A 20-year-old man presented to his university's student health clinic with intermittent pain in his right knee that began two months earlier. He had no history of knee injury or surgery and was otherwise in good health.
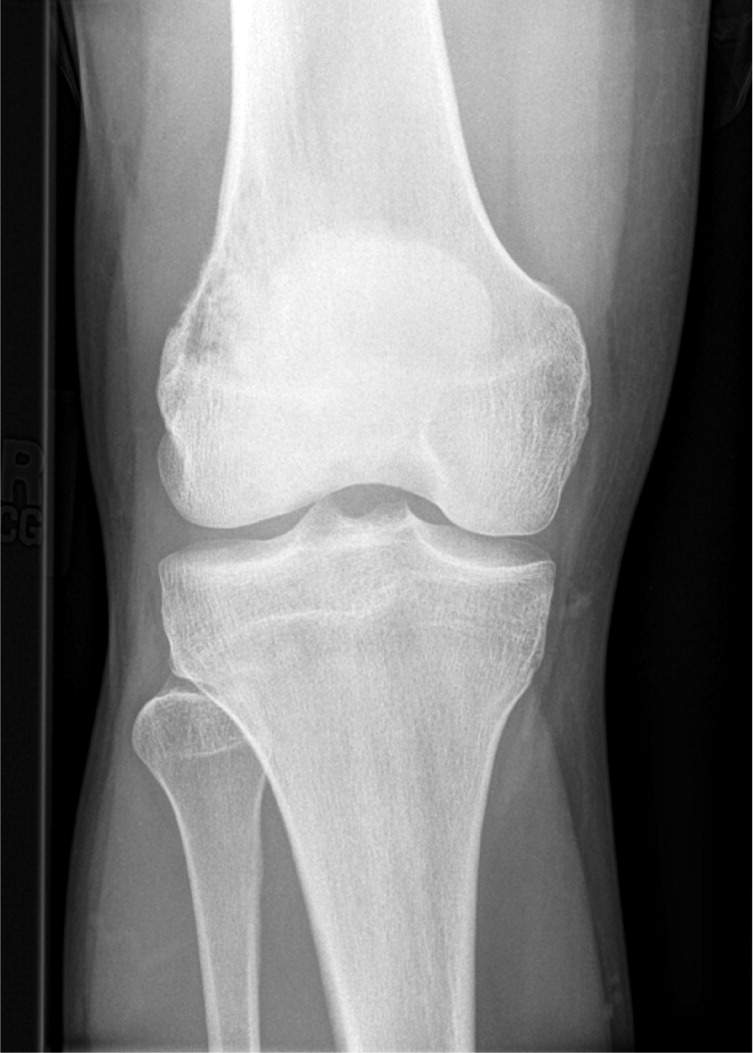
Physical examination showed a visually normal knee with no effusion. He had normal range of motion but slight tenderness to palpation over the lateral femoral condyle. Testing of the medial and lateral collateral ligaments showed no laxity, and the iliotibial band was not tight. Radiography of the knee was performed (see accompanying figure).
Question
Based on the patient's history, physical examination and radiographic findings, which one of the following is the most likely diagnosis?
A. Giant cell tumor of bone.
B. Myositis ossificans.
C. Nonossifying fibroma.
D. Osteoid osteoma.
E. Osteosarcoma.
Discussion
The answer is E: osteosarcoma. Osteosarcomas are common primary malignant bone tumors, with more than 2,400 new cases annually in the United States. Although osteosarcomas can occur at any age, 75 percent of patients with the condition are in adolescence to early 20s. It is more common in males than in females, with a male-to-female ratio of 1.6:1.1 The typical presentation includes mild or intermittent pain around the involved area. As the tumor increases in size, pain intensifies and swelling may be appreciated. Although osteosarcomas can occur in any metaphyseal area of long bones, the distal femur or proximal tibia is the most common location, followed by the proximal humerus.2
The patient's radiograph demonstrates mixed lytic and blastic features with cortical destruction along the lateral femoral condyle, which are typical findings in osteosarcoma.2 Radiographs often show medullary and cortical destruction with a sunburst or velvety appearance of neoplastic bone along the periosteum. Codman triangle (a triangular shadow between the cortex and raised periosteum) may also be present.3
Osteosarcoma is an aggressive neoplasm, with metastasis in 20 percent of patients at the time of diagnosis. Patients without metastases have a five-year survival rate of 80 percent.4
Giant cell tumors of bone are uncommon, nonmalignant, locally aggressive tumors that occur after skeletal maturity. They are more common in women.1 Giant cell tumors develop in the epiphysis of long bones, most commonly in the distal femur or proximal tibia. Radiographs typically show a large eccentric, osteolytic lesion extending into the soft tissue.2
Myositis ossificans is a benign reactive ossification process within muscle tissue, usually following trauma. Most lesions occur along the femur in adolescent athletes. The key radiologic feature is the “zonal phenomenon,” with radiolucent immature bone in the center of the lesion and mature radiodense bone at the periphery.3
Nonossifying fibromas are the most common bony lesions in children and adolescents.2 Most are asymptomatic, incidental findings on radiography. Radiographs show elliptical radiolucent lesions with sclerotic borders in the cortex of long bones near the growth plates. These lesions are not neoplasms, and most resolve spontaneously with skeletal maturity. Large and progressive lesions that involve more than 50 percent of the medullary cavity are prone to pathologic fracture.2
Osteoid osteomas are benign neoplasms that primarily occur in adolescence or the early 20s, and are more common in males.3 Osteomas usually develop in the proximal femur and tibia. Radiographs show a well-circumscribed, 1- to 2-cm lesion with a central osteoblastic area or “nidus” surrounded by a sclerotic border.2 Clinically, pain is more severe at night and relieved with aspirin or other nonsteroidal anti-inflammatory drugs.3
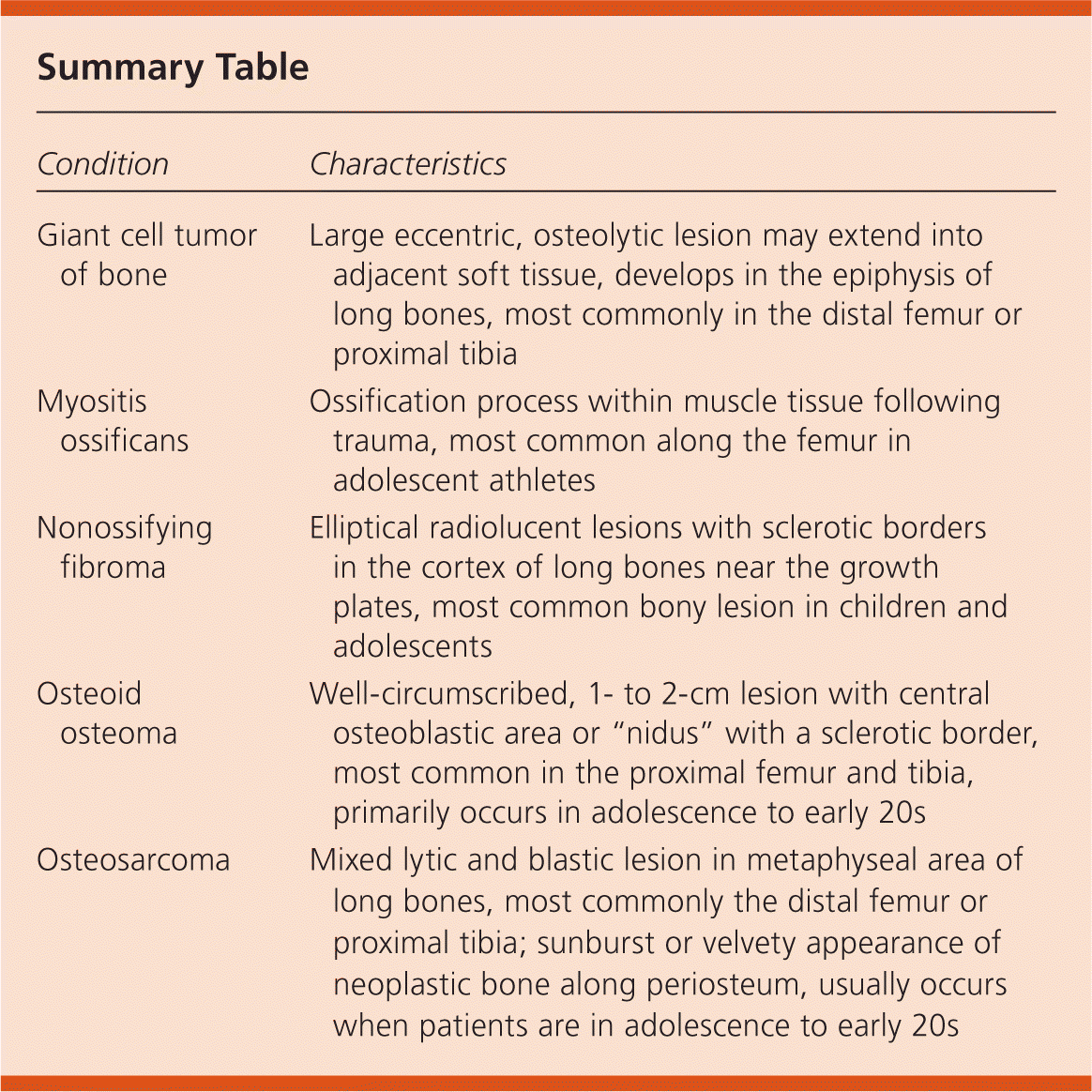
Summary Table
| Condition | Characteristics |
|---|---|
| Giant cell tumor of bone | Large eccentric, osteolytic lesion may extend into adjacent soft tissue, develops in the epiphysis of long bones, most commonly in the distal femur or proximal tibia |
| Myositis ossificans | Ossification process within muscle tissue following trauma, most common along the femur in adolescent athletes |
| Nonossifying fibroma | Elliptical radiolucent lesions with sclerotic borders in the cortex of long bones near the growth plates, most common bony lesion in children and adolescents |
| Osteoid osteoma | Well-circumscribed, 1- to 2-cm lesion with central osteoblastic area or “nidus” with a sclerotic border, most common in the proximal femur and tibia, primarily occurs in adolescence to early 20s |
| Osteosarcoma | Mixed lytic and blastic lesion in metaphyseal area of long bones, most commonly the distal femur or proximal tibia; sunburst or velvety appearance of neoplastic bone along periosteum, usually occurs when patients are in adolescence to early 20s |

