maintenance of genital tissues and secretions, pelvic muscle tone, and elasticity. In postmenopausal women, decreased estrogen levels induce vulvovaginal atrophy, leading to pain and trauma during sex. Vaginal application of estrogen results in improved dyspareunia, less vaginal dryness, improved vaginal mucosal maturation indices, and reduced vaginal pH. Because oral forms of estrogen may not alleviate vulvovaginal atrophy, topical formulations may be preferable. Tablets, gels, creams, and vaginal rings are equally effective. Systemic absorption of vaginal estrogen is limited, but still a concern. The lowest effective dose should be used for the least amount of time to alleviate symptoms. The optimal duration of treatment has not been determined, but daily treatment for a few weeks has been advocated, with gradual tapering based on symptoms.
Androgen levels decrease in women of reproductive age until menopause, after which no further decrease is observed. Many studies have shown that sexual desire and sexual activity increase with androgen supplementation; however, the results of other studies have been equivocal. Although transdermal testosterone is an effective short-term treatment for hypoactive sexual desire disorder in women, it has not been approved by the U.S. Food and Drug Administration for this use. The main risks associated with androgen therapy in women are hirsutism, acne, virilization, and cardiovascular complications. A possible association with breast cancer also has been reported.