A 55-year-old man with human immunodeficiency virus (HIV) presented with a penile mass that began six years earlier. He reported intermittent itching on the penis but no pain. The mass had been enlarging slowly, and the surface had eroded. The lesion was treated with oral antivirals and antibiotics, with little response. A biopsy was inconclusive.
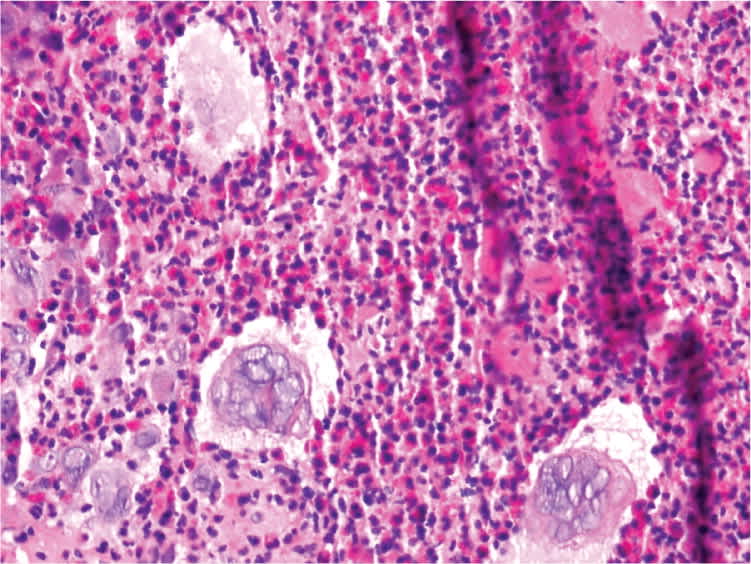
Examination revealed a large, indurated mass, with a superficial erythematous erosion and yellow exudate covering approximately 80 percent of the penile surface (Figure 1). A repeat biopsy demonstrated ulceration with a diffuse, dermal, mixed inflammatory infiltrate (Figure 2). Multinucleated giant epidermal cells with steelgray nuclei were also identified.
Figure 1.
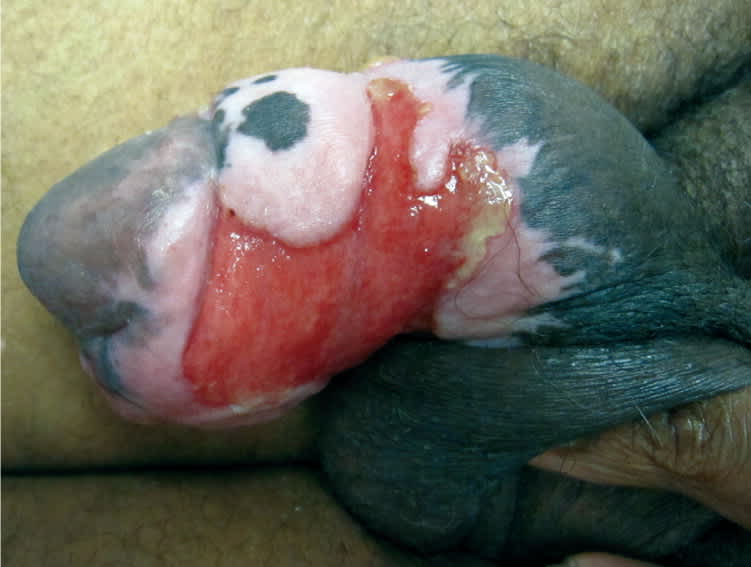
Figure 2.
Question
Based on the patient's history, physical examination, and laboratory results, which one of the following is the most likely diagnosis?
A. Condylomata acuminata (genital warts).
B. Herpes simplex virus.
C. Squamous cell carcinoma.
D. Syphilis.
Discussion
The answer is B: Herpes simplex virus (HSV). Genital HSV infection is one of the most common sexually transmitted infections worldwide. It typically manifests as clusters of painful vesicles and superficial erosions, without induration. Indurated lesions may occur in patients with underlying immunosuppression. Coinfection with HIV can cause longer, more frequent, and more severe recurrences. In these patients, hypertrophic lesions that mimic neoplasia can occur. Although histologic evaluation is helpful, findings are occasionally non-specific,1 requiring a repeat biopsy.
Hypertrophic HSV lesions occur in patients who have HIV with varying levels of immunity. In one patient, hypertrophic HSV persisted for three years despite the achievement of immune recovery through highly active antiretroviral therapy.2
Acyclovir (Zovirax), an inhibitor of viral DNA polymerase, is the first-line treatment for HSV infection. Hypertrophic lesions may require prolonged treatment. Viral resistance necessitates antiviral medications that do not require phosphorylation by viral thymidine kinase, such as foscarnet and cidofovir (Vistide).
Condylomata acuminata (genital warts related to human papillomavirus infection) typically appear as sessile or pedunculated, exophytic, verrucous papules without erosions. Genital warts are usually not painful.
Genital squamous cell carcinoma can present similarly to hypertrophic HSV lesions and requires histologic evaluation for definitive diagnosis. It typically appears as indurated nodules or plaques with erosions, or ulcers with raised edges.
Syphilis initially appears as a small genital papule, then develops into a larger, firm, painless ulcer (chancre) with possible enlargement of regional lymph nodes. The lesion heals spontaneously within weeks without treatment.
Summary Table
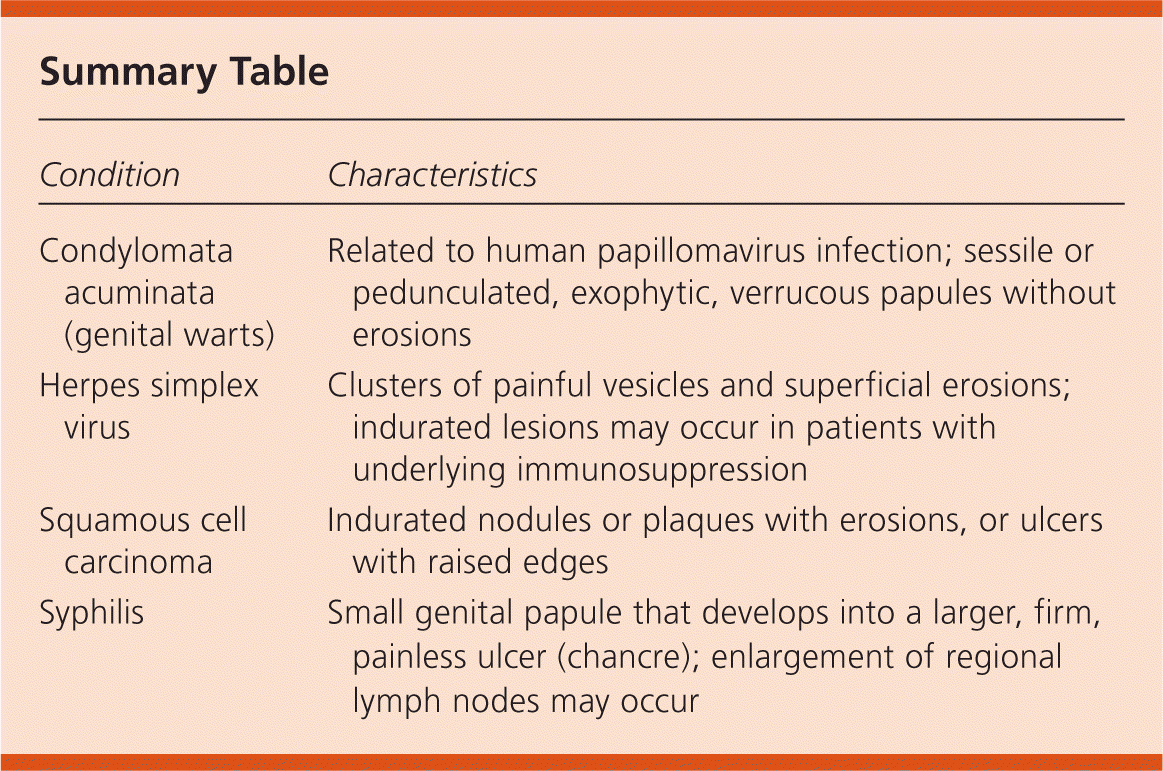
| Condition | Characteristics |
|---|---|
| Condylomata acuminata (genital warts) | Related to human papillomavirus infection; sessile or pedunculated, exophytic, verrucous papules without erosions |
| Herpes simplex virus | Clusters of painful vesicles and superficial erosions; indurated lesions may occur in patients with underlying immunosuppression |
| Squamous cell carcinoma | Indurated nodules or plaques with erosions, or ulcers with raised edges |
| Syphilis | Small genital papule that develops into a larger, firm, painless ulcer (chancre); enlargement of regional lymph nodes may occur |

