Clinical Scenario
You have just completed the well-child examination of an eight-year-old boy with a body mass index (BMI) of 18.6 kg per m2 (90th percentile for age and sex). His parents recognize that he is overweight. You provide individual counseling in the office about optimal nutrition, increasing physical activity, and limiting screen time and sweetened beverages. His parents ask if enrolling him in a school-based obesity prevention program would help prevent further weight gain.
Clinical Question
Do interventions for preventing obesity in children work?
Evidence-Based Answer
Overall, children up to 12 years of age benefited from school-based obesity prevention interventions; this effect was not demonstrated among adolescents 13 years and older. Although the overall effect size was small, interventions that promoted physical activity, alone or in combination with diet, were effective in slowing or preventing increases in BMI when compared with control interventions.1 (Strength of Recommendation: C, based on consensus, disease-oriented evidence, usual practice, expert opinion, or case series.)
Cochrane Abstract
Background: Prevention of childhood obesity is an international public health priority given the significant impact of obesity on acute and chronic diseases, general health, development, and well-being. The international evidence base for strategies that governments, communities, and families can implement to prevent obesity and promote health has been accumulating, but remains unclear.
Objectives: This review aims primarily to update the previous Cochrane review of childhood obesity prevention research and determine the effectiveness of evaluated interventions intended to prevent obesity in children, assessed by change in body mass index (BMI). Secondary aims were to examine the characteristics of the programs and strategies to answer the question, “What works for whom, why, and for what cost?”
Search Methods: The searches were rerun in CENTRAL, Medline, EMBASE, PsychINFO, and CINAHL in March 2010 and relevant Web sites were searched. Non–English-language papers were included and experts were contacted.
Selection Criteria: The review includes data from childhood obesity prevention studies that used a controlled study design (with or without randomization). Studies were included if they evaluated interventions, policies, or programs in place for 12 weeks or more. If studies were randomized at a cluster level, six clusters were required.
Data Collection and Analysis: Two review authors independently extracted data and assessed the risk of bias of included studies. Data were extracted on intervention implementation, cost, equity, and outcomes. Outcome measures were grouped according to whether they measured adiposity, physical activity–related behaviors, or diet-related behaviors. Adverse outcomes were recorded. A meta-analysis was conducted using available BMI or standardized BMI (zBMI) score data with subgroup analysis by age group (zero to five years, six to 12 years, and 13 to 18 years, corresponding to stages of developmental and childhood settings).
Main Results: This review includes 55 studies (an additional 36 studies found for this update). The majority of the studies targeted children six to 12 years of age. The meta-analysis included 37 studies of 27,946 children and demonstrated that programs were effective at reducing adiposity, although not all individual interventions were effective, and there was a high level of observed heterogeneity (I2 = 82 percent). Overall, children in the intervention group had a standardized mean difference in adiposity (measured as BMI or zBMI) of –0.15 kg per m2 (95% confidence interval [CI], –0.21 to –0.09). Intervention effects by age subgroups were–0.26 kg per m2 (95% CI, –0.53 to 0.00; zero to five years), –0.15 kg per m2 (95% CI, –0.23 to –0.08; six to 12 years), and –0.09 kg per m2 (95% CI, –0.20 to 0.03; 13 to 18 years). Heterogeneity was apparent in all three age groups and could not be explained by randomization status or the type, duration, or setting of the intervention. Only eight studies reported on adverse effects, and no evidence of adverse outcomes, such as unhealthy dieting practices, increased prevalence of underweight, or body image sensitivities, was found. Interventions did not appear to increase health inequalities, although this was examined in fewer studies.
Authors’ Conclusions: The authors found strong evidence to support beneficial effects of childhood obesity prevention programs on BMI, particularly for programs targeted to children six to 12 years of age. However, given the unexplained heterogeneity and the likelihood of small study bias, these findings must be interpreted cautiously. A broad range of program components were used in these studies, and although it is not possible to distinguish which of these components contributed most to the beneficial effects observed, our synthesis indicates the following to be promising policies and strategies:
- School curriculum that includes healthy eating, physical activity, and positive body image
- Increased sessions for physical activity and the development of fundamental movement skills throughout the school week
- Improvements in the nutritional quality of the food supply in schools
- Environments and cultural practices that support children eating healthier foods and being active throughout each day
- Support for teachers and other staff to implement health promotion strategies and activities (e.g., professional development, capacity-building activities)
- Parent support and home activities that encourage children to be more active, eat more nutritious foods, and spend less time in screen-based activities
However, study and evaluation designs need to be strengthened, and reporting should be extended to capture process and implementation factors, outcomes in relation to measures of equity, longer-term outcomes, potential harms, and costs.
Childhood obesity prevention research must now move toward identifying how effective intervention components can be embedded within health, education, and care systems, and achieve long-term sustainable impacts.
These summaries have been derived from Cochrane reviews published in the Cochrane Database of Systematic Reviews in the Cochrane Library. Their content has, as far as possible, been checked with the authors of the original reviews, but the summaries should not be regarded as an official product of the Cochrane Collaboration; minor editing changes have been made to the text (http://www.cochrane.org).
Practice Pointers
In the United States, 32 percent of children and adolescents two to 19 years of age are overweight,2 and 17 percent are obese.3 Childhood obesity is associated with an increased incidence of hypertension, dyslipidemia, diabetes mellitus, asthma, mental health disorders, and adult obesity.4,5 If current trends in childhood obesity continue, there will be an additional 65 million obese adults in the United States by 2030. This translates into a potential 6 to 8.5 million additional cases of diabetes, 5 to 7.3 million additional cases of heart disease, and 492,000 to 669,000 additional cases of cancer at an estimated direct medical cost of $48 to $66 billion.6
This Cochrane review examined the effectiveness of multiple interventions designed to prevent obesity among children and adolescents. These interventions focused on diet and nutrition, physical activity, and lifestyle, alone or in combination. Most were conducted fully or partially at schools, meaning that children had to attend a specific school to be eligible for enrollment in the target program. Although outcomes such as skinfold thickness, percentage of body fat, and prevalence of overweight and obesity were described, BMI and standardized BMI (adjusted for child age and sex) were the most consistently reported outcome measures. Individual studies predominantly showed a beneficial change or no change in BMI or standardized BMI in the intervention groups when compared with control patients. When the results of all the studies were combined in a meta-analysis, children in the intervention groups had a –0.15 (95% confidence interval, –0.21 to –0.09) standardized mean change in BMI or standardized BMI compared with control patients.1 Similar changes in BMI have been linked to decreased blood pressure and insulin levels and an improved lipid profile and aerobic fitness level.7
Some studies in the meta-analysis looked at physical activity, others at dietary interventions, and others at a combination of the two. Patients in groups that included some component of physical activity saw a significant decrease in BMI change compared with control patients. When studies of dietary interventions alone were pooled, they showed no difference in BMI change between intervention and control patients. Pooled analysis revealed that interventions were effective in children up to 12 years of age, but found no statistically significant benefit in adolescents 13 to 18 years of age.
In the United States, preventing childhood obesity is of national public interest. The U.S. Preventive Services Task Force recommends that physicians screen for obesity in children six years and older, based on evidence that screening and intervention provide a net benefit with respect to weight status.8 The Guide to Community Preventive Services, on the other hand, states that there is insufficient evidence to support physician education, feedback, or reminders to prevent and control obesity. However, the Community Guide does recommend work site programs, community-level behavioral interventions to reduce screen time, and technology-supported coaching and counseling to promote and maintain weight loss.9
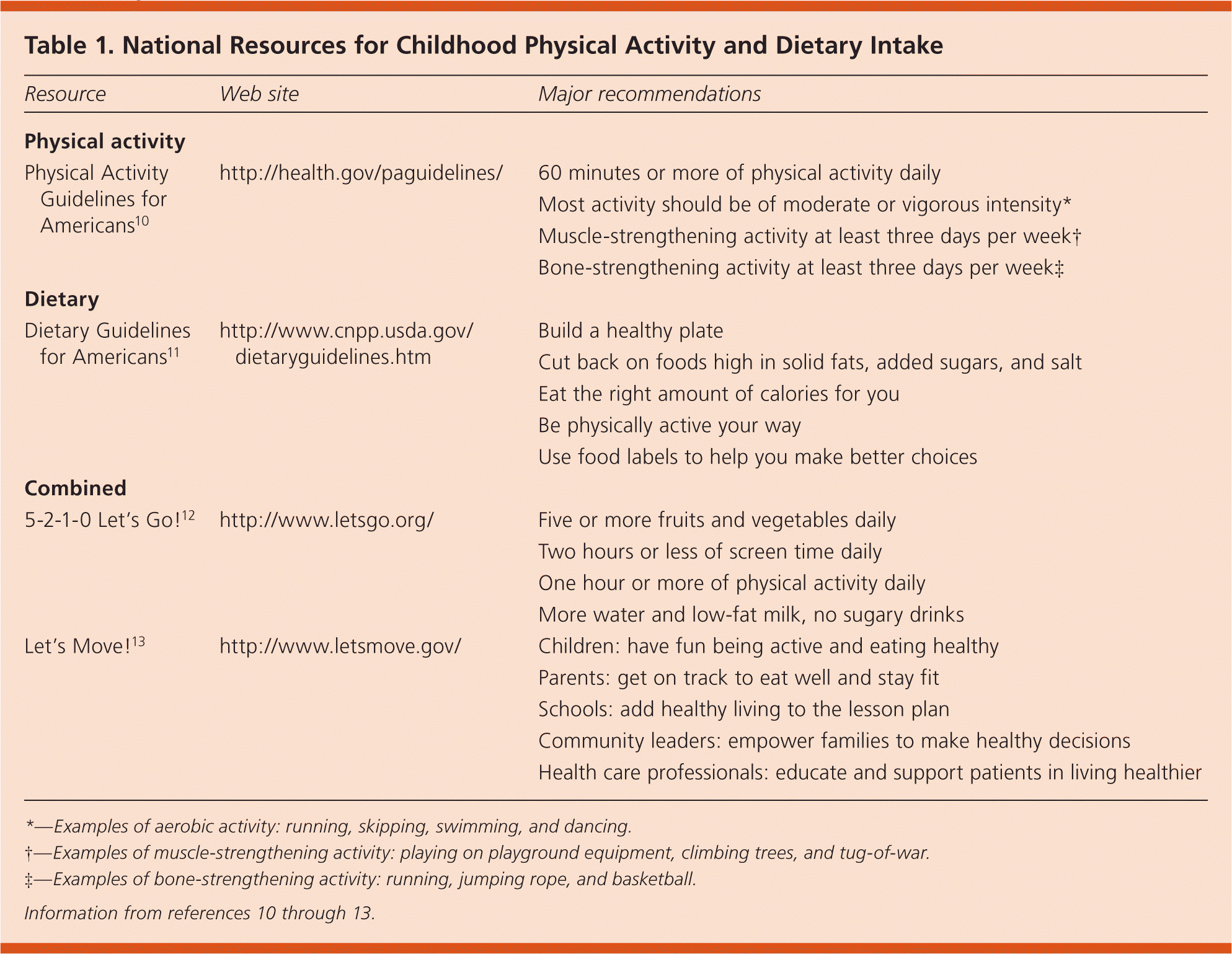
Programs such as the 2008 Physical Activity Guidelines for Americans, the Dietary Guidelines for Americans, the “5–2–1–0 Let’s Go!” program, and the Let’s Move! campaign provide sample community-based structured recommendations for childhood physical activity and dietary intake (Table 1).10–13 This updated Cochrane review provides evidence that these and other programs can help prevent childhood obesity. As a result, primary care physicians should encourage parents, educators, and policy makers to consider the use of these programs.
Table 1. National Resources for Childhood Physical Activity and Dietary Intake
| Resource | Web site | Major recommendations |
|---|---|---|
| Physical activity | ||
| Physical Activity Guidelines for Americans10 | http://health.gov/paguidelines/ | 60 minutes or more of physical activity daily |
| Most activity should be of moderate or vigorous intensity* | ||
| Muscle-strengthening activity at least three days per week† | ||
| Bone-strengthening activity at least three days per week‡ | ||
| Dietary | ||
| Dietary Guidelines for Americans11 | http://www.cnpp.usda.gov/dietaryguidelines.htm | Build a healthy plate |
| Cut back on foods high in solid fats, added sugars, and salt | ||
| Eat the right amount of calories for you | ||
| Be physically active your way | ||
| Use food labels to help you make better choices | ||
| Combined | ||
| 5-2-1-0 Let’s Go!12 | http://www.letsgo.org/ | Five or more fruits and vegetables daily |
| Two hours or less of screen time daily | ||
| One hour or more of physical activity daily | ||
| More water and low-fat milk, no sugary drinks | ||
| Let’s Move!13 | http://www.letsmove.gov/ | Children: have fun being active and eating healthy |
| Parents: get on track to eat well and stay fit | ||
| Schools: add healthy living to the lesson plan | ||
| Community leaders: empower families to make healthy decisions | ||
| Health care professionals: educate and support patients in living healthier | ||
*—Examples of aerobic activity: running, skipping, swimming, and dancing.
†—Examples of muscle-strengthening activity: playing on playground equipment, climbing trees, and tug-of-war.
‡—Examples of bone-strengthening activity: running, jumping rope, and basketball.

