An otherwise healthy 16-year-old boy presented with an asymptomatic, black to brown plaque on his right proximal forearm. The lesion was present at birth, but was flatter and lighter in color. Physical examination revealed a discrete, oval-shaped plaque that measured 7 × 3 cm. The lesion had a cobblestone pattern with prominent hair growth (see accompanying figure).
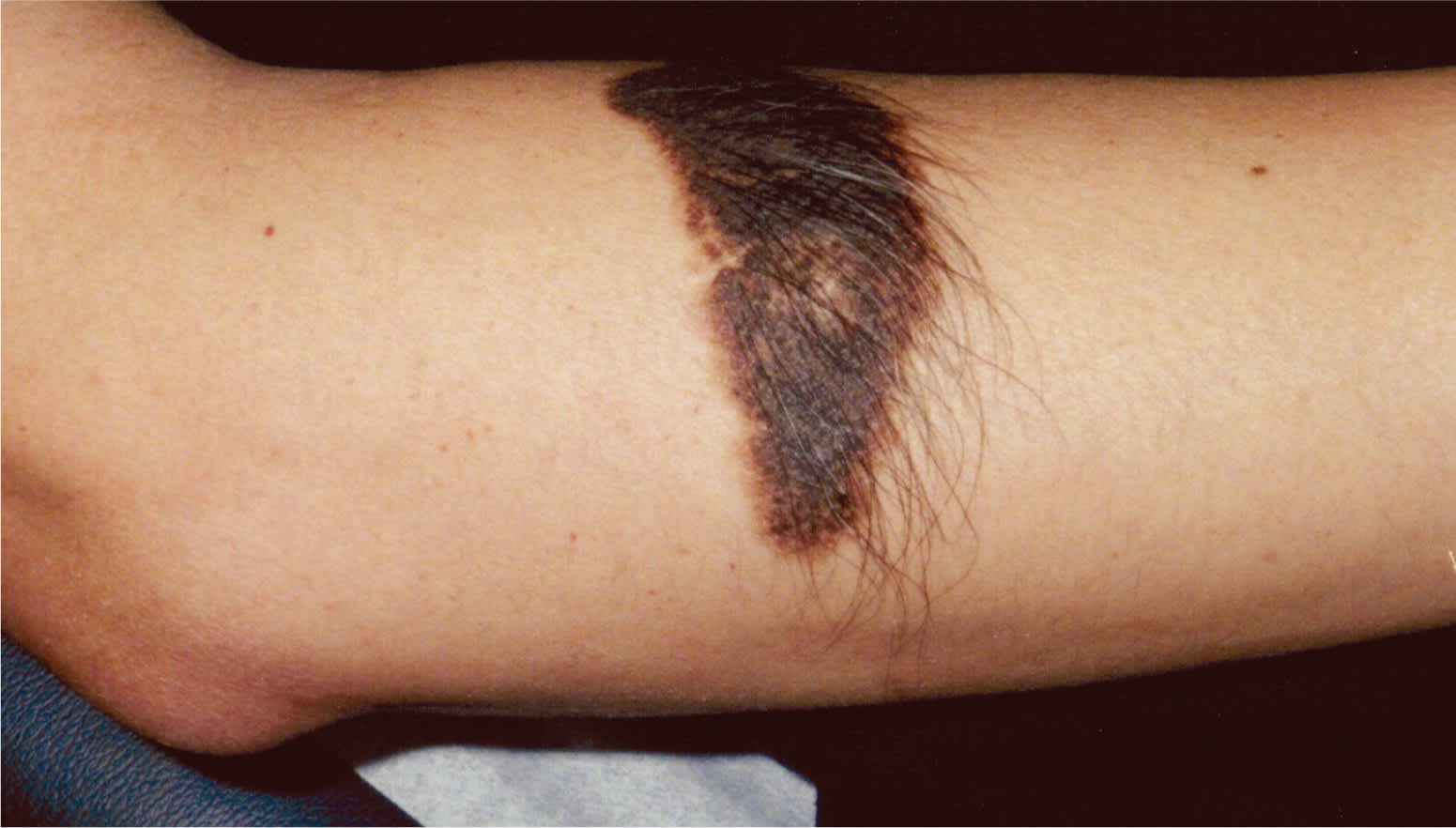
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Acquired melanocytic nevus.
B. Becker nevus.
C. Congenital melanocytic nevus.
D. Melanoma.
E. Plexiform neurofibroma.
Discussion
The answer is C: congenital melanocytic nevus. Congenital melanocytic nevi are generally present at birth or appear within the first few months of life.1 The incidence ranges from 1 to 2 percent for any size of congenital melanocytic nevi to approximately one in 20,000 for giant nevi.2 Most congenital melanocytic nevi are intradermal or compound in nature.3 They are classified according to their expected diameter in adulthood as small (less than 1.5 cm), medium or intermediate (1.5 to 19.9 cm), and large or giant (20 cm or greater).2,4,5 Small and medium nevi are usually round or oval and symmetric. At birth, these lesions are flat or mildy palpable and tan in color, but over time they become raised and darken. They may have a verrucous or cobblestone surface.5 Hypertrichosis may become prominent.
Giant congenital melanocytic nevi can have irregular color patterns and are often accompanied by multiple smaller “satellite” nevi. Although nevi are usually benign, some, particularly giant nevi, may be associated with the development of malignant melanoma.1 Congenital melanocytic nevi, especially those occurring in the posterior trunk, may rarely involve the central nervous system.
The usual treatment for small and medium congenital melanocytic nevi is observation.4 The decision to remove a lesion is based on the malignant potential and its cosmetic outcome.4 Prophylactic excision is performed for giant congenital melanocytic nevi to lower the risk of melanoma. Other treatments include superficial excision, laser treatment, curettage, chemical peel, and dermabrasions with regular follow-up. A conservative approach with serial photography of the nevus and close follow-up has also been recommended.2 All patients with congenital melanocytic nevi should be instructed on sun protection.1,4
Acquired melanocytic nevi are small (less than 8 mm in diameter), well circumscribed, and round or ovoid with a homogenous surface and even pigmentation. Compared with the congenital type, acquired melanocytic nevi are smaller, are more uniform in architecture and morphology, and occur in greater numbers.
Becker nevi are more common in males. They typically appear at 10 to 20 years of age as a brownish, circumscribed macule or patch that gradually enlarges in an irregular fashion, similar to a geographic configuration.6 Hypertrichosis may develop a few years after the pigmentation. The lesion is asymptomatic and unilateral with a predilection for the upper torso, often the shoulder.
Melanoma is a malignant tumor that can present as an enlarging, asymmetric, variegated lesion with an irregular border. It is rare in childhood and typically does not have hypertrichosis. Melanoma can be diagnosed with a biopsy.
Plexiform neurofibromas are a subcutaneous manifestation of type 1 neurofibromatosis.7 They are often present at birth and result from diffuse thickening of nerve trunks.7 Although most are associated with tender, firm nodules, early lesions may appear as hyperpigmentation and hypertrichosis.
Summary Table
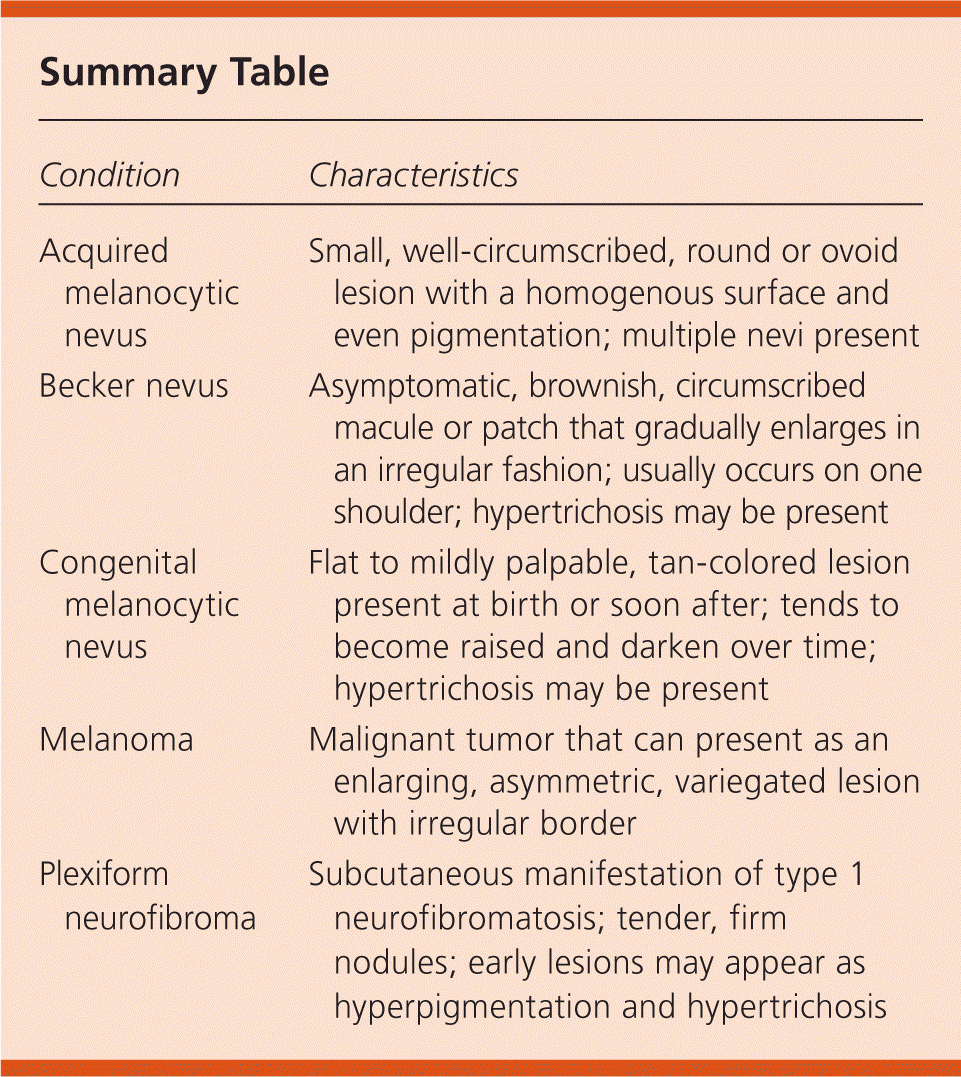
| Condition | Characteristics |
|---|---|
| Acquired melanocytic nevus | Small, well-circumscribed, round or ovoid lesion with a homogenous surface and even pigmentation; multiple nevi present |
| Becker nevus | Asymptomatic, brownish, circumscribed macule or patch that gradually enlarges in an irregular fashion; usually occurs on one shoulder; hypertrichosis may be present |
| Congenital melanocytic nevus | Flat to mildly palpable, tan-colored lesion present at birth or soon after; tends to become raised and darken over time; hypertrichosis may be present |
| Melanoma | Malignant tumor that can present as an enlarging, asymmetric, variegated lesion with irregular border |
| Plexiform neurofibroma | Subcutaneous manifestation of type 1 neurofibromatosis; tender, firm nodules; early lesions may appear as hyperpigmentation and hypertrichosis |

