
Am Fam Physician. 2013;88(10):669-675
Author disclosure: No relevant financial affiliations.
Child abuse is the third leading cause of death in children between one and four years of age, and almost 20% of child homicide victims have contact with a health care professional within a month of their death. Therefore, family physicians are in an ideal position to detect and intervene in cases of suspected child maltreatment. There is currently insufficient evidence that screening parents or guardians for child abuse reduces disability or premature death. Assessment for physical abuse involves evaluation of historical information and physical examination findings, as well as radiographic and laboratory studies, if indicated. The history should be obtained in a nonaccusatory manner and should include details of any injuries or incidents, the patient's medical and social history, and information from witnesses. The physical examination should focus on bruising patterns, injuries or findings concerning for abuse, and palpation for tenderness or other evidence of occult injury. Skeletal survey imaging is indicated for suspected abuse in children younger than two years. Imaging may be indicated for children two to five years of age if abuse is strongly suspected. Detailed documentation is crucial, and includes photographing physical examination findings. Physicians are mandated by law to report child abuse to the local child protective services or law enforcement agency. After a report is made, the child protection process is initiated, which involves a multidisciplinary team approach.
Child abuse is a significant problem that often goes unrecognized until severe injury or death has occurred.1 In 2008, the number of child abuse fatalities was six times that of influenza A (H1N1) fatalities in children.2 In 2009, child abuse was the third leading cause of death in children between one and four years of age.3 As many as 50% of abused children are abused multiple times.4 According to one study, almost 20% of child homicide victims had contact with a health care professional within one month of their death.1
Although the devastating and sometimes deadly consequences of child abuse are undeniable, studies providing data on optimal means of prevention, intervention, and management are lacking. A systematic review for the U.S. Preventive Services Task Force found insufficient evidence that screening and behavioral interventions for parents or guardians for physical abuse or neglect of children reduced disability or premature death.5
Child protective services agencies received approximately 3.4 million referrals involving the alleged maltreatment of approximately 6.2 million children during the 2011 federal fiscal year.6 Teachers, law enforcement, legal personnel, and social services were the most common sources of reports that year, whereas medical personnel accounted for 8.4% of referrals.6 Child abuse is a diagnosis physicians cannot afford to miss. Family physicians can play a key role in protecting children by considering abuse as part of the differential and reporting it if suspected.
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Bruising on the torso, ear, or neck in a child four years or younger, or bruising in any region in a child younger than four months, requires further evaluation for abuse. | C | 15 |
| Skeletal survey imaging is recommended for all cases of suspected abuse in children younger than two years. | C | 18 |
| Metaphyseal lesions, posteromedial rib fractures, scapular or spinous process fractures, and sternal fractures identified on radiography have relatively high specificity for physical abuse. | C | 20, 21 |
| Hepatic transaminase levels have modest predictive value for occult abdominal injury in children in whom abdominal computed tomography is not already planned. | C | 23 |
Definition
The Child Abuse Prevention and Treatment Act, as amended by the Keeping Children and Families Safe Act of 2003, defines abuse as “any recent act or failure to act on the part of a parent or caretaker which results in death, serious physical or emotional harm, sexual abuse or exploitation” or “an act or failure to act which presents an imminent risk of serious harm.”7 Each state has its own definition of child abuse based on this standard, although there is significant variation in intolerance of corporal punishment and in what constitutes abuse.8 Most states recognize four major types of maltreatment: neglect, physical abuse, psychological maltreatment, and sexual abuse. Because of the broad nature of this topic, this article focuses on physical abuse.
Recognition, Screening, and Prevention
The American Academy of Family Physicians acknowledges that the diagnosis and treatment of child abuse are complex, and require a multidisciplinary approach to caring for the child involved, as well as the child's family.9 There is insufficient evidence that any specific screening strategy or behavioral intervention produces better health outcomes than clinician awareness and evaluation of potential signs of abuse.5 Table 1 summarizes key steps that physicians can take to counsel families and prevent abuse.10

| Step | Comment |
|---|---|
| Obtain and periodically update a child's social history. | Screen for risk factors or problems, and reinforce or correct parenting skills; see the parent assessment form at http://brightfutures.aap.org/pdfs/Other%203/PSQ_screen.pdf and other resources at http://brightfutures.aap.org. |
| Acknowledge difficulties and frustrations with parenting. | Provide anticipatory guidance for situations or developmental stages that may be triggers for child maltreatment. |
| Talk with parents about their infant's crying and how they cope with it. | Discuss normal infant behavior and methods to respond to crying. |
| Recognize the increased risk of abuse in children with disabilities. | Discuss options for respite care; talk with parents about who else has contact with their child. |
| Assess parents for intimate partner violence and postpartum depression. | Refer parents to appropriate community services if intimate partner violence is identified, and provide or refer for appropriate care for depression. |
| Guide parents in providing effective discipline. | See American Academy of Pediatrics' guidance at http://pediatrics.aappublications.org/content/101/4/723.full. |
History
In addition to asking parents, caregivers, or other witnesses for a detailed description of the circumstances surrounding a suspicious injury, assessing the child's general medical, social, and developmental history is critical.8 A complete, well-documented history that occurs early in the course of evaluation can serve crucial legal and medical roles. The history should be obtained in a thorough but nonaccusatory manner.8 Features of the history that should be elicited, as well as features that are concerning for intentional trauma, are listed in Table 2.8,11 Physicians must evaluate the consistency of a caregiver's history with other findings from the history or physical examination.

| Comprehensive history components |
| Medical history, including prior injuries, trauma, hospitalizations, medical illnesses, or congenital conditions |
| Family history, particularly of bleeding disorders, bone disorders, or metabolic/genetic conditions |
| Pregnancy history, including whether the pregnancy was planned or unplanned |
| Description of familial disciplinary patterns or practices |
| Description of the child's temperament, especially whether he or she is typically active, fussy, easygoing, etc. |
| History of abuse toward the child, siblings, or parents |
| Developmental history, including milestones, language, gross motor skills, and fine motor skills |
| History of substance abuse by parents, caregivers, or others in the home |
| Recent social or financial stressors |
| History of violent interactions among other family members |
| Historical components that suggest intentional trauma |
| No explanation or vague explanation for a significant injury |
| Significant delay in seeking medical attention |
| An important detail of the history changes dramatically over time |
| Explanation is inconsistent with the pattern, age, or severity of the injury |
| History does not explain the injuries identified |
| Explanation is inconsistent with the child's physical or developmental capabilities |
| Different witnesses provide markedly different explanations for the injury |
Physically abused children may present with nonspecific symptoms. Children with severe injuries resulting from abuse may present with difficulty breathing or unresponsiveness.1 Children who are evaluated for an apparent life-threatening event may also be victims of abuse. In a prospective series of 243 infants admitted to a tertiary care medical center for evaluation of an apparent life-threatening event, 2.5% were diagnosed with abusive head injuries.12 Epistaxis in children is common, but may be a sign of physical abuse during the first two years of life.13 In a retrospective series of infants who were evaluated for symptoms that were not initially recognized as the result of abusive head trauma, 65% were described as irritable and 56% were vomiting.14
Physical Examination
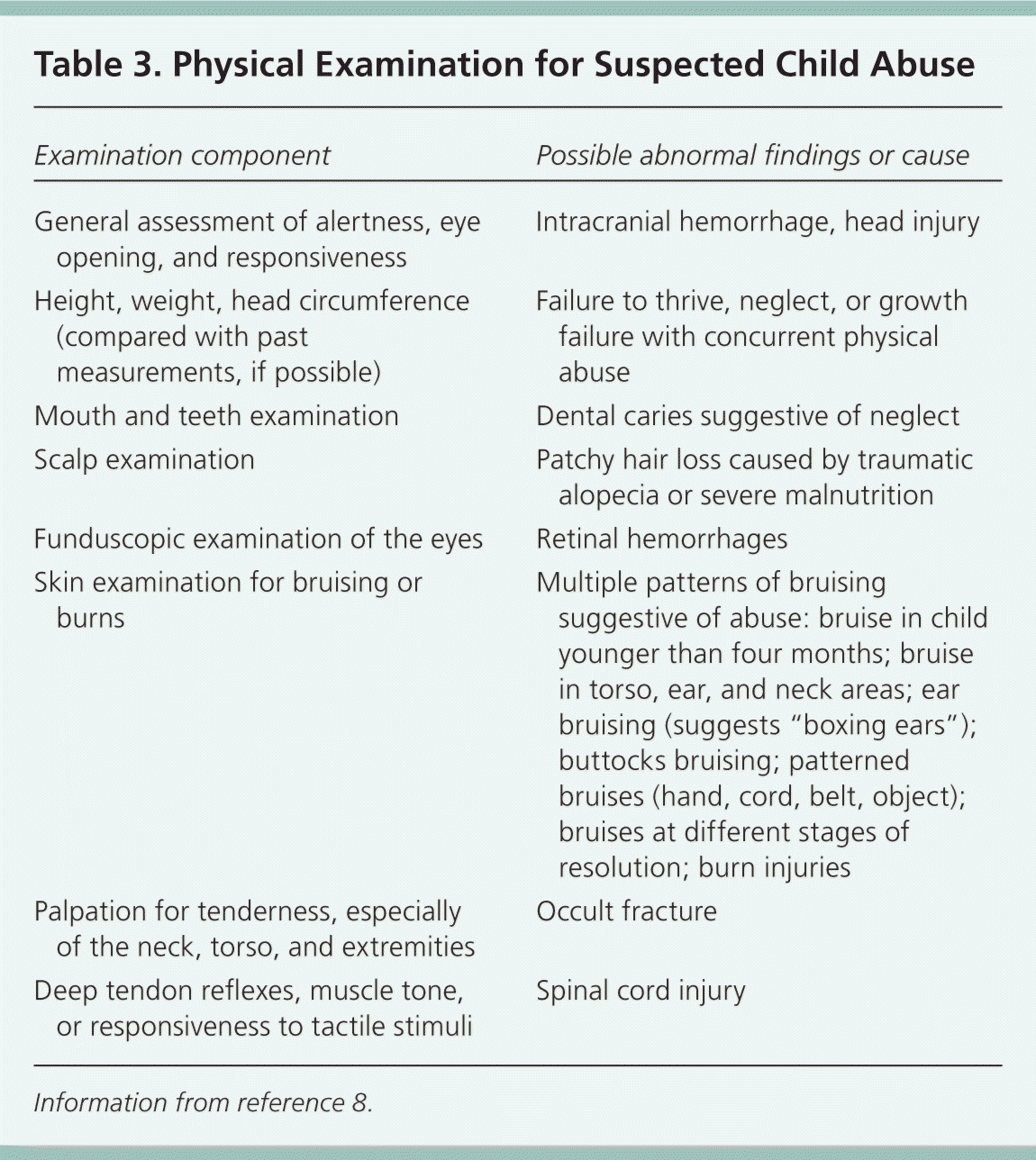
Table 3 lists physical examination steps to perform in an evaluation for child abuse, with possible causes or findings that are suggestive of abuse.8 In general, injuries to multiple areas, injuries in various stages of healing, and specific patterns of injuries are suspicious for physical abuse.11 Although accidental injuries often occur on bony prominences, inflicted injuries tend to occur in protected areas, such as the neck, buttocks, trunk, and upper arms.8 The TEN-4 bruising clinical decision rule may be useful to identify children and infants who should be evaluated for physical abuse.15 This rule was developed from a case-control study of 95 children younger than 48 months who were admitted to a pediatric intensive care unit because of trauma.15 The TEN-4 rule states that bruising on the torso, ear, or neck (TEN) in a child four years or younger, or bruising of any region in a child younger than four months, requires further evaluation for abuse. The initial study reported a sensitivity and specificity of 97% and 84%, respectively.
| Examination component | Possible abnormal findings or cause |
|---|---|
| General assessment of alertness, eye opening, and responsiveness | Intracranial hemorrhage, head injury |
| Height, weight, head circumference (compared with past measurements, if possible) | Failure to thrive, neglect, or growth failure with concurrent physical abuse |
| Mouth and teeth examination | Dental caries suggestive of neglect |
| Scalp examination | Patchy hair loss caused by traumatic alopecia or severe malnutrition |
| Funduscopic examination of the eyes | Retinal hemorrhages |
| Skin examination for bruising or burns | Multiple patterns of bruising suggestive of abuse: bruise in child younger than four months; bruise in torso, ear, and neck areas; ear bruising (suggests “boxing ears”); buttocks bruising; patterned bruises (hand, cord, belt, object); bruises at different stages of resolution; burn injuries |
| Palpation for tenderness, especially of the neck, torso, and extremities | Occult fracture |
| Deep tendon reflexes, muscle tone, or responsiveness to tactile stimuli | Spinal cord injury |
A cross-sectional survey of 973 children presenting for well-child visits found bruises in 203 children (21%).16 Consistent with previous studies, this study found bruising to be rare in children younger than six months; however, children between six and nine months of age who were beginning to ambulate (“cruise”) started to show bruises in predictable locations, such as the leg, knee, or forehead, as well as in less common areas, such as the back and chest.
Unusual events or accidents, in addition to uncommon medical problems, may also explain an observed clinical pattern. Coagulopathies (e.g., leukemia, cystic fibrosis with vitamin K deficiency, hemophilia, von Willebrand disease) may cause easy bruising, retinal hemorrhages, subdural hematomas, and other findings suggestive of abuse.17
Radiographic Imaging
Physical abuse often results in skeletal injury. Radiographic imaging of children with suspected physical abuse may consist of evaluation of localizing symptoms or physical examination signs, as well as screening skeletal surveys. Although skeletal injuries (other than skull fractures) are not always the life-threatening injuries most associated with abuse, identification of occult fractures may provide the clearest evidence of abuse as the cause of other identified injuries.
Skeletal survey imaging is typically recommended for all cases of suspected abuse in children younger than two years. Children older than five years can usually give a sufficient history of pain, and screening imaging is not recommended. Instead, imaging should be based on clinical findings. Screening imaging in children between two and five years of age should be guided by other findings or indicators of possible abuse, and performed in cases where abuse is strongly suspected.18 The content of the skeletal survey imaging series is outlined in Table 4.19 In general, each anatomic region should be imaged separately so that optimal exposure and image quality are ensured for each area; single-image studies (“babygrams”) are not considered sufficient for diagnosis and should be avoided.20 Obtaining both oblique projections to the anteroposterior view of the rib cage may increase the yield of rib fractures.19 Other imaging studies, such as computed tomography of the head, nuclear medicine imaging, or positron emission tomography, may be indicated depending on patient circumstances. Concerning findings on radiographic imaging include injury patterns that are highly or moderately specific for the diagnosis of child abuse20,21 (Table 522 ). Findings with relatively high specificity include metaphyseal lesions, posteromedial rib fractures, scapular or spinous process fractures, and sternal fractures.20,21

| Appendicular skeleton |
| Humeri (AP) |
| Forearms (AP) |
| Hands (PA) |
| Femurs (AP) |
| Lower legs (AP) |
| Feet (AP) |
| Axial skeleton |
| Thorax (AP, lateral, right and left obliques), to include ribs, thoracic and upper lumbar spine |
| Pelvis (AP), to include the mid lumbar spine |
| Lumbosacral spine (lateral) |
| Cervical spine (lateral) |
| Skull (frontal and lateral) |

| Highly specific injuries* |
| Classic metaphyseal lesions |
| Rib fractures, especially posteromedial |
| Sternal, scapular, and spinous process fractures |
| Moderately specific injuries* |
| Multiple fractures |
| Fractures in different stages of healing |
| Epiphyseal separations |
| Vertebral body fractures and subluxations |
| Digital fractures |
| Complex skull fractures |
| Common but low specificity |
| Clavicular fractures |
Laboratory Studies
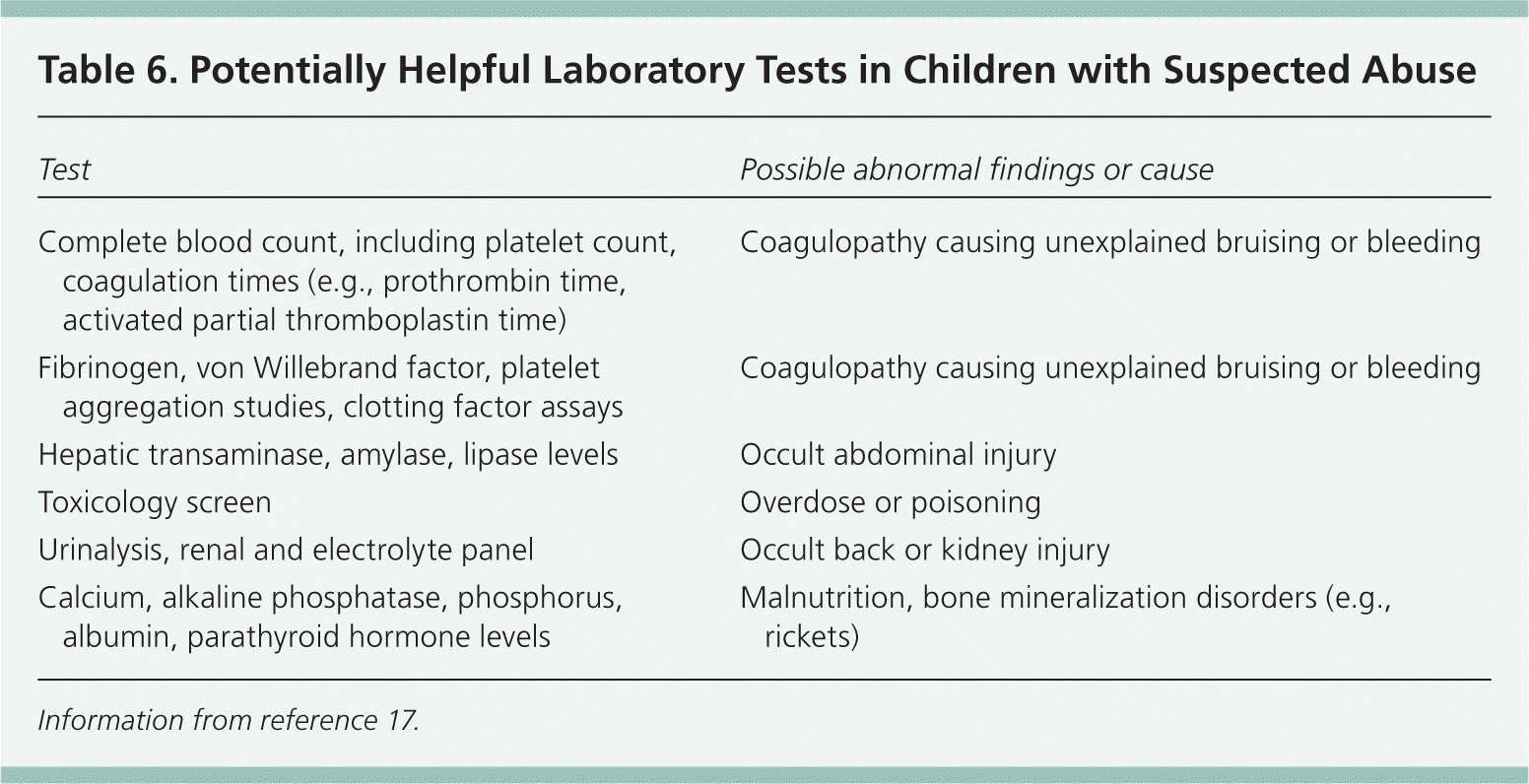
Laboratory studies are useful to identify disorders that might explain observed findings (particularly coagulopathies), or occult or more severe injury not evident on examination. Table 6 lists useful laboratory studies and their possible findings.17 Testing for sexually transmitted infection may be necessary if sexual abuse is suspected.
| Test | Possible abnormal findings or cause |
|---|---|
| Complete blood count, including platelet count, coagulation times (e.g., prothrombin time, activated partial thromboplastin time) | Coagulopathy causing unexplained bruising or bleeding |
| Fibrinogen, von Willebrand factor, platelet aggregation studies, clotting factor assays | Coagulopathy causing unexplained bruising or bleeding |
| Hepatic transaminase, amylase, lipase levels | Occult abdominal injury |
| Toxicology screen | Overdose or poisoning |
| Urinalysis, renal and electrolyte panel | Occult back or kidney injury |
| Calcium, alkaline phosphatase, phosphorus, albumin, parathyroid hormone levels | Malnutrition, bone mineralization disorders (e.g., rickets) |
Hepatic transaminase levels have a modest sensitivity and specificity (77% and 82%, respectively) for occult abdominal injuries at a cutoff level of 80 U per L (1.34 μkat per L). Although universal screening of injured children is not indicated, it may be useful to measure transaminase levels in children with suspected abuse (particularly suspected abdominal injuries) in whom abdominal computed tomography is not already planned.23
Documentation
Documentation of the history, physical examination, diagnostic study results, clinical impression, and diagnostic reasoning is vital not only for medical care, but also for legal purposes. This includes photography of physical examination findings that raise concern for abuse. Although digital photography has largely replaced traditional film, a few principles should be followed to provide the best documentation, regardless of the technology. Table 7 lists simple principles to follow to ensure that photographs will be of suitable quality and provide the best evidence should investigation of child abuse proceed to legal action.24

| Utilize a system to keep track of the patient's name and date of the photographs. |
| Take a picture of the child's/adolescent's face with the name card to identify him/her. |
| Take full-body photographs for identification purposes. |
| When photographing the patient's back, have the child/adolescent turn his/her face toward the camera for identification purposes. |
| Take photographs head-on so that the surface to be photographed is parallel to the camera and at the same level. |
| Compose the picture the way you normally look at the area. |
| Use an uncluttered, neutral-colored background. Skin is best photographed against a blue background. |
| Lighting is crucial to accurate color reproduction. In the absence of proper lighting, it is very important to document in writing in the medical chart the color and description of the lesion. |
| Document a finding with several shots taken from different distances and angles. Take some photographs of a lesion that include landmarks such as an elbow or a knee so that the lesion is seen in its proper location. |
| Use the rule of three. Take at least two shots of three orientations: full body, medium range of the finding, and close up. |
| Document the size of the injury by using an inch scale. Be sure that there is at least one other close-up of the injury without the scale to demonstrate that the scale was not covering evidence. |
| Document pattern or circumferential injuries, such as burns and bite marks, using photographs showing anteroposterior and lateral views. |
| Use close-ups to document pattern injuries and marks of restraint or bondage so that these injuries might later be compared with the rope or object that made the marks. |
| Take close-up photographs of hands and fingernails to show damage to the nails; missing nails; or traces of blood, skin, or hair. |
| Photograph transfer evidence that may be present on the patient's body or clothing, such as dirt, gravel, or vegetation. |
| Ultraviolet light may be helpful for photographing bite wounds months later, even when the overlying skin appears totally normal. |
| It may be useful to take serial photographs of injuries over a period of time to show progression of healing. |
Reporting
Physicians and other health care professionals are mandated by law to report child maltreatment in 48 states. The remaining two states mandate that all persons report child abuse.25 If a physician suspects or has reason to believe that a child has been abused or neglected, he or she must notify the local child protective services office or law enforcement agency. An additional resource is the Childhelp National Child Abuse Hotline at 800-4-A-CHILD (800-422-4453).
After a report of suspected child maltreatment has been made, the child protection process is initiated. Details of this process are beyond the scope of this article, but include intake (determine whether the report meets statutory and agency guidelines for investigation), initial assessment and investigation (determine whether maltreatment occurred), family assessment, case planning (specify goals to eliminate the risk of maltreatment), service provision (provide in-home services), evaluation of family progress, and case closure (determine if the family can protect the child without further child protective services intervention). The child protection process varies from state to state, but ideally involves the legal system and a multidisciplinary team approach.26
Communicating with Family Members
Parents are understandably frightened and concerned when physicians raise the issue of child abuse. There are no clear guidelines for effective communication strategies, although development of an initial rapport with the child and the family is important and beneficial during further discussions. Table 8 summarizes additional recommendations for communicating with the patient and the family, particularly a nonoffending caregiver.27

| Develop an initial rapport with the family as well as the child/adolescent patient. |
| Clearly state your role as an advocate for the child/adolescent. |
| Remain neutral in tone, and avoid confrontational or accusatory statements. |
| Invite parents to step out of the room so you can interview the child/adolescent alone. |
| Explain that abuse can exist in the absence of physical examination findings. |
| Explain that you need help assessing the child/adolescent for safety or possible abuse, and introduce the need for other agencies. |
| Inform parents if you need to contact police and/or child protective services; however, it is not necessary to tell parents if you are concerned that notifying them would increase the risk to the child/adolescent. |
| Explain your duty to report concerns, and explain your concerns to family members. |
| Remind the family that you will be present and available throughout the process. |
Data Sources: A Medline literature search was conducted using the MeSH term child abuse. To focus our search on physical abuse, the search did not include the MeSH term child abuse, sexual. The search was limited to English, human, core clinical journals (AIM), all child (0 to 18 years of age), and publication years 1995 to 2013. Secondary searches were conducted on this initial broad data set: limited to review articles, combined with the keyword and MeSH term communication, combined with the keyword prevention, and combined with the keyword screening. We also performed this search in the Cochrane Database of Systematic Reviews. Search dates: December 13, 2011, and October 20, 2013.
