
A more recent article on the spiritual assessment is available.
Am Fam Physician. 2012;86(6):546-550
See Editor's Note.
Author disclosure: No relevant financial affiliations to disclose.
More than 80 percent of Americans perceive religion as important. Issues of belief can affect the health care encounter, and patients may wish to discuss spirituality with their physician. Many physicians report barriers to broaching the subject of spirituality, including lack of time and experience, difficulty identifying patients who want to discuss spirituality, and the belief that addressing spiritual concerns is not a physician's responsibility. Spiritual assessment tools such as the FICA, the HOPE questions, and the Open Invite provide efficient means of eliciting patients' thoughts on this topic. The spiritual assessment allows physicians to support patients by stressing empathetic listening, documenting spiritual preferences for future visits, incorporating the precepts of patients' faith traditions into treatment plans, and encouraging patients to use the resources of their spiritual traditions and communities for overall wellness. Conducting the spiritual assessment also may help strengthen the physician-patient relationship and offer physicians opportunities for personal renewal, resiliency, and growth.
Family medicine promotes comprehensive care in a holistic context. As a result, family physicians often broach a diverse array of topics during clinical encounters to assess patients' perceptions of health and their ability to cope. Some of these topics include economic issues, family systems, cultural and social determinants of wellness (e.g., community of origin, immigrant status, occupation, education), and spirituality.
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Patients should have a spiritual assessment upon admission to the hospital. | C | 9 |
| Addressing spirituality may help when forming a comprehensive treatment program for patients with chronic pain. | C | 10 |
| Spirituality should be addressed as one of the core components of quality palliative care. | C | 11 |
Definitions
The Merriam-Webster Dictionary defines spiritual as “of, relating to, consisting of, or affecting the spirit” or, alternatively, “concerned with religious values.”1 Religion is defined as “a personal set or institutionalized system of religious attitudes, beliefs, and practices.”2 Although persons who are religious may consider themselves spiritual, there are many who consider themselves spiritual but not religious. Because family physicians care for patients of all affiliations, creeds, and beliefs, this article uses the term spirituality because of its greater inclusivity.
Scope of Spiritual Beliefs
The perceived importance of spirituality by patients and physicians is borne out by secular opinion polls, medical literature, hospital regulations, and clinical practice guidelines. Gallup polls indicate that 91 percent of U.S. adults believe in God or a universal spirit, and that 81 percent consider religion important.3 Research studies demonstrate that up to 94 percent of hospitalized patients believe spiritual health is as important as physical health,4 that 40 percent of patients use faith to cope with illness,5 and that 25 percent of patients use prayer for healing each year.6 Similarly, other reports demonstrate that more than 80 percent of family physicians identify themselves as Protestant, Catholic, or Jewish; that 79 percent identify themselves as very or somewhat strong in their beliefs7; and that 78 percent feel somewhat or extremely close to God.8 The Joint Commission now requires a patient spiritual assessment upon hospital admission.9 Guidelines from the Institute for Clinical Systems Improvement state that addressing spirituality may help in creating comprehensive treatment plans for those with chronic pain,10 and guidelines from the National Consensus Project for Quality Palliative Care state that spirituality is a core component of palliative care.11
Patients and Physicians
Given its pervasiveness, spirituality commonly affects patient encounters. A study of 456 outpatients at six academic medical centers found that in the ambulatory setting, 33 percent wanted their physician to inquire about religious beliefs, and 19 percent wanted their physician to pray with them.12 If dying, 70 percent would want their physician to know their beliefs, and 50 percent would want their physician to pray with them.12 A study performed at hospitals in North Carolina and Pennsylvania demonstrated that 77 percent of family medicine inpatients felt that physicians should consider their spiritual needs, and 48 percent wanted their physician to pray with them.4 Despite this, most ambulatory and hospitalized patients report that their physician never discussed beliefs with them,4,13 even though 85 to 90 percent of physicians felt they should be aware of patient spiritual orientation.14,15
When asked to identify barriers to the spiritual assessment, physicians pointed to a lack of time (71 percent), lack of experience taking spiritual histories (59 percent), difficulty identifying patients who wanted to discuss spiritual issues (56 percent), and the belief that addressing spiritual concerns is not part of the physician's role (31 percent).16 To address these objections, there are tools and training programs available to improve physicians' efficiency in raising spiritual issues.17,18 Additionally, there is literature indicating which patients—including those who are hospitalized or terminally ill—are more likely to welcome a spiritual assessment.4,12 With respect to the relevance of spirituality, there is research purporting beneficial links between spirituality and a host of conditions, including cardiovascular disease, cancer, depression, adolescent risk behaviors, anxiety, pain, poor self-reported health, and death.19–28
Whom and When to Assess
Older patients, hospitalized patients, and patients with terminal illness often wish to share their beliefs, to hear those of their physician, and to have their physician pray for or with them.4,12,29 Physicians may consider conducting a spiritual assessment with patients who fall into these groups, or with other established or new patients. In addition, physicians may wish to assess patients who face existential crises, such as those in whom a chronic disease has been diagnosed, those with worsening illness, or those with new or persistent mental health disease. Finally, physicians may consider the casual remarks that patients sometimes make about their faith or spiritual practices as cues inviting discussion. In some cases, a spiritual conversation is most easily introduced when patients bring up concerns and crises without prompting.
Conducting the Spiritual Assessment
Before conducting a spiritual assessment, physicians should consider their personal faith tradition, beliefs and practices, positive and negative experiences, attitudes on faith and healing, and comfort and ability to participate in another's spirituality or share their own. Some physicians may not consider themselves spiritual, may not wish to discuss spirituality, or may vary in their level of ease or capability in discussing spiritual concerns. Rather than a coercive responsibility, conducting a spiritual assessment and offering spiritual support are similar to eliciting a social history and empathizing after the delivery of a negative diagnosis. They provide yet another way to understand and support patients in their experience of health and illness.
Several tools exist to help physicians conduct a spiritual history. The FICA Spiritual History Tool (Table 130 ) uses an acronym to guide health professionals through a series of questions designed to elicit patient spirituality and its potential effect on health care. Starting with queries about faith and belief, it proceeds to ask about their importance to the patient, the patient's community of faith, and how the patient wishes the physician to address spirituality in his or her care.

| Category | Sample questions |
|---|---|
| Faith and belief | Do you have spiritual beliefs that help you cope with stress?
|
| Importance | Have your beliefs influenced how you take care of yourself in this illness? |
| Community | Are you part of a spiritual or religious community? |
| Is this of support to you, and how? | |
| Address in care | How would you like me to address these issues in your health care? |
The HOPE questions are another tool (Table 2).31 These questions lead the physician from general concepts to specific applications by asking about patients' sources of hope and meaning, whether they belong to an organized religion, their personal spirituality and practices, and what effect their spirituality may have on medical care and end-of-life decisions.

| Category | Sample questions |
|---|---|
| H: sources of hope | What are your sources of hope, strength, comfort, and peace? |
| What do you hold on to during difficult times? | |
| O: organized religion | Are you part of a religious or spiritual community? |
| Does it help you? How? | |
| P: personal spirituality and practices | Do you have personal spiritual beliefs? |
| What aspects of your spirituality or spiritual practices do you find most helpful? | |
| E: effects on medical care and end-of-life issues | Does your current situation affect your ability to do the things that usually help you spiritually? |
| As a doctor, is there anything that I can do to help you access the resources that usually help you? | |
| Are there any specific practices or restrictions I should know about in providing your medical care? | |
| If the patient is dying: How do your beliefs affect the kind of medical care you would like me to provide over the next few days/weeks/months? |
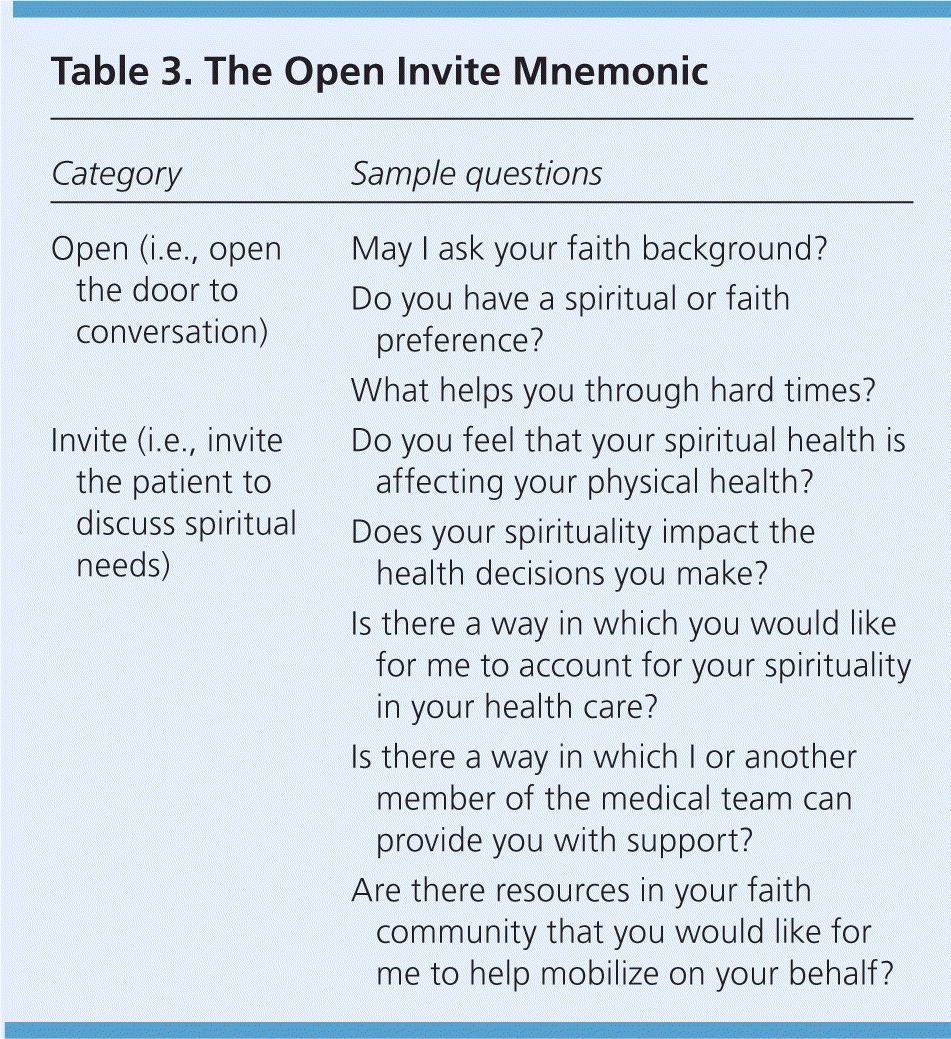
A third tool, the Open Invite, is a patient-focused approach to encouraging a spiritual dialogue. It is structured to allow patients who are spiritual to speak further, and to allow those who are not to easily opt out. First, it reminds physicians that their role is to open the door to conversation and invite (never require) patients to discuss their needs. Preaching or prescribing spiritual practices generally is beyond the proper bounds of the physician-patient relationship. Second, Open Invite provides a mnemonic for the general types of questions a physician may use (Table 3). The tool provides questions that allow the physician to broach the topic of spirituality. Questions may be similar to those used in the FICA and HOPE mnemonics, or may be customized. Examples include, “May I ask your faith background?” or “Do you have a spiritual or faith preference?” The “invite” questions are used to encourage patients to discuss their needs as their comfort allows. Sample questions include, “Does your spirituality impact the health decisions you make?” or “Is there a way in which you would like for me to account for your spirituality in your health care?” The key to this approach is to use questions that are natural and conversational while being respectful and nonthreatening.
| Category | Sample questions |
|---|---|
| Open (i.e., open the door to conversation) | May I ask your faith background? |
| Do you have a spiritual or faith preference? | |
| What helps you through hard times? | |
| Invite (i.e., invite the patient to discuss spiritual needs) | Do you feel that your spiritual health is affecting your physical health? |
| Does your spirituality impact the health decisions you make? | |
| Is there a way in which you would like for me to account for your spirituality in your health care? | |
| Is there a way in which I or another member of the medical team can provide you with support? | |
| Are there resources in your faith community that you would like for me to help mobilize on your behalf? |
Incorporation of Spiritual Needs into Patient Care
After spiritual needs have been identified, the physician may incorporate the results of the assessment into patient care. The most basic thing a physician can do is to listen compassionately. Regardless of whether patients are devout in their spiritual traditions, their beliefs are important to them. By listening, physicians signal their care for their patients and recognition of this dimension of their lives. Empathetic listening may be all the support a patient requires.
Another way to incorporate the spiritual assessment is to document the patient's spiritual perspective, background, stated impact on medical care, and openness to discussing the topic. Physicians may find this information helpful when readdressing the subject in the future or during times of crisis when sources of comfort and meaning become crucial. This documentation also helps meet hospital regulatory requirements for conducting a spiritual assessment.9
An additional way to incorporate the assessment is to consider how different traditions and practices may affect standard medical practice. For instance, patients of the Jehovah's Witness tradition tend to refuse blood transfusion; believers in faith healing may delay traditional medical care in hopes of a miracle; and Muslim and Hindu women tend to decline sensitive (and sometimes general) examinations by male physicians. Patients with certain beliefs may experience substantial psychological duress if they believe a condition is caused by a lack of belief or transgressions on their part.
Physicians also need to consider how practices may influence acute or chronic health states. For example, many Muslims fast during Ramadan, which may affect glucose control and other physiologic factors in the ambulatory and inpatient settings. Persons of some faiths observe strict dietary codes, such as halal and kosher laws, which may require physicians to alter traditional nutrition counseling. It is important to remember, however, that patients may not adhere to each specific belief or practice of their faith. Physicians should avoid making assumptions when asking patients how their particular practices may affect their medical care.
The spiritual assessment also allows patients to identify spiritual beliefs, practices, and resources that may positively impact their health. Helpful questions include, “Do you have spiritual practices, such as praying, meditating, listening to music, or reading sacred text, that you find helpful or comforting?” and “Are you part of a faith community? If so, does it have resources such as a home visitation program, a food pantry, or health screening?” Physicians can reinforce positive coping behaviors and, with the patient's permission, offer to contact the patient's spiritual community to mobilize community faith resources as appropriate.
Finally, there may be some instances in which physician and patient faith traditions coincide. In these cases, if the patient requests, the physician may consider offering faith-specific support. This may include patient-or physician-led prayer. Given the variety of spiritual practices followed in multicultural societies, it is best not to assume that a physician's spirituality mirrors that of his or her patients. Prayer should not be a goal of a spiritual assessment, and physicians should not attempt to get patients to agree with them on specific faith issues.
Potential Benefits in the Physician-Patient Relationship
Assessing and integrating patient spirituality into the health care encounter can build trust and rapport, broadening the physician-patient relationship and increasing its effectiveness. Practical outcomes may include improved adherence to physician-recommended lifestyle changes or compliance with therapeutic recommendations. Additionally, the assessment may help patients recognize spiritual or emotional challenges that are affecting their physical and mental health. Addressing spiritual issues may let them tap into an effective source of healing or coping.
For physicians, incorporating patient spirituality brings the potential for renewal, resiliency, and growth, even in difficult encounters. Sometimes physicians have few medical solutions for problems that cause suffering, such as incurable disease, chronic pain, grief, domestic violence, and broken relationships. In these situations, providing comfort to patients can increase professional satisfaction and prevent burnout.32
Data Sources: A PubMed search was completed using the following keywords and medical subject headings (MeSH): spirituality, faith, and religion. The search included randomized controlled trials, clinical trials, meta-analyses, systematic reviews, and review articles. Also searched were the National Guideline Clearinghouse, the Institute for Clinical Systems Improvement, the Cochrane Database of Systematic Reviews, and the National Center for Complementary and Alternative Medicine Web site. Search dates: November 2010 through August 2011.
editor's note: This article reviews the suggested uses and potential benefits of spiritual assessment in clinical practice. We anticipate that readers along the broad spectrum of religious belief may have varying views on this topic. Some readers may think that spirituality is not an ethically appropriate area for family physicians to address, especially when the faith traditions of physicians and patients differ. In addition, associations between religious beliefs and health outcomes are inconsistent.1 Others might feel that a generic spiritual (rather than religious) assessment trivializes religious beliefs, and minimizes potential benefits of explicitly incorporating faith into patient encounters to promote holistic healing.2 We welcome your comments about this article and look forward to the discussion. Add your comments below or tell us what you think at afpedit@aafp.org.—KENNETH W. LIN, MD,Associate Deputy Editor for AFP Onlineand JAY SIWEK, MD, Editor.
REFERENCES
1. Weaver AJ, Koenig HG. Religion, spirituality, and their relevance to medicine: an update. Am Fam Physician. 2006;73(8):1336-1337.
2. Larimore WL. Providing basic spiritual care for patients: should it be the exclusive domain of pastoral professionals? Am Fam Physician. 2001;63(1):36-41.
