Case Scenario
A patient came to my office with a rash under her arm. I had seen her only once before for a refill of her diabetes mellitus medications. At that time, she was instructed to return for a comprehensive new-patient examination, which she never scheduled. On examination, her vital signs were unremarkable, her glucose level was 190 mg per dL (10.55 mmol per L), and she was obese, with a body mass index of 34 kg per m2. I noted an erythematous ring under the left axilla. I concluded that she had intertrigo and prescribed a cortisone/antifungal ointment. I asked her to come back if the rash did not resolve. Shortly afterward, I took a vacation. While I was away, the patient returned and saw my partner for what she described as pain in her joints, particularly her knees. My partner attributed the pain to arthritis caused by her obesity and prescribed ibuprofen. A few days after I returned, I received notice from a rheumatologist from whom my patient had sought further consultation for her rash. The note stated that my patient had been diagnosed with erythema migrans, that an initial Lyme titer had been positive, and that treatment for Lyme disease had been initiated. Looking back, I realize that the erythematous ring with central clearing was consistent with erythema migrans, even though the diagnosis of Lyme disease had not occurred to me. I am concerned that I missed this, although I have recently made some lucky guesses that have been life-saving for my patients. How can I make my diagnoses more reliable?
Commentary
Many medical errors have been identified as systemic and addressed with interventions, such as checklists.1 However, a substantial number of errors that occur in diagnosis and treatment are attributed to flaws in clinical reasoning.2 It is unknown how often such errors occur, but they are most common in primary care specialties. Some estimates suggest that diagnostic errors in emergency departments occur 5 to 10 percent of the time.2,3 In a setting where there is continuity of care, diagnostic error rates are likely lower.
Errors in diagnostic reasoning are often attributed to biases or heuristics (Table 13,4). Many biases are nothing more than practical diagnostic shortcuts and, in most cases, actually lead to correct decision making.4,5 A wide variety of diagnostic biases have been described in the literature. These include the notions that common diseases occur more often, and that a single diagnosis accounting for numerous symptoms is better than cobbling together several explanations. However, at times, pearls become pitfalls. They can lead to erroneous conclusions, as in this case scenario.
Table 1. Diagnostic Biases and Prevention Strategies
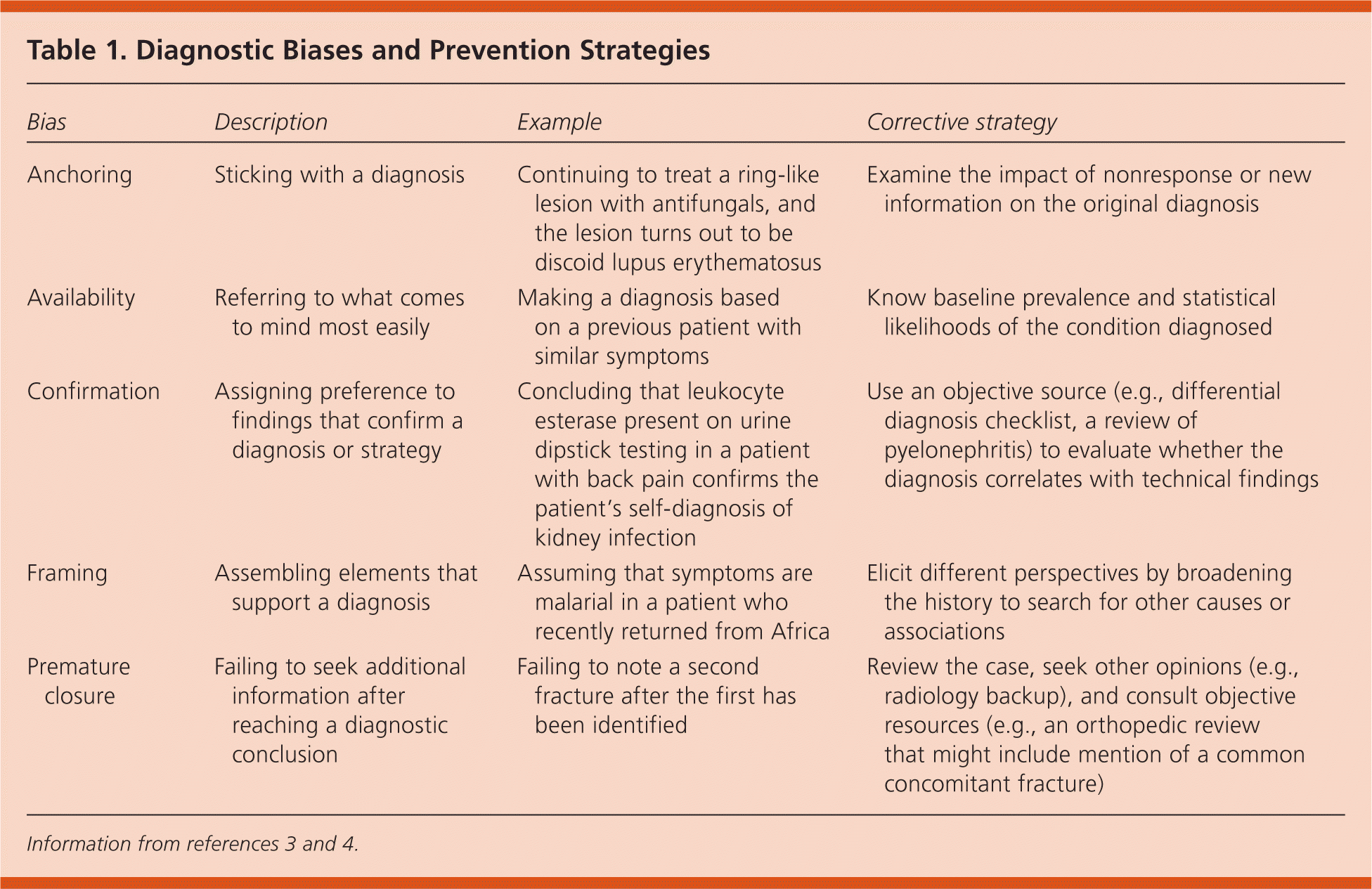
| Bias | Description | Example | Corrective strategy |
|---|---|---|---|
| Anchoring | Sticking with a diagnosis | Continuing to treat a ring-like lesion with antifungals, and the lesion turns out to bediscoid lupus erythematosus | Examine the impact of nonresponse or new information on the original diagnosis |
| Availability | Referring to what comes to mind most easily | Making a diagnosis based on a previous patient with similar symptoms | Know baseline prevalence and statistical likelihoods of the condition diagnosed |
| Confirmation | Assigning preference to findings that confirm a diagnosis or strategy | Concluding that leukocyte esterase present on urine dipstick testing in a patient with back pain confirms the patient's self-diagnosis of kidney infection | Use an objective source (e.g., differential diagnosis checklist, a review of pyelonephritis) to evaluate whether the diagnosis correlates with technical findings |
| Framing | Assembling elements that support a diagnosis | Assuming that symptoms are malarial in a patient who recently returned from Africa | Elicit different perspectives by broadening the history to search for other causes or associations |
| Premature closure | Failing to seek additional information after reaching a diagnosticconclusion | Failing to note a second fracture after the first has been identified | Review the case, seek other opinions (e.g., radiology backup), and consult objective resources (e.g., an orthopedic review that might include mention of a common concomitant fracture) |
This scenario demonstrates several biases that might interfere with making a correct diagnosis. One commonly described bias is known as the availability bias, which refers to the ease with which a particular answer comes to mind. For example, a physician might make a diagnosis based on a recent patient with similar symptoms. This bias often excludes diagnostic possibilities, as illustrated by this physician's failure to consider erythma migrans in the differential diagnosis.
Sometimes a constellation of findings (e.g., diabetes, obesity, and underarm rash) suggests one diagnosis more readily than another. This constellation then becomes a frame, which is a sort of narrative that disallows other diagnoses. Although the case scenario does not provide the patient history, another frame might have grouped erythematous rash with central clearing, tick bite, and endemic area. This frame would then have led to the correct pattern recognition. Disregarding the possibility of other diagnoses also can lead to premature closure. With this bias, the physician does not seek additional information after reaching a conclusion about a diagnosis.
Availability and framing biases may anchor a diagnosis in the physician's mind, making it hard to dislodge. When a patient does not respond to treatment, an anchoring bias would lead a physician to prescribe a stronger dose or a different formulation of a previously prescribed medication rather than consider another diagnosis. In this scenario, anchoring might have come into play when the partner evaluated the patient's joint pain. Rather than considering Lyme arthritis (although, in fact, a late finding), the physician might have assumed from the information in the patient's chart that any subsequent symptoms were related to one of the original findings (e.g., obesity). Relying on another physician's opinions illustrates the bias of groupthink, or blind obedience, in which an agreement is reached based on an authoritative source (e.g., laboratory and imaging test results) without sufficient examination. Another bias associated with diagnostic tests is the confirmation bias, which leads the interpreter to overemphasize findings that support the original diagnosis. As this discussion shows, there is considerable overlap among biases.
How can diagnostic errors be prevented? Unfortunately, it is easier to elucidate the barriers to error prevention than to remedy them. One barrier is that physicians often do not get feedback on errors. In this case, the physician learned of the error because the rheumatologist forwarded the test results, allowing the receiving physician to compare the results with the previous diagnosis. But this is likely the exception rather than the rule. Another barrier is the large number of shortcuts that physicians are expected to make every day because there simply is not enough time to evaluate every diagnosis.
Interventions to reduce diagnostic errors remain speculative, and there is no fail-safe approach. Advocates of metacognition suggest teaching the sources of biases and implementing mental awareness practices to counter them.6 In one study, reflective reasoning was found to reduce availability bias in residents.7 Physicians who analyzed a spectrum of diagnostic possibilities made a more accurate diagnosis than those who relied on a previous case with similar features. For practical use of a diagnostic checklist to reduce error, see the video profiled in the following blog posting: http://commonsensemd.blogspot.com/2011/05/checklists-and-decision-support-in.html. However, interventions such as this may make it difficult to work in a timely and efficient manner.8
In the case presented, the physician arranged for follow-up, but follow-up has limitations. For example, the rash might have disappeared, in which case the diagnosis might have been delayed despite further review. Little is known about whether point-of-care decision making reduces medical error; however, consulting a problem-oriented application on a handheld device would have provided a broader differential diagnosis. Involving team members, such as medical assistants or nurses, in a systematic way to gather historical elements or generate the differential diagnosis also may be helpful. To illustrate, in a newspaper report of a case involving a patient with Lyme arthritis, a nurse ultimately made the correct diagnosis when the patient's “mysterious ailment” was discussed during a staff meeting, but this was after the patient had undergone several unnecessary orthopedic surgeries.9 Although this approach has not been studied, many physicians are willing to offer a second opinion for a student, resident, or colleague to help reach a correct diagnosis.

