Am Fam Physician. 2012;86(9):826-833
Author disclosure: No relevant financial affiliations to disclose.
Family physicians should be able to recognize findings on physical examination and history that suggest the presence of a genetic syndrome to aid in the diagnosis and treatment of potentially affected patients, as well as subspecialty referral. General themes that can alert family physicians to the presence of genetic conditions include dysmorphic features that are evident on physical examination; multiple anomalies in one patient; unexplained neurocognitive impairment; and a family history that is suggestive of a hereditary disease. The presence of one obvious malformation should not limit the full evaluation, because additional, subtler findings will often be important in the differential diagnosis. Taking an accurate three-generation family history is invaluable when considering a genetic syndrome. Important elements include the age and sex of family members; when family members were affected by disease or when they died; the ethnic background; and if there is consanguinity. Genetic subspecialists can assist family physicians in diagnosis, suggest additional testing and referrals if warranted, help direct medical care, and provide counseling for affected patients and their families.
Although many genetic conditions are individually rare, they are common in aggregate and place a great burden on affected patients and the medical system.1–3 Congenital malformations (many of which are related to genetic disturbances) occur in approximately 5 percent of live-born infants; a much higher proportion of conceptions are affected by genetic anomalies.4,5 In one study, an estimated 79 of 1,000 live-born infants were found to have a genetic syndrome and/or congenital malformation by 25 years of age.6
| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
| A full dysmorphology examination is best conducted by a trained clinical geneticist; a primary care physician should conduct a thorough physical examination. | C | 9–12 | — |
| In the assessment of developmental delay and/or neurocognitive impairment, neuroimaging is warranted when a structural, degenerative, or metabolic process is suspected. | C | 19, 20 | Discussion with a radiologist or neurologist may assist with the choice of imaging modality. |
| A three-generation family history should be obtained when a genetic syndrome is suspected or identified. Genetic counselors can be invaluable in this regard. | C | 26, 28 | A combination of open-ended and specific questions is useful to ascertain the presence of relatively common conditions (such as those that involve cancer or neurocognitive disturbances); it also allows for identification of medical issues that “run in the family.” |
Prompt recognition of features suggestive of genetic conditions can improve the selection of appropriate, cost-effective diagnostic tests; the performance of well-informed genetic counseling related to issues such as prognosis and future family planning; and timely referral to subspecialists.7,8 Therefore, it is important for family physicians to be able to recognize general themes that can suggest the presence of a genetic syndrome and identify patients who would benefit from referral to clinical geneticists.
General themes that can alert family physicians to the presence of genetic conditions include dysmorphic features; multiple anomalies in one patient that may be related to a unifying cause; unexplained neurocognitive impairment; and a family history that is suggestive of a hereditary disease.
Dysmorphic Features
Dysmorphic features may result from a perturbation of human development.9 This perturbation can be a direct effect of a genetic mutation or can indirectly involve a genetic disturbance, such as in the case of gestational exposure to a teratogen. Figures 1A through 1I are examples of dysmorphic features that can be found on physical examination that may be helpful in the diagnosis of genetic syndromes.
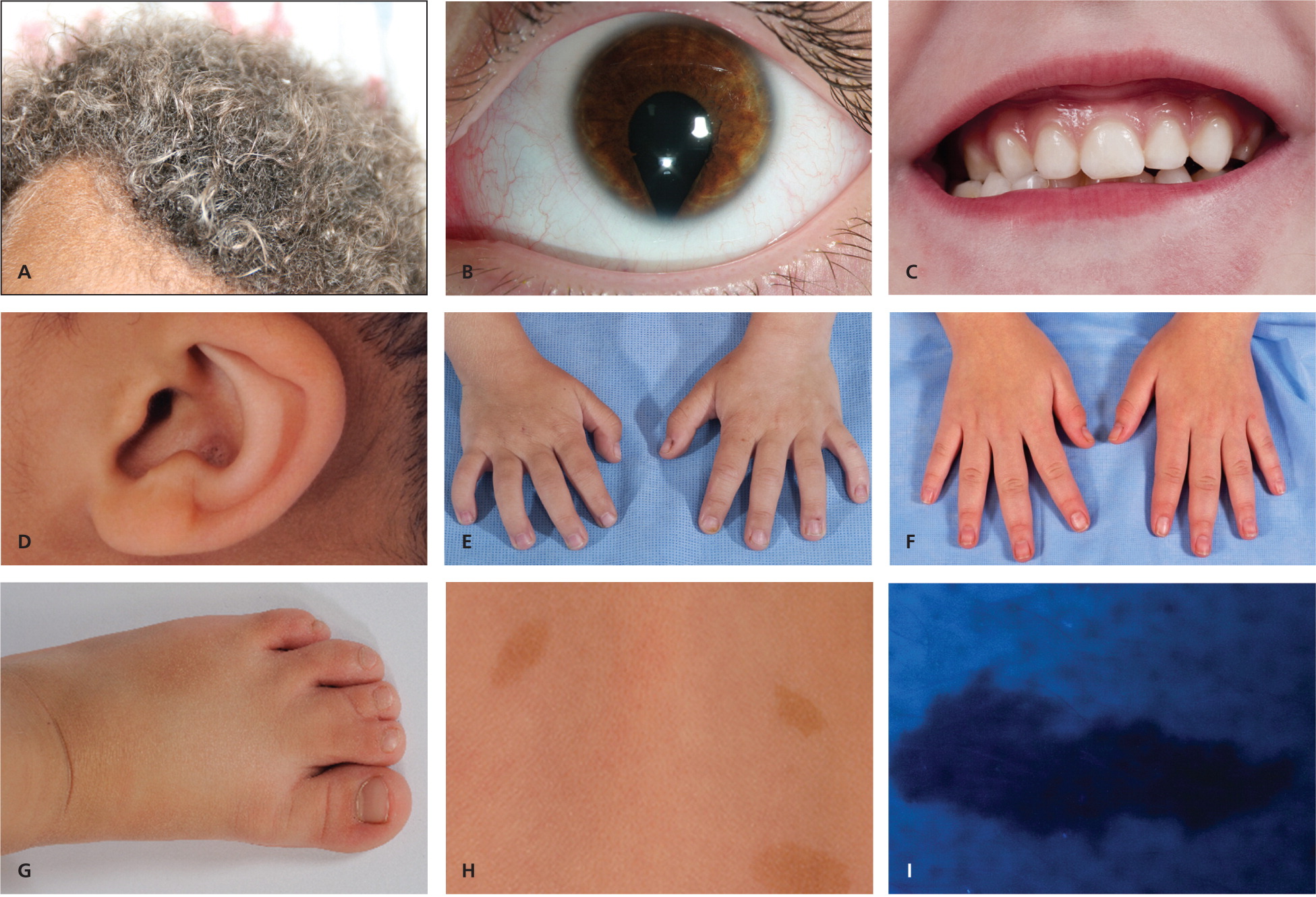
A full dysmorphology examination is best conducted by a trained clinical geneticist; a primary care physician should conduct a thorough physical examination.9–12 An essential component of the physical examination for genetic syndromes is comparison with established normative values. In addition to weight, height, and head circumference, examples of other important measurements include interpupillary distance (the distance between the center of the pupils) if a midline defect is suspected (as in the case of holoprosencephaly, the most common malformation of the human forebrain), or the size of the limbs in the case of a skeletal dysplasia.7,13 These values must be interpreted in the context of the patient's longitudinal growth, as well as the family background.
The absence or presence of certain features in family members can be a clue that a feature is either pathologic or merely a familial or ethnic variant. For example, inner epicanthal folds (small folds of skin over the medial eyes) can occur in persons with Down syndrome, and are also described in more than 50 other syndromes, including Noonan syndrome, Rubinstein-Taybi syndrome, and Smith-Lemli-Opitz syndrome. However, epicanthal folds are also a normal finding in many persons of Asian or Native American descent.7,14 Recently, an effort has been made to codify physical descriptors, which can help with communication and establishment of the differential diagnosis.10
The presence of one obvious malformation should not limit the full evaluation, because additional, subtler findings will often be important in the differential diagnosis. For example, a newborn might be immediately noted to have a cleft palate, which has a broad differential diagnosis. A patient with a cleft palate; hypocalcemia; a ventricular septal defect; and subtle physical features, such as a broad nasal root, overfolded helices of the ears, and long, narrow fingers and toes, likely has 22q11.2 deletion syndrome (formerly called DiGeorge syndrome), which has a prevalence of approximately one in 4,000 live births.15
Cluster of Findings
Many genetic conditions are suggested through a combination of clinical features, including the physical appearance of the patient, laboratory abnormalities, and aspects of family history.14 For example, an adolescent presenting for a sports physical examination who is noted to have arachnodactyly (long, thin fingers) and pectus excavatum, and whose father died of an aortic dissection would be suspected of having Marfan syndrome.16 Short stature and thumb anomalies in a child who also has aplastic anemia may suggest Fanconi anemia, and confirmation would be important to institute surveillance for long-term complications.17
There are several possible explanations for the presence of a cluster of findings in a patient with a genetic syndrome. One common reason is pleiotropy, in which a mutation in a single gene results in multiple effects on separate organ systems. For example, in Holt-Oram syndrome, sometimes called heart-hand syndrome, mutations in the gene TBX5 cause congenital heart and limb malformations.18 Another possible explanation for the presence of a cluster of findings is that the patient has a contiguous gene syndrome, in which he or she has deletions (missing genetic material) or duplications (extra genetic material) involving a certain portion of a chromosome. Because all genes in the deleted or duplicated intervals are affected, the involvement of many genes can result in a complicated clinical picture. The 22q11.2 deletion syndrome is a well-known example of a contiguous gene syndrome.15
Table 1 lists resources that can be helpful in establishing a differential diagnosis based on the presence of several distinct features.
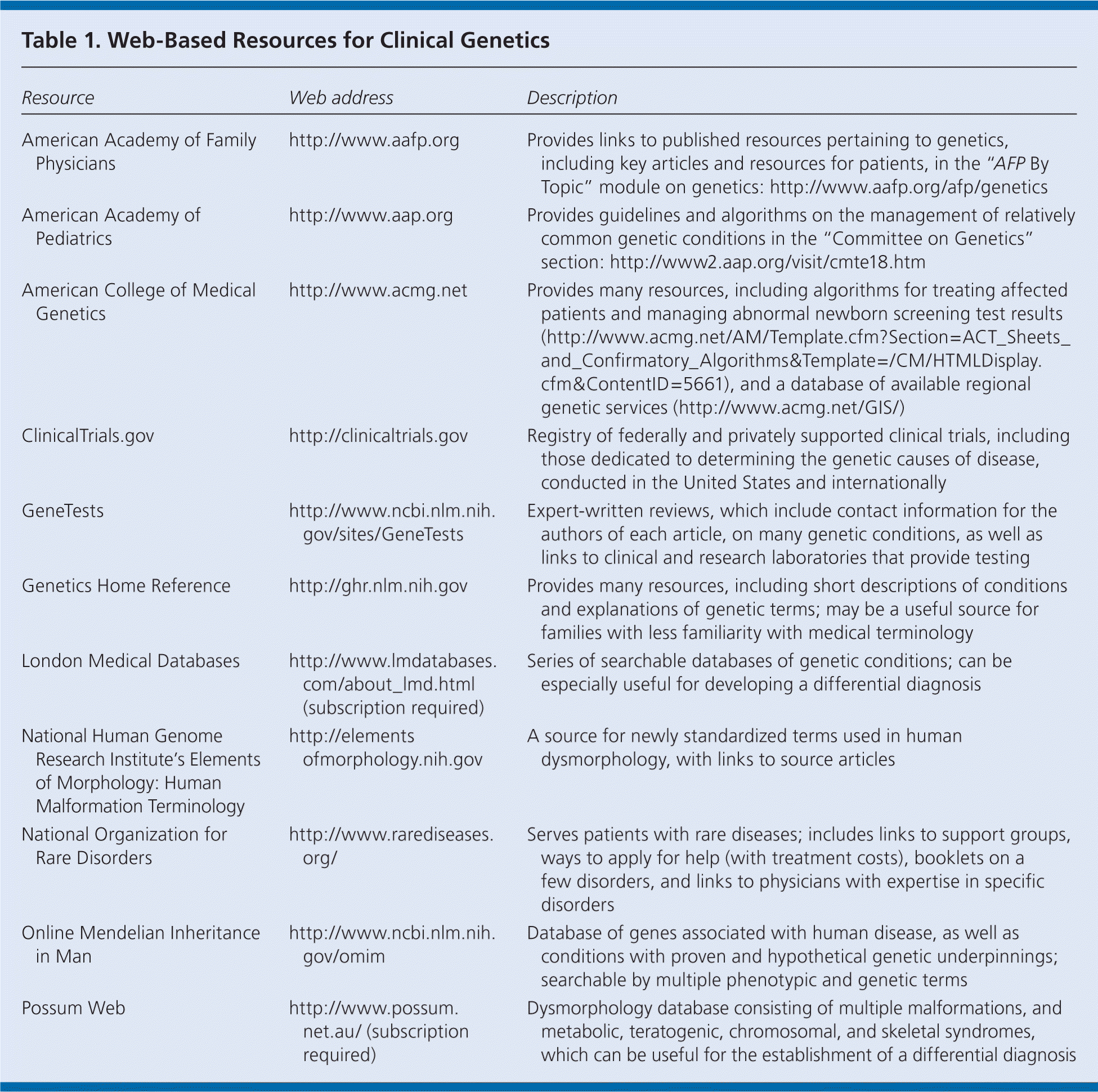
| Resource | Web address | Description |
|---|---|---|
| American Academy of Family Physicians | https://www.aafp.org | Provides links to published resources pertaining to genetics, including key articles and resources for patients, in the “AFP By Topic” module on genetics: https://www.aafp.org/afp/genetics |
| American Academy of Pediatrics | http://www.aap.org | Provides guidelines and algorithms on the management of relatively common genetic conditions in the “Committee on Genetics” section: http://www2.aap.org/visit/cmte18.htm |
| American College of Medical Genetics | http://www.acmg.net | Provides many resources, including algorithms for treating affected patients and managing abnormal newborn screening test results (http://www.acmg.net/AM/Template.cfm?Section=ACT_Sheets_and_Confirmatory_Algorithms&Template=/CM/HTMLDisplay.cfm&ContentID=5661), and a database of available regional genetic services (http://www.acmg.net/GIS/) |
| ClinicalTrials.gov | http://clinicaltrials.gov | Registry of federally and privately supported clinical trials, including those dedicated to determining the genetic causes of disease, conducted in the United States and internationally |
| GeneTests | http://www.ncbi.nlm.nih.gov/sites/GeneTests | Expert-written reviews, which include contact information for the authors of each article, on many genetic conditions, as well as links to clinical and research laboratories that provide testing |
| Genetics Home Reference | http://ghr.nlm.nih.gov | Provides many resources, including short descriptions of conditions and explanations of genetic terms; may be a useful source for families with less familiarity with medical terminology |
| London Medical Databases | http://www.lmdatabases.com/about_lmd.html (subscription required) | Series of searchable databases of genetic conditions; can be especially useful for developing a differential diagnosis |
| National Human Genome Research Institute's Elements of Morphology: Human Malformation Terminology | http://elementsofmorphology.nih.gov | A source for newly standardized terms used in human dysmorphology, with links to source articles |
| National Organization for Rare Disorders | http://www.rarediseases.org/ | Serves patients with rare diseases; includes links to support groups, ways to apply for help (with treatment costs), booklets on a few disorders, and links to physicians with expertise in specific disorders |
| Online Mendelian Inheritance in Man | http://www.ncbi.nlm.nih.gov/omim | Database of genes associated with human disease, as well as conditions with proven and hypothetical genetic underpinnings; searchable by multiple phenotypic and genetic terms |
| Possum Web | http://www.possum.net.au/ (subscription required) | Dysmorphology database consisting of multiple malformations, and metabolic, teratogenic, chromosomal, and skeletal syndromes, which can be useful for the establishment of a differential diagnosis |
Neurocognitive Impairment
In many genetic conditions, neurocognitive impairment may be the first and most obvious sign of disease.19 Genetic conditions can produce neurocognitive impairment in a number of different ways, including via structural brain malformations, aberrant signaling involving genes that play important neurologic roles, and inborn errors of metabolism, the latter of which can cause neurologic disease because of an inadequate amount of a needed substrate or accumulation of a toxic metabolite. Phenylketonuria, galactosemia, methylmalonic acidemia, and maple syrup urine disease are examples of conditions caused by inborn errors of metabolism that are included in newborn screening.20,21 In the assessment of developmental delay and/or neurocognitive impairment, neuroimaging is warranted when a structural, degenerative, or metabolic process is suspected.19,20
Neurocognitive impairment related to genetic conditions may be recognized in childhood; however, some conditions, such as Huntington disease or some types of Charcot-Marie-Tooth disease, as well as familial forms of complex disorders, such as Parkinson disease and Alzheimer disease, may manifest much later in life.22–25 Key historical items should include the degree and type of dysfunction; the timing, both in terms of when the dysfunction was first noticed as well as how the impairment has changed with time (including whether or not there has been regression, or loss of developmental milestones); and if there are any recognized triggers.
Inborn errors of metabolism, such as phenylketonuria, deserve special attention, largely because medical interventions in these disorders can be especially important for preventing neurocognitive impairment.20,21 For example, it may be necessary to remove a type of food source that cannot be properly metabolized (phenylalanine in the case of phenylketonuria). These interventions may influence the degree of cognitive impairment, and can be a matter of life or death.
Suspicious Family History
Taking an accurate three-generation family history (Figure 226,27 ) is important when a genetic syndrome is suspected or identified. Genetic counselors can be invaluable in this regard.26,28 It is critical to consider all health-related issues, even if they do not appear to be directly connected to the primary condition. For example, genetic syndromes may be suggested by a preponderance of early cancer diagnoses (e.g., colon cancer and other cancer types in familial adenomatous polyposis; breast and ovarian cancer and other cancer types in BRCA1- or BRCA2-related cancer), early or unusual onset of a relatively common condition such as cardiac disease (e.g., familial hyperlipidemia, inherited arrhythmia), or a history of unusual reactions to a certain medication (e.g., severe or life-threating reactions to anesthetic agents, such as what may occur in patients with succinylcholine esterase deficiency).26,29,30
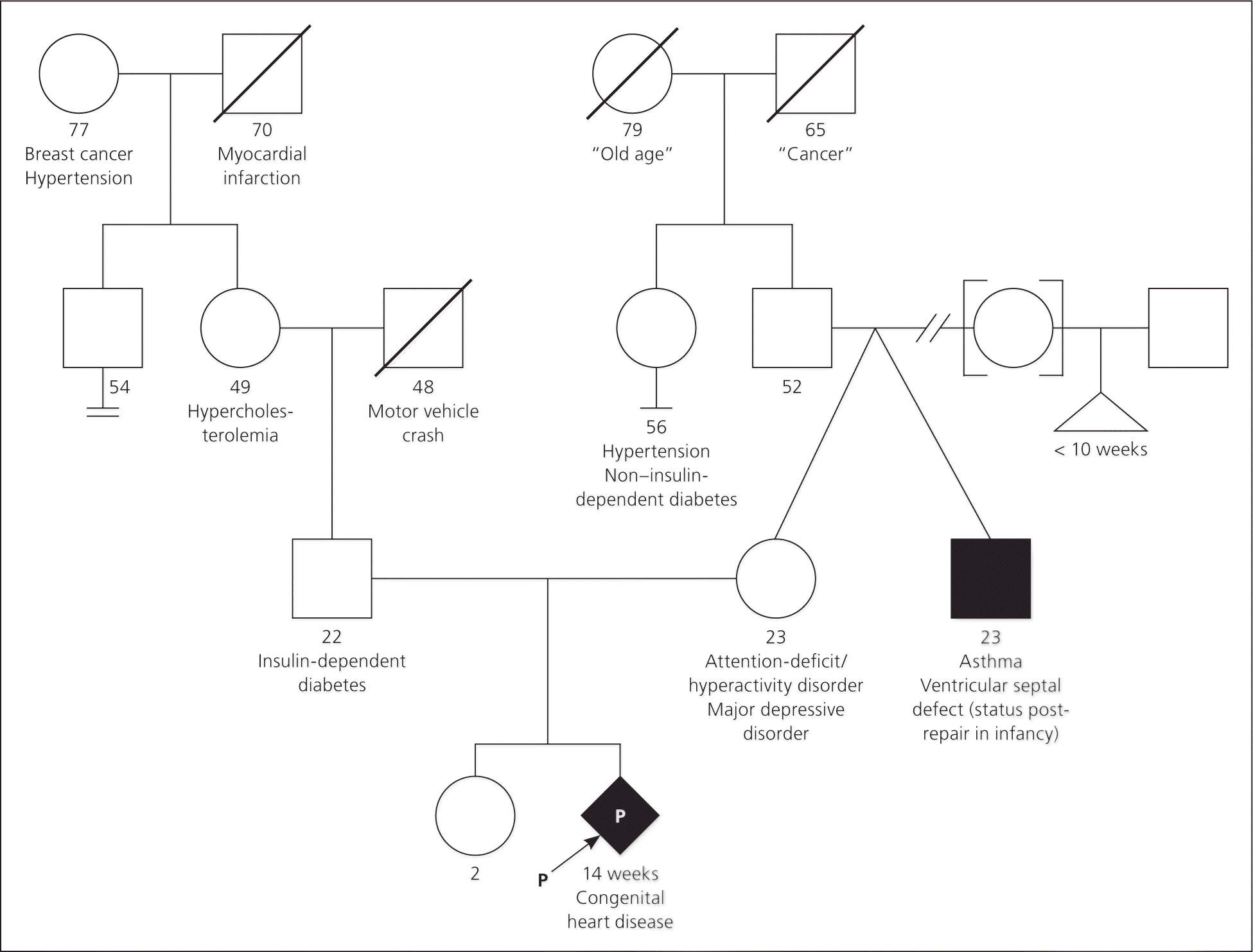
Important elements include the age and sex of family members; when family members were affected by disease or when they died; the ethnic background; and if there is any consanguinity, which may give evidence for the presence of a recessive condition. Many genetic diseases will present differently in terms of timing, clinical features, and even the chance of being affected at all, depending on the age and sex of the person. Knowing these facts may also help determine the likely inheritance pattern, and can be helpful in calculating the recurrence risk. Some conditions are more common in certain ethnicities, such as Tay-Sachs disease in persons of Ashkenazi Jewish descent and sickle cell disease in persons of African descent.26,31 Taking a thorough family history may require patients to contact relatives to help provide key details. Additionally, when physicians are attempting to diagnose a patient with dysmorphic features, they may be aided by the now almost ubiquitous presence of advanced handheld devices that can store photographs of family members.
Genetic Testing and Referral
Some genetic conditions are diagnosed on clinical grounds. Geneticists can assist in diagnosis, suggest additional testing and referrals if warranted, help direct medical care, and provide counseling for affected patients and their families. Physicians can locate a regional geneticist through the American College of Medical Genetics Web site at http://www.acmg.net/GIS/.
For other patients, the diagnosis is made through genetic testing. There is a wide array of tests that may be used.8 The choice of test depends on the nature of the condition, the expense and availability of the test, and the specific clinical scenario (for example, the testing strategy may be different if a condition were suspected in an adult versus a fetus). Ultimately, whether or not a patient or family elects to undergo testing is a matter of personal choice, and patients should be counseled regarding what a test may or may not reveal.
Table 2 lists selected genetic tests. In addition to these specialized tests, however, physicians should be aware that many genetic conditions are suspected or confirmed by commonly ordered tests, such as plain radiography, complete blood count, or a basic metabolic panel. For example, wormian bones might be visible in a radiographic image of the skull in a patient with osteogenesis imperfecta, and thrombocytopenia would be evident in a patient with Wiskott-Aldrich syndrome.32,33 Family physicians can work in conjunction with genetic subspecialists when performing appropriate diagnostic and confirmatory testing.
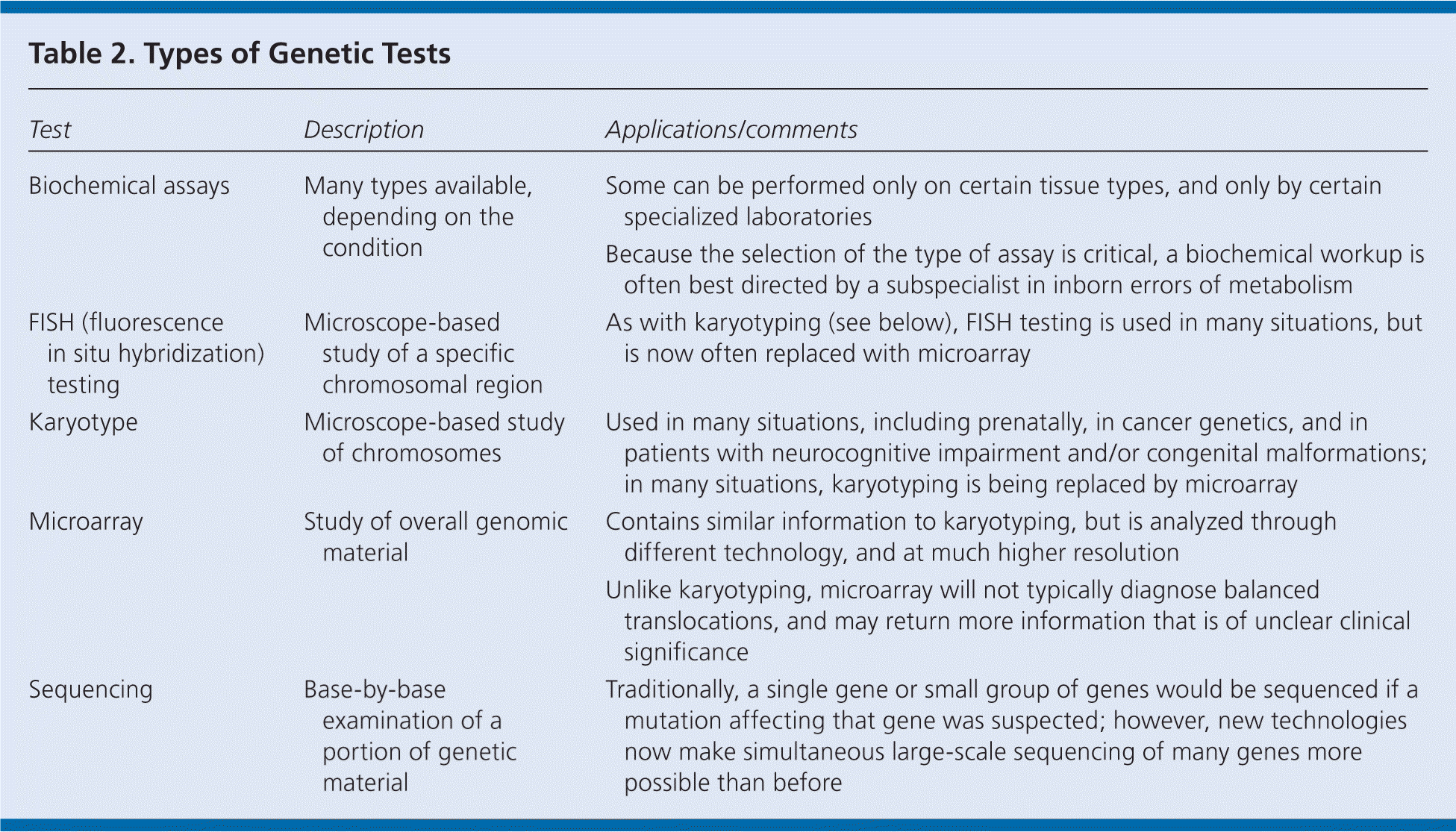
| Test | Description | Applications/comments |
|---|---|---|
| Biochemical assays | Many types available, depending on the condition | Some can be performed only on certain tissue types, and only by certain specialized laboratories |
| Because the selection of the type of assay is critical, a biochemical workup is often best directed by a subspecialist in inborn errors of metabolism | ||
| FISH (fluorescence in situ hybridization) testing | Microscope-based study of a specific chromosomal region | As with karyotyping (see below), FISH testing is used in many situations, but is now often replaced with microarray |
| Karyotype | Microscope-based study of chromosomes | Used in many situations, including prenatally, in cancer genetics, and in patients with neurocognitive impairment and/or congenital malformations; in many situations, karyotyping is being replaced by microarray |
| Microarray | Study of overall genomic material | Contains similar information to karyotyping, but is analyzed through different technology, and at much higher resolution |
| Unlike karyotyping, microarray will not typically diagnose balanced translocations, and may return more information that is of unclear clinical significance | ||
| Sequencing | Base-by-base examination of a portion of genetic material | Traditionally, a single gene or small group of genes would be sequenced if a mutation affecting that gene was suspected; however, new technologies now make simultaneous large-scale sequencing of many genes more possible than before |
Certain resources may be helpful in determining the type of genetic testing that is recommended and available (Table 1). For example, the GeneTests Web site (http://www.ncbi.nlm.nih.gov/sites/GeneTests) can be used to find a laboratory that conducts testing for a certain genetic condition, and the National Institutes of Health–based ClinicalTrials.gov Web site (http://clinicaltrials.gov) can help locate relevant research studies, which can also be a useful way to find physicians with expertise in a rare disorder.
Data Sources: A PubMed search was completed in Clinical Queries combining the key terms genetics, primary care, and referral. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. Also searched were the Agency for Healthcare Research and Quality, the Cochrane database, the Institute for Clinical Systems Improvement, and the National Guideline Clearinghouse database. Search date: August 16, 2011.