Personality disorders have been documented in approximately 9 percent of the general U.S. population. Psychotherapy, pharmacotherapy, and brief interventions designed for use by family physicians can improve the health of patients with these disorders. Personality disorders are classified into clusters A, B, and C. Cluster A includes schizoid, schizotypal, and paranoid personality disorders. Cluster B includes borderline, histrionic, antisocial, and narcissistic personality disorders. Cluster C disorders are more prevalent and include avoidant, dependent, and obsessive-compulsive personality disorders. Many patients with personality disorders can be treated by family physicians. Patients with borderline personality disorder may benefit from the use of omega-3 fatty acids, second-generation antipsychotics, and mood stabilizers. Patients with antisocial personality disorder may benefit from the use of mood stabilizers, antipsychotics, and antidepressants. Other therapeutic interventions include motivational interviewing and solution-based problem solving.
Treatment of primary care patients who have challenging personality traits must be carefully managed by the family physician to ensure patient-centered quality medical care. Commonly encountered provocative patient behaviors include actions that are demanding, dependent, aggressive, angry, and manipulative; these behaviors often leave physicians feeling helpless, frustrated, irritated, or angry. Patients with personality disorders have increased utilization of primary care and mental health services.1,2
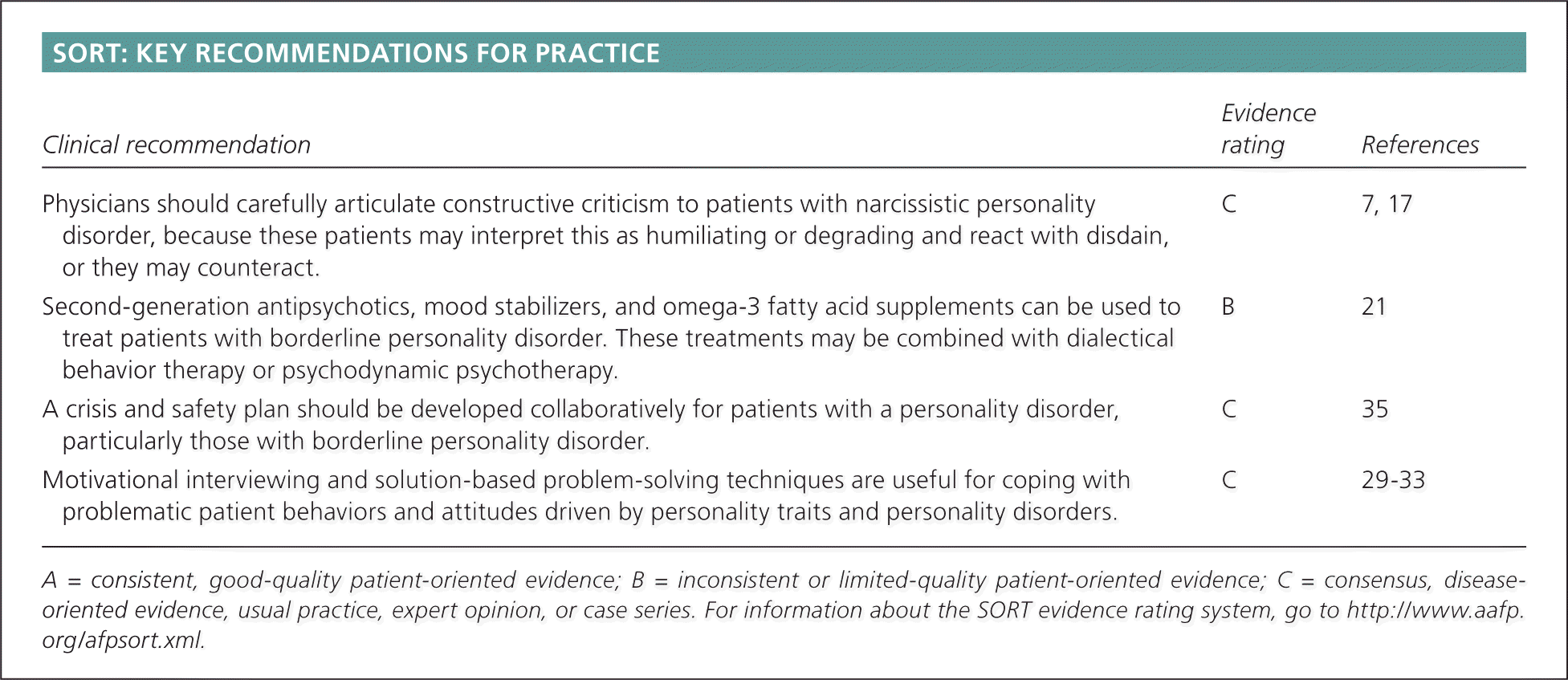
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Physicians should carefully articulate constructive criticism to patients with narcissistic personality disorder, because these patients may interpret this as humiliating or degrading and react with disdain, or they may counteract. | C | 7, 17 |
| Second-generation antipsychotics, mood stabilizers, and omega-3 fatty acid supplements can be used to treat patients with borderline personality disorder. These treatments may be combined with dialectical behavior therapy or psychodynamic psychotherapy. | B | 21 |
| A crisis and safety plan should be developed collaboratively for patients with a personality disorder, particularly those with borderline personality disorder. | C | 35 |
| Motivational interviewing and solution-based problem-solving techniques are useful for coping with problematic patient behaviors and attitudes driven by personality traits and personality disorders. | C | 29–33 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Personality disorders are an axis II diagnosis, allowing an axis I disorder (e.g., bipolar disorder) and a personality disorder to be listed concurrently for the same patient. Several studies have shown that personality disorders commonly occur with axis I diagnoses, which impact function and clinical prognosis.3–6 The Diagnostic and Statistical Manual of Mental Disorders, 4th ed., text rev. (DSM-IV-TR), defines personality disorder as “an enduring pattern of inner experience and behavior that deviates markedly from the expectations of the individual's culture.”7 The pattern is inflexible and pervasive across a broad range of personal and social situations; leads to clinically significant distress or impairment in social, occupational, or other important areas of functioning; is stable and of long duration; and has an onset traceable to at least adolescence or early adulthood.
Studies have reported that 9 to 14.8 percent of patients have at least one personality disorder.5,8 Many patients have multiple personality disorders or traits that span several types of disorders, and significant comorbidity exists with alcohol and chemical abuse, and with anger traits. Because the traits of personality disorders tend to be stable over time,9 these disorders have been considered not amenable to treatment; however, multiple treatments are now available, including cognitive behavior therapy, dialectical behavior therapy, mentalization-based therapy, transference-focused psychotherapy, and pharmacotherapy (e.g., typical and atypical antipsychotics, antidepressants, mood stabilizers10,11).12,13 Although these treatments have been studied for use in several personality disorders, most of the medical literature is limited to borderline personality disorder.
Personality Disorder Types
Personality disorders are classified into clusters A, B, and C. Cluster A, characterized as odd or eccentric personalities, includes paranoid, schizoid, and schizotypal personality disorders. Cluster B, characterized as dramatic, emotional, or erratic personalities, includes antisocial, borderline, histrionic, and narcissistic personality disorders. Cluster C disorders, characterized as anxious or fearful, are more prevalent and include avoidant, dependent, and obsessive-compulsive personality disorders.
CLUSTER A
Table 1 lists the DSM-IV-TR criteria for the cluster A personality disorders: schizoid (detachment from social relationships), schizotypal (acute discomfort with and reduced capacity for close relationships, as well as cognitive or perceptual distortions and behavioral eccentricities), and paranoid (pervasive distrust and suspiciousness of others).7
Table 1. Cluster A Personality Disorders

| Diagnostic Criteria for 301.0 Paranoid Personality Disorder |
A. A pervasive distrust and suspiciousness of others such that their motives are interpreted as malevolent, beginning by early adulthood and present in a variety of contexts, as indicated by four (or more) of the following:
|
| B. Does not occur exclusively during the course of schizophrenia, a mood disorder with psychotic features, or another psychotic disorder and is not due to the direct physiological effects of a general medical condition. |
| Diagnostic Criteria for 301.20 Schizoid Personality Disorder |
A. A pervasive pattern of detachment from social relationships and a restricted range of expression of emotions in interpersonal settings, beginning by early adulthood and present in a variety of contexts, as indicated by four (or more) of the following:
|
| B. Does not occur exclusively during the course of schizophrenia, a mood disorder with psychotic features, another psychotic disorder, or a pervasive developmental disorder and is not due to the direct physiological effects of a general medical condition. |
| Diagnostic Criteria for 301.22 Schizotypal Personality Disorder |
A. A pervasive pattern of social and interpersonal deficits marked by acute discomfort with, and reduced capacity for, close relationships as well as by cognitive or perceptual distortions and eccentricities of behavior, beginning by early adulthood and present in a variety of contexts, as indicated by five (or more) of the following:
|
| B. Does not occur exclusively during the course of schizophrenia, a mood disorder with psychotic features, another psychotic disorder, or apervasive developmental disorder. |
Reprinted with permission from American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 4th ed., text rev. Copyright © 2000. Washington, DC: American Psychiatric Association; 2000:694, 697, 701.
The prevalence of schizoid personality disorder ranges from 0.5 to 7 percent in the general population to as high as 14 percent in the homeless population.5,14,15 Physicians may have difficulty establishing and maintaining a relationship with these patients, who may not respond to stimuli in a typical way.16 Because persons with schizotypal personality disorder have intense anxiety in social situations with unfamiliar people, it is important to establish a therapeutic relationship.16 The physician should adopt a professional stance, provide clear explanations, tolerate odd beliefs and behaviors, and avoid overinvolvement in the patient's personal or social issues.17
Approximately 3 percent of the U.S. population has schizotypal personality disorder.5 This disorder may have a genetic component and may be a clinical precursor to schizophrenia. Numerous pharmacotherapies have been suggested for certain subtypes of this disorder, whereas patients with other subtypes may be more responsive to psychosocial intervention.18
Paranoid personality disorder has a prevalence of 0.5 to 2.5 percent in the general population, 2 to 10 percent among persons in outpatient settings, and 10 to 30 percent among persons in inpatient psychiatric settings.7 These patients are difficult to engage in a therapeutic relationship for medical or mental health issues. Physicians should provide a formal, honest, and professional discussion without being too friendly, too warm, or too humorous. Physicians should expect belittling comments, accusations, and potentially litigious threats from these patients, yet they should allow these patients to express grievances without confirming or confronting the paranoid beliefs.17,19
CLUSTER B
There are four cluster B personality disorders: borderline (instability of interpersonal relationships and self-image, with marked impulsivity), histrionic (excessive emotionality and attention-seeking behavior), antisocial (disregard for and violation of the rights of others), and narcissistic (grandiosity, need for admiration, and lack of empathy). The diagnostic criteria from DSM-IV-TR are listed in Table 2.7
Table 2. Cluster B Personality Disorders

| Diagnostic Criteria for 301.7 Antisocial Personality Disorder |
A. There is a pervasive pattern of disregard for and violation of the rights of others occurring since age 15 years, as indicated by three (or more) of the following:
|
| B. The individual is at least age 18 years. |
| C. There is evidence of conduct disorder with onset before age 15 years. |
| D. The occurrence of antisocial behavior is not exclusively during the course of schizophrenia or a manic episode. |
| Diagnostic Criteria for 301.83 Borderline Personality Disorder |
A pervasive pattern of instability of interpersonal relationships, self-image, and affects, and marked impulsivity beginning by early adulthood and present in a variety of contexts, as indicated by five (or more) of the following:
|
| Diagnostic Criteria for 301.50 Histrionic Personality Disorder |
A pervasive pattern of excessive emotionality and attention seeking, beginning by early adulthood and present in a variety of contexts, as indicated by five (or more) of the following:
|
| Diagnostic Criteria for 301.81 Narcissistic Personality Disorder |
A pervasive pattern of grandiosity (in fantasy or behavior), need for admiration, and lack of empathy, beginning by early adulthood and present in a variety of contexts, as indicated by five (or more) of the following:
|
Reprinted with permission from American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders . 4th ed., text rev. Copyright © 2000. Washington, DC: American Psychiatric Association; 2000:706, 710, 714, 717.
Borderline personality disorder has a prevalence of 1.6 percent in the general population.5 It is the most studied and has the most detailed treatment recommendations,20 usually involving a multimodal approach and numerous components of psychotherapy.12 A recent Cochrane review found that second-generation antipsychotics, mood stabilizers, and dietary supplementation with omega-3 fatty acids have some beneficial effects in patients with borderline personality disorder. Treatment with antidepressants is not widely supported for patients with this disorder, but it may be helpful in those with comorbid conditions.21 Physicians should avoid excessive familiarity with these patients because it can lead to mistrust. In addition, physicians should understand that although angry outbursts may occur, limits must be set, a venue for frequent follow-up (e.g., telephone or office visits) must be created, and clear explanations without technical jargon must be provided.17
Histrionic personality disorder has a prevalence that ranges from less than 1 percent to 3 percent.5,22 Patients with this disorder can present multiple challenges; they require empathy with boundary setting to limit potentially manipulative behaviors, such as suicidal gestures.22 Emphasizing objective data while maintaining a professional concern for the patient's feelings and emotions may be helpful.17
Antisocial personality disorder has a prevalence of 1 percent in the general population.5 It is associated with substance abuse, acute anxiety, delusional states, and factitious disorders.22 Medications such as mood stabilizers, atypical antipsychotics, and antidepressants may have some effect on the anxiety, impulsivity, and anger components of this disorder.10 However, a recent Cochrane review did not definitively show that pharmacologic treatment is effective.23 This disorder may have social, legal, and financial implications; therefore, multiple treatment options must be considered. Because of the risk of manipulative behaviors by the patient, the physician should use caution (especially in dealing with new, ill-defined illnesses), be fair and consistent, and set clear limits.17
Although only 1 percent of patients in the general population meet the full diagnostic criteria for narcissistic personality disorder, it is present in 2 to 16 percent of the clinical population.5 These patients can be demanding, with an attitude of entitlement and “specialness,” but the physician should focus on concrete points and attempt to channel patient traits into improving their health.17 Several medications are helpful in treating components of this disorder, such as anger and mood lability.10 When diagnosing and treating patients with narcissistic personality disorder, physicians must acknowledge that the patient's behavior is protective of his or her sense of internal control and self-esteem.24 Narcissistic functioning has two components: external and internal. External functioning serves as a protective armor (e.g., self-enhanced and self-preoccupied, controlling, insensitive, critical, aggressive, condescending, provocative), whereas internal functioning indicates vulnerability, dysregulation, and compromised abilities (e.g., low self-esteem, self-criticism, insecurity, inferiority, loneliness, isolation, hypersensitivity, fear, rage, shame). As such, constructive criticism to patients with narcissistic personality disorder should be carefully worded, because these patients may interpret this as humiliating or degrading and react with disdain, or they may counteract.7,17
CLUSTER C
Table 3 lists the DSM-IV-TR diagnostic criteria for the three cluster C personality disorders: avoidant (social inhibition, feelings of inadequacy, and hypersensitivity to negative evaluation), obsessive-compulsive (preoccupation with orderliness, perfectionism, and mental and interpersonal control), and dependent (submissive and clinging behavior, and fears of separation).7
Table 3. Cluster C Personality Disorders

| Diagnostic Criteria for 301.82 Avoidant Personality Disorder |
A pervasive pattern of social inhibition, feelings of inadequacy, and hypersensitivity to negative evaluation, beginning by early adulthood and present in a variety of contexts, as indicated by four (or more) of the following:
|
| Diagnostic Criteria for 301.6 Dependent Personality Disorder |
A pervasive and excessive need to be taken care of that leads to submissive and clinging behavior and fears of separation, beginning by early adulthood and present in a variety of contexts, as indicated by five (or more) of the following:
|
| Diagnostic Criteria for 301.4 Obsessive-Compulsive Personality Disorder |
A pervasive pattern of preoccupation with orderliness, perfectionism, and mental and interpersonal control, at the expense of flexibility, openness, and efficiency, beginning by early adulthood and present in a variety of contexts, as indicated by four (or more) of the following:
|
Reprinted with permission from American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 4th ed., text rev. Copyright © 2000. Washington, DC: American Psychiatric Association; 2000:721, 725, 729.
Avoidant personality disorder occurs in 5.2 percent of the general population5 and is common in persons with social phobia.22 Pharmacotherapy and psychotherapy may provide some benefit.25 Patients with avoidant personality disorder routinely respond to direct questions with “I'm not sure,” and may seem evasive. Encouraging the patient in a nonjudgmental manner to report symptoms and validating the patient's concerns are helpful.17
Obsessive-compulsive personality disorder is present in approximately 2.4 percent of the general population5 and is often confused with obsessive-compulsive disorder, which is an axis I diagnosis. Patients with this personality disorder generally exhibit traits that are somewhat adaptive and supportive of the ego and are seldom distressing, whereas patients with obsessive-compulsive disorder tend to have recurrent unpleasant thoughts and ritualized behaviors. Patients with obsessive-compulsive personality disorder tend to fear losing control and have increased attention to detail, to the point of missing the bigger picture. Physicians should be thorough with examinations and explanations, but should not focus on variables or uncertainties.17 Psychotherapeutic therapies, including short-term inpatient therapy, have been successful for patients with obsessive-compulsive personality disorder.26 Treatment with selective serotonin reuptake inhibitors may be helpful, especially if anxiety is present.27
Dependent personality disorder is the least prevalent of the cluster C disorders; it occurs in 0.6 percent of the general population5 and is more common in victims of spousal abuse.28 Physicians should provide reassurance and schedule routine follow-up (e.g., telephone or office visits) with the understanding that the patient may feel that urgent evaluations are necessary based on his or her sense of need, rather than on the medical necessity of the situation.17
Problem-Focused Office Management Tools
Family physicians may be more effective and optimistic when armed with concrete problem-focused tools that can be used in the 15-minute clinical visit. These tools are designed to avoid being drawn into the patient's pathologic personality traits, which often results in conflict. The techniques should be user-friendly, nonconfrontational, practical for use in a single patient visit or longitudinal continuity of care, and effective in primary care.
One tool is a modified version of motivational interviewing, which has been proven effective in adults29 and children30 (Table 4). The hypothetical patient is an example of a help-rejecter who exemplifies a cluster B mixture of the borderline and histrionic personality disorder types. The second tool is the problem-solving technique 31 (Table 5). For illustrative purposes, the step-by-step presentation uses a dependent, clinging patient who displays a combination of symptoms of dependent and avoidant personality disorders. The motivational interviewing and problem-solving techniques are useful for coping with problematic patient behaviors and attitudes driven by personality traits and personality disorders.32,33
Table 4. Step-by-Step Implementation of Motivational Interviewing

| Step | Example |
|---|---|
| 1. Ask for permission to discuss the problem. Intent is to increase awareness of a problem that the patient is avoiding or denying. | “I'm concerned about our working relationship because it seems that you often dismiss my medical advice, but continue to ask for recommendations. Would it be okay for us to talk about this now?” |
| 2. Elicit talk about change. Intent is to evoke thoughts about the disadvantages of the status quo, the advantages of change, specific change possibilities, and taking the first step toward change. | “What do you think will happen if the pattern of dismissing medical advice does not change?” |
| “What could work for you if you decided to change?” | |
| “What might be some good things about changing?” | |
| “What would you be willing to try as a first step?” | |
| 3. Importance check. Intent is to have the patient rate his or her readiness and motivation to embrace behavior change, and to reinforce talk about change. | “On a scale of 1 to 10, with 1 being the lowest and 10 being the highest, how important is it for you to change the pattern that we have been discussing and to try the new approach?” |
| 4. Ability check. Intent is to assess the patient's confidence in his or her ability to change and to overcome barriers to change. | “On a scale of 1 to 10, how confident are you that you will succeed in making a behavior change?” |
| “What do you see as barriers to becoming more self-confident and to independently making informed choices, and how might you overcome these obstacles?” | |
| 5. Statement to terminate the motivational interview for today. Intent is to summarize the main discussion points, the patient's commitment to change, and the follow-up plan. It is important to state what the patient has agreed to, but also what he or she has not agreed to. | “If I may summarize our discussion, the problem in our working relationship appears to be the pattern of dismissing medical advice. You are motivated to make changes with my encouragement, and you are specifically going to work on________.” |
| “Let's talk about this again in a couple of weeks to check on your progress, to talk about how you are coping with barriers to change, and to modify the solution a bit, if necessary.” |
Table 5. Step-by-Step Implementation of Problem Solving

| Step | Example |
|---|---|
| 1. Problem identification. Intent is to identify a specific problem that the physician perceives as interfering with good medical care. | “What is the problem here?” |
| “What needs to be fixed?” | |
| 2. Consider multiple potential solutions. Intent is to collaboratively consider and brainstorm alternative solutions to the agreed-on problem. | “What might you do differently so that less care or support from others will not prevent you from following medical advice?” |
| “What are the possible consequences of each option that was identified in our brainstorming discussion?” | |
| 3. Seek patient commitment. Intent is to get a commitment from the patient to try a new and preferred solution and to set a starting time. | “Which of these solutions are you willing to try?” |
| “Please state exactly what you are going to do and when.” | |
| “When are you willing to start?” | |
| 4. Summary statement. Intent is to summarize the main points of the discussion and schedule follow-up to assess outcomes so that the patient is not put off if the first solution does not work; to address new barriers that may arise; to encourage the patient to apply the solution consistently; and to model positive self-reinforcement for small initial success. | “If I may summarize our discussion, the problem seems to be a lack of self-confidence and, perhaps, a fear of disapproval when you need to make decisions about your medical care. These lead to being too dependent on others for making choices. You are willing to try a new solution or plan with my encouragement, and you are specifically going to do________ starting _________. Does this summarize the plan fairly?” |
| “Let's talk about this again in a couple of weeks to check on your progress, to talk about how you are coping with barriers to change, and to modify the solution a bit, if necessary.” |
A core strategy for family physicians is an intervention based on active listening, mindfulness, and strengthening the connection to the patient's most cherished values. This intervention was designed for family physicians and addresses the concerns of emotional endurance and job satisfaction while caring for patients with personality disorders.34 When treating patients with a personality disorder, physicians should consider a collaboratively developed crisis and safety plan, particularly for those with borderline personality disorder.35
Because of the longitudinal nature of the expression of personality disorders and the continuity of primary care, family physicians should understand the frequency and characteristics of these disorders and their implications on the interpersonal relationship between the physician and patient. As effective treatments for personality disorders continue to emerge, family physicians can direct treatment and improve long-term patient care.
Data Sources: PubMed and Google Scholar were searched using the keywords personality disorders and the individual personality disorders: cluster A, cluster B, cluster C, paranoid, schizoid, schizotypal, antisocial, borderline, histrionic, narcissistic, avoidant, dependent, and obsessive-compulsive. For each disorder, the search included treatments, guidelines, reviews, and psychotherapies. The search was not restricted to a particular timeline; however, the most recent peer-reviewed articles were identified from among the search results. Diagnostic criteria from the DSM-IV-TR and suggested diagnostic criteria from the Diagnostic and Statistical Manual of Mental Disorders, 5th ed., were also reviewed. Data sources included peer-reviewed manuscripts, published books, and Cochrane reviews. Search period: September and October 2010.

