
Am Fam Physician. 2012;86(11):1024
Author disclosure: No relevant financial affiliations to disclose.
Youth with special health care needs who receive care within a patient-centered medical home (PCMH) are significantly more likely to receive services for transitioning to adult care. Broader implementation of the PCMH may contribute to wider use of health care transition counseling and enhanced support for such patients as they prepare to enter adulthood.
With advancements in the treatment of chronic conditions in children over the past 20 years, more than 90 percent of youth with special health care needs will survive into adulthood.1 As such, millions of patients will transition from more family-centered childhood models of care to adult models of care in order to receive more developmentally appropriate care, to facilitate access to adult specialty health care professionals, and to maintain the long-term benefits of primary and preventive care. The need to orchestrate this transition is a Healthy People 2020 objective.2 Best practices for health care transition have been formulated in the context of the PCMH, which aims to provide family-centered, continuous, and comprehensive care.3,4
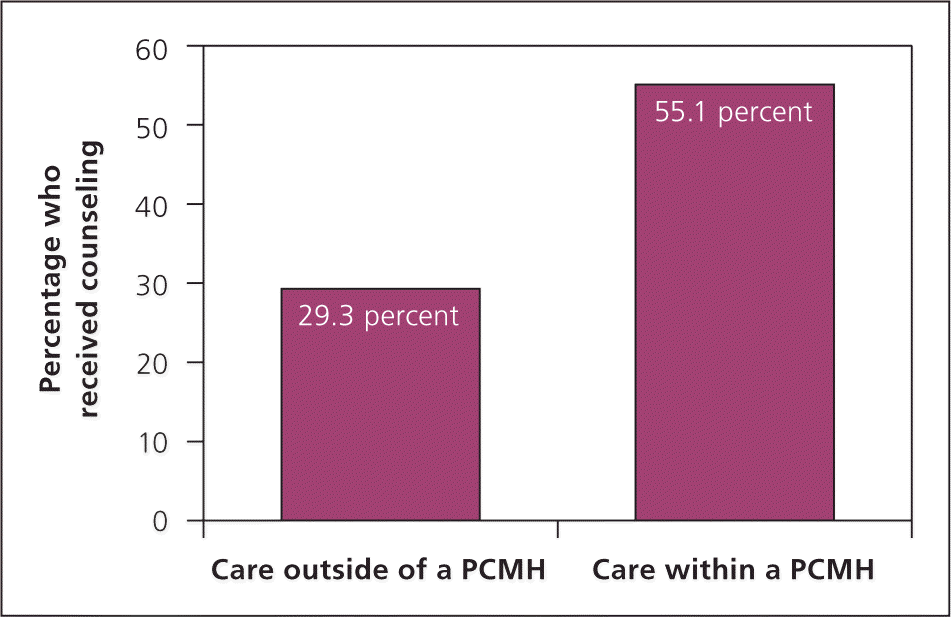
According to the 2009 to 2010 National Survey for Children with Special Health Care Needs, only 40 percent of youth with special health care needs participate in health care transition counseling.5 Those who obtain care within a PCMH, however, are almost three times more likely to receive transition services than those who receive care outside of a PCMH (odds ratio = 2.96; 95% confidence interval, 2.94 to 2.97; see accompanying figure).5
The association between the PCMH and transition counseling merits further investigation, but may be explained by the inherent ability of the PCMH to facilitate coordinated care and discussions about health care transition. To ensure that all youth with special health care needs successfully transition to adult care, widespread adoption of the PCMH will likely be critical. Training programs that focus on PCMH transformation and legislation for reimbursement of care coordination are key to increasing the number of these youth who receive this valuable care planning.
