
Am Fam Physician. 2012;85(12):1170-1176
A more recent article on Management of Acute Ankle Sprains is available.
Patient information: See related handout on how to care for an ankle sprain, written by the author of this article.
Author disclosure: No relevant financial affiliations to disclose.
Ankle sprains are a common problem seen by primary care physicians, especially among teenagers and young adults. Most ankle sprains are inversion injuries to the lateral ankle ligaments, although high sprains representing damage to the tibiofibular syndesmosis are becoming increasingly recognized. Physicians should apply the Ottawa ankle rules to determine whether radiography is needed. According to the Ottawa criteria, radiography is indicated if there is pain in the malleolar or midfoot zone, and either bone tenderness over an area of potential fracture (i.e., lateral malleolus, medial malleolus, base of fifth metatarsal, or navicular bone) or an inability to bear weight for four steps immediately after the injury and in the emergency department or physician's office. Patients with ankle sprain should use cryotherapy for the first three to seven days to reduce pain and improve recovery time. Patients should wear a lace-up ankle support or an air stirrup brace combined with an elastic compression wrap to reduce swelling and pain, speed recovery, and protect the injured ligaments as they become more mobile. Early mobilization speeds healing and reduces pain more effectively than prolonged rest. Pain control options for patients with ankle sprain include nonsteroidal anti-inflammatory drugs, acetaminophen, and mild opioids. Because a previous ankle sprain is the greatest risk factor for an acute ankle sprain, recovering patients should be counseled on prevention strategies. Ankle braces and supports, ankle taping, a focused neuromuscular training program, and regular sport-specific warm-up exercises can protect against ankle injuries, and should be considered for patients returning to sports or other high-risk activities.
Acute ankle sprain is one of the most common reasons for primary care office and emergency department visits in the United States, with an overall incidence of 2.15 per 1,000 person-years.1 Teenagers and young adults have the highest rates of ankle sprain, with a peak incidence of 7.2 per 1,000 person-years for those 15 to 19 years of age.1 Nearly one-half of all ankle sprains occur during athletic activity, with basketball being the most commonly involved sport.2 The greatest risk factor for ankle sprain is a previous ankle sprain, which underscores the importance of proper treatment and effective prevention strategies.
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| The Ottawa ankle rules should be used to rule out fractures and prevent unnecessary radiography in patients with suspected ankle sprain. | A | 6, 7 |
| Cryotherapy should be applied for the first three to seven days to reduce pain and improve recovery time in patients with ankle sprain. | B | 11–13 |
| An air stirrup brace combined with an elastic compression wrap, or a lace-up support alone, reduces pain and recovery time after an ankle sprain and allows early mobilization. | B | 15–17 |
| Early mobilization and focused range-of-motion exercises reduce pain and recovery time after an ankle sprain, and are preferred to prolonged rest. | B | 18, 19 |
| Patients at risk of reinjury after an ankle sprain should participate in a neuromuscular training program. | B | 35, 36 |
| Air stirrup braces, lace-up supports, and athletic taping can reduce the risk of ankle sprains during sports. | B | 39, 40 |
Diagnosis
HISTORY AND PHYSICAL EXAMINATION
Patients presenting with an ankle sprain should be asked to describe the mechanism of the injury. Most ankle sprains are injuries to the lateral ligaments of the ankle (i.e., anterior talofibular and calcaneofibular ligaments; Figure 13), and are caused by inversion of the ankle with some degree of plantar flexion. History of another mechanism of injury (e.g., eversion, forced severe plantar flexion, dorsiflexion) should raise suspicion of an unusual ligamentous injury or fracture.
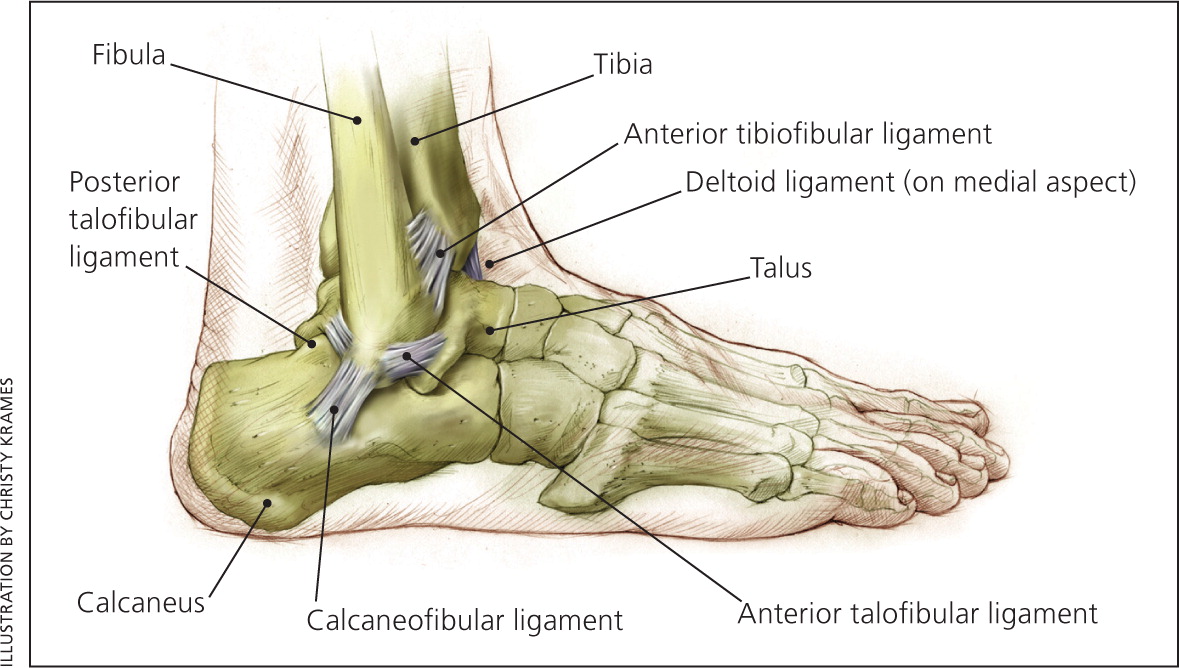
In a typical lateral ankle sprain, tenderness, swelling, and ecchymosis are found over the anterior talofibular and calcaneofibular ligaments. Acute injuries do not have swelling or bruising over the forefoot or toes. However, if the injury is at least one day old, if proper treatment has not been applied, and if the patient has been ambulating, swelling and bruising may be found down the entire foot and toes as a result of gravity.
GRADING
Lateral ankle sprains classically are graded I, II, or III, representing no, partial, or complete rupture of the lateral ligaments, respectively. Tests of ligament integrity are difficult to perform at the time of acute injury because of pain and swelling; therefore, clinical grading usually is somewhat subjective and based on the amount of pain, swelling, and bruising present. At least one study has shown that the ability to accurately identify grade III sprains clinically is limited.4 Clinical grading of ankle sprains does not affect initial treatment, so it is of limited use.
OTTAWA ANKLE RULES
Ankle sprains should be evaluated using the Ottawa ankle rules (Figure 23 ), which are well-established clinical guidelines used to determine the need for radiography.5–7 According to the Ottawa ankle rules, ankle radiography is needed if there is pain in the malleolar zone, plus either bone tenderness over areas of potential fracture (namely the posterior edge or tip of the lateral or medial malleolus) or an inability to bear weight for four steps immediately after the injury and in the emergency department or physician's office. Foot radiography is needed if there is pain in the midfoot zone, plus either bone tenderness over areas of potential fracture (namely the base of the fifth metatarsal or the navicular bone of the midfoot) or an inability to bear weight for four steps immediately after the injury and in the emergency department or physician's office.
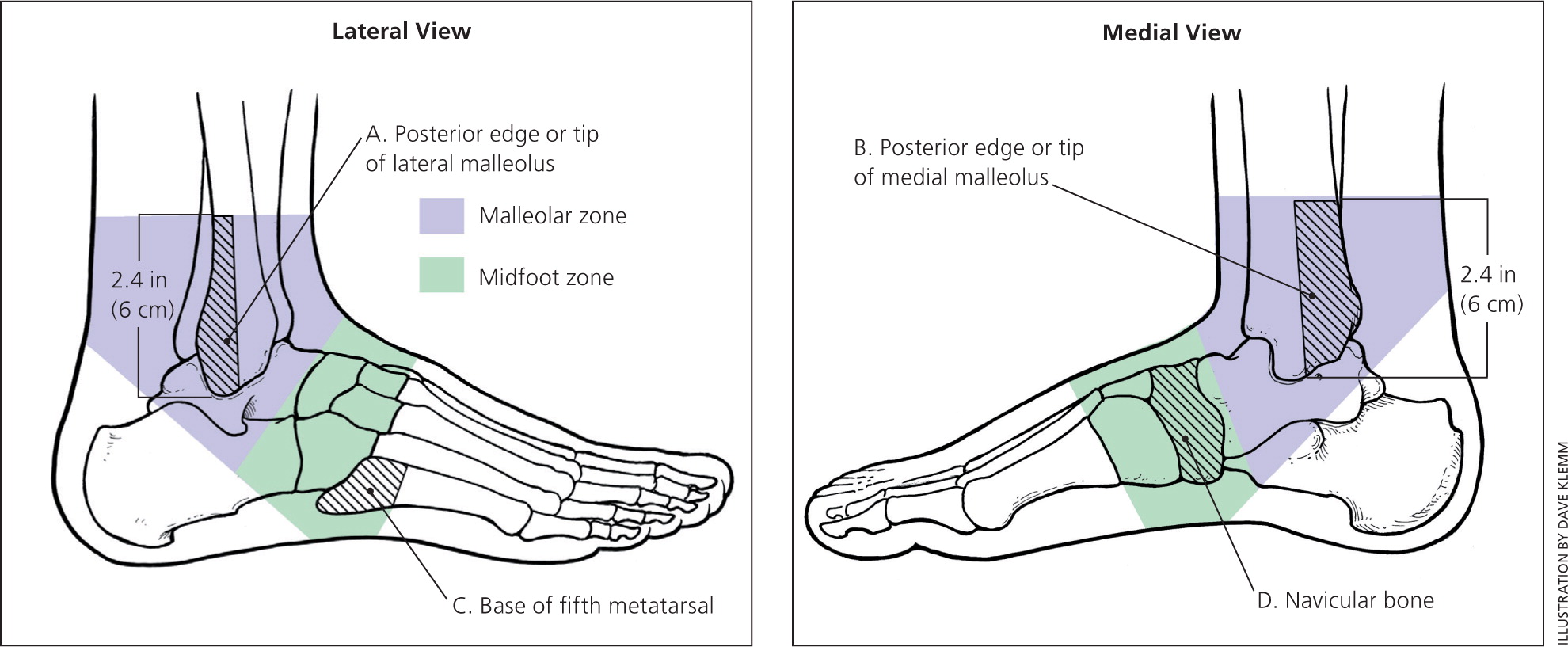
Multiple studies have demonstrated that the Ottawa ankle rules are nearly 100 percent sensitive for detecting fractures in adults and children as young as five years.6 Therefore, negative findings eliminate the need for radiography. However, because specificity is low (30 to 50 percent), positive findings do not necessarily indicate that a fracture is present, but do indicate that radiography is needed to confirm or rule out fracture.7
HIGH (SYNDESMOTIC) ANKLE SPRAIN
The tibiofibular syndesmosis refers to the joint formed by the distal ends of the tibia and fibula. This joint is supported by the anterior tibiofibular ligament, the posterior superficial and deep tibiofibular ligaments, and the interosseous membrane. A high ankle sprain is an injury to these ligaments.
High ankle sprains often occur in persons participating in football, downhill skiing, and other field sports, and may represent up to 10 percent of ankle sprains in some populations.8 This injury can occur through a variety of mechanisms similar to more common lateral sprains, although a rotational component to the injury seems to be a common factor.9
Clinical diagnosis is made by attempting to mechanically separate the distal tibia and fibula, thereby stressing the syndesmosis and eliciting pain proximal to the ankle joint. This is done by squeezing the lower leg at midcalf (squeeze test), having patients cross their legs with the injured leg resting at midcalf on the knee (crossed-leg test; Figure 33), or externally rotating the ankle with the foot dorsiflexed (rotation test).
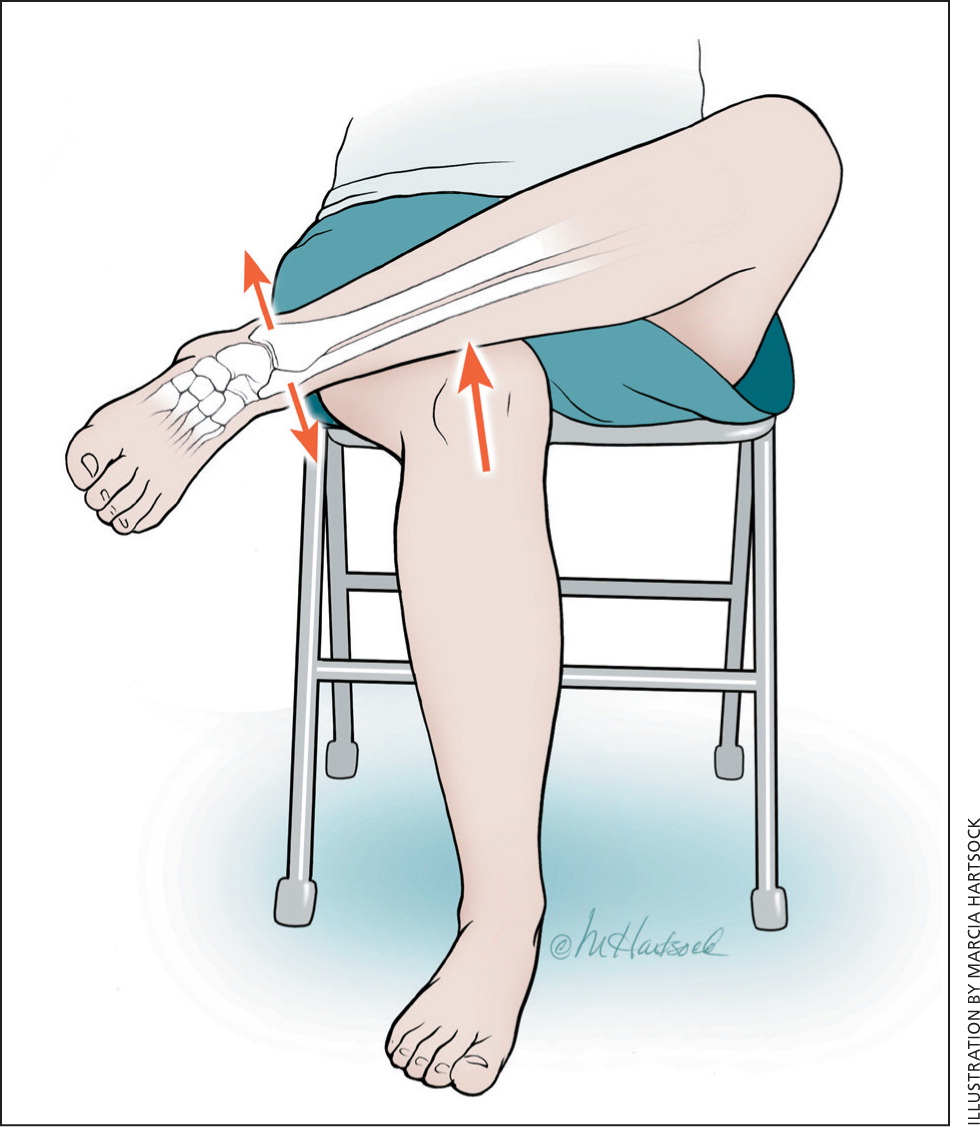
Plain radiography may show diastasis of the tibia and fibula in complete ruptures; however, magnetic resonance imaging is more accurate in identifying partial and complete ligament injuries,8 and should be considered in patients with considerable disability from an injury suggestive of a high sprain.
The severity of these injuries varies widely, but cases often result in significant time lost from work or sports (up to four to five months). Although there is increasing interest in this injury, there are no comparative studies of conservative treatment modalities or surgery.10
Treatment
CRYOTHERAPY
There is modest evidence supporting three to seven days of cryotherapy for short-term treatment of soft tissue injuries in terms of pain control11 and return to work or sports.12 Ice or cold packs should be applied directly to the injury to achieve a numbing effect, and the area should be checked periodically to avoid frostbite injury. Most studies have used a protocol of 20 minutes every two hours. However, when this protocol was compared with an intermittent protocol of 10 minutes on, 10 minutes off, and 10 minutes on every two hours for three days while awake, the intermittent protocol demonstrated greater short-term pain relief, although there were similar pain relief and functional outcomes at one week.13
COMPRESSION, SUPPORT, AND BRACING
A 2002 Cochrane review of nine trials concluded that an air stirrup brace or lace-up support is more effective than an elastic compression wrap for reducing swelling and time to return to activities in patients with ankle sprain.14 The review also found that a lace-up support is superior to an air stirrup brace for reduction of acute swelling.14 A later randomized trial confirmed the superiority of the air stirrup brace over the elastic compression wrap.15 However, another randomized trial of 172 patients compared the combination of an air stirrup brace and elastic compression wrap with either method alone, and found that the combination was superior in terms of overall joint function at the 10-day follow-up and the one-month follow-up.16
Based on these studies, an air stirrup brace combined with an elastic compression wrap, or a lace-up support alone, appears to be a better choice than an elastic compression wrap alone. A below-knee cast for 10 days applied two to three days postinjury may provide slightly better pain control and return to activity in patients with severe ankle sprains who cannot bear sufficient weight to permit ambulation with an air stirrup brace or lace-up support; however, use of a cast does not alter long-term outcomes.17
MOBILIZATION
Although the quality of studies is somewhat limited, there is evidence suggesting that early mobilization during which the patient bears weight as tolerated for daily activities (functional mobilization) is superior to prolonged rest in regard to time to return to work or sports, long-term ability to return to sports, persistent swelling, long-term ankle instability, and patient satisfaction.18 Evidence also shows that focused range-of-motion exercises started within the first week, in addition to functional mobilization, provide even greater benefits in regard to return to sports or work.19 Bearing weight and exercising can begin as soon as pain allows.
The decision about when an athlete can return to sports in a functional ankle brace is variable and depends on the severity of the sprain, the degree of pain, and the risk of reinjury. The American College of Sports Medicine, in collaboration with the American Academy of Family Physicians and other organizations, offers guidelines on the decision to return to activity (Table 1).20 The guidelines also are available in a format for coaches and athletes.21

| The status of anatomic and functional healing |
| The status of chronic injury |
| That the athlete poses no undue risk to the safety of other participants |
| Restoration of sport-specific skills |
| Psychosocial readiness |
| Ability to perform safely with equipment modification, bracing, and orthoses |
| Compliance with applicable federal, state, local, school, and governing body regulations |
ANTI-INFLAMMATORY MEDICATION
There is extensive literature on the use of nonsteroidal anti-inflammatory drugs (NSAIDs) for the treatment of acute ankle sprains and other soft tissue injuries. The potential benefit of NSAIDs in reducing excessive inflammation is countered by evidence that prolonged use can impair the healing of fractured bones and injured tendons.22
Studies of ankle sprains have shown that a variety of NSAIDs are relatively safe and superior to placebo for pain control and return to activity, including piroxicam (Feldene),23 celecoxib (Celebrex),24 diclofenac (Voltaren),25 and ibuprofen.25 Topical NSAIDs, such as diclofenac gel (Solaraze), also can provide effective pain control with fewer systemic adverse effects than oral NSAIDs.26
Comparisons of various NSAIDs have not demonstrated any one agent to be superior to another. In one study, the cyclooxygenase-2 inhibitor celecoxib was found to be comparable to the non–cyclooxygenase inhibitor naproxen (Naprosyn) in terms of global assessment and functional improvement.27 However, another study found that acetaminophen was comparable to ibuprofen for pain relief and functional results, suggesting that pain control, rather than modulation of inflammation, may be the primary benefit of NSAID therapy.28
At this time, the evidence does not support the systematic use or superiority of NSAIDs for the treatment of the inflammatory response to acute ankle sprains.29 Oral or topical NSAIDs, acetaminophen, and mild opioids are all reasonable options for pain control.
SURGERY
Surgical repair previously has been advocated as an option for the treatment of severe (grade III) acute ankle sprains. In a 2007 Cochrane review, pooled data suggested that surgery was beneficial for chronic pain, functional instability, and return to preinjury level of sport participation; however, there were major methodologic flaws that made these conclusions questionable.30 Furthermore, there were trends toward longer recovery times, more ankle stiffness, and impaired mobility in those who had surgery compared with conservative treatment.
Evidence does not clearly support immediate surgical repair of lateral ankle sprains. Consideration of surgery is best reserved for patients with chronic ankle instability who do not respond to rehabilitation.31
OTHER OPTIONS
A 2011 Cochrane review of five clinical trials found no benefit with therapeutic ultrasound for the treatment of acute ankle sprains.32 A 2005 Cochrane review of nine small trials of hyperbaric oxygen therapy on soft tissue injuries, including one on ankle sprains, found no benefits with hyperbaric oxygen therapy.33 Therefore, these therapies cannot be recommended.
Prevention
Because most ankle sprains resolve in two to six weeks, many patients do not return for follow-up. However, because a previous ankle sprain is the greatest risk factor for recurrent injuries, a more aggressive approach to follow-up is indicated.
FOLLOW-UP FOR LIGAMENTOUS INSTABILITY
Patients with significant ankle sprains should be examined four to six weeks after the injury to assess for symptoms or physical findings of ligamentous instability. The anterior drawer test (Figure 43 ) assesses the integrity of the anterior talofibular ligament. Significant anterior subluxation compared with the uninjured ankle suggests damage to this ligament. The talar tilt test (Figure 53 ) stresses the calcaneofibular ligament. Laxity compared with the uninjured ankle suggests ligament damage.
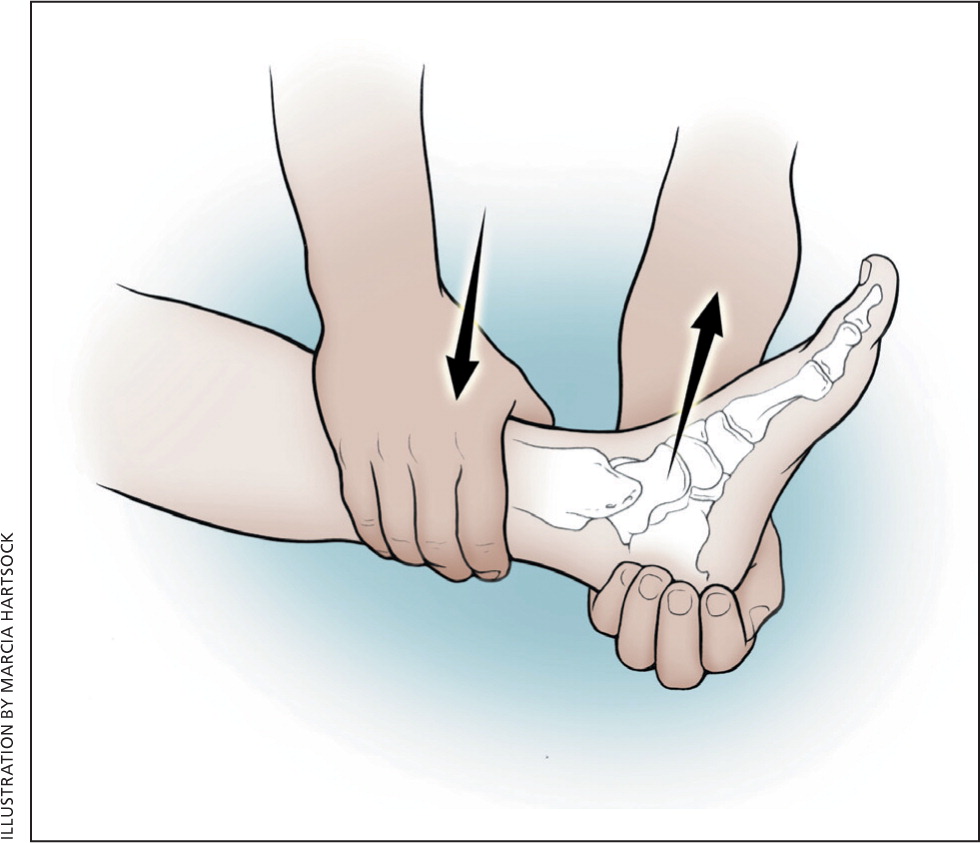
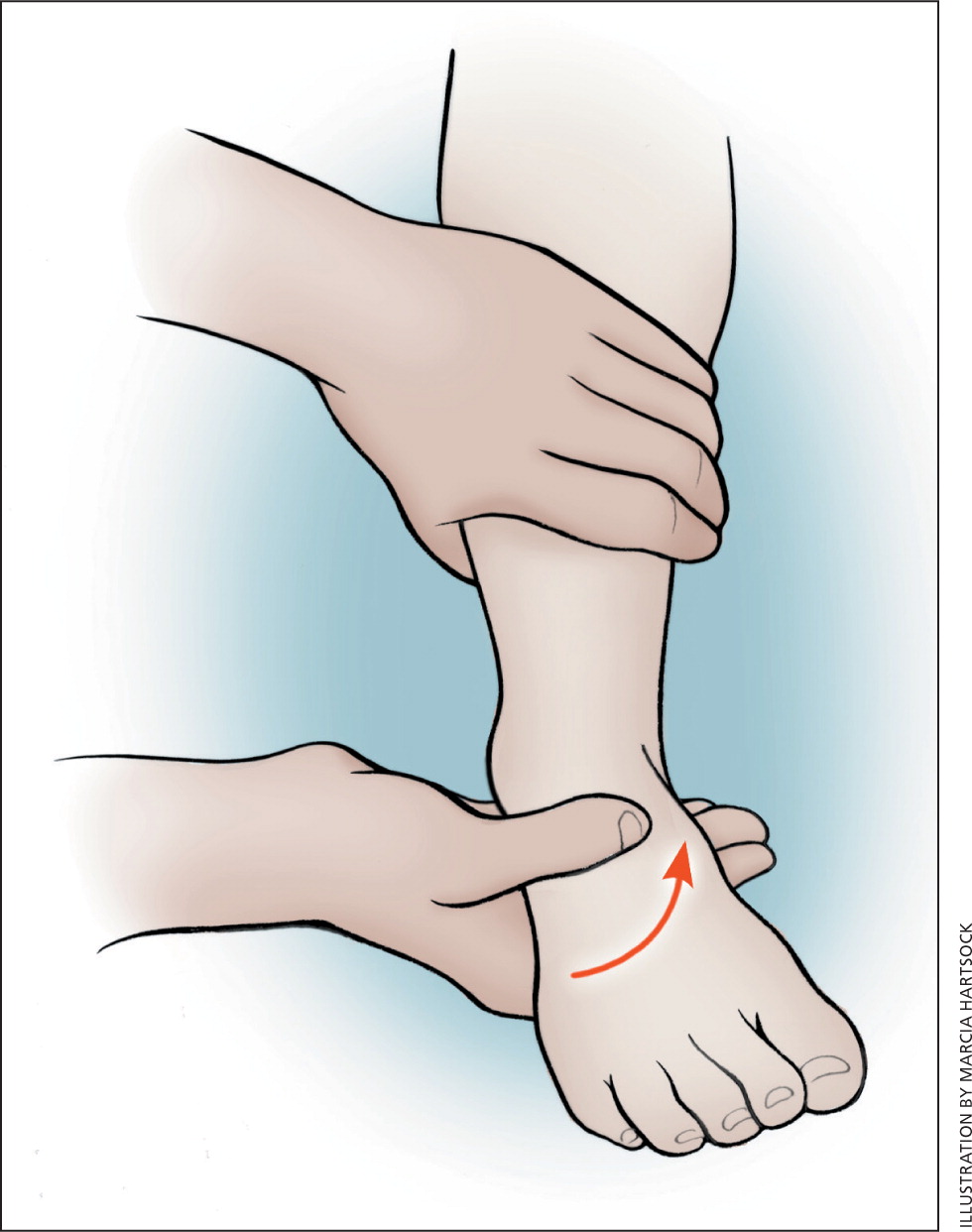
Patients with persistent instability identified by symptoms or by examination should be referred for rehabilitation. In addition, patients who are returning to high-risk activities and sports, including those without evidence of instability, should be counseled about rehabilitation exercises and taping.
REHABILITATION EXERCISES
Rehabilitation after an ankle sprain consists of specific exercises focused on proprioceptive training and strengthening (Table 234 ). There is substantial evidence that incorporating these exercises is effective at reducing future ankle injuries as well as knee, hamstring, and other lower limb injuries in athletes.35,36 All athletes returning to sports after an ankle sprain should participate in a neuromuscular training program, as should nonathletic patients who have persistent instability perceived during activity or detected on physical examination.

| Proprioception (balance training) |
| Balance on one leg for 30 to 60 seconds |
| Balance on one leg and play catch with a partner |
| Perform balance exercises on wobble board |
| One-leg mini squats with other leg extended in different directions |
| Strengthening |
| Range-of-motion exercises using resistance band |
| Calf raises |
| Plyometrics |
| Scissor hops: start in a lunge position; jump and land with the other foot forward |
| Standing squat jumps: start in a squat position; jump and land softly |
| Bounding: take large bounding steps at 50 percent of maximal running speed |
In addition to the exercises outlined in Table 2,34 there is mounting evidence that a focused sport-specific warm-up (e.g., running, cutting, skips, jumps, other sport-specific movements at gradually increasing speed) before intense exercise also reduces the risk of lower limb injuries.37 In contrast, static stretching has no effect on injury prevention, and is not recommended in the absence of or in place of a proper warm-up.38
SUPPORTS AND TAPING
Substantial evidence supports the effectiveness of air stirrup braces and lace-up supports in protecting against ankle sprains in high-risk sports.39 However, ankle taping, when applied properly, also can be effective. A 2010 review of seven studies found that taping was as effective as braces, with a 71 percent reduction in sprains with taping versus a 69 percent reduction with braces.40 However, it is important to note that taping has more variables that can influence its effectiveness, including the skill of the trainer, the sport, and the amount of playing time, all of which can reduce the effectiveness. Many athletes find the stiffness of an air stirrup or lace-up support unacceptable or detrimental to performance and thus prefer taping. An example of good taping technique can be viewed at http://www.youtube.com/watch?v=TnbKqMHgGmc&feature=related.
Data Sources: A literature search was completed in PubMed using the following keywords: ankle sprain, treatment, prevention, medications, compression, support, brace, cryotherapy, functional treatment, exercises, warm-up, and stretching. Other sources searched included the Agency for Healthcare Research and Quality evidence reports, Cochrane Database of Systematic Reviews, the National Guidelines Clearinghouse, and Essential Evidence Plus. Search date: March 6, 2011.
