A 30-year-old woman presented with a nonpruritic vesicular eruption on the palms that began one week earlier. One day before the rash developed, the patient had a burning, tingling sensation in the same area. She did not have a fever or other systemic symptoms. The review of systems was unremarkable, and she was not pregnant. The patient had zoster on her trunk 10 years earlier, but no known recent contact with anyone who had a similar rash. Physical examination revealed multiple vesicles on the palms in various stages of healing with faint surrounding erythema (see accompanying figure). There was no fluctuance, induration, warmth, scaling, or exudate.
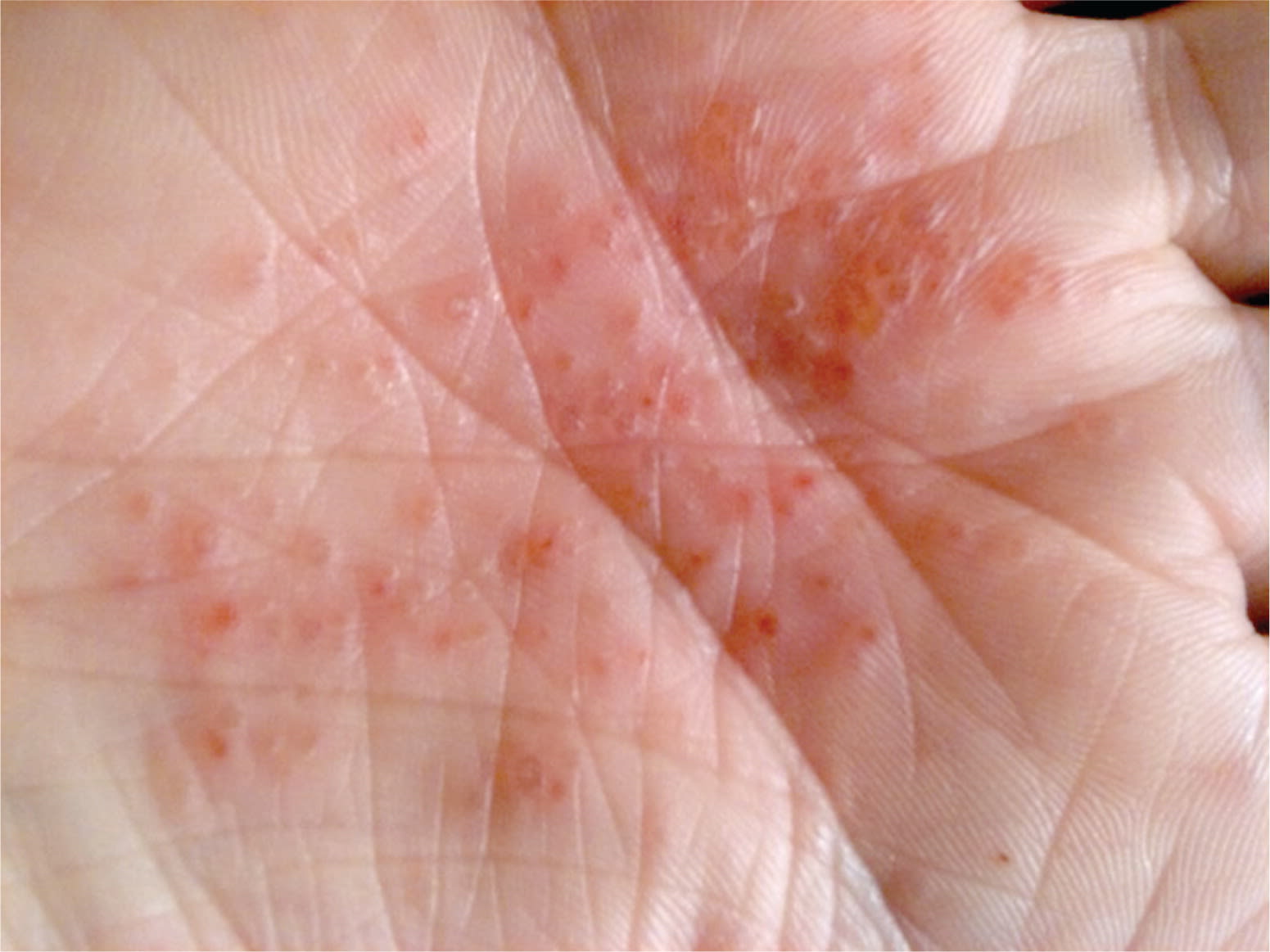
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Dyshidrotic eczema.
B. Herpetic whitlow.
C. Id reaction.
D. Palmoplantar pustulosis.
E. Secondary syphilis.
Discussion
The answer is A: dyshidrotic eczema. Dyshidrotic eczema, also known as dyshidrosis and pompholyx, is a vesicular eruption that primarily affects the palmar aspect of the hands and lateral aspects of the fingers. It also may occur on the plantar aspect of the feet. The most common presentation is a symmetrical eruption of pruritic vesicles that resolves in three to four weeks with residual scaling.1,2 The etiology is unknown, but associated factors include stress, allergic reaction (particularly exposure to nickel and other metals), fungal infections, and genetic predisposition.3
Diagnosis of dyshidrotic eczema is clinical and based on a detailed history and the appearance of the rash. In less obvious cases, rapid plasma reagin testing and a potassium hydroxide preparation should be considered as part of the diagnostic workup. A culture of the vesicles may rule out a secondary infection. A punch biopsy of the affected area will reveal spongiosis with an epidermal lymphocytic infiltrate.4
Initial therapy focuses on causative or exacerbating factors. Treatment may include a short course of topical corticosteroids.1 Emollients and antihistamines may be used to soothe itching. Topical immunomodulators such as tacrolimus (Protopic) or pimecrolimus (Elidel) are beneficial in refractory cases.3
Herpetic whitlow typically forms as grouped vesicles on the lateral edge of the thumb. The condition is most common in persons who come in contact with saliva, such as dental hygienists and children who suck their thumbs. Herpetic whitlow, like dyshidrotic eczema, may be preceded by pain or tingling. However, herpetic whitlow typically presents unilaterally.5
Id reactions are symmetrical, vesicular eruptions that may be pruritic and can closely resemble dyshidrotic eczema. However, id reactions occur in the presence of an inflammatory process, such as acute Tinea pedis infection or stasis dermatitis, at a distant site. The eruptions most commonly occur on the lateral aspect of the fingers, and they resolve with treatment of the inciting inflammatory process.1
Palmoplantar pustulosis is a type of pustular psoriasis that is localized to the palms and soles. It appears as an erythematous eruption that varies in morphology from vesicular to pustular and has a chronic, recurrent course. It occurs predominantly in patients with a history of smoking.6 Palmoplantar pustulosis has a similar appearance to dyshidrotic eczema that is secondarily infected, but the pruritus is typically less severe. The lesions contain a sterile infiltrate, consisting of neutrophils and eosinophils.6
Secondary syphilis, caused by Treponema pallidum, occurs one to six months after the initial (primary) infection. The reddish-brown rash is bilateral and varies in morphology from macular to papulonodular. A vesicular eruption does not occur. Distribution ranges from the palms and soles to the entire body and mucous membranes. The lesions are painless, nonpruritic, and noninflammatory. The patient may have systemic signs and symptoms, such as fever, sore throat, painless lymphadenopathy, weight loss, myalgias, and fatigue.1
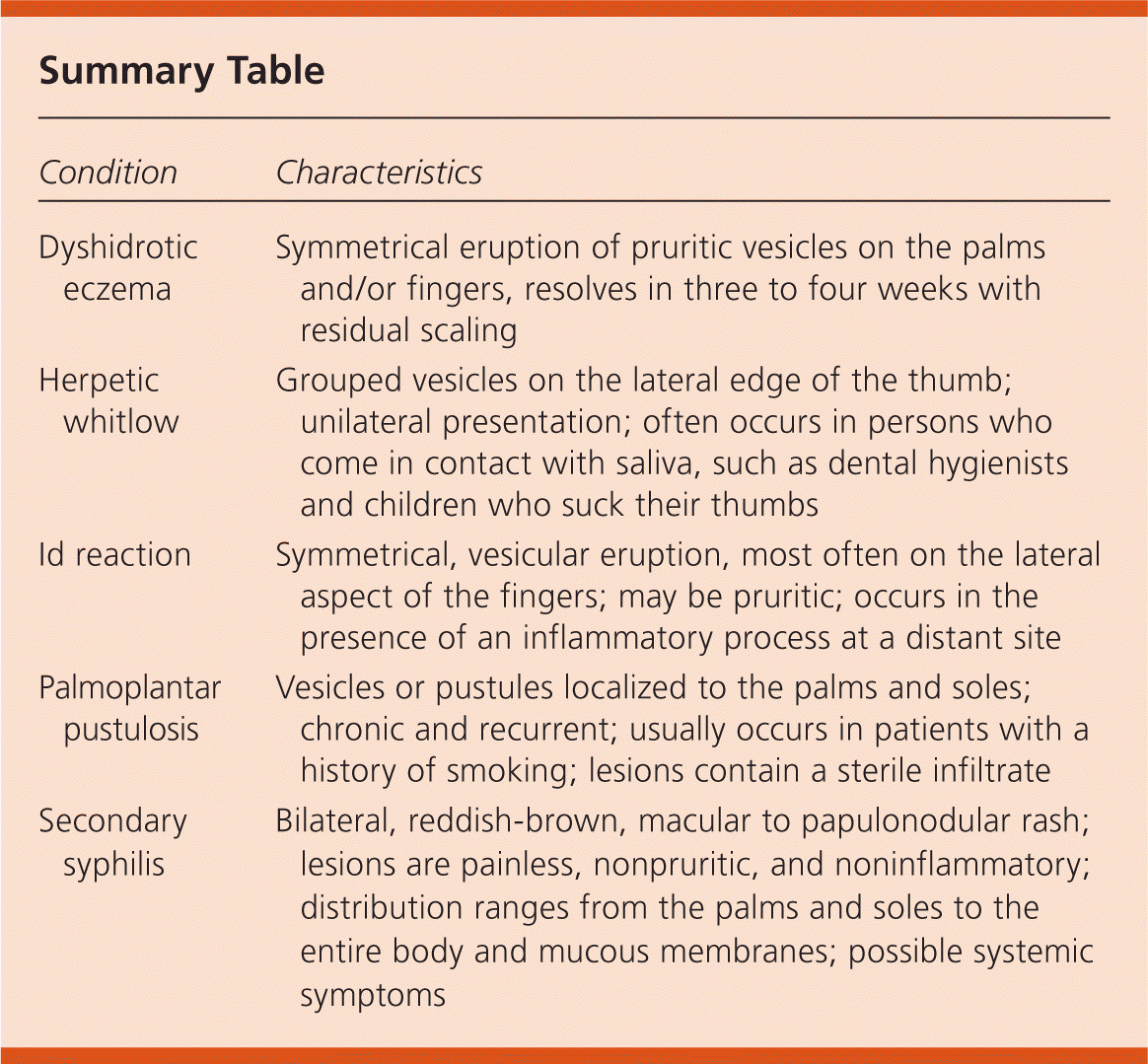
Summary Table
| Condition | Characteristics |
|---|---|
| Dyshidrotic eczema | Symmetrical eruption of pruritic vesicles on the palms and/or fingers, resolves in three to four weeks with residual scaling |
| Herpetic whitlow | Grouped vesicles on the lateral edge of the thumb; unilateral presentation; often occurs in persons who come in contact with saliva, such as dental hygienists and children who suck their thumbs |
| Id reaction | Symmetrical, vesicular eruption, most often on the lateral aspect of the fingers; may be pruritic; occurs in the presence of an inflammatory process at a distant site |
| Palmoplantar pustulosis | Vesicles or pustules localized to the palms and soles; chronic and recurrent; usually occurs in patients with a history of smoking; lesions contain a sterile infiltrate |
| Secondary syphilis | Bilateral, reddish-brown, macular to papulonodular rash; lesions are painless, nonpruritic, and noninflammatory; distribution ranges from the palms and soles to the entire body and mucous membranes; possible systemic symptoms |

