In 2010, as many as 45% of active primary care physicians (PCPs) were practicing at sites with five or fewer physicians. This large cohort of practices faces unique challenges in meeting the increasing demands of practice transformation, payer reporting requirements, and integrated delivery that merit policy maker and payer attention.
Efforts to transform and enhance national primary care practices are well underway, with some evidence that shows decreasing costs with expanding access and quality.1 Innovations have been implemented in practices that are part of larger, integrated systems or when there are shared community resources that support population management functions. Less has been written about transforming smaller practices, the number of which has not been well characterized.
Using National Provider Identifiers, which are required of physicians billing Medicare and Medicaid, we identified and located all PCPs by their street address and categorized all U.S. practices according to the number of PCPs collocated in a single site (see accompanying figure).2 Of the nearly 283,000 PCPs with National Provider Identifiers, more than 127,500 (45.0%) are located at sites with five or fewer physicians. Nearly 35,000 (12.4%) PCPs are at sites with more than 75 PCPs. Notably, clinics with five or fewer PCPs make up the majority (88.9%) of all practice sites.
Figure.
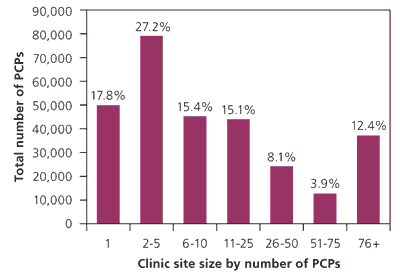
Number of primary care physicians (PCPs) by size of clinic site.
NOTE: The use of street address to identify practice sites means that the number of PCPs in different practices but with the same address are combined, as if they work at the same practice site, potentially producing an underestimation of small practices.
Information from reference 2.
Given these dimensions, transformation efforts must accommodate a wide range of practice sizes and configurations. Solo or small sites that are part of larger clinical networks will likely benefit from their larger network management and resources3 but may still need individualized strategies for successful transformation. The Affordable Care Act–authorized Primary Care Extension Program and initiatives to help create shared, community resources for small practices will be needed to achieve practice transformation on the scale required to improve health and health care, and reduce costs.
The information and opinions contained in research from the Graham Center do not necessarily reflect the views or the policy of the AAFP.

