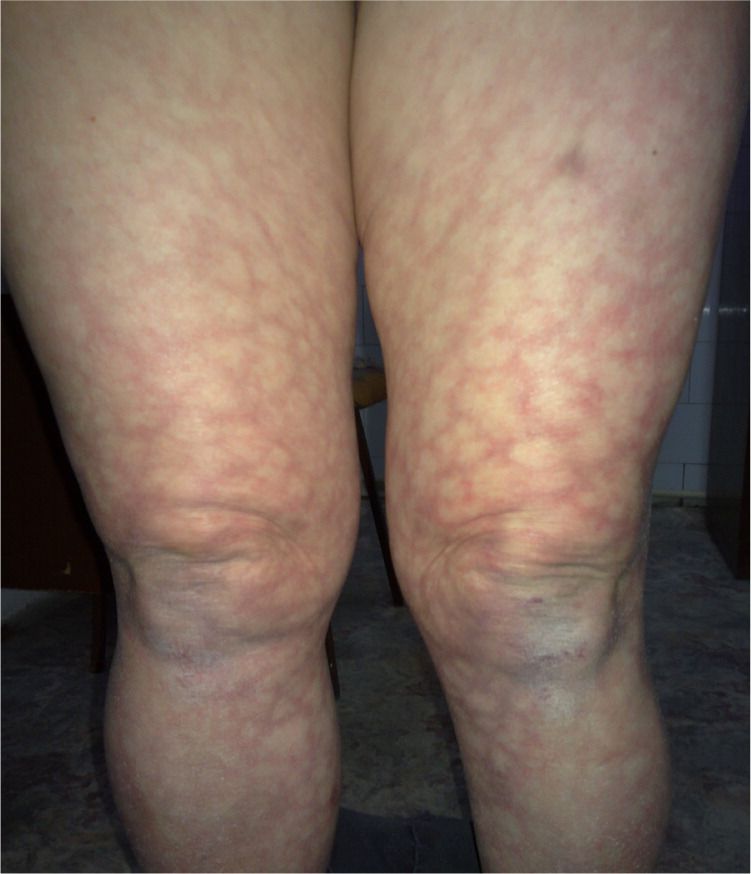
A 61-year-old woman with a 20-year history of rheumatoid arthritis presented to a dermatologist during the winter. Physical examination showed a large, reddish-violet, reticular discoloration of the legs (see accompanying figure). The lesions had been present for less than two months and were asymptomatic.
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Acrocyanosis.
B. Erythema ab igne.
C. Erythrocyanosis.
D. Livedo reticularis.
Discussion
The answer is D: livedo reticularis. Livedo reticularis is a reticular, reddish-violet discoloration of the skin that typically affects the limbs, although it can be generalized.1 The rash becomes worse with exposure to cold temperatures. The diagnosis requires determining a possible systemic association. Associations include antiphospholipid antibody syndrome, Sneddon syndrome, autoimmune disease/vasculitis, hematologic conditions/thrombosis, vessel wall disorders/emboli, neurologic conditions, infectious diseases, neoplasia, and medication use.2 A complete history, physical examination, and laboratory testing should be performed to look for signs of systemic associations, and appropriate treatment of the underlying cause should be initiated. In the case of physiologic or idiopathic livedo reticularis, avoidance of cold temperatures should be recommended.
Acrocyanosis is a persistent, cyanotic or erythrocyanotic, mottled discoloration of the hands, feet, and face. It may be idiopathic or secondary to a systemic disorder.3 It often occurs in infants shortly after birth, and is more common in winter.
Erythema ab igne, or toasted skin syndrome, usually is caused by exposure to topical or convection heat that is used to relieve localized pain or cold (e.g., hot water bottle, heating pad). The rash appears as localized, net-like, erythematous, and hyperpigmented skin lesions. The rash is caused by prolonged thermal radiation exposure that damages the skin.4 The size and shape of the lesions are typically consistent with the heat source.
Erythrocyanosis is a persistent, dusky erythema occurring at sites with a thick layer of underlying subcutaneous fat, such as the thighs and lower legs. It is exacerbated by cold and therefore is usually more prominent during the winter. Erythrocyanosis is most common on the lower legs and in women. The disorder may persist indefinitely, but spontaneous improvement can occur in adolescent patients.3
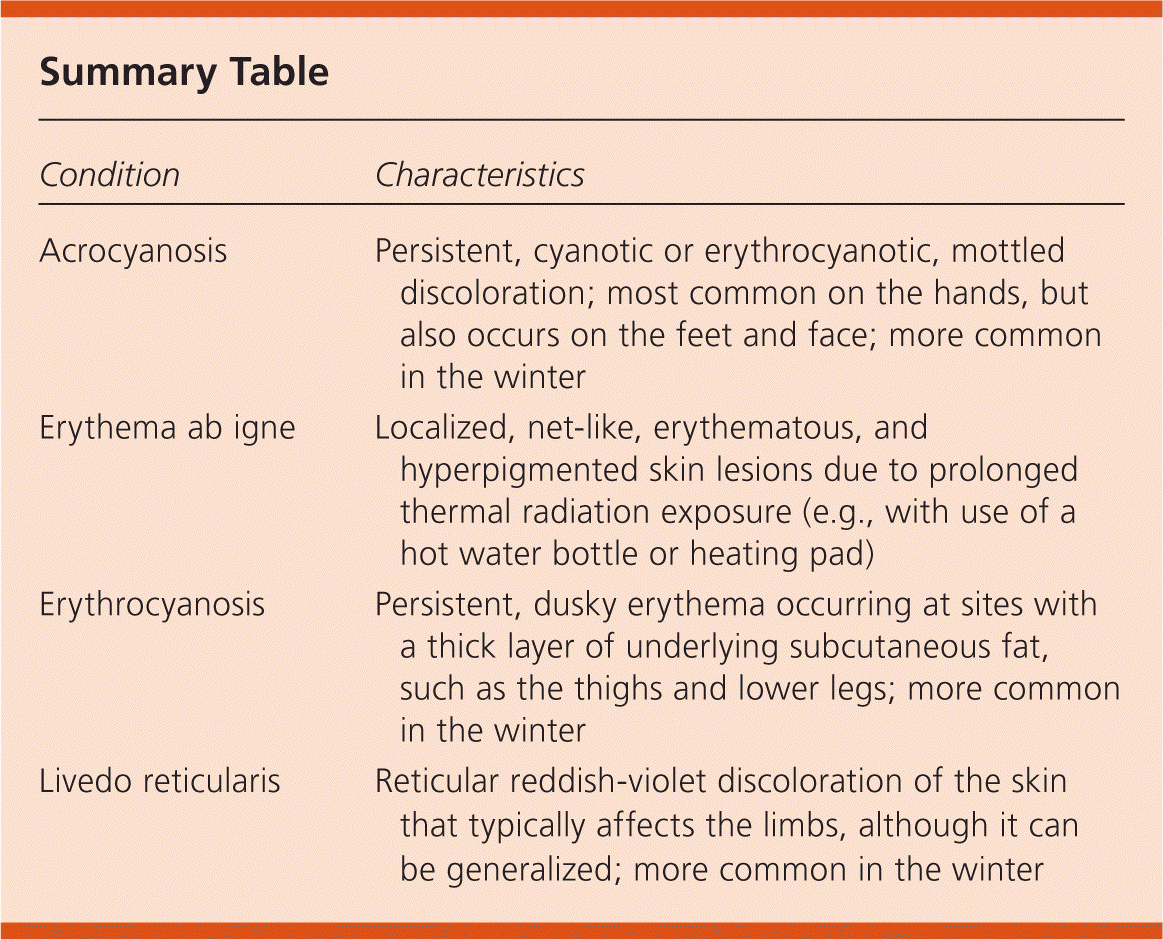
Summary Table
| Condition | Characteristics |
|---|---|
| Acrocyanosis | Persistent, cyanotic or erythrocyanotic, mottled discoloration; most common on the hands, but also occurs on the feet and face; more common in the winter |
| Erythema ab igne | Localized, net-like, erythematous, and hyperpigmented skin lesions due to prolonged thermal radiation exposure (e.g., with use of a hot water bottle or heating pad) |
| Erythrocyanosis | Persistent, dusky erythema occurring at sites with a thick layer of underlying subcutaneous fat, such as the thighs and lower legs; more common in the winter |
| Livedo reticularis | Reticular reddish-violet discoloration of the skin that typically affects the limbs, although it can be generalized; more common in the winter |

