A 76-year-old man with a 110-pack-year smoking history and resultant chronic obstructive pulmonary disease presented for a routine primary care appointment. He appeared to have severe hypoxia because of the generalized blue-gray discoloration of his skin and fingernails (Figures 1 and 2).
Figure 1.
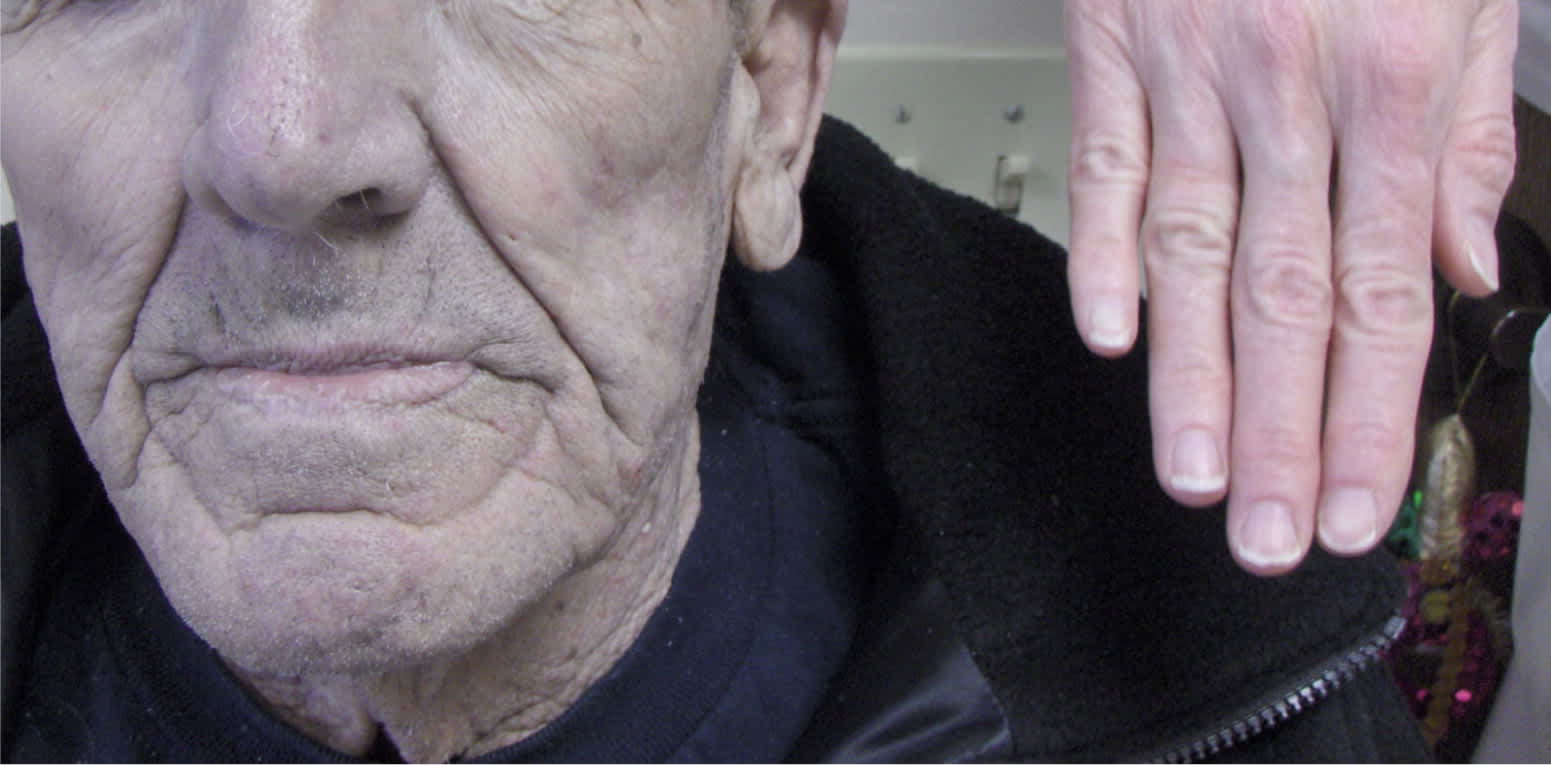
Figure 2.
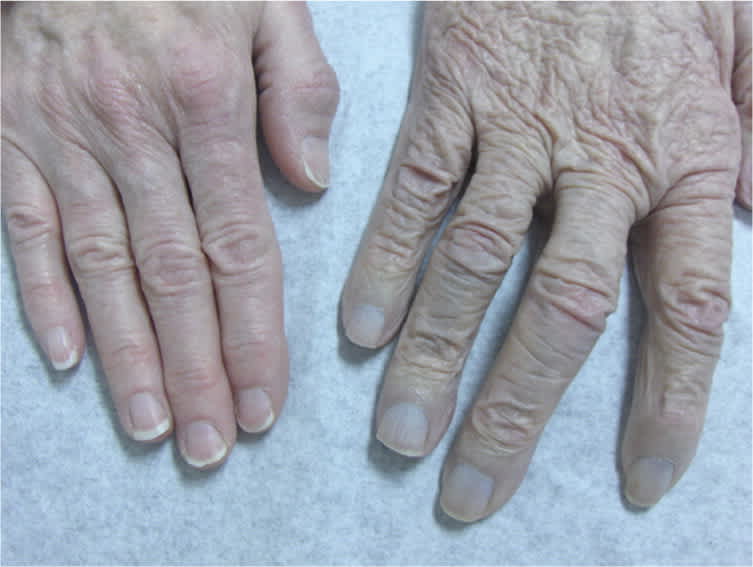
He had no history of heart disease or alcohol abuse. He had a history of drinking 3 to 4 oz of a colloidal silver solution daily to boost his immune system. After three years, the patient stopped taking the supplement. On physical examination, the patient was breathing comfortably and speaking in full sentences. His oxygen saturation was 95 percent on room air, and he had a barrel chest. Results of routine laboratory tests were normal.
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Addison disease.
B. Amiodarone-induced hyperpigmentation.
C. Argyria.
D. Hemochromatosis.
E. Polycythemia vera.
Discussion
The answer is C: argyria. Argyria is a rare skin condition associated with chronic exposure to products containing silver. The silver is typically deposited diffusely in skin, fingernails, oral mucosa, and conjunctival membranes.1
The skin discoloration associated with using colloidal silver is more pronounced in sun-exposed areas, such as the face and hands. It is thought to result from the reduction reaction of colorless silver in the dermis by sunlight exposure.2 Histologic examination shows silver granules in the dermis, which are particularly evident near the basal layer of sweat glands.3 There is no effective treatment for this condition, although silver chelating agents have been tried. Sun avoidance and use of sunscreen may be helpful in decreasing further skin discoloration. Other potential effects from consuming large doses of colloidal silver include agranulocytosis, pleural edema, and coma.4
Addison disease, or primary adrenal insufficiency, is most commonly caused by autoimmune destruction of the adrenal glands. The pituitary gland drives up production of adrenocorticotropic hormone levels to stimulate the adrenal glands, and melanocyte-stimulating hormone is also produced as a by-product. The increased melanin production causes skin hyperpigmentation with a “muddy” appearance.5 The hyperpigmentation is diffuse, but it is more pronounced on sun-exposed areas, scars, skinfolds, and pressure points (e.g., elbows, knees, knuckles, toes). Patients with Addison disease have hyponatremia and hyperkalemia.
Amiodarone is an iodinated compound used in the treatment of ventricular arrhythmias that are refractory to other medications. Several systemic and dermatologic adverse effects are attributed to amiodarone, including pulmonary fibrosis; thyroid abnormalities; fulminant hepatitis; keratitis; chronic anxiety reaction; photosensitivity; and cutaneous hyperpigmentation, which affects 2 to 5 percent of patients.6 The pigmentation is characterized clinically by progressive blue-gray discoloration of predominantly sun-exposed areas.
Hemochromatosis is characterized by inappropriately increased absorption and storage of dietary iron. It is one of the most common genetic errors of metabolism. Hemochromatosis is characterized by a diffuse slate-gray or bronze pigmentation in sun-exposed skin because of iron and melanin deposition. Disease onset generally occurs between 30 and 50 years of age. The condition affects men more often than women. Other findings include diabetes mellitus and a high serum iron level. Hemochromatosis is treated with repeated phlebotomy to reduce excessive iron stores.7
Polycythemia vera is a chronic myeloproliferative disorder characterized by increased red blood cell mass. It results in erythema of the skin and is classically known to cause pruritus after bathing. Polycythemia vera should be suspected in patients with elevated hemoglobin or hematocrit levels, splenomegaly, or portal venous thrombosis. Treatment includes phlebotomy with the possible addition of myelosuppressive agents based on risk stratification.8
Summary Table

| Condition | Characteristics |
|---|---|
| Addison disease | Autoimmune destruction of the adrenal glands causing a “muddy” appearance of the skin; hyperpigmentation most pronounced on sun-exposed areas, scars, skinfolds, and pressure points (e.g., elbows, knees, knuckles, toes); hyponatremia and hyperkalemia present |
| Amiodarone-induced hyperpigmentation | Blue-gray discoloration of sun-exposed skin |
| Argyria | Rare skin condition associated with prolonged use of silver-containing products; typically affects skin, fingernails, oral mucosa, and conjunctival membranes; histologic examination shows silver granules in the dermis, particularly in the basal layer of sweat glands |
| Hemochromatosis | Genetic error of metabolism; inappropriately increased absorption and storage of dietary iron causes a diffuse slate-gray or bronze pigmentation of sun-exposed skin |
| Polycythemia vera | Chronic myeloproliferative disorder causing erythema of the skin; classically known to cause pruritus after bathing |

