Key Points for Practice
- The guideline emphasizes that lifestyle modification remains a critical component of ASCVD reduction.
- Four groups most likely to benefit from statin therapy are identified:
- 1. Patients with any form of clinical ASCVD
- 2. Patients with primary LDL-C levels of 190 mg per dL or greater
- 3. Patients with diabetes mellitus, 40 to 75 years of age, with LDL-C levels of 70 to 189 mg per dL
- 4. Patients without diabetes, 40 to 75 years of age, with an estimated 10-year ASCVD risk ≥ 7.5%
- Risk assessment for 10-year and lifetime risk is recommended using an updated ASCVD risk calculator: http://my.americanheart.org/cvriskcalculator
From the AFP Editors
Decades of research have demonstrated an association between high levels of low-density lipoprotein cholesterol (LDL-C) and an increased risk of atherosclerotic cardiovascular disease (ASCVD), including coronary heart disease, stroke, and peripheral arterial disease. Randomized controlled trials (RCTs) have found that treating with statins reduces ASCVD events. Based on these data, the Blood Cholesterol Expert Panel from the American College of Cardiology (ACC) and the American Heart Association (AHA) issued an updated evidence-based guideline in 2013 that addresses the use of fixed doses of cholesterol-lowering drugs (statins) to reduce the risk of ASCVD in adults 21 years and older.
What Is New in the Guideline?
FOUR STATIN BENEFIT GROUPS
This updated guideline focuses on reducing the risk of ASCVD in four statin benefit groups: (1) persons with clinical ASCVD (i.e., acute coronary syndromes, or a history of myocardial infarction, stable or unstable angina, coronary or other arterial revascularization, stroke, transient ischemic attack, or peripheral arterial disease of atherosclerotic origin); (2) persons with primary elevations of LDL-C levels of 190 mg per dL (4.92 mmol per L) or greater; (3) persons with diabetes mellitus who are 40 to 75 years of age with LDL-C levels of 70 to 189 mg per dL (1.81 to 4.90 mmol per L) but without clinical ASCVD; and (4) persons without clinical ASCVD or diabetes who have LDL-C levels of 70 to 189 mg per dL and an estimated 10-year ASCVD risk of 7.5% or greater. The guideline identifies high- and moderate-intensity statin therapy for use in primary and secondary prevention (Table 1). Less evidence is available to support nonstatin therapy for ASCVD prevention.
Table 1. High-, Moderate-, and Low-Intensity Statin Therapy (Used in the RCTs Reviewed by the Expert Panel)*

| High intensity | Moderate intensity | Low intensity |
|---|---|---|
| Daily dosage lowers LDL-C by approximately ≥ 50% on average | Daily dosage lowers LDL-C by approximately 30% to 50% on average | Daily dosage lowers LDL-C by < 30% average |
| Atorvastatin (Lipitor), 40† to 80 mg | Atorvastatin, 10(20)mg | Simvastatin, 10 mg |
| Rosuvastatin (Crestor), 20(40)mg | Rosuvastatin, (5)10 mg | Pravastatin, 10 to 20 mg |
| Simvastatin (Zocor), 20 to 40 mg‡ | Lovastatin, 20 mg | |
| Pravastatin (Pravachol), 40(80)mg | Fluvastatin, 20 to 40 mg | |
| Lovastatin (Mevacor), 40 mg | Pitavastatin, 1 mg | |
| Fluvastatin XL (Lescol XL), 80 mg | ||
| Fluvastatin, 40 mg twice daily | ||
| Pitavastatin (Livalo), 2 to 4 mg |
note: Specific statins and dosages noted in bold were evaluated in RCTs included in critical question 1, critical question 2, and the Cholesterol Treatment Trialists 2010 meta-analysis included in critical question 3 (see full guideline for details). All of these RCTs demonstrated a reduction in major cardiovascular events. Statins and dosages listed in italics are approved by the U.S. Food and Drug Administration but were not tested in the RCTs reviewed.
LDL-C = low-density lipoprotein cholesterol; RCT = randomized controlled trial.
*—Individual responses to statin therapy varied in the RCTs and should be expected to vary in clinical practice. There might be a biologic basis for a less-than-average response.
†—Evidence from one RCT only: down-titration if unable to tolerate atorvastatin, 80 mg, in Incremental Decrease through Aggressive Lipid Lowering study.
‡—Although simvastatin, 80 mg, was evaluated in RCTs, initiation of simvastatin, 80 mg, or titration to 80 mg is not recommended by the U.S. Food and Drug Administration because of the increased risk of myopathy, including rhabdomyolysis.
Adapted with permission from Stone NJ, Robinson JG, Lichtenstein AH, et al. 2013 ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation. 2014;129(25 suppl 2):S13.
Promotional and commercial use of the material in print, digital, or mobile device format is prohibited without the permission from the publisher Lippincott Williams & Wilkins. Please contact journalpermissions@lww.com for further information.
NEW PERSPECTIVE ON GOALS FOR LDL-C AND/OR NON–HDL-C LEVELS
The Expert Panel did not find evidence to support the use of specific LDL-C or non–high-density lipoprotein cholesterol (HDL-C) target levels. Although many clinicians use target levels (e.g., LDL-C levels less than 70 mg per dL for secondary prevention and less than 100 mg per dL [2.59 mmol per L] for primary prevention), evidence has shown that using the maximum tolerated statin intensity in persons who will benefit reduces ASCVD events. No RCTs were identified that titrated drug therapy to a specific target level to improve ASCVD outcomes. Using LDL-C targets could lead to under-treating with evidence-based statin therapy or overtreating with nonstatin drugs that have not been shown to reduce ASCVD events in RCTs.
GLOBAL RISK ASSESSMENT FOR PRIMARY PREVENTION
The Pooled Cohort Equations are recommended to estimate the 10-year risk and lifetime risk of ASCVD in white and black adults, with the goal of identifying high-risk persons who will benefit from statin therapy. Before initiating statin therapy, physicians and patients should discuss potential benefits, adverse effects, drug-drug interactions, and patient preferences. The absolute risk reduction in ASCVD events associated with statin therapy can be estimated by multiplying the 10-year ASCVD risk by the anticipated relative risk reduction based on the intensity of the statin (roughly 30% for moderate intensity and 45% for high intensity). The net ASCVD risk-reduction benefit is approximately the number of potential ASCVD events prevented with statin therapy vs. the number of potential excess adverse effects.
The Expert Panel acknowledges that persons 70 years or older may have the greatest potential for risk reduction with statin use, even without other risk factors. For example, for persons in this age group, the estimated 10-year risk is 7.5% or greater, which is a risk threshold for which a reduction in ASCVD events has been demonstrated in RCTs. Although evidence supports continuing the use of statins beyond 75 years of age in those already tolerating the drugs, limited data were available to support the initiation of statins for primary prevention in patients older than 75 years without clinical ASCVD.
SAFETY CONSIDERATIONS, BIOMARKERS, AND NONINVASIVE TESTS
RCT results identified safety concerns in persons taking statins. To maximize safety in men and in women who are not pregnant or nursing, physicians should select the appropriate statin and dose based on patient characteristics, ASCVD risk level, and potential for adverse effects. Characteristics that predispose patients to adverse effects from statin therapy include, but are not limited to, the following: multiple or serious comorbidities, such as impaired renal or hepatic function; a history of previous statin intolerance or muscle disorders; unexplained elevated levels of alanine transaminase greater than three times the upper limit of normal; patient characteristics or concomitant use of medications that affect statin metabolism; and age older than 75 years. See Table 8 in the full guideline for additional safety recommendations.
For persons who do not fall into one of the four statin benefit groups, other factors may be considered when making treatment decisions, including a primary LDL-C level of 160 mg per dL (4.14 mmol per L) or greater, or other evidence of genetic hyperlipidemias; family history of premature ASCVD before 55 years of age in a first-degree male relative or before 65 years of age in a first-degree female relative; high-sensitivity C-reactive protein level of 2 mg per L (19.05 nmol per L) or greater; coronary artery calcium score of 300 Agatston units or greater, or being in the 75th percentile or greater for age, sex, and ethnicity; ankle-brachial index less than 0.9; or elevated lifetime risk of ASCVD.
Statin Recommendations
The Expert Panel's treatment recommendations are divided into several major categories and are summarized in Table 2. An algorithm for determining appropriate statin therapy for patients who are candidates for treatment is presented in eFigure A. Specific classes of recommendation, levels of evidence, and their definitions are available in the full guideline.
Table 2. Summary of Major Recommendations for the Treatment of Blood Cholesterol to Reduce ASCVD Risk in Adults

| Encourage heart-healthy lifestyle habits for all individuals | ||
| Initiate or continue appropriate intensity of statin therapy | ||
| Clinical ASCVD* | ||
| Age ≤ 75 years and no safety concerns: high-intensity statin (COE = I; LOE = A) | ||
| Age > 75 years or safety concerns: moderate-intensity statin (COE = I; LOE = A) | ||
| Primary prevention: primary LDL-C ≥ 190 mg per dL (4.92 mmol per L) | ||
| Rule out secondary causes of hyperlipidemia (see Table 6 in full guideline) | ||
| Age ≥ 21 years: high-intensity statin (COE = I; LOE = B) | ||
| Achieve at least a 50% reduction in LDL-C (COE = IIa; LOE = B) | ||
| Consider LDL-C–lowering nonstatin therapy to further reduce LDL-C (COE = IIb; LOE = C) | ||
| Primary prevention: persons 40 to 75 years of age with diabetes mellitus and with LDL-C of 70 to 189 mg per dL (1.81 to 4.90 mmol per L) | ||
| Moderate-intensity statin (COE = I; LOE = A) | ||
| Consider high-intensity statin when ≥ 7.5% 10-year ASCVD risk using the Pooled Cohort Equations† (COE = IIa; LOE = B) | ||
| Primary prevention: persons 40 to 75 years of age without diabetes and with LDL-C of 70 to 189 mg per dL | ||
| Estimate 10-year ASCVD risk using the risk calculator based on the Pooled Cohort Equations† in those not receiving a statin; estimate risk every 4 to 6 years (COE = I; LOE = B) | ||
| To determine whether to initiate a statin, engage in a clinician-patient discussion of the potential for ASCVD risk reduction, adverse effects, drug-drug interactions, and patient preferences (COE = IIa; LOE = C) | ||
| Reemphasize heart-healthy lifestyle habits and address other risk factors | ||
| • ≥ 7.5% 10-year ASCVD risk: moderate- or high-intensity statin (COE = I; LOE = A) | ||
| • 5% to < 7.5% 10-year ASCVD risk: consider moderate-intensity statin (COE = IIa; LOE = B) | ||
| • Other factors may be considered‡: LDL-C ≥ 160 mg per dL (4.14 mmol per L), family history of premature cardiovascular disease, high-sensitivity C-reactive protein ≥ 2 mg per L (19.05 nmol per L), coronary artery calcium score ≥ 300 Agatston units, ankle-brachial index < 0.9, or elevated lifetime ASCVD risk (COE = IIb; LOE = C) | ||
| Primary prevention when LDL-C < 190 mg per dL and age < 40 or > 75 years, or < 5% 10-year ASCVD risk | ||
| Statin therapy may be considered in select individuals‡ (COE = IIb; LOE = C) | ||
| Statin therapy is not routinely recommended for individuals with New York Heart Association class II to IV heart failure or who are receiving maintenance hemodialysis | ||
| Regularly monitor adherence to lifestyle and drug therapy with lipid and safety assessments | ||
| Assess adherence, response to therapy, and adverse effects within 4 to 12 weeks following statin initiation or change in therapy (COE = I; LOE = A) | ||
| Measure fasting lipid levels (COE = I; LOE = A) | ||
| Do not routinely monitor alanine transaminase or creatine kinase levels unless symptomatic (COE = IIa; LOE = C) | ||
| Screen and treat type 2 diabetes according to current practice guidelines; heart-healthy lifestyle habits should be encouraged to prevent progression to diabetes (COE = I; LOE = B) | ||
| Anticipated therapeutic response: approximately ≥ 50% reduction in LDL-C from baseline for high-intensity statin and 30% to < 50% for moderate-intensity statin (COE = IIa; LOE = B) | ||
| • Insufficient evidence for LDL-C or non–HDL-C treatment targets from RCTs | ||
| • For those with unknown baseline LDL-C, an LDL-C < 100 mg per dL (2.59 mmol per L) was observed in RCTs of high-intensity statin therapy | ||
| Less than anticipated therapeutic response: | ||
| • Reinforce improved adherence to lifestyle and drug therapy (COE = I; LOE = A) | ||
| • Evaluate for secondary causes of hyperlipidemia if indicated (see Table 6 in full guideline) (COE = I; LOE = A) | ||
| • Increase statin intensity, or if on maximally tolerated statin intensity, consider addition of nonstatin therapy in select high-risk individuals§ (COE = IIb; LOE = C) | ||
| Regularly monitor adherence to lifestyle and drug therapy every 3 to 12 months after adherence has been established; continue assessment of adherence for optimal ASCVD risk reduction and safety (COE = I; LOE = A) | ||
| In individuals intolerant of the recommended intensity of statin therapy, use the maximally tolerated intensity of statin (COE = I; LOE = B) | ||
| If there are muscle or other symptoms, establish that they are related to the statin (COE = IIa; LOE = B) | ||
| For specific recommendations on managing muscle symptoms, see Table 8 in full guideline | ||
ASCVD = atherosclerotic cardiovascular disease; COE = class of recommendation||; HDL-C = high-density lipoprotein cholesterol; LDL-C = low-density lipoprotein cholesterol; LOE = level of evidence¶; RCTs = randomized controlled trials.
*—Clinical ASCVD includes acute coronary syndromes, or a history of myocardial infarction, stable or unstable angina, coronary or other arterial revascularization, stroke, transient ischemic attack, or peripheral arterial disease presumed to be of atherosclerotic origin.
†—Estimated 10-year or “hard” ASCVD risk includes first occurrence of nonfatal myocardial infarction, coronary heart disease death, and nonfatal and fatal stroke as used by the Risk Assessment Work Group in developing the Pooled Cohort Equations (see http://my.americanheart.org/cvriskcalculator and http://www.cardiosource.org/science-and-quality/practice-guidelines-and-quality-standards/2013-prevention-guideline-tools.aspx).
‡—These factors may include primary LDL-C ≥ 160 mg per dL or other evidence of genetic hyperlipidemias; family history of premature ASCVD with onset before 55 years of age in a first-degree male relative or before 65 years of age in a first-degree female relative; high-sensitivity C-reactive protein ≥ 2 mg per L; coronary artery calcium score ≥ 300 Agatston units or ≥ 75th percentile for age, sex, and ethnicity (for additional information, see http://www.mesa-nhlbi.org/CACReference.aspx); ankle-brachial index < 0.9; or lifetime risk of ASCVD. Additional factors that may aid in individual risk assessment may be identified in the future.
§—High-risk individuals include those with clinical ASCVD, an untreated LDL-C ≥ 190 mg per dL suggesting genetic hypercholesterolemia, or diabetes.
||—Classes of recommendation: I = procedure or treatment should be performed or administered; IIa = it is reasonable to perform procedure or administer treatment; IIb = procedure or treatment may be considered.
¶—Levels of evidence: A = multiple populations evaluated (data derived from multiple randomized clinical trials or meta-analyses); B = limited populations evaluated (data derived from a single randomized trial or nonrandomized studies); C = very limited populations evaluated (only consensus opinion of experts, case studies, or standard of care).
eFigure A. Major Recommendations for Statin Therapy for ASCVD Prevention
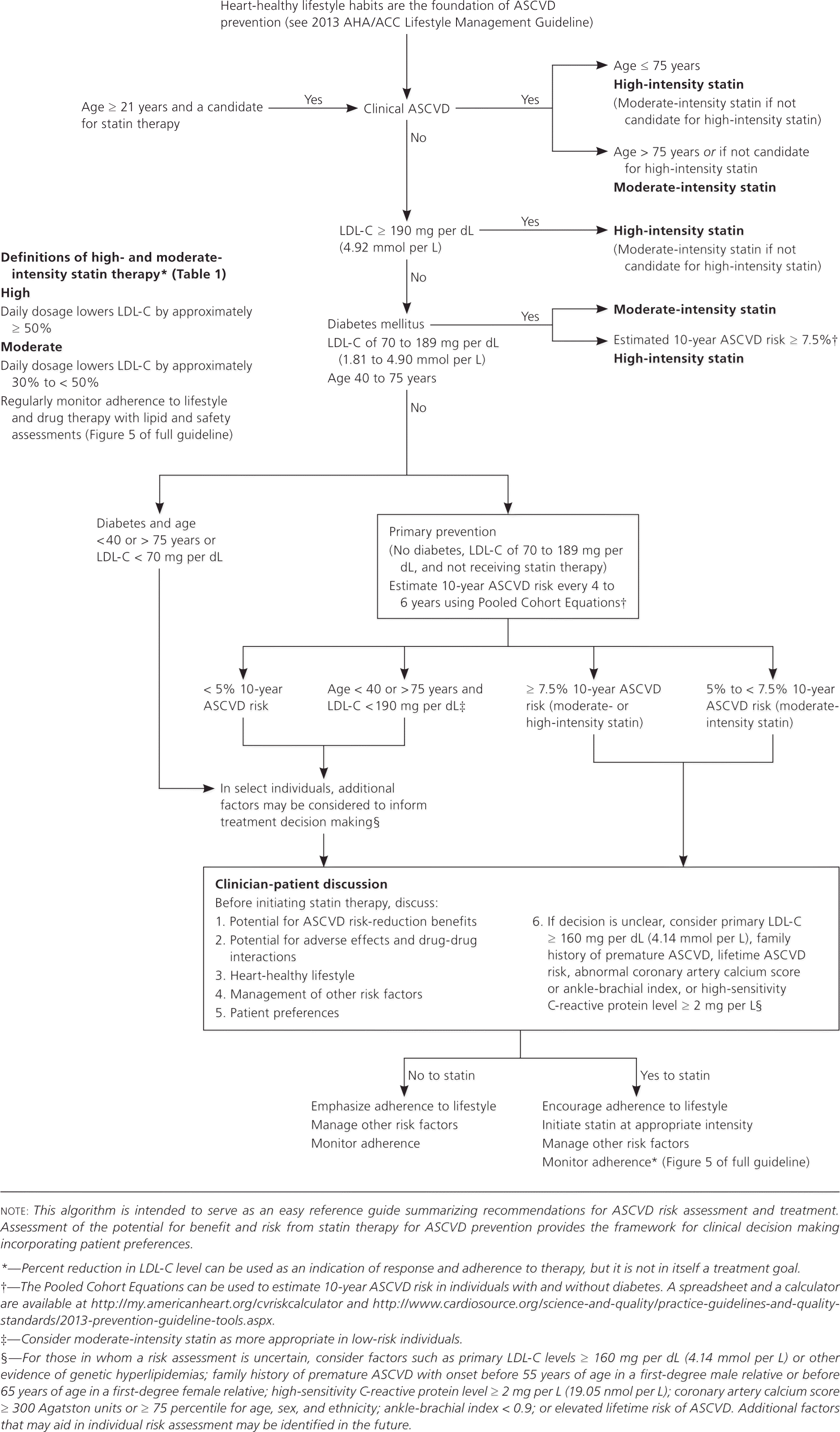
Algorithm for the prevention of ASCVD with statin therapy. (ACC = American College of Cardiology; AHA = American Heart Association; ASCVD = atherosclerotic cardiovascular disease; LDL-C = low-density lipoprotein cholesterol.)
Adapted with permission from Stone NJ, Robinson JG, Lichtenstein AH, et al. 2013 ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation. 2014;129(25 suppl 2):S9.
Promotional and commercial use of the material in print, digital, or mobile device format is prohibited without the permission from the publisher Lippincott Williams & Wilkins. Please contact journalpermissions@lww.com for further information.
TREATMENT TARGETS
There are no recommendations for or against specific target levels for LDL-C or non–HDL-C in the primary or secondary prevention of ASCVD.
SECONDARY PREVENTION
In men and women up to 75 years of age who have clinical ASCVD, high-intensity statin therapy should be initiated unless contraindicated. For persons with clinical ASCVD in whom high-intensity statin therapy is contraindicated but would otherwise be used, or in persons with characteristics predisposing to statin-associated adverse effects, moderate-intensity statins should be the second option, if tolerated. When initiating moderate- or high-intensity statin therapy in persons older than 75 years who have clinical ASCVD, it is reasonable to evaluate for potential risk-reduction benefits, adverse effects, and drug-drug interactions. Patient preferences should also be considered. Continuation of statin therapy is reasonable in persons who tolerate it.
PRIMARY PREVENTION IN PERSONS 21 YEARS OR OLDER WITH LDL-C LEVEL OF 190 MG PER DL OR GREATER
Persons who have LDL-C levels of 190 mg per dL or greater, or triglyceride levels of 500 mg per dL (5.65 mmol per L) or greater should be assessed for secondary causes of hyperlipidemia. Persons 21 years or older who have LDL-C levels of 190 mg per dL or greater should be treated with statin therapy. High-intensity statins should be used unless contraindicated. If high-intensity statins are not tolerated, the maximum tolerated intensity should be used. In persons with untreated LDL-C levels of 190 mg per dL or greater, statin therapy may be intensified to achieve a minimum 50% LDL-C reduction. When maximum intensity of statin therapy is reached, a nonstatin may be added to further reduce LDL-C levels. Potential benefits, adverse events, drug-drug interactions, and patient preferences should be considered.
PRIMARY PREVENTION IN PERSONS WITH DIABETES AND LDL-C LEVEL OF 70 TO 189 MG PER DL
Persons 40 to 75 years of age who have diabetes should start or continue moderate-intensity statin therapy. In those with 7.5% or greater estimated 10-year ASCVD risk, high-intensity statin therapy is reasonable, unless contraindicated. In persons younger than 40 years or older than 75 years, potential benefits, adverse events, drug-drug interactions, and patient preferences should be considered when deciding to initiate, continue, or intensify statin therapy.
PRIMARY PREVENTION IN PERSONS WITHOUT DIABETES AND WITH LDL-C LEVEL OF 70 TO 189 MG PER DL
The Pooled Cohort Equations should be used to estimate the 10-year ASCVD risk in persons without clinical ASCVD to guide initiation of statin therapy. In persons 40 to 75 years of age without clinical ASCVD or diabetes and with an estimated 10-year ASCVD risk of 7.5% or greater, moderate- to high-intensity statin therapy should be used. If the 10-year risk of ASCVD is 5% to less than 7.5%, treatment with a moderate-intensity statin is reasonable. Before initiating statin therapy, it is reasonable for clinicians and patients to engage in a discussion about the potential for ASCVD risk-reduction benefits, adverse events, drug-drug interactions, and patient preferences. Persons with LDL-C less than 190 mg per dL who do not fall into a statin benefit group or for whom risk-based treatment is uncertain, other factors may be used to inform treatment decision making. Statin therapy may be considered after evaluating for potential benefits, adverse events, drug-drug interactions, and patient preferences.
HEART FAILURE AND HEMODIALYSIS
There are no recommendations on initiating or discontinuing statin therapy in patients with New York Heart Association class II through IV ischemic systolic heart failure or in patients on maintenance hemodialysis.
Guideline source: American College of Cardiology and American Heart Association
Evidence rating system used? Yes
Literature search described? Yes
Guideline developed by participants without relevant financial ties to industry? No
Published source: Circulation, June 24, 2014
Available at: http://circ.ahajournals.org/content/129/25_suppl_2/S1
Endorsed with qualifications by the AAFP, June 2014: https://www.aafp.org/patient-care/clinical-recommendations/all/cholesterol.html

