
A more recent article on Bell palsy is available.
Am Fam Physician. 2014;89(3):209-212
Related letter: Acupuncture for the Treatment of Bell Palsy
Author disclosure: No relevant financial affiliations.
Bell palsy is an acute affliction of the facial nerve, resulting in sudden paralysis or weakness of the muscles on one side of the face. Testing patients with unilateral facial paralysis for diabetes mellitus or Lyme disease is not routinely recommended. Patients with Lyme disease typically present with additional manifestations, such as arthritis, rash, or facial swelling. Diabetes may be a comorbidity of Bell palsy, but testing is not needed in the absence of other indications, such as hypertension. In patients with atypical symptoms, magnetic resonance imaging with contrast enhancement can be used to rule out cranial mass effect and to add prognostic value. Steroids improve resolution of symptoms in patients with Bell palsy and remain the preferred treatment. Antiviral agents have a limited role, and may improve outcomes when combined with steroids in patients with severe symptoms. When facial paralysis is prolonged, surgery may be indicated to prevent ocular desiccation secondary to incomplete eyelid closure. Facial nerve decompression is rarely indicated or performed. Physical therapy modalities, including electrostimulation, exercise, and massage, are neither beneficial nor harmful.
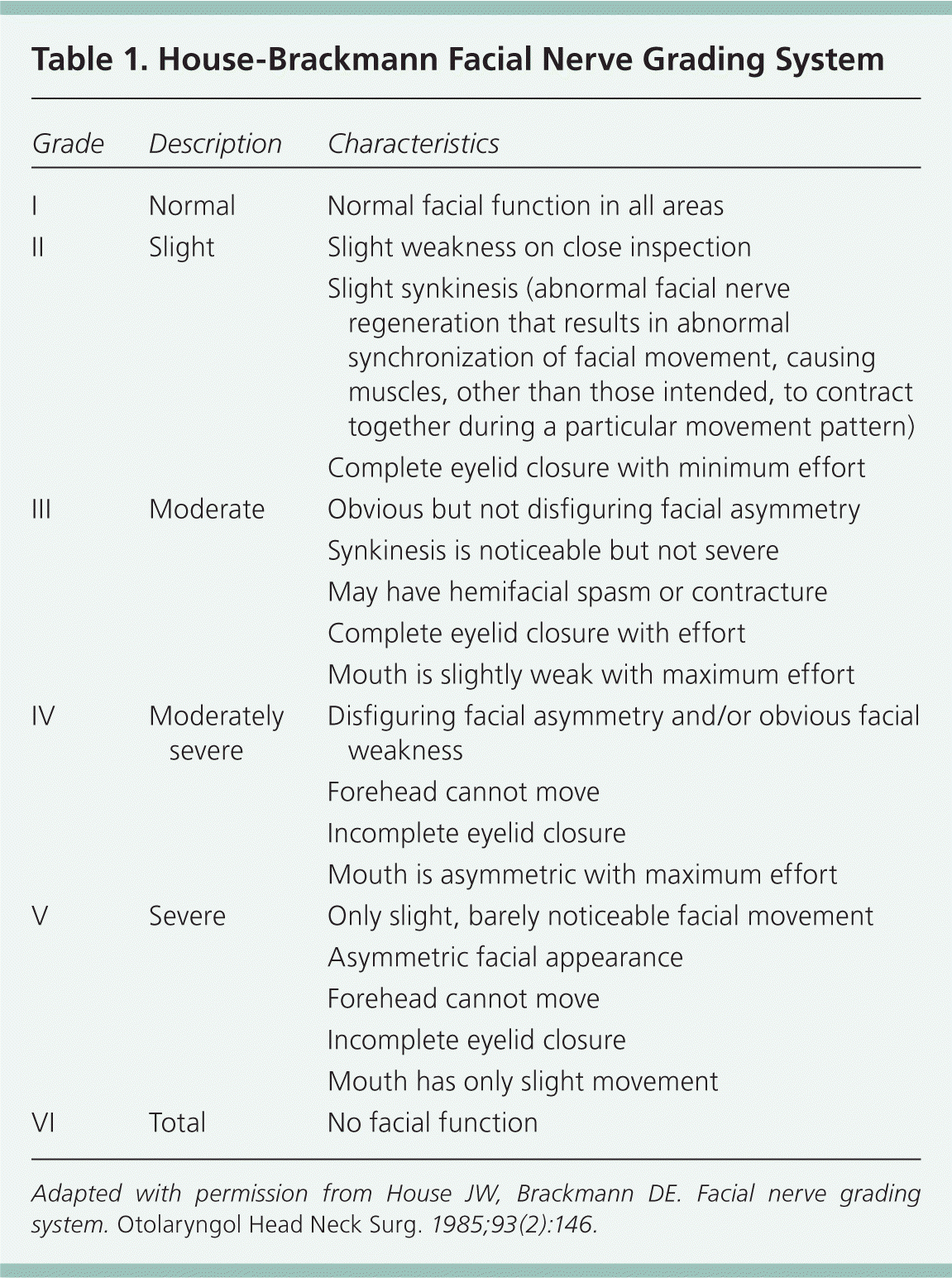
Bell palsy is an acute affliction of the facial nerve, resulting in sudden paralysis or weakness of the muscles on one side of the face. In addition to facial asymmetry, altered taste and unilateral tear production are common. Symptoms usually resolve within three months. The condition can affect patients of any age, although the prevalence peaks between 40 and 49 years.1 The severity of symptoms is assessed using the House-Brackmann grading system (Table 1).2
| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
| Routine testing for Borrelia burgdorferi is not recommended for patients with Bell palsy in the absence of additional symptoms of Lyme disease. | C | 3–6 | Consensus guideline based on prospective studies |
| Routine testing for diabetes mellitus or insulin resistance is not recommended for patients with Bell palsy in the absence of other indications. | C | 7, 8 | Consensus guideline based on observational studies |
| Magnetic resonance imaging should be considered when symptoms of Bell palsy do not improve over time or worsen. | C | 10–13 | Observational studies and consensus guidelines |
| Steroids reduce the duration of symptoms and are the preferred treatment for Bell palsy. | A | 9, 15, 17–19 | RCT and meta-analysis based on RCT |
| Physical therapy is neither beneficial nor harmful in the management of Bell palsy. | B | 23 | Meta-analysis |
| Grade | Description | Characteristics |
|---|---|---|
| I | Normal | Normal facial function in all areas |
| II | Slight | Slight weakness on close inspection |
| Slight synkinesis (abnormal facial nerve regeneration that results in abnormal synchronization of facial movement, causing muscles, other than those intended, to contract together during a particular movement pattern) | ||
| Complete eyelid closure with minimum effort | ||
| III | Moderate | Obvious but not disfiguring facial asymmetry |
| Synkinesis is noticeable but not severe | ||
| May have hemifacial spasm or contracture | ||
| Complete eyelid closure with effort | ||
| Mouth is slightly weak with maximum effort | ||
| IV | Moderately severe | Disfiguring facial asymmetry and/or obvious facial weakness |
| Forehead cannot move | ||
| Incomplete eyelid closure | ||
| Mouth is asymmetric with maximum effort | ||
| V | Severe | Only slight, barely noticeable facial movement |
| Asymmetric facial appearance | ||
| Forehead cannot move | ||
| Incomplete eyelid closure | ||
| Mouth has only slight movement | ||
| VI | Total | No facial function |
Should Patients with Apparent Bell Palsy Be Tested for Diabetes Mellitus or Lyme Disease?
Patients with Lyme disease usually have additional clinical manifestations, such as a history of tick bite, arthritis, rash, or facial swelling. Therefore, Borrelia burgdorferi testing is not recommended with isolated seventh nerve palsy. Diabetes has been shown to be a comorbidity in persons with Bell palsy, but it is not considered an etiology. Therefore, routine testing for diabetes or insulin resistance in the setting of Bell palsy is not indicated.
EVIDENCE SUMMARY
Facial palsy is rarely the only presenting symptom in patients with Lyme disease. In one study, 69 patients with presumed Bell palsy were clinically and serologically evaluated for Lyme borreliosis.3 None of the patients with Bell palsy had evidence of Lyme disease. In a separate group of nine patients with Lyme peripheral facial palsy, all had additional manifestations not present in patients with Bell palsy.3 Furthermore, three observational cohort studies demonstrated near uniformity of additional symptoms in patients who had Lyme borreliosis compared with patients who had Bell palsy.4–6 As a result, testing for antibodies to B. burgdorferi is not recommended for patients with a seventh nerve palsy who do not have additional manifestations of Lyme disease.
There is limited evidence to support testing for diabetes or insulin resistance in patients with Bell palsy in the absence of other indications (e.g., hypertension). A 2007 study evaluated several neurologic parameters of peripheral nerves (e.g., neurologic examinations, needle electromyography, electrophysiologic characteristics) in 132 patients who had diabetes, with and without peripheral facial paralysis. The results showed that Bell palsy is not a component of diabetic neuropathy.7 Diabetes is probably a compounding or predisposing factor, as suggested by a 2011 case-control study that found an association between Bell palsy and impaired glucose tolerance.8
What Is the Role of Imaging in Patients with Bell Palsy?
When Bell palsy symptoms do not improve over time or worsen in severity, magnetic resonance imaging (MRI) should be considered. MRI provides information about facial nerve inflammation but also may reveal cranial mass effect resulting in the palsy.
EVIDENCE SUMMARY
Bell palsy typically follows a predictable recovery pattern. Approximately 70% of untreated patients recover completely, and 85% of untreated patients have complete or near normal recovery.9 In patients who do not recover, MRI can determine typical facial nerve inflammatory patterns and, more importantly, rule out cranial mass effect from a schwannoma, a hemangioma, a meningioma, or a primitive or secondary cholesteatoma.10 MRI with contrast enhancement also has prognostic value in patients with acute idiopathic facial palsy.11 In children with facial palsy who underwent gadolinium-enhanced MRI, more than 40% showed nerve enhancement. In those without nerve enhancement, the mean time to recovery was significantly shorter (9.5 vs. 19.3 weeks).12
There is no consensus regarding the optimal timing for ordering imaging. It is reasonable to consider MRI in patients with an unremitting or progressive peripheral palsy lasting longer than two months.13 Facial twitching or spasms may result from tumor irritation of the facial nerve and should lead to prompt evaluation.1
Do Antivirals or Steroids, Alone or in Combination, Improve Patient Outcomes?
Steroids should be used to treat Bell palsy, but antivirals alone are ineffective. A typical regimen of 60 to 80 mg of prednisone daily for one week should be initiated as early as possible in the disease process. The combination of steroids and antivirals has not been proven to have a synergistic effect, and cannot be recommended routinely.9 However, in severe cases (i.e., level IV or greater on the House-Brackmann grading system [Table 12] ), a combination of prednisone and valacyclovir (Valtrex; typically 1 g three times daily for one week) may be offered, although it may not increase the probability of facial function improvement by more than 7%. Patients should be counseled that benefits may be modest at best, but risks and adverse effects are minimal.14
EVIDENCE SUMMARY
A 2009 meta-analysis of 18 randomized controlled trials (RCTs) involving 2,786 patients showed that steroids alone are beneficial for treating Bell palsy; however, antiviral agents alone were comparable to placebo.9
The effectiveness of combination steroids and antiviral agents vs. steroids alone is controversial. In a meta-analysis of seven RCTs, combination therapy was found to be marginally more effective than treatment with steroids alone. The results narrowly missed the threshold for clinical significance (relative risk = 0.75; 95% confidence interval, 0.56 to 1.00; P = .05).9 Studies indicating a synergistic effect with the combination of antivirals and steroids generally have a small number of participants. Additionally, several RCTs showed that steroids alone were effective for Bell palsy,15 whereas antivirals had no benefit when taken alone16 or when combined with steroids.9,14,17,18
Three multicenter RCTs with more than 1,500 adults compared combined regimens of prednisolone, antivirals, and placebo. Prednisolone was found to be beneficial, whereas the addition of acyclovir (Zovirax) showed no difference and valacyclovir showed a minimal benefit.17 In a double-blind, placebo-controlled, randomized trial of 496 patients with Bell palsy who were recruited within 72 hours of symptom onset, patients benefited from steroid treatment but not from acyclovir alone or in combination with prednisolone.18 A consensus guideline from the American Academy of Neurology suggests that patients with severe Bell palsy may be offered antivirals in combination with prednisolone after being counseled that benefit has not been established and may be modest at best, but risk is minimal.14
When Is It Appropriate to Offer Surgical Management of Bell Palsy?
Surgical management includes preventing complications of ocular desiccation and facial nerve decompression. Surgical intervention to prevent ocular desiccation is indicated when the facial nerve appears to be permanently impaired. Facial nerve decompression may be considered on a case-by-case basis by a neurotologist. The possible adverse effects, coupled with the poor quality of studies that show benefit, make this a rare option in current practice.
EVIDENCE SUMMARY
Without a functioning facial nerve, the eye is prone to desiccation secondary to incomplete eyelid closure. For this reason, when patients first present with Bell palsy, they should be given artificial tears and advised to tape their eye shut at night. When symptoms continue for several weeks, surgical management should be considered to prevent irreversible ocular damage.19
Surgical options range from mildly invasive techniques, such as eyelid weights, to more complex operations, such as temporalis muscle transfer, which attempts to restore functionality.20 Details of these operations are beyond the scope of this article.
Facial nerve decompression for sequelae of permanent facial palsy is not recommended routinely because of possible adverse effects and limited effectiveness. A 2011 Cochrane review found that RCTs showing effectiveness for facial nerve decompression were of low quality and insufficient for deciding whether the procedure is beneficial or harmful.21 In a 2011 survey of members of the American Otological Society and the American Neurotology Society, more than two-thirds of respondents would recommend surgery if patients met established electrophysiologic criteria. Lack of evidence was the most common reason for not recommending surgery. One-third of respondents had not performed a surgical decompression in the previous 10 years, and 95% performed fewer than one procedure per year.22
What Is the Role of Physical Therapy in the Management of Bell Palsy?
Physical therapy has not been proven beneficial or harmful in the management of Bell palsy.
EVIDENCE SUMMARY
The main modalities of physical therapy involve electrostimulation, exercise, and massage. Studies have evaluated the effect of these options on symptom duration and degree of resolution. A 2011 Cochrane review demonstrated no high-quality evidence of benefit or harm.23
Data Sources: We searched PubMed Clinical Queries, the Cochrane Database of Systematic Reviews, Essential Evidence Plus, the U.S. Preventive Services Task Force, and the Institute for Clinical Systems Improvement. In addition, the most recent review articles from the following journals were reviewed: the New England Journal of Medicine, the Journal of the American Medical Association, and American Family Physician. We identified highly cited studies found within these review articles and major databases to include in our review as appropriate. We limited our search timeline to the previous five years. Search dates: October 2011 and October 2013.
