
Am Fam Physician. 2014;90(2):80
Author disclosure: No relevant financial affiliations.
Increasing racial and ethnic diversity in the U.S. population has not been fully realized in the physician workforce. Family physicians, the most widely distributed of the physician specialties, are on the front line of a physician trend toward greater racial and ethnic diversity over the past two decades, but residents still lag behind national growth in the underrepresented minority population.
Using two decades worth of data from the U.S. census and the Association of American Medical Colleges, we explored trends in racial and ethnic composition among family medicine residents relative to those in the U.S. population at large. Underrepresented minority populations in the United States have increased over the past 20 years. From 1990 to 2012, the population increased from 9% to 17% for Hispanics/Latinos, from 11.7% to 12.2% for blacks/African Americans, and from 0.87% to 0.89% for Native Americans. During the same period, minority representation among family medicine residents changed from 4.9% to 9.4% for Hispanics/ Latinos, from 4.2% to 7.9% for blacks/ African Americans, and from 0.7% to 0.9% for Native Americans. Between 1990 and 2012 in the United States, there was increasing diversity among family medicine residents, with a declining ratio of white residents to the white population (see accompanying figure) and a substantive rise in the ratio of Asian residents to the Asian population (from 1.7:1.0 in 1990 to 5.1:1.0 in 2012). Growth in resident-to-population ratios was seen for each of the three underrepresented minority groups, although at different paces. During the same period, a similar trend of increasing underrepresented minority diversity occurred in pediatric and internal medicine residency programs.
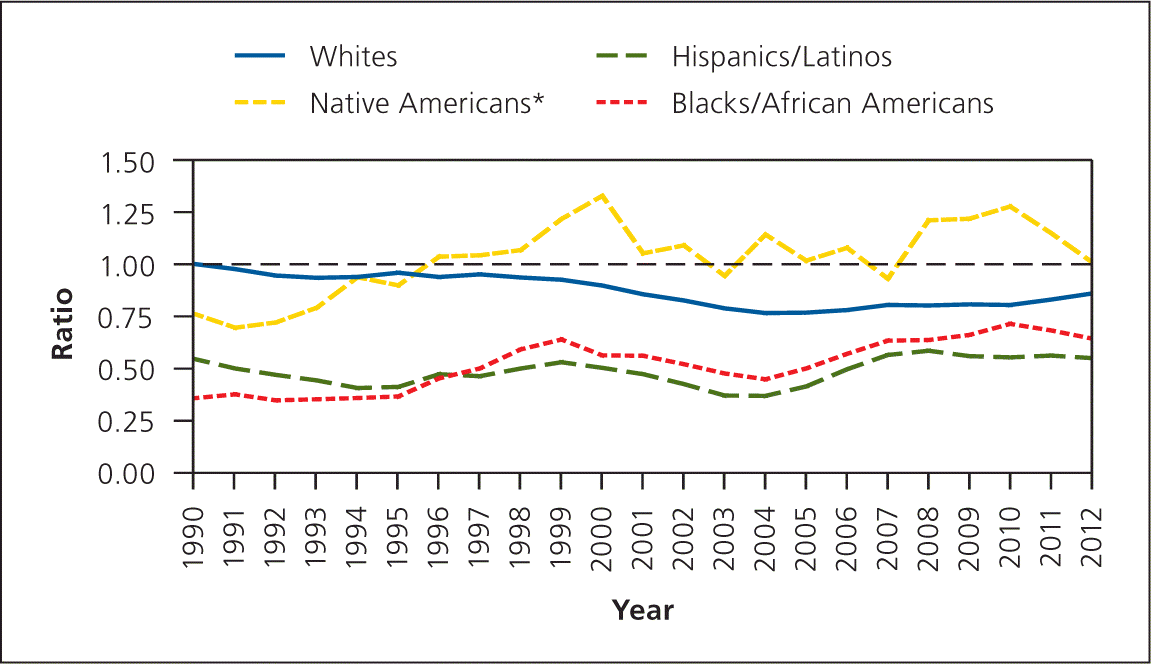
Diversifying the physician workforce has particularly profound implications in an era of insurance expansion that disproportionately affects underrepresented minority patients. Family physicians, the most widely and proportionally distributed of the physician specialties, are also increasingly diverse in their racial and ethnic backgrounds. However, as minority populations in the United States continue to expand, these findings highlight the need to foster entry into the discipline among underrepresented minorities to ensure a primary care work-force reflective of the population it serves.
