Most patients who are seriously ill experience grief when confronted with the losses and limitations imposed by the illness. Grief is a reaction to any loss.1 Grief manifests as emotional, social, spiritual, physical, cognitive, and behavioral changes through which a person attempts to reorganize and resolve or adjust to loss at his or her own pace.2,3 A seriously ill patient's grief manifests itself as loss-oriented grief or restoration-oriented grief.4 Loss-oriented grief is focused on the patient's struggle coming to terms with having a serious illness, and includes sentiments like, “I have difficulty accepting that I have this illness.”4 Restoration-oriented grief is focused on assimilating the losses imposed by the illness, and includes sentiments like, “I plan to make the most of the time I have left.”4 In contrast, depression is neither universal nor normal in patients who are seriously ill.5
Differentiating between grief and depression in a patient who is seriously ill is important because the management strategies for each condition are different. It can be difficult to distinguish between depression and grief because they have overlapping symptoms (i.e., sadness, crying, loss of appetite, weight, sleep) and may coexist.4,6 Thus, affective and somatic symptoms are typically unhelpful in identifying depression. Instead, cognitive manifestations of depression, such as anhedonia (loss of pleasure), hopelessness, worthlessness, loss of self-esteem, active and persistent desire for an early death, and persistent dysphoria, are hallmarks of depression.
There is a common belief that serious illness invariably leads to a loss of total pleasure and to complete hopelessness. However, most patients who are seriously ill work hard to accept that they have a potentially limited life span, to reestablish a new equilibrium that incorporates the knowledge of life with impending death, and to try to make the most of the remaining time. Many find joy in spending time with their loved ones and relishing the simple pleasures of life. One of my patients who was dying of cancer was intensely grieving over the fact that she would not be alive to raise her young daughter. However, she always greatly enjoyed my visits, especially when I would bring her a slice of hot apple pie with a scoop of her favorite vanilla ice cream and sit down to help her plan for completing some of her life goals.
As patients progress through serious illness, hope shifts. Hope for a cure may change to hope for better symptom control or hope for reconciliation with estranged loved ones. The loss of hope is an excellent indicator of underlying clinical depression. Approximately one in five patients who are seriously ill is likely depressed.7 Early identification and aggressive management of depression with a combination of pharmacologic and nonpharmacologic modalities are effective and may alleviate suffering in these patients.
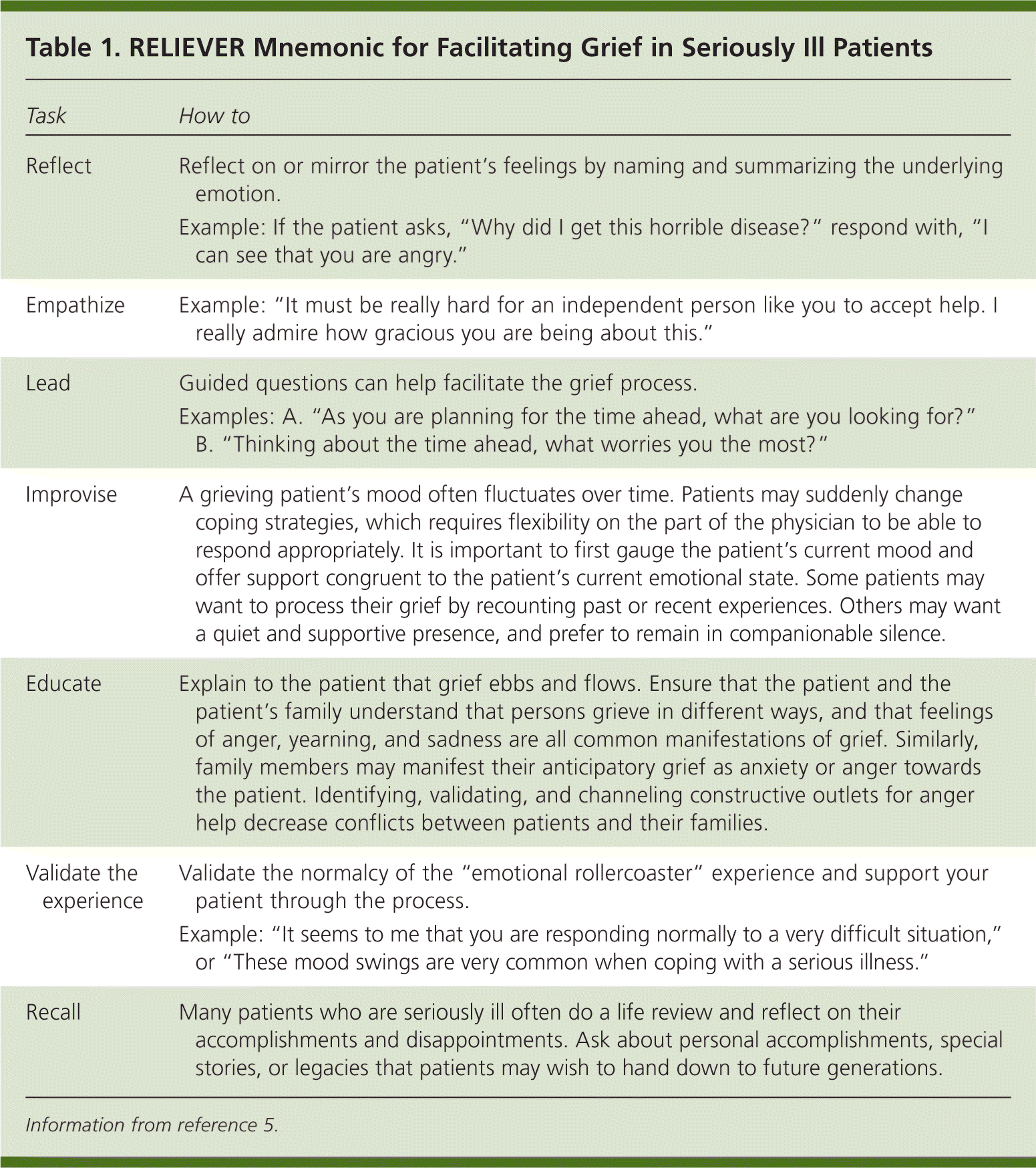
In this issue of American Family Physician, Widera and Block discuss the presentation and management of grief and depression at the end of life.8 They state that the majority of persons who are grieving cope with their distress without involving health care professionals, and that physicians can help patients who are grieving by encouraging them to make use of external sources of support. The acronym RELIEVER (reflect, empathize, lead, improvise, educate, validate the experience, recall), as described in Table 1,5 can serve as a reminder about supportive interventions that can facilitate preparatory grief. Such facilitation can be done by trained physicians, allied health professionals, and the patient's family and friends.
Table 1. RELIEVER Mnemonic for Facilitating Grief in Seriously Ill Patients
| Task | How to |
|---|---|
| Reflect | Reflect on or mirror the patient's feelings by naming and summarizing the underlying emotion. |
| Example: If the patient asks, “Why did I get this horrible disease?” respond with, “I can see that you are angry.” | |
| Empathize | Example: “It must be really hard for an independent person like you to accept help. I really admire how gracious you are being about this.” |
| Lead | Guided questions can help facilitate the grief process. |
| Examples: A. “As you are planning for the time ahead, what are you looking for?” B. “Thinking about the time ahead, what worries you the most?” | |
| Improvise | A grieving patient's mood often fluctuates over time. Patients may suddenly change coping strategies, which requires flexibility on the part of the physician to be able to respond appropriately. It is important to first gauge the patient's current mood and offer support congruent to the patient's current emotional state. Some patients may want to process their grief by recounting past or recent experiences. Others may want a quiet and supportive presence, and prefer to remain in companionable silence. |
| Educate | Explain to the patient that grief ebbs and flows. Ensure that the patient and the patient's family understand that persons grieve in different ways, and that feelings of anger, yearning, and sadness are all common manifestations of grief. Similarly, family members may manifest their anticipatory grief as anxiety or anger towards the patient. Identifying, validating, and channeling constructive outlets for anger help decrease conflicts between patients and their families. |
| Validate the experience | Validate the normalcy of the “emotional rollercoaster” experience and support your patient through the process. |
| Example: “It seems to me that you are responding normally to a very difficult situation,” or “These mood swings are very common when coping with a serious illness.” | |
| Recall | Many patients who are seriously ill often do a life review and reflect on their accomplishments and disappointments. Ask about personal accomplishments, special stories, or legacies that patients may wish to hand down to future generations. |
Information from reference 5.

