Original Article: Ulcer on Lower Lip of Deployed Serviceman [Photo Quiz]
Issue Date: March 1, 2011
Available at: https://www.aafp.org/afp/2011/0301/p601.html
to the editor: This Photo Quiz is a poor clinical representation of ecthyma (see accompanying figure). No Gram stain was performed to show gram-positive cocci, and no culture was obtained to confirm the species involved.
Figure.
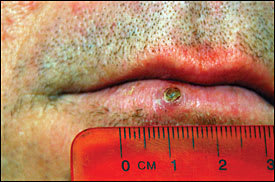
There is not enough clinical evidence to suggest involvement of the deep dermis or the presence of exudate that would be expected from a bacterial infection. The statement “the bump became firmer and slowly enlarged” is more suggestive of the normal healing process of a superficial erosion or wound of the skin than bacterial impetigo with invasion of the dermis. Lack of histologic and microbial findings suggests that the diagnosis is based on clinical findings alone.
A biopsy probably would have revealed normal granulation tissue and epithelization under a dry eschar. Near complete healing over four weeks (as shown in the photo) does not suggest ecthyma, and might simply indicate wound healing delayed by inability to dress the wound appropriately and exposure to saliva, food, and friction.
in reply: Thank you for your comments. Although this patient's presentation was not classic for ecthyma, given the details in this particular case, it is a relatively good example. Ecthyma can occur on mucosal surfaces, although they are not the most common site.
As stated in the history and physical examination discussion, the patient was deployed to an austere environment, and consultation was accomplished through the military's teledermatology network. In these situations, culture often is not available. In this particular case, the patient had a known shaving injury to his lip. The plan was to treat presumptively with an antibiotic with gram-positive coverage. If this was not successful, arrangements were in place to biopsy the patient's lesion. He responded rapidly and completely to treatment. Although scarring often results from ecthyma, a lip lesion such as this usually heals well.
In the military teledermatology network we receive hundreds of consults per year. An understanding of the environment unique to a service member is crucial to the development of a differential diagnosis and subsequent treatment. Given these considerations, I stand by the original diagnosis.

