
Am Fam Physician. 2014;89(5):395-397
Guideline source: American Academy of Pediatrics
Evidence rating system used? No
Literature search described? No
Guideline developed by participants without relevant financial ties to industry? Not reported
The American Academy of Pediatrics (AAP) has published a guideline on the management of gastroesophageal reflux (GER) in children based on recommendations from the North American and European Societies for Pediatric Gastroenterology, Hepatology, and Nutrition. It is important to determine whether the patient has gastroesophageal reflux disease (GERD) to facilitate appropriate treatment and to determine which patients need to be referred to a gastroenterologist. GER is defined as the physiologic passage of gastric contents into the esophagus and generally requires conservative management. GERD is reflux associated with troublesome symptoms or complications and may require further evaluation and treatment.
Diagnosis
CLINICAL FEATURES OF GERD
Troublesome symptoms or complications of reflux in full-term infants include feeding refusal, recurrent vomiting, poor weight gain, irritability, sleep disturbance, and respiratory symptoms. GERD in infants can also be associated with coughing, choking, wheezing, or upper respiratory tract symptoms. However, relying on symptoms to diagnose GERD can be difficult in infants, especially because medication does not always resolve symptoms. Rates of GERD are reportedly lower in breastfed infants compared with formula-fed infants, and the incidence peaks at four months of age.
Common troublesome symptoms and complications in children older than one year and in adolescents include abdominal pain or heartburn, recurrent vomiting, dysphagia, asthma, recurrent pneumonia, and upper airway symptoms (e.g., chronic cough, hoarseness).
DIAGNOSTIC STUDIES
In most children, and especially in adolescents, diagnostic studies are not needed to diagnose uncomplicated GER and GERD. However, a clinical history and physical examination are important to detect warning signs of more serious conditions. Warning signs include bilious vomiting, gastrointestinal tract bleeding, consistently forceful vomiting, fever, lethargy, hepatosplenomegaly, bulging fontanelle, macro- or microcephaly, seizures, abdominal tenderness or distension, genetic or metabolic syndrome, and associated chronic disease.
If used, diagnostic tests should be thought out and performed in a manner that can help establish a causal relationship between reflux and symptoms, to evaluate the effectiveness of treatment, and to exclude other diagnoses. Upper gastrointestinal tract radiography assesses the anatomy and can possibly document a motility disorder. Esophageal pH monitoring and intraluminal esophageal impedance can quantify GER. Upper endoscopy with esophageal biopsy is the primary method for excluding other conditions that can mimic the symptoms of GERD and evaluate for GERD-related esophageal injury. Other options include multichannel intraluminal impedance monitoring and scintigraphy.
Treatment
LIFESTYLE MODIFICATION
In infants with complicated GER or GERD, feeding changes may minimize symptoms. These changes include modifying maternal diet in breastfed infants and changing formula in formula-fed infants, reducing feeding volume while increasing feeding frequency, and thickening formula. A two- to four-week trial of a maternal exclusion diet that restricts at least milk and egg is recommended in breastfeeding infants with GERD symptoms, whereas an extensively hydrolyzed protein or amino acid–based formula may be appropriate in formula-fed infants. Thickening feedings may reduce symptoms, but there is concern for an increased risk of necrotizing enterocolitis in preterm infants. Keeping infants in an upright or prone position may also be effective, although only when awake and under supervision.
Older children and adolescents with GERD may benefit from losing weight if needed, not smoking or using alcohol, avoiding foods that may trigger symptoms, and chewing sugarless gum. Positioning changes may be helpful, but are not as well studied as in infants.
PHARMACOTHERAPY
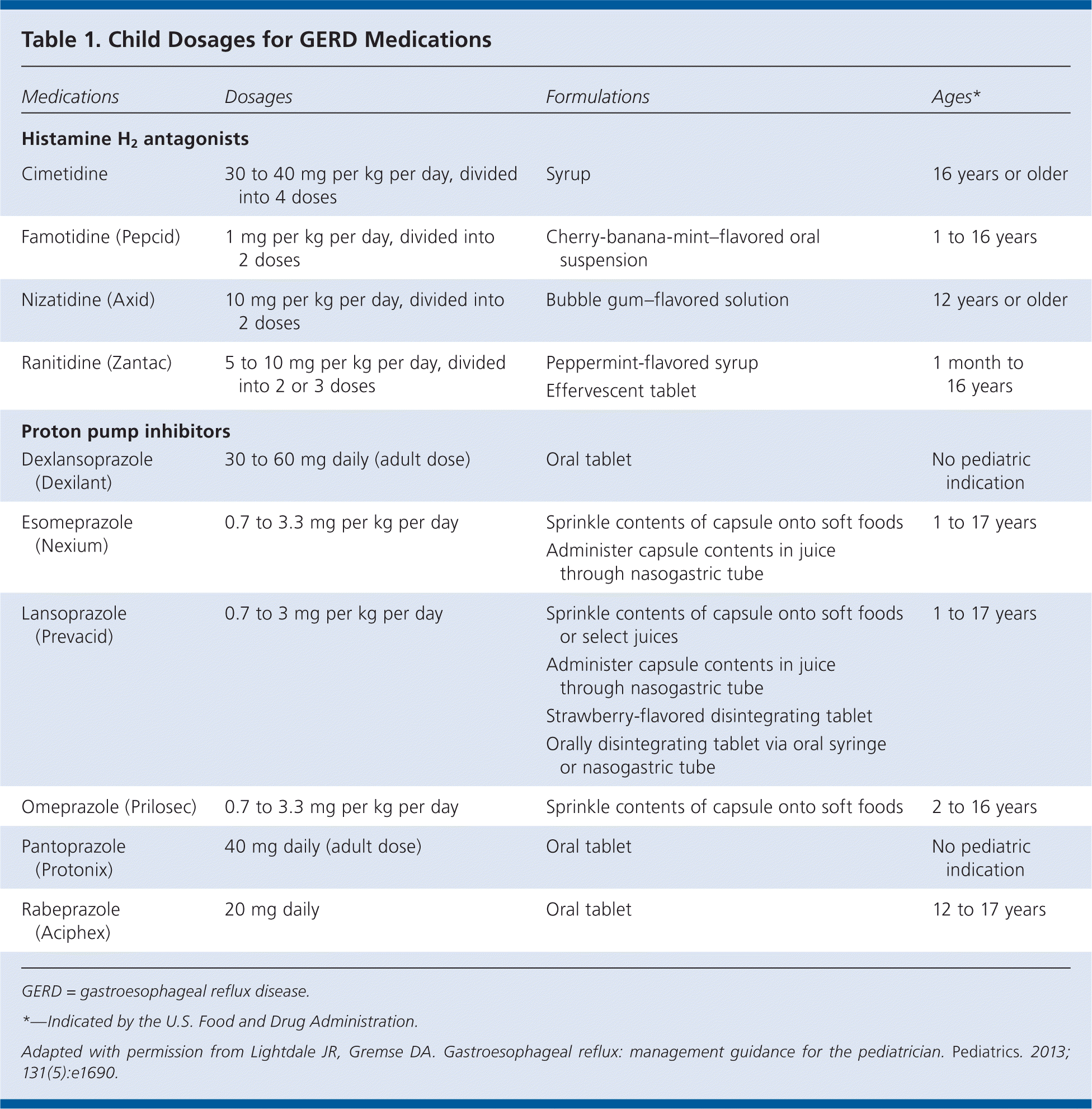
Acid suppressants or prokinetic agents may be used to treat GERD in infants and children. Table 1 includes child dosages of GERD medications. Acid suppressants, which include antacids, histamine H2 antagonists, and proton pump inhibitors, are more commonly used because of growing evidence that they are more effective than prokinetic agents; however, there is significant concern about the overprescription of acid suppressants, especially proton pump inhibitors. Because of risks, chronic antacid therapy is generally not recommended to treat GERD in children.
| Medications | Dosages | Formulations | Ages* |
|---|---|---|---|
| Histamine H2 antagonists | |||
| Cimetidine | 30 to 40 mg per kg per day, divided into 4 doses | Syrup | 16 years or older |
| Famotidine (Pepcid) | 1 mg per kg per day, divided into 2 doses | Cherry-banana-mint–flavored oral suspension | 1 to 16 years |
| Nizatidine (Axid) | 10 mg per kg per day, divided into 2 doses | Bubble gum–flavored solution | 12 years or older |
| Ranitidine (Zantac) | 5 to 10 mg per kg per day, divided into 2 or 3 doses | Peppermint-flavored syrup Effervescent tablet | 1 month to 16 years |
| Proton pump inhibitors | |||
| Dexlansoprazole (Dexilant) | 30 to 60 mg daily (adult dose) | Oral tablet | No pediatric indication |
| Esomeprazole (Nexium) | 0.7 to 3.3 mg per kg per day | Sprinkle contents of capsule onto soft foods | 1 to 17 years |
| Administer capsule contents in juice through nasogastric tube | |||
| Lansoprazole (Prevacid) | 0.7 to 3 mg per kg per day | Sprinkle contents of capsule onto soft foods or select juices | 1 to 17 years |
| Administer capsule contents in juice through nasogastric tube | |||
| Strawberry-flavored disintegrating tablet | |||
| Orally disintegrating tablet via oral syringe or nasogastric tube | |||
| Omeprazole (Prilosec) | 0.7 to 3.3 mg per kg per day | Sprinkle contents of capsule onto soft foods | 2 to 16 years |
| Pantoprazole (Protonix) | 40 mg daily (adult dose) | Oral tablet | No pediatric indication |
| Rabeprazole (Aciphex) | 20 mg daily | Oral tablet | 12 to 17 years |
H2 antagonists are effective, but long-term use is limited. They can cause tachyphylaxis within six weeks and may increase the risk of liver disease and gynecomastia. Proton pump inhibitors are the most potent acid suppressants and are superior to H2 antagonists. Effectiveness is related to timing of dosing (ideally, about 30 minutes before meals), and the metabolism of proton pump inhibitors differs in children compared with adults. Evidence suggests that acid suppression, with H2 antagonists or proton pump inhibitors, may be a risk factor for community-acquired pneumonia, gastroenteritis, candidemia, and necrotizing enterocolitis in preterm infants.
Prokinetic agents can decrease GERD symptoms by improving contractility of the body of the esophagus, increasing lower esophageal sphincter pressure, and increasing the rate of gastric emptying. However, the benefits of these agents may not outweigh the adverse effects, which include drowsiness, restlessness, and extrapyramidal reactions. There is insufficient evidence to support the routine use of prokinetic agents for GERD in children.
SURGERY
Fundoplication (i.e., the gastric fundus is wrapped around the distal esophagus) is the most common surgical intervention to prevent reflux in children. Total esophagogastric dissociation is rarely used if fundoplication is ineffective. Both procedures are associated with significant morbidity and are used only in carefully selected patients who have not improved with pharmacologic treatment or who have severe risk of aspiration of gastric contents. Before surgery, other etiologies should be carefully considered, and parents should be counseled about realistic expectations from surgery.
