
This is an updated and corrected version of the article that appeared in print.
Am Fam Physician. 2012;86(2):173-180
Patient information: A handout on this topic is available at https://familydoctor.org/familydoctor/en/diseases-conditions/shortness-of-breath.html.
Author disclosure: No relevant financial affiliations to disclose.
Chronic dyspnea is shortness of breath that lasts more than one month. The perception of dyspnea varies based on behavioral and physiologic responses. Dyspnea that is greater than expected with the degree of exertion is a symptom of disease. Most cases of dyspnea result from asthma, heart failure and myocardial ischemia, chronic obstructive pulmonary disease, interstitial lung disease, pneumonia, or psychogenic disorders. The etiology of dyspnea is multi-factorial in about one-third of patients. The clinical presentation alone is adequate to make a diagnosis in 66 percent of patients with dyspnea. Patients' descriptions of the sensation of dyspnea may be helpful, but associated symptoms and risk factors, such as smoking, chemical exposures, and medication use, should also be considered. Examination findings (e.g., jugular venous distention, decreased breath sounds or wheezing, pleural rub, clubbing) may be helpful in making the diagnosis. Initial testing in patients with chronic dyspnea includes chest radiography, electrocardiography, spirometry, complete blood count, and basic metabolic panel. Measurement of brain natriuretic peptide levels may help exclude heart failure, and d-dimer testing may help rule out pulmonary emboli. Pulmonary function studies can be used to identify emphysema and interstitial lung diseases. Computed tomography of the chest is the most appropriate imaging study for diagnosing suspected pulmonary causes of chronic dyspnea. To diagnose pulmonary arterial hypertension or certain interstitial lung diseases, right heart catheterization or bronchoscopy may be needed.
Chronic dyspnea has been defined as shortness of breath lasting longer than one month.1 A consensus statement from the American Thoracic Society defines dyspnea as a “subjective experience of breathing discomfort that consists of qualitatively distinct sensations that vary in intensity.”2 When shortness of breath is greater than expected for a given level of exertion, it is considered pathologic and a symptom of disease.3
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Electrocardiography and measurement of brain natriuretic peptide levels should be ordered if heart failure is suspected. | C | 1 |
| In patients with dyspnea, spirometry should be performed to diagnose airflow obstruction. | C | 24 |
| Measurement of maximal inspiratory and expiratory pressures should be done when neuromuscular causes of dyspnea are suspected. | C | 7 |
| In chronic dyspnea likely due to diffuse pulmonary disease, when the diagnosis is unclear, high-resolution noncontrast computed tomography of the chest should be performed. [updated] | C | 8 |
| Ventilation/perfusion lung scanning should be done in patients with unexplained pulmonary hypertension to exclude chronic thromboembolic pulmonary hypertension. | C | 31 |
Patients with chronic dyspnea present with stable, but not necessarily normal, vital signs. In addition to a history and physical examination, several diagnostic tests have been shown to be valuable in clarifying the underlying problem and planning appropriate treatment.
Diagnostic Considerations
Chemoreceptors in the brain and vascular system, mechanoreceptors in the chest wall and diaphragm, and pulmonary vagal receptors are thought to regulate breathing. Cortical cerebral pathways allow conscious appraisal of the chemical environment and the mechanical status of the lungs. Dissociation between the motor command and the mechanical response of the respiratory system may produce a sensation of respiratory discomfort.2
The perception of dyspnea derives from multiple physiologic and environmental factors, and may induce secondary physiologic and behavioral responses.2 Descriptions of sensations from patients are generally not attributable to a specific diagnosis. Psychogenic dyspnea may be an acute presentation or a background symptom in generalized anxiety disorder.4 Depression has been associated with an increase in chronic obstructive pulmonary disease (COPD) exacerbations.5
Causes of Dyspnea
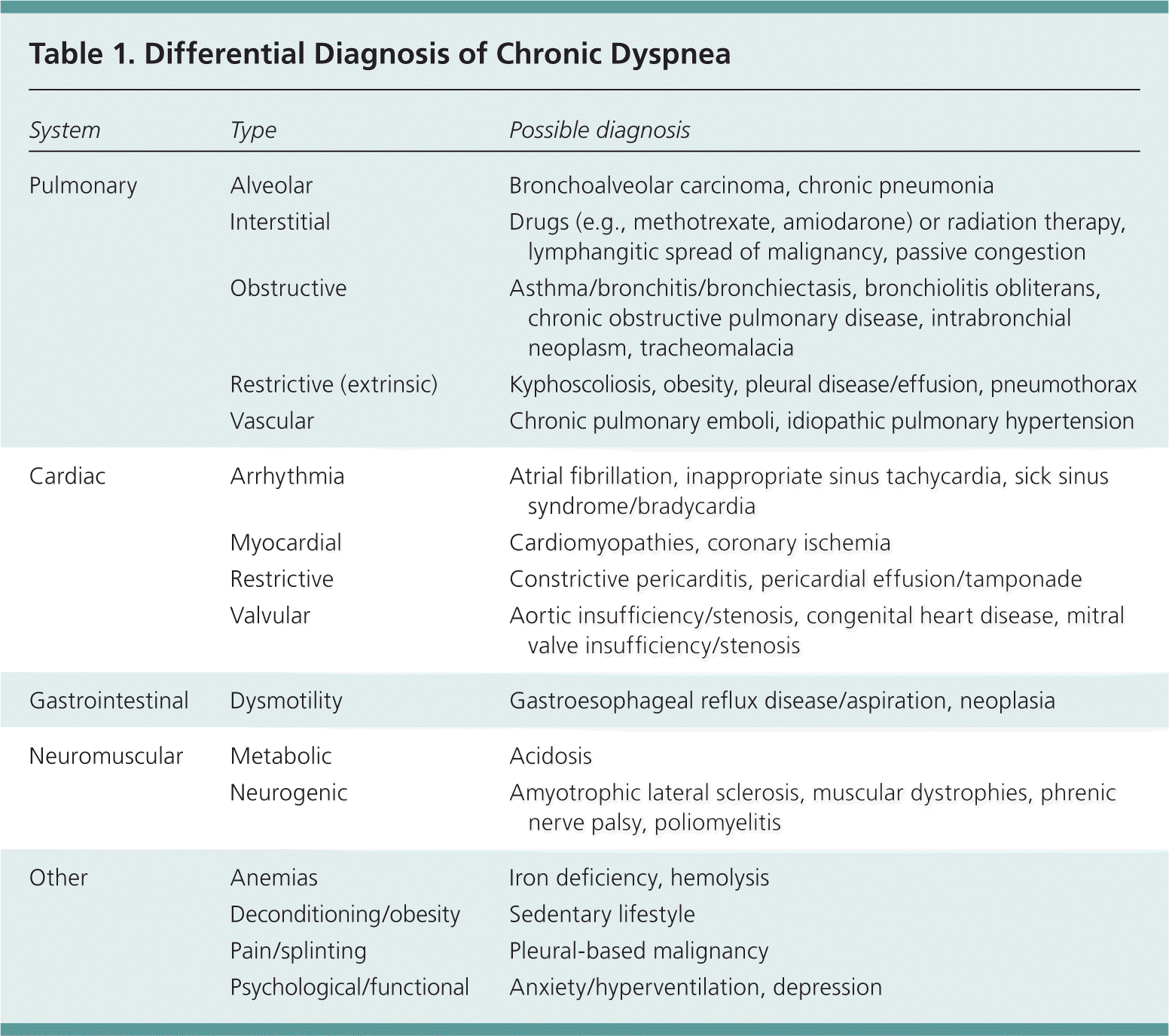
| System | Type | Possible diagnosis |
|---|---|---|
| Pulmonary | Alveolar | Bronchoalveolar carcinoma, chronic pneumonia |
| Interstitial | Drugs (e.g., methotrexate, amiodarone) or radiation therapy, lymphangitic spread of malignancy, passive congestion | |
| Obstructive | Asthma/bronchitis/bronchiectasis, bronchiolitis obliterans, chronic obstructive pulmonary disease, intrabronchial neoplasm, tracheomalacia | |
| Restrictive (extrinsic) | Kyphoscoliosis, obesity, pleural disease/effusion, pneumothorax | |
| Vascular | Chronic pulmonary emboli, idiopathic pulmonary hypertension | |
| Cardiac | Arrhythmia | Atrial fibrillation, inappropriate sinus tachycardia, sick sinus syndrome/bradycardia |
| Myocardial | Cardiomyopathies, coronary ischemia | |
| Restrictive | Constrictive pericarditis, pericardial effusion/tamponade | |
| Valvular | Aortic insufficiency/stenosis, congenital heart disease, mitral valve insufficiency/stenosis | |
| Gastrointestinal | Dysmotility | Gastroesophageal reflux disease/aspiration, neoplasia |
| Neuromuscular | Metabolic | Acidosis |
| Neurogenic | Amyotrophic lateral sclerosis, muscular dystrophies, phrenic nerve palsy, poliomyelitis | |
| Other | Anemias | Iron deficiency, hemolysis |
| Deconditioning/obesity | Sedentary lifestyle | |
| Pain/splinting | Pleural-based malignancy | |
| Psychological/functional | Anxiety/hyperventilation, depression |
Asthma, congestive heart failure and myocardial ischemia, COPD, interstitial lung disease, pneumonia, and psychogenic disorders account for approximately 85 percent of all cases of shortness of breath.7 Cardiac and pulmonary etiologies predominate. The etiology of chronic dyspnea is multifactorial in up to one-third of patients.8 Although a definitive etiology is usually found, one study showed that clinical presentation alone is adequate to make a diagnosis in 66 percent of patients with dyspnea.9 Table 2 provides a summary of clues in the evaluation of chronic dyspnea.
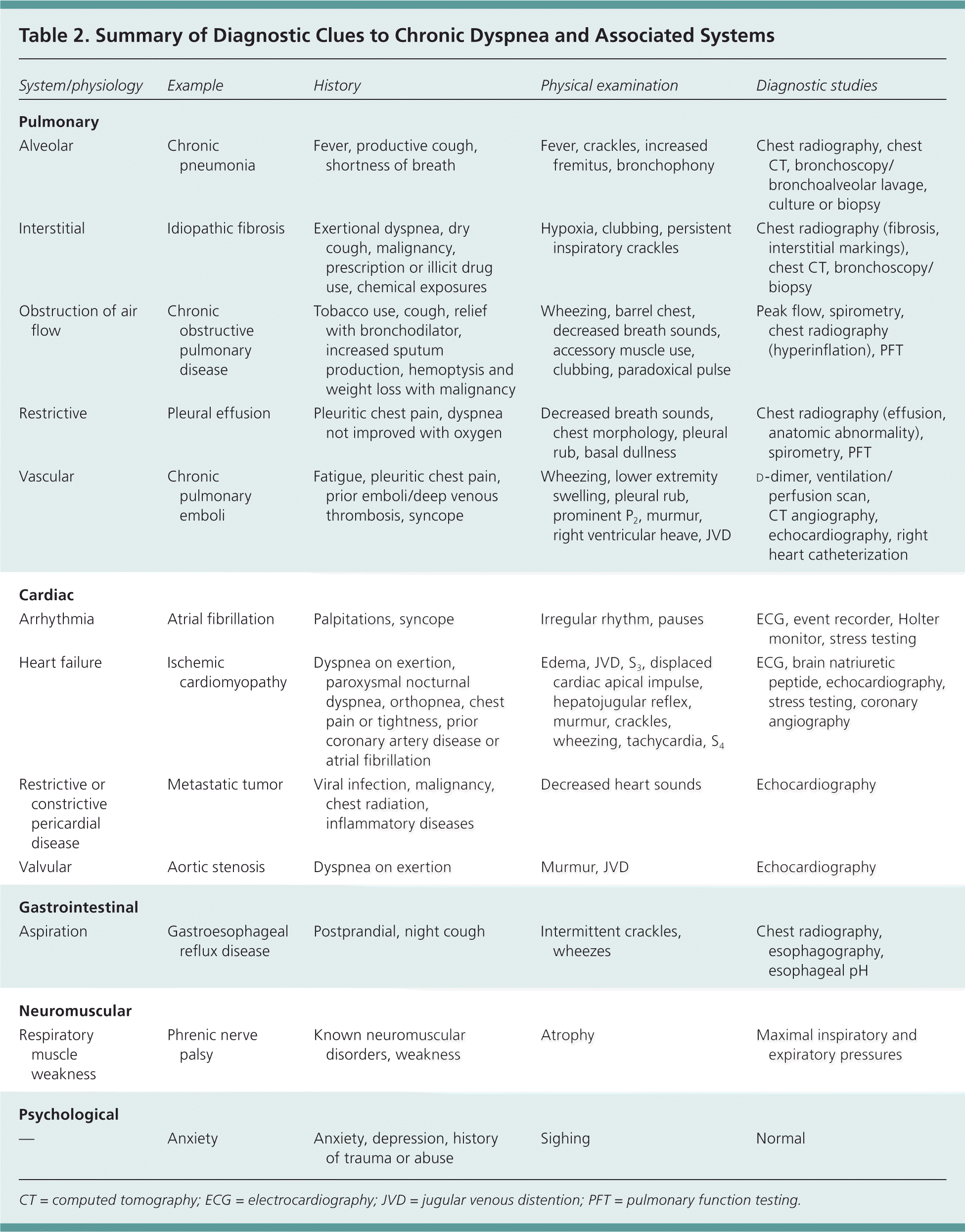
| System/physiology | Example | History | Physical examination | Diagnostic studies |
|---|---|---|---|---|
| Pulmonary | ||||
| Alveolar | Chronic pneumonia | Fever, productive cough, shortness of breath | Fever, crackles, increased fremitus, bronchophony | Chest radiography, chest CT, bronchoscopy/bronchoalveolar lavage, culture or biopsy |
| Interstitial | Idiopathic fibrosis | Exertional dyspnea, dry cough, malignancy, prescription or illicit drug use, chemical exposures | Hypoxia, clubbing, persistent inspiratory crackles | Chest radiography (fibrosis, interstitial markings), chest CT, bronchoscopy/biopsy |
| Obstruction of air flow | Chronic obstructive pulmonary disease | Tobacco use, cough, relief with bronchodilator, increased sputum production, hemoptysis and weight loss with malignancy | Wheezing, barrel chest, decreased breath sounds, accessory muscle use, clubbing, paradoxical pulse | Peak flow, spirometry, chest radiography (hyperinflation), PFT |
| Restrictive | Pleural effusion | Pleuritic chest pain, dyspnea not improved with oxygen | Decreased breath sounds, chest morphology, pleural rub, basal dullness | Chest radiography (effusion, anatomic abnormality), spirometry, PFT |
| Vascular | Chronic pulmonary emboli | Fatigue, pleuritic chest pain, prior emboli/deep venous thrombosis, syncope | Wheezing, lower extremity swelling, pleural rub, prominent P2, murmur, right ventricular heave, JVD | d-dimer, ventilation/ perfusion scan, CT angiography, echocardiography, right heart catheterization |
| Cardiac | ||||
| Arrhythmia | Atrial fibrillation | Palpitations, syncope | Irregular rhythm, pauses | ECG, event recorder, Holter monitor, stress testing |
| Heart failure | Ischemic cardiomyopathy | Dyspnea on exertion, paroxysmal nocturnal dyspnea, orthopnea, chest pain or tightness, prior coronary artery disease or atrial fibrillation | Edema, JVD, S3, displaced cardiac apical impulse, hepatojugular reflex, murmur, crackles, wheezing, tachycardia, S4 | ECG, brain natriuretic peptide, echocardiography, stress testing, coronary angiography |
| Restrictive or constrictive pericardial disease | Metastatic tumor | Viral infection, malignancy, chest radiation, inflammatory diseases | Decreased heart sounds | Echocardiography |
| Valvular | Aortic stenosis | Dyspnea on exertion | Murmur, JVD | Echocardiography |
| Gastrointestinal | ||||
| Aspiration | Gastroesophageal reflux disease | Postprandial, night cough | Intermittent crackles, wheezes | Chest radiography, esophagography, esophageal pH |
| Neuromuscular | ||||
| Respiratory muscle weakness | Phrenic nerve palsy | Known neuromuscular disorders, weakness | Atrophy | Maximal inspiratory and expiratory pressures |
| Psychological | ||||
| — | Anxiety | Anxiety, depression, history of trauma or abuse | Sighing | Normal |
History
To clarify dyspnea, the patient history should address the onset, character, duration, severity, periodicity, and progression of symptoms. Aggravating and ameliorating factors also should be noted.
Patients with heart failure may have air hunger or a suffocating sensation, and those with asthma often describe a sensation of chest tightness.2 An exacerbation of heart failure may be described as a sensation of shortness of breath with exertion.3 The sense of increased effort of breathing is a common feature of conditions characterized by abnormal mechanical loads (e.g., COPD, interstitial lung disease) and neuromuscular weakness.2
Airway obstruction, including COPD, should be suspected in patients who are short of breath with cough or with increased sputum production, especially those with a history of smoking. Wheezing also is a common symptom in patients with airway obstruction10 but, like cough, may be present in those with asthma or heart failure. Patients may have advanced airflow limitation but only mild dyspnea.11
Standard inventories to determine the association between level of activity and dyspnea are available.2 A five-item scale that assesses age, wheezing, dyspnea, smoking, and cough may be helpful in identifying patients who should be assessed with spirometry (Figure 1).12 Using a cutoff value of 18 or less, the negative predictive value of the questionnaire is 92.3 percent, with an 82.6 percent sensitivity for the diagnosis of COPD.12

Patients with intermittent symptoms may be experiencing episodes of reflux and aspiration, or recurrent pulmonary emboli. Heart failure may be variable and progressive over time. COPD, pulmonary hypertension, interstitial lung diseases, and neuromuscular disorders typically are insidious.7
Fever may be associated with infectious, inflammatory, or neoplastic processes. Postprandial or recumbent dyspnea may indicate gastroesophageal reflux disease or aspiration.7 Pleuritic chest discomfort is associated with stimulation of chest wall afferent nerves and may indicate malignancy, pleural-based infection, or pulmonary infarction.
Use of beta blockers may aggravate asthma. Amiodarone and methotrexate are associated with interstitial toxicity and pulmonary fibrosis.13,14 Asbestos exposure causes interstitial disease and malignancies; bird exposure or illicit drug use may cause interstitial or bronchoalveolar inflammation or infection.
Immobility, prolonged travel, or malignancy may suggest thromboembolic disease, which can result in progressive pulmonary hypertension. Response to treatments such as afterload reduction, diuretics, or bronchodilators can provide clues to the underlying disease process.
Physical Examination
Initial appearance, weight, vital signs, peak flow, and pulse oximetry provide important suggestions of underlying physiology. Paradoxical pulse (exaggerated variation in blood pressure with respiration) may suggest COPD, asthma, or pericardial disease.15 Tachycardia may accompany decompensation or anemia. Initial clinical judgment is helpful in diagnosing heart failure when COPD is present.16
Jugular venous distention in a setting of dyspnea suggests congestive heart failure.16 Accessory muscle use, decreased diaphragmatic excursions, unilateral dullness, hyperresonance, and abnormal breath sounds, including wheezes and crackles, should be noted. The dominant examination finding in patients with bronchiectasis is pulmonary crackles or rales, generally bibasilar.17 Decreased breath sounds and wheezing support the presence of COPD.18
Hepatomegaly, ascites, hepatojugular reflux, or edema can be caused by right-sided heart failure or pulmonary hypertension. The presence of clubbing should prompt evaluation to exclude lung cancer, bronchiectasis, or idiopathic pulmonary fibrosis.20
Initial Diagnostic Studies
Following the history and physical examination, initial testing should include pulse oximetry, complete blood count, basic metabolic panel, chest radiography, electrocardiography and, commonly, spirometry. If the diagnosis remains unclear after these tests, anxiety or hyperventilation, deconditioning, or neuromuscular disease should be considered.7 An algorithm for evaluating patients with chronic dyspnea is available at https://www.aafp.org/afp/2005/0415/p1529.html.
CHEST RADIOGRAPHY
Chest radiography is important in evaluating patients with chronic dyspnea of suspected pulmonary origin with or without other physical examination findings. Negative chest radiography does not rule out infiltrative lung disease. Chest radiography is appropriate for patients with heart failure in the setting of new signs or symptoms. In about one-half of patients with chronic heart failure, cardiomegaly is visible on radiography, and evidence of specific chamber enlargement is helpful in detecting valvular heart disease.6
ELECTROCARDIOGRAPHY
Electrocardiography may confirm rhythm abnormality as a factor in dyspnea, and should be ordered if heart failure is suspected.1 Underlying heart disease, electrolyte abnormalities, or systemic disease should be considered. A history of atrial fibrillation increases the likelihood of congestive heart failure.16 Ongoing ischemia or prior infarction may be discovered. Low precordial QRS voltages may be caused by pericardial effusion, infiltrative heart disease, COPD, hypothyroidism, or obesity.3 Electrocardiography has a high sensitivity, but low specificity, for determining the presence of left ventricular systolic dysfunction.23
SPIROMETRY
In patients with dyspnea, spirometry should be performed to diagnose airflow obstruction.24 A reduced forced expiratory volume in one second (FEV1) or FEV1/forced vital capacity (FVC) ratio indicates obstructive airway disease, such as COPD, chronic bronchitis, or asthma; restrictive lung disease is suggested by reduced FVC and normal or increased FEV1/FVC ratio, but must be confirmed by measurement of lung volumes.7,15 The flow-volume loop differentiates intra- or extrathoracic obstruction, and fixed or variable obstructive disorders.25
LABORATORY EVALUATION
Initial laboratory testing for chronic shortness of breath should include a complete blood count and basic metabolic panel. Anemia may cause dyspnea, and polycythemia may indicate chronic hypoxia. Leukocytosis or neutropenia, as well as abnormalities in white blood cell differential, may suggest underlying infectious or immune processes. Carbon dioxide retention indicates reduced gas exchange compatible with COPD or advanced interstitial lung disease.
Brain natriuretic peptide (BNP) is a cardiac neurohormone secreted by myocardium in response to ventricular wall tension.3 In patients with dyspnea, plasma N-terminal pro-BNP concentrations are increased in left ventricular dilatation, hypertrophy, systolic dysfunction, or diastolic dysfunction, but not by pulmonary dysfunction.21 BNP and N-terminal pro-BNP levels can be used to distinguish between heart failure and pulmonary causes of dyspnea.26,27
d-dimer is a marker of fibrin degradation. Plasma levels of d-dimer are directly related to the severity of pulmonary emboli and can help define the risk of recurrence of thromboembolic disease. A negative test can help exclude pulmonary embolus in patients with low pretest probability.28
Advanced Studies
Additional testing depends on the suspected cause of dyspnea, and may include comprehensive pulmonary function tests, echocardiography, computed tomography (CT), ventilation/perfusion scanning, stress testing, bronchoscopy or, occasionally, right or left heart catheterization.
COMPREHENSIVE PULMONARY FUNCTION TESTS
Pulmonary function tests include blood gas evaluation, lung volume measurement (i.e., residual volume, functional residual capacity, and total lung capacity) and carbon monoxide diffusion in the lung (DLCO), in addition to spirometry. Total lung capacity is reduced in persons with parenchymal restrictive disease, but is normal or increased in those who have obstructive disorders with air trapping.1 In a patient who has normal spirometry and lung volumes but a reduced DLCO, the differential diagnosis includes anemia, early interstitial lung disease, and pulmonary vascular disease. Patients with emphysema typically have low DLCO. In patients with bronchiectasis, dyspnea is more closely correlated with lung hyperinflation than with airflow obstruction parameters.29 Reduced maximal inspiratory and expiratory pressures is evidence of neuromuscular causes of dyspnea.7
ECHOCARDIOGRAPHY
The American College of Cardiology and the American Heart Association recommend echocardiography (or alternative imaging) when heart failure is suspected.30 Like chest radiography, transthoracic echocardiography is appropriate for patients with dyspnea of suspected cardiac origin.6 Helpful data obtained include right ventricular and pulmonary artery pressures, ejection fraction, wall thickness and compliance, and valvular anomalies.
COMPUTED TOMOGRAPHY
In chronic dyspnea of uncertain diagnosis likely due to diffuse pulmonary disease, the most appropriate imaging study is high-resolution noncontrast chest CT. Chronic or acute pulmonary embolism may need to be excluded using CT contrast angiography.8 CT is helpful in diagnosing inflammatory disorders or malignancies, interstitial lung disease, mediastinal disease, or occult emphysema. [updated]
VENTILATION/PERFUSION SCANNING
In patients with unexplained pulmonary hypertension, ventilation/perfusion scanning should be performed to exclude chronic thromboembolic pulmonary hypertension.31 Ventilation/perfusion scanning is more sensitive than CT pulmonary angiography for detection of chronic thromboembolic pulmonary disease in patients with pulmonary hypertension.32
STRESS TESTING
Cardiovascular stress testing with or without imaging may clarify the likelihood of coronary ischemia. Cardiopulmonary stress testing provides information on ventilatory gas exchange during exercise testing and metabolic oxygen demands.33 This may further clarify difficult to define dyspnea.
LESS COMMON AND INVASIVE TESTING
Diagnostic bronchoscopy, complemented by bronchiolar lavage or biopsy, may be needed to clarify interstitial lung diseases, such as sarcoidosis or malignancy, and confirm atypical or fungal infectious processes. Right heart catheterization is required to confirm the diagnosis of pulmonary arterial hypertension, to assess the severity of the hemodynamic impairment, and to test the vasoreactivity of the pulmonary circulation.31 Gallium scanning occasionally may be used to identify inflammatory, neoplastic, or infectious processes.7
Data Sources: Literature searches were performed in Essential Evidence Plus, PubMed, Dynamed, and Database of Reviews of Effects (DARE–Centre for Reviews and Dissemination). Search terms included dyspnea, chronic dyspnea, COPD, pulmonary arterial hypertension, interstitial lung disease, congestive heart failure, thromboembolic disease, pulmonary function testing, spirometry, and right heart catheterization. Guidelines of the American Thoracic Society, the American College of Radiology, and the American Heart Association also were reviewed. Search date: November 1, 2010.
Editor's Note: Table 3 has been removed from this article due to the identification of multiple errors and inconsistencies with the cited references that were discovered during a subsequent review.
