Although falls are a common cause of injury in older persons, they are not just a normal part of the aging process. The American Geriatrics Society and British Geriatrics Society recommend that all adults older than 65 years be screened annually for a history of falls or balance impairment. An individualized risk assessment should be performed, with corresponding multifactorial intervention, for those who report a single fall and have unsteadiness; who report two or more falls; who report difficulties with gait or balance; or who seek medical attention because of a fall. The following components should be included in multifactorial interventions: exercise, particularly balance, strength, and gait training; modification of the home environment; minimization of medications, especially psychoactive medications; management of postural hypotension; and management of foot problems and footwear. These interventions are effective in decreasing falls and fall-related injuries in the community and nursing home settings, as well as in decreasing the number of persons who fall in the subacute hospital setting. Prevention of falls and, most importantly, of injury and death is possible. An evidence-based fall prevention prescription may be used to efficiently accomplish management.
The risk of falls and resulting serious injury increases with age, but falls are not an unavoidable consequence of aging. A history of falls is associated with a two- to sixfold increased risk of a future fall.1 Noninjurious falls are a harbinger of potentially life-threatening events, and an opportunity for physicians to intervene. Falls are the leading cause of death from injury in persons older than 65 years,2 and mortality from falls has increased by 42 percent over the past decade.3 Approximately 25 percent of persons who fall have moderate to severe injuries, ranging from bruises or lacerations to hip fractures or traumatic brain injury, resulting in more than 1.9 million emergency department visits annually.2 Injuries, such as hip fracture, and falls are risk factors for placement in a nursing home,4 where the fall risk is nearly three times that of persons living in the community.5
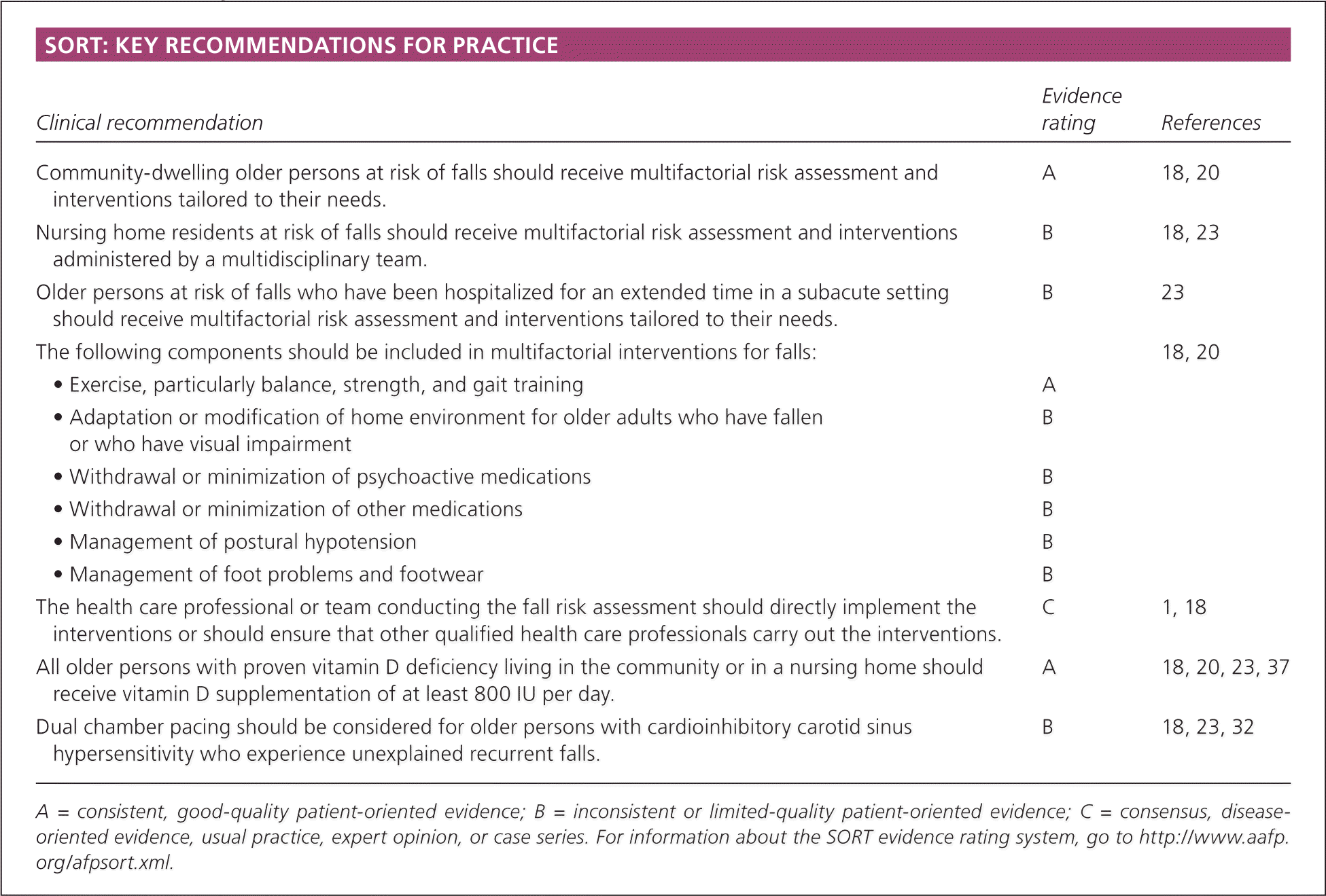
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References | |
|---|---|---|---|
| Community-dwelling older persons at risk of falls should receive multifactorial risk assessment and interventions tailored to their needs. | A | 18, 20 | |
| Nursing home residents at risk of falls should receive multifactorial risk assessment and interventions administered by a multidisciplinary team. | B | 18, 23 | |
| Older persons at risk of falls who have been hospitalized for an extended time in a subacute setting should receive multifactorial risk assessment and interventions tailored to their needs. | B | 23 | |
| The following components should be included in multifactorial interventions for falls: | 18, 20 | ||
| • Exercise, particularly balance, strength, and gait training | A | ||
| • Adaptation or modification of home environment for older adults who have fallen or who have visual impairment | B | ||
| • Withdrawal or minimization of psychoactive medications | B | ||
| • Withdrawal or minimization of other medications | B | ||
| • Management of postural hypotension | B | ||
| • Management of foot problems and footwear | B | ||
| The health care professional or team conducting the fall risk assessment should directly implement the interventions or should ensure that other qualified health care professionals carry out the interventions. | C | 1, 18 | |
| All older persons with proven vitamin D deficiency living in the community or in a nursing home should receive vitamin D supplementation of at least 800 IU per day. | A | 18, 20, 23, 37 | |
| Dual chamber pacing should be considered for older persons with cardioinhibitory carotid sinus hypersensitivity who experience unexplained recurrent falls. | B | 18, 23, 32 | |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Multifactorial risk assessment and intervention strategies are effective in decreasing the rate of falls and have a similar risk reduction to that of other prevention measures, such as statins for cardiovascular disease.6 This article provides a tool for management of this often preventable problem in older persons—an evidence-based prescription for decreasing falls.
Risk Factors
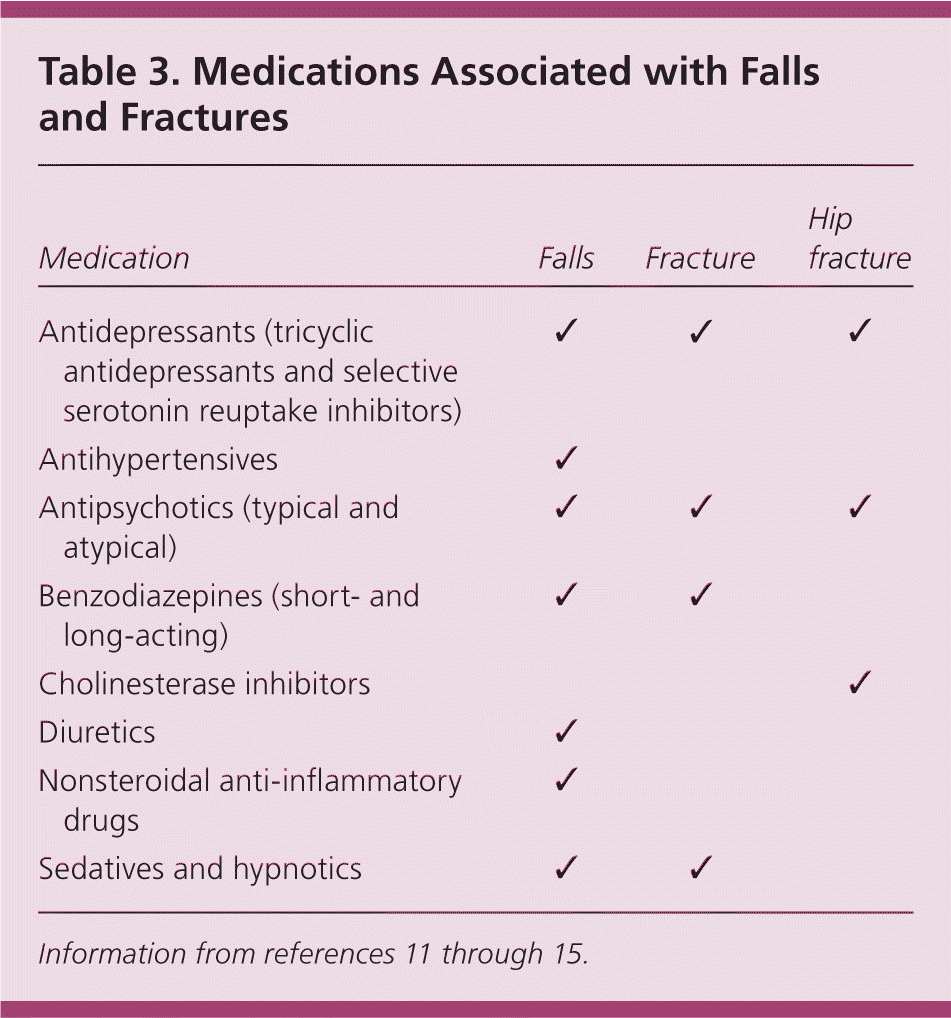
There are many risk factors for falls, some of which are modifiable (Tables 1,1,7 2,1,8–10 and 311–15 ). The strongest modifiable risk factors are balance impairment, gait impairment, and muscle weakness. A history of a fall is predictive of another fall.1,5,16 Fear of falling can result in a downward cascade of events leading to social isolation and loss of function, as well as more falls.8 Increased physical activity and the use of restraints, in addition to other risk factors listed in Tables 1,1,7 2,1,8–10 and 3,11–15 increase the risk of injurious falls.16 Approximately 60 percent of falls are the result of multiple factors17; therefore, persons who have fallen require multifactorial assessment and intervention.
Table 1. Nonmodifiable Risk Factors for Falls in Older Persons
Table 2. Potentially Modifiable Risk Factors for Falls in Older Persons

| Environmental hazards | |
| Medications (especially psychoactive [Table 3]) | |
| Polypharmacy (four or more prescription medications) | |
| Metabolic factors | |
| Dehydration | |
| Diabetes mellitus | |
| Low body mass index | |
| Vitamin D deficiency | |
| Musculoskeletal factors | |
| Balance impairment | |
| Foot problems | |
| Gait impairment | |
| Impaired activities of daily living | |
| Lower extremity muscle weakness | |
| Musculoskeletal pain | |
| Use of assistive device | |
| Neuropsychologic factors | |
| Delirium | |
| Depression | |
| Dizziness or vertigo | |
| Fear of falling8 | |
| Parkinson disease | |
| Peripheral neuropathy | |
| Sensory impairment | |
| Auditory impairment | |
| Multifocal lens use | |
| Visual impairment | |
| Other | |
| Acute illness | |
| Alcohol intoxication | |
| Anemia9 | |
| Cardiac arrhythmia | |
| Inappropriate footwear | |
| Obstructive sleep apnea10 | |
| Orthostatic hypotension | |
| Urinary incontinence | |
Table 3. Medications Associated with Falls and Fractures
| Medication | Falls | Fracture | Hip fracture |
|---|---|---|---|
| Antidepressants (tricyclic antidepressants and selective serotonin reuptake inhibitors) | ✓ | ✓ | ✓ |
| Antihypertensives | ✓ | ||
| Antipsychotics (typical and atypical) | ✓ | ✓ | ✓ |
| Benzodiazepines (short- and long-acting) | ✓ | ✓ | |
| Cholinesterase inhibitors | ✓ | ||
| Diuretics | ✓ | ||
| Nonsteroidal anti-inflammatory drugs | ✓ | ||
| Sedatives and hypnotics | ✓ | ✓ |
Assessment
According to the American Geriatrics Society (AGS) and British Geriatrics Society (BGS) 2010 clinical practice guidelines, all patients older than 65 years should be asked annually about whether they have fallen, the number of falls they have had, and whether they have difficulty walking or with balance.18 A gait and balance evaluation should be performed in every person who reports a single fall using one of the following tools: the Get Up and Go test, the Timed Get Up and Go test, the Berg Balance Scale (http://www.fallpreventiontaskforce.org/pdf/BergBalanceScale.pdf), or the Performance-Oriented Mobility Assessment (http://web.missouri.edu/~proste/tool/Tinetti-Balance-Gait--POMA.rtf).18 There is not enough evidence to suggest superiority of one test over another, but the Get Up and Go test is the most time-efficient, taking less than one minute to administer.1 With this test, the person is asked to get out of a chair without the use of his or her arms (if possible), walk 10 ft (3 m), turn, return to the chair, and sit down. If the person has unsteadiness or is not able to get out of the chair without the use of his or her arms, this suggests muscle weakness and a need for further assessment. In a timed version of this test, a person 60 to 69 years of age should be able to complete this walk in 9 seconds, a person 70 to 79 years of age in 10.2 seconds, and a person 80 to 99 years of age in 12.7 seconds. Slower times warrant further assessment.19
A multifactorial fall risk assessment should be performed in all older persons who report a single fall and have unsteadiness on gait examination; who report two or more falls; who report difficulties with gait or balance; or who seek medical attention because of a fall18 (Figure 118,20; Table 418,20–24 ). When possible, corroboration of the history by a caregiver (by telephone, if necessary) is useful because patients may overestimate their functional capabilities or may have underlying cognitive impairment. The history should include circumstances, frequency, associated symptoms, injuries, medication review (prescribed and over-the-counter), other relevant acute or chronic medical problems, assessment of activities of daily living and use of assistive devices, and fear of falling.18 The physical examination should include detailed gait assessment using one of the previously mentioned gait tests and including tandem and semitandem stance; evaluation of muscle strength; neurologic examination; cardiovascular examination, including postural blood pressure; assessment of visual acuity; and examination of the feet and footwear.18 An environmental assessment, including home safety, is also recommended.18 Any person seeking medical attention or presenting to the emergency department because of a fall should be carefully evaluated for underlying acute illness. The health care professional or team conducting the fall risk assessment should directly implement the interventions or should ensure that other qualified health care professionals carry out the interventions.1,18
Figure 1. Prevention of Falls in Community-Dwelling Older Adults
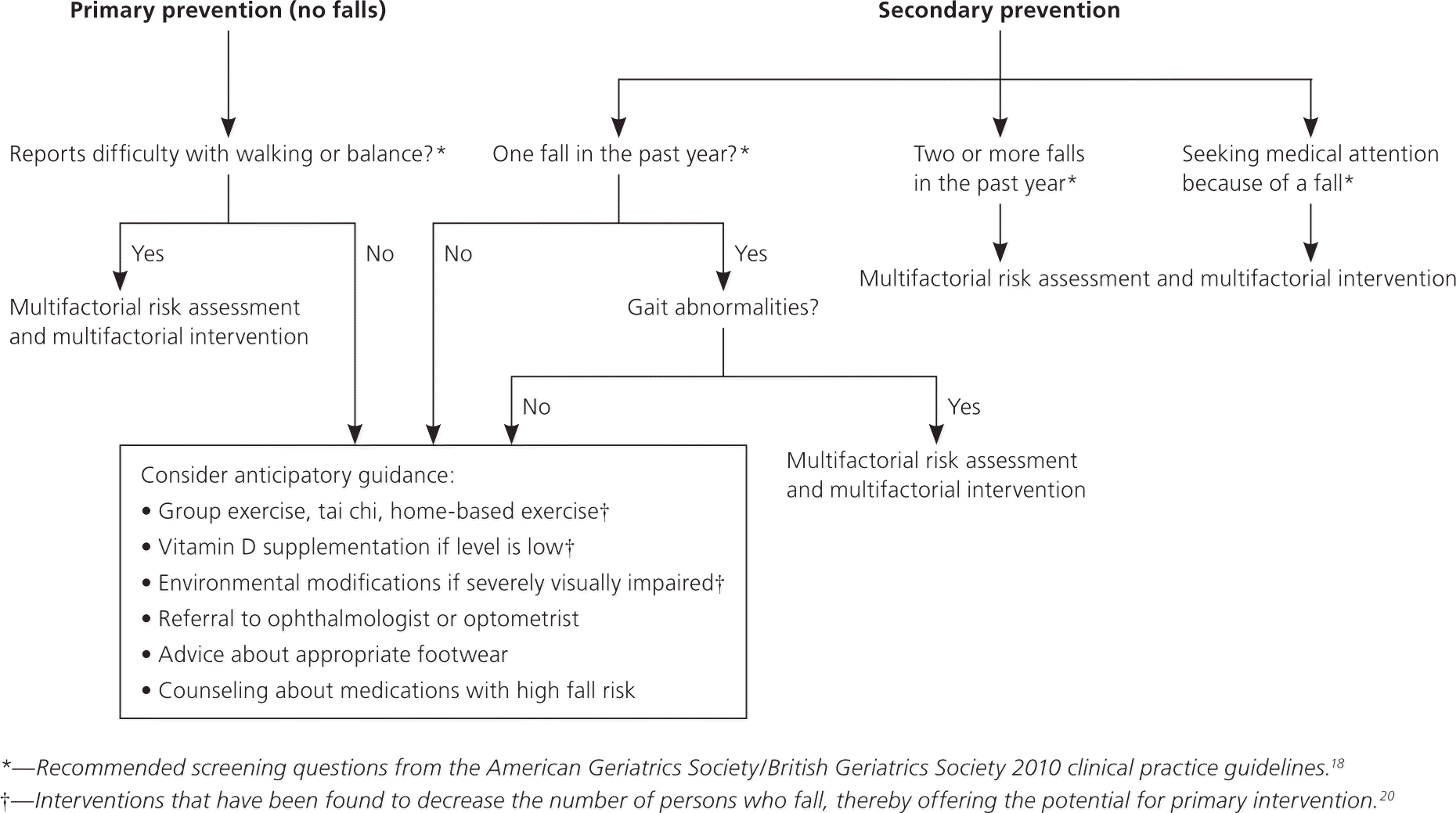
Algorithm for primary and secondary prevention of falls in community-dwelling older adults.
Information from references 18 and 20.
Table 4. Evaluation and Management of Falls in Older Persons
| Multifactorial risk assessment | Management | ||
|---|---|---|---|
| History | Physical examination and laboratory evaluation | Intervention | Evidence for intervention in these clinical settings |
| Evaluate injury | Treatment of acute underlying condition or chronic musculoskeletal or neurologic disease | Multifactorial intervention in community, hospital, or nursing home |
| Consider complete blood count and chemistry panel, especially if presenting with an acute fall | |||
| Consider dual energy x-ray absorptiometry | Treatment of osteoporosis | Decreased hip fractures in single interventions |
| Evaluate the environment in the home (QI) or in the hospital or nursing home (at the time of the fall, if possible) | Environmental hazard modification (QI) | AGS/BGS guidelines in community or nursing home; multifactorial intervention in community, hospital, or nursing home |
| Home safety intervention in high-risk persons (previous fall or at least one risk factor) | ↓ rate / ↓ risk in single intervention in community | ||
| Home safety intervention in persons with severe visual impairment | ↓ rate / ↓ risk in single intervention in community | ||
| Check for toxicity of medications, such as digoxin or anticonvulsants; check 25-hydroxyvitamin D level | Medication reduction, especially psychotropic medications (QI*) | AGS/BGS guidelines in community or nursing home; multifactorial intervention in community, hospital, or nursing home |
| Prescribing modification program for primary care physicians21 | ↓ risk in single intervention in community | ||
| Vitamin D supplementation if vitamin D level is low | AGS/BGS guidelines in community or nursing home; multifactorial intervention in community, hospital, or nursing home; ↓ rate/↓ risk in single intervention in community; ↓ rate in single intervention in nursing home | ||
| Vitamin D supplementation of at least 800 IU per day for those at increased risk of falls (regardless of vitamin D levels) | AGS/BGS guidelines in community or nursing home | ||
| Obtain postural blood pressure and pulse, especially if any dizziness or suggestion of fall associated with change in position (QI) | Treatment of orthostatic hypotension (treat underlying causes, if possible) | AGS/BGS guidelines in community; multifactorial intervention in community, hospital, or nursing home |
| Check cardiac examination (electrocardiography if syncope suggested) | Treatment of cardioinhibitory carotid sinus hypersensitivity with cardiac pacing | AGS/BGS guidelines in community; multifactorial intervention in community or nursing home; ↓ rate in single intervention in community |
| Examine feet and footwear | Advice about appropriate footwear (shoes with low heel height and high surface contact area) | AGS/BGS guidelines in community; multifactorial intervention in community or hospital |
| Management of foot problems/referral to podiatrist when necessary | AGS/BGS guidelines in community; multifactorial intervention in community or nursing home | ||
| Antislip shoe device used in icy conditions20 | ↓ rate in single intervention in community | ||
| Check neurologic examination and cognitive status (QI) with tool such as Mini-Mental State Examination; complete blood count, chemistry panel, urinalysis, chest radiography if signs and symptoms of acute illness are present | Treat underlying precipitants of delirium, such as infection | Multifactorial intervention in hospital |
| Nonpharmacologic management of confusion by nursing staff | Multifactorial intervention in hospital | ||
| Examine muscle strength, and gait and balance with the Get Up and Go test, Timed Get Up and Go test, Berg Balance Scale, or Performance-Oriented Mobility Assessment (QI) | If balance or gait is impaired: | |
| Physical therapy for gait and balance training/assistive device recommendations (QI) | AGS/BGS guidelines in community or nursing home; multifactorial intervention in community, hospital, or nursing home | ||
| Multiple component group exercise targeting at least two of the following: strength, balance, flexibility, endurance | AGS/BGS guidelines in community; multifactorial intervention in community; ↓ rate / ↓ risk in single intervention in community | ||
| Tai chi group exercise (strength and balance) | AGS/BGS guidelines in community; multifactorial intervention in community; ↓ rate / ↓ risk in single intervention in community | ||
| Multiple component home-based exercise targeting at least two of the following: strength, balance, flexibility, endurance | AGS/BGS guidelines in community; multifactorial intervention in community; ↓ rate / ↓ risk in single intervention in community | ||
| Supervised strengthening with or without gait and balance exercise program (QI) | AGS/BGS guidelines in nursing home ; multifactorial intervention in hospital or nursing home; ↓ risk in single intervention in hospital | ||
| Hip protectors | Multifactorial intervention in hospital or nursing home | ||
| Check visual acuity (QI) | Referral to ophthalmologist or optometrist | Multifactorial intervention in community, hospital, or nursing home |
| Use of eyewear | Multifactorial intervention in community or hospital | ||
| Expedited cataract surgery for first eye22 | AGS/BGS guidelines in community; ↓ rate in single intervention in community | ||
| Avoidance of use of multifocal lenses while climbing stairs or walking | AGS/BGS guidelines in community | ||
| — | Reduction of restraints | Decreased injurious falls in single intervention in nursing home |
| — | Patient and family education | AGS/BGS guidelines in community or nursing home; multifactorial intervention in community, hospital, or nursing home |
| — | Staff education | AGS/BGS guidelines in community or nursing home; multifactorial intervention in hospital or nursing home |
note: According to the AGS/BGS guidelines, multifactorial fall risk assessment should be performed and interventions (tailored to the identified risk factors), including an appropriate exercise program, should be provided to all community-dwelling older adults; both should be considered in long-term care.18 Based on evidence from the Cochrane database, multifactorial fall risk assessment and interventions (tailored to the identified risk factors) should be performed in the community20 and acute/subacute hospital settings,23 and through use of a multidisciplinary team in the nursing home setting.23 QI apply to the community setting unless otherwise specified.24
AGS = American Geriatrics Society; BGS = British Geriatrics Society; QI = Assessing Care of Vulnerable Elders quality indicators; ↓ rate = significantly decreased rate and number of falls20,23 ; ↓ risk = significantly decreased number of persons who fall (primary prevention).20,23
*—Benzodiazepine reduction or discontinuation.
†—Recommended with caution in the nursing home setting. 18
Multifactorial vs. Single Interventions
In each setting (community, hospital, and nursing home), individualized assessment with corresponding multifactorial intervention tailored to the needs of the patient and involving a combination of components (e.g., gait and balance training, medication reduction) reduces fall rates.20,23 However, there is wide variability among studies in terms of administration of individual components, and there is not enough evidence to assess the contributions of individual components. Therefore, although single interventions are usually not as effective, they reveal data that are more specific to that individual component (e.g., exercise alone).
Community Setting
MULTIFACTORIAL INTERVENTIONS
According to the AGS/BGS guidelines, a multifactorial intervention should include an exercise program with muscle strengthening and gait and balance training; home environment modification; minimization of medications; and management of postural hypotension, foot problems, and footwear18 (Table 418,20–24 ). Older persons should be advised that walking in shoes with low heels and a high surface contact area may reduce the risk of falls.18 Multifactorial interventions are most effective,18 but there is conflicting evidence about which interventions to recommend.25 If available, consultation with a geriatrician may be considered. When older persons living in the community received an assessment and multifactorial interventions tailored to their needs, the number of falls was reduced by 25 percent.20 A randomized trial evaluating these strategies found that they can also significantly reduce hip and other fractures and head injuries, and decrease the use of medical services related to falls.26 Of greatest significance, one meta-analysis found that death was prevented by multidimensional fall prevention programs.27
SINGLE INTERVENTIONS
The AGS/BGS guidelines recommend that the physician monitor the patient's progress toward improving home safety.18 The goal is safe performance of daily activities, which can be monitored with the assistance of a home health agency, when appropriate. The limited effectiveness of some home modification programs may be related to the variability in participants' compliance with recommendations.
Reducing medication use can dramatically decrease falls. In one study, withdrawal of psychotropic medications resulted in a 66 percent reduction in the rate of falls.28 Another trial showed that educating family physicians about their prescribing practices can reduce falls by 39 percent.21 Ultimately, the effectiveness of medication withdrawal is determined by patient compliance; therefore, patients and caregivers must be educated about increased fall risk with certain medications (Table 3).11–15 Any medication that was initiated or increased shortly before a fall should be considered as a cause.
The AGS/BGS guidelines recommend that vitamin D supplementation of at least 800 IU per day be provided to older persons with proven vitamin D deficiency.18 A U.S. Preventive Services Task Force draft statement recommends vitamin D supplementation to prevent falls in older adults at increased fall risk.29 The Institute of Medicine (IOM) does not make specific recommendations for those at high risk of falls, but it recommends 800 IU of vitamin D per day for persons older than 70 years and for those at high risk of osteoporosis (600 IU per day for persons 51 to 70 years of age). The IOM also suggests that a 25-hydroxyvitamin D level of 20 ng per mL (49.92 nmol per L) is sufficient for the general population, but does not specify target levels for high-risk persons.30 In a Cochrane review, vitamin D supplementation (with or without calcium) decreased the number of persons who fell and the number of falls in men and women living in the community with lower baseline vitamin D levels (less than 24 ng per mL [59.90 nmol per L]).20 The number needed to treat to prevent one person from falling was 15.31
Cardioinhibitory carotid sinus hypersensitivity should be considered in the differential diagnosis when a patient experiences unexplained recurrent falls, especially falls associated with syncope or rapid head turning.18 Dual chamber pacing reduces falls and syncope, as well as soft tissue injury, by nearly 70 percent in patients with carotid sinus hypersensitivity.32
The AGS/BGS guidelines specify that all older adults who are at risk of falling should be offered an exercise program incorporating balance, gait, and strength training, such as physical therapy.18 Flexibility and endurance training can also be offered, but not as sole components. Individual (home) or group exercises tailored to the person's physical capabilities should be recommended by qualified health professionals or fitness instructors, who should also review progress and make program adjustments as needed.18,20 A U.S. Preventive Services Task Force draft statement also recommends exercise or physical therapy for older adults at increased risk of falls and found that the harms (e.g., paradoxical increase in falls with increased activity) are small.29
A Cochrane review found that exercise programs that contain multiple components significantly reduce the number of both falls and persons who fell. The number of persons who fell was reduced by 17 to 35 percent with group exercise, individually prescribed home-based exercise, or tai chi, but there is not enough evidence to suggest superiority of any one of these types of programs. In most studies, the exercise program was a minimum of 12 weeks in duration, with sessions ranging from 30 to 90 minutes each and occurring one to three times per week.20
In older women who need cataract surgery (first eye), surgery should be expedited because it reduces fall rate by 34 percent.22 According to the AGS/BGS guidelines, there is insufficient evidence to recommend for or against vision interventions, because new eyewear and multifocal lenses (especially when wearing them while climbing stairs or walking) may increase falls.18
The Toolkit for Implementing Community-Based Multifactorial Interventions: The Fall Prevention Prescription
Physicians may miss the opportunity to intervene because of the seemingly nonacute nature of a fall (especially a noninjurious fall). To make multifactorial interventions more user-friendly, a fall prevention prescription is proposed (Table 5; Figure 2). All components of the prescription are evidence-based and can be used to fulfill the need for documentation of quality indicators.24
Table 5. Toolkit for Implementing Community-Based Multifactorial Interventions: The Fall Prevention Prescription

| 1. Screen all persons older than 65 years annually for a history of falls, frequency of falls, and difficulty with gait and balance, as recommended by the American Geriatrics Society and British Geriatrics Society. Consider using the annual influenza vaccination as a reminder by screening for falls during the same time. | |
| 2. Train nursing staff to automatically document postural blood pressure and pulse, vision, functional history, and activities of daily living with any recent fall or history of falls. | |
| 3. Identify outpatient physical therapy programs and home health companies that specialize in physical therapy for falls and balance impairment. | |
| 4. Identify home health companies that provide home safety evaluation and follow-up for adherence to recommendations. | |
| 5. Identify companies that provide services for home safety modification (e.g., installation of grab bars in the bathroom).* | |
| 6. Identify group exercise programs or tai chi programs with strength, gait, and balance components.† | |
| 7. Input the above information (numbers 3 through 6) into the fall prevention prescription (Figure 2) and photocopy. | |
| 8. Identify and photocopy patient education materials, such as: | |
| • Patient information handout: “Tips for Preventing Falls,” p. 1277 | |
| • Patient information Web site: http://www.healthinaging.org/agingintheknow/chapters_ch_trial.asp?ch=21 | |
| • Home safety checklist: http://www.cdc.gov/HomeandRecreationalSafety/Falls/CheckListForSafety.html | |
| • Dietary sources of calcium: http://www.health.gov/dietaryguidelines/dga2005/document/html/appendixb.htm | |
| 9. Complete assessment and prescription for all older patients who report a single fall and have unsteadiness on gait examination; who report two or more falls; who report difficulties with gait or balance; or who seek medical attention because of a fall. | |
*—The National Association of Home Builders Certified Aging-in-Place Specialists can provide modifications or remodeling (http://www.nahb.org/directory.aspx?sectionID=0&directoryID=188), and the local Council on Aging may also be able to suggest resources.
†—Local Council on Aging, hospitals, and senior centers may offer these types of programs.
Figure 2. Fall Prevention Prescription

After completing a multifactorial risk assessment, use this fall prevention prescription in all older persons who report a single fall and have unsteadiness on gait examination; who report two or more falls; who report difficulties with gait or balance; or who seek medical attention because of a fall.
Hospital Setting
MULTIFACTORIAL INTERVENTIONS
Individualized assessment and multifactorial interventions that include similar components to the interventions used for community-dwelling older persons can be effective in the hospital setting (Table 4).18,20–24 Some additional components in effective interventions, which reduce the number of falls by 31 percent, include staff education and nonpharmacologic management of confusion by nursing staff. However, the effectiveness of these components was documented best in the subacute hospital setting where the length of stay was longer.23 The Centers for Medicare and Medicaid Services has designated falls occurring during hospitalization as preventable hospital-acquired conditions; therefore, any additional costs of care or increased length of stay because of subsequent fracture, dislocation, or brain injury are the responsibility of the hospital. Of note, falls were the largest category of hospital-acquired conditions, costing hospitals an estimated $7.6 million from October 2008 through June 2009 (net savings for the Centers for Medicare and Medicaid Services).33 This may increase pressure to physically or pharmacologically restrain patients; therefore, physicians must be diligent about avoiding restraining patients, because it increases the risk of injurious falls.34 More research is needed, especially in the acute hospital setting where the length of stay is short.
SINGLE INTERVENTIONS
Although data are limited, supervised exercise in the subacute hospital setting has been shown to significantly decrease fall risk.23
Nursing Home Setting
MULTIFACTORIAL INTERVENTIONS
A Cochrane review of four randomized controlled trials found that multidisciplinary team administration of multifactorial assessment and intervention (Table 418,20–24 ) is effective in older persons living in nursing homes because it reduces the rate of falls by 40 percent and the risk of hip fracture by 52 percent.23 The interventions contained many similar components to the interventions provided for community-dwelling persons, but may have also included staff education. Low beds and bed alarms also may have been used, although there is little evidence for their use. The evidence for effectiveness of exercise programs in long-term care is insufficient; exercise programs should be recommended with caution (because of the possible increased risk of falls and injury in frail older persons).18
SINGLE INTERVENTIONS
According to the IOM report, persons at high risk of osteoporosis (e.g., institutionalized older persons) should receive 800 IU of vitamin D per day.30 Vitamin D may reduce the rate of falls in long-term care residents with low baseline vitamin D levels (average levels less than 20 ng per mL).23 Hip protectors may reduce the incidence of hip fractures in persons living in nursing homes, but poor compliance has contributed to continuing uncertainty regarding their effectiveness.35
OSTEOPOROSIS TREATMENT
In addition to 1,200 mg of calcium (preferably from dietary sources) and 800 IU of vitamin D3 recommended per day, bisphosphonates are also recommended for up to five years to reduce fractures from falls.36 Supplementation with 800 IU of vitamin D3 and 1,200 mg of calcium per day reduces hip fractures by 25 percent in women living in nursing homes.37 Vitamin D is generally well-tolerated, but adverse effects must be monitored because there is a statistically significant increase in hypercalcemia, renal stones or insufficiency, and gastrointestinal effects.37 In women with osteoporosis, two out of 100 women taking placebo will have a hip or wrist fracture compared with one out of 100 women taking alendronate (Fosamax).38 Similarly, risedronate (Actonel)39 and yearly intravenous zoledronic acid (Reclast)36 also reduce hip fractures.40 The benefits of fracture prevention far outweigh the rare risk of atypical femur fracture that has been associated with bisphosphonates.41 Although ibandronate (Boniva), raloxifene (Evista), and calcitonin reduce vertebral fractures, their effect on fall-related fractures, especially hip fractures, is not proven.36
OTHER INTERVENTIONS
Personal emergency response systems have been found to decrease hospitalization and may be considered for community-dwelling older persons.42 Although some nursing homes have reported an increase in falls since the federal regulations to reduce restraints were instituted in 1990, most facilities have had a decrease in fall-related injuries.43
Quality Indicators
The Assessing Care of Vulnerable Elders quality indicators are evidence-based quality of care indicators that are relevant to persons older than 65 years who are at increased risk of death or functional decline.24 Although they are not practice guidelines and were developed to measure care at the level of a health system, they can serve as a minimal standard by which physicians may evaluate their own practice. All assessment and management should occur within three months of the report of a fall24 (Table 418,20–24 ).
Data Sources: A PubMed search was completed in Clinical Queries using the key terms falls in the elderly. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. Also searched were the Agency for Healthcare Research and Quality evidence reports, Bandolier, the Cochrane database, the Institute for Clinical Systems Improvement, the National Guideline Clearinghouse database, Physicians' Information and Education Resource, U.S. Preventive Services Task Force (USPSTF), and UpToDate. Search date: June 5, 2010. An updated search in PubMed, the Cochrane database, and USPSTF was completed on February 11, 2011.


