Am Fam Physician. 2015;91(2):86-92
Patient information: See related handout on wound care, written by the authors of this article.
Author disclosure: No relevant financial affiliations.
Lacerations, abrasions, burns, and puncture wounds are common in the outpatient setting. Because wounds can quickly become infected, the most important aspect of treating a minor wound is irrigation and cleaning. There is no evidence that antiseptic irrigation is superior to sterile saline or tap water. Occlusion of the wound is key to preventing contamination. Suturing, if required, can be completed up to 24 hours after the trauma occurs, depending on the wound site. Tissue adhesives are equally effective for low-tension wounds with linear edges that can be evenly approximated. Although patients are often instructed to keep their wounds covered and dry after suturing, they can get wet within the first 24 to 48 hours without increasing the risk of infection. There is no evidence that prophylactic antibiotics improve outcomes for most simple wounds. Tetanus toxoid should be administered as soon as possible to patients who have not received a booster in the past 10 years. Superficial mild wound infections can be treated with topical agents, whereas deeper mild and moderate infections should be treated with oral antibiotics. Most severe infections, and moderate infections in high-risk patients, require initial parenteral antibiotics. Severe burns and wounds that cover large areas of the body or involve the face, joints, bone, tendons, or nerves should generally be referred to wound care specialists.
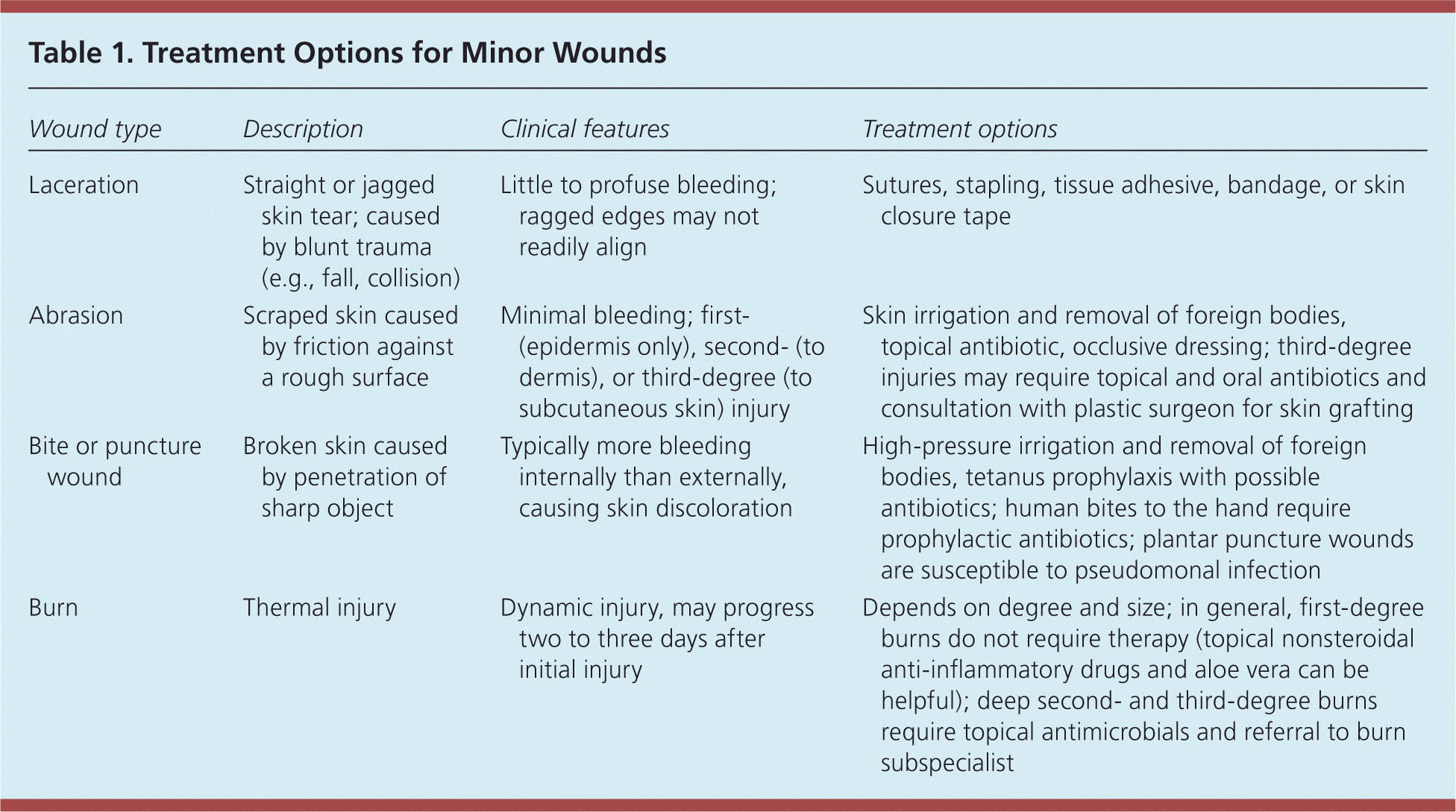
Family physicians often treat patients with minor wounds, such as simple lacerations, abrasions, bites, and burns. This article reviews common questions associated with wound healing and outpatient management of minor wounds (Table 1). More chronic, complex wounds such as pressure ulcers1 and venous stasis ulcers2 have been addressed in previous articles.
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Tap water produces similar outcomes to sterile saline irrigation of minor wounds. | B | 4, 5 |
| Noninfected wounds caused by clean objects may undergo primary closure up to 18 hours from the time of injury. Wounds on the head and face may be closed up to 24 hours from the time of injury. | B | 12, 13 |
| Tissue adhesives can be used as an alternative for closure of simple, noninfected lacerations in which the wound edges are easily approximated in areas of low tension and moisture. | A | 15–17 |
| Sutures can be uncovered and allowed to get wet within the first 24 to 48 hours without increasing the risk of infection. | B | 19 |
| Prophylactic systemic antibiotics are not necessary for healthy patients with clean, noninfected, nonbite wounds. | A | 20, 24 |
| Topical antimicrobials should be considered for mild, superficial wound infections. Mupirocin (Bactroban) is preferred for wounds with suspected methicillin-resistant Staphylococcus aureus. | C | 31, 33–35 |
| Nonsuperficial mild to moderate wound infections can be treated with oral antibiotics. | B | 30, 31 |
| Most severe wound infections, and moderate infections in high-risk patients, require initial parenteral antibiotics, with transition to oral antibiotics after therapeutic response. | C | 30, 31 |

| Recommendation | Sponsoring organization |
|---|---|
| Avoid antibiotics and wound cultures in emergency department patients with uncomplicated skin and soft tissue abscesses after successful incision and drainage and with adequate medical follow-up. | American College of Emergency Physicians |
| Do not routinely use topical antibiotics on a surgical wound. | American Academy of Dermatology |
| Wound type | Description | Clinical features | Treatment options |
|---|---|---|---|
| Laceration | Straight or jagged skin tear; caused by blunt trauma (e.g., fall, collision) | Little to profuse bleeding; ragged edges may not readily align | Sutures, stapling, tissue adhesive, bandage, or skin closure tape |
| Abrasion | Scraped skin caused by friction against a rough surface | Minimal bleeding; first- (epidermis only), second- (to dermis), or third-degree (to subcutaneous skin) injury | Skin irrigation and removal of foreign bodies, topical antibiotic, occlusive dressing; third-degree injuries may require topical and oral antibiotics and consultation with plastic surgeon for skin grafting |
| Bite or puncture wound | Broken skin caused by penetration of sharp object | Typically more bleeding internally than externally, causing skin discoloration | High-pressure irrigation and removal of foreign bodies, tetanus prophylaxis with possible antibiotics; human bites to the hand require prophylactic antibiotics; plantar puncture wounds are susceptible to pseudomonal infection |
| Burn | Thermal injury | Dynamic injury, may progress two to three days after initial injury | Depends on degree and size; in general, first-degree burns do not require therapy (topical nonsteroidal anti-inflammatory drugs and aloe vera can be helpful); deep second- and third-degree burns require topical antimicrobials and referral to burn subspecialist |
Should Water or an Antiseptic Be Used to Cleanse a Wound?
Antiseptics are commonly used to irrigate contaminated wounds. In studies of clean surgical incisions, there was no high-quality evidence that one antiseptic was superior to another for preventing wound infections. Tap water and sterile saline irrigation of uncomplicated skin lacerations appear to be equally effective. Patients may prefer irrigation with warm fluids.
EVIDENCE SUMMARY
A systematic review of 13 studies of skin antiseptics used before clean surgical incisions found no high-quality evidence of significant differences in effectiveness.3 A systematic review of seven randomized controlled trials (RCTs) demonstrated no significant difference in the risk of infection when using tap water vs. sterile saline when cleaning acute or chronic wounds.4 A single-blind RCT involving 715 patients demonstrated similar rates of infection with tap water and sterile saline irrigation (4% vs. 3.3%, respectively) in uncomplicated skin lacerations requiring staple or suture repair.5 Three RCTs found no significant difference in infection rates with tap water irrigation vs. no cleansing.4 A small RCT involving 38 patients found that warm saline was preferred over room temperature solution.6
Should Wounds Be Occluded?
EVIDENCE SUMMARY
Dressings protect the wound by acting as a barrier to infection and absorbing wound fluid. A moist wound bed stimulates epithelial cells to migrate across the wound bed and resurface the wound.8 A dry environment leads to cell desiccation and causes scab formation, which delays wound healing. Older studies in animals and humans suggest that moist wounds had faster rates of re-epithelialization compared with dry wounds.9–11
When Is It No Longer Reasonable to Suture a Wound?
Guidelines recommend primary closure of wounds that are clean and have no signs of infection within six to 12 hours of the injury; one study suggests that suturing can be delayed for up to 18 hours.12,13 Wounds to areas with an extensive vascular supply (e.g., head, face) may be closed up to 24 hours from the time of injury.13 Because of the high risk of infection, bite wounds are typically left open unless they are on the face and are potentially disfiguring. Bite wounds may be reevaluated after antibiotic treatment for delayed primary closure.14
EVIDENCE SUMMARY
A 1988 case series of 204 minor, noninfected suture repair wounds that did not involve nerves, blood vessels, tendons, or bones found significantly higher rates of healing for wounds closed up to 19 hours after injury compared with later closure (92% vs. 77%).12 Scalp and facial wounds repaired later than 19 hours after injury had higher healing rates compared with wounds involving other body areas (96% vs. 66%).12 There have been no RCTs comparing primary closure with delayed closure of nonbite traumatic wounds.13
Is Tissue Adhesive as Effective as Suturing for Minor Lacerations?
Simple lacerations are often closed with sutures or staples. However, tissue adhesives are equally effective for low-tension wounds with linear edges that can be evenly approximated. Tissue adhesives are not recommended for wounds with complex jagged edges or for those over high-tension areas (e.g., hands, joints).15 Tissue adhesives are easy to use, require no anesthesia and less procedure time, and provide good cosmetic results.15–17
EVIDENCE SUMMARY
An RCT of 814 patients comparing tissue adhesive (octyl cyanoacrylate) with standard wound closure for traumatic lacerations found that tissue adhesive resulted in statistically significant faster procedure times (three vs. five minutes).16 There was no difference in rates of infection or wound dehiscence, or in the appearance of the wound after three months. A systematic review of 11 studies comparing tissue adhesive with standard wound closure for acute lacerations found that tissue adhesives are less painful and require less procedure time.17 The review found no difference in cosmetic outcomes; however, there was a small but statistically significant increased rate of dehiscence and erythema with tissue adhesives.
Can Sutures Get Wet?
Although patients are often instructed to keep their wounds covered and dry after suture placement, sutures can get wet within the first 24 to 48 hours without increasing the risk of infection.
EVIDENCE SUMMARY
An observational study of 100 patients who washed their sutured wounds within 24 hours showed no infection or dehiscence of the wound.18 An RCT of 857 patients found no increased incidence of infection in patients who kept their wounds dry and covered for 48 hours vs. those who removed their dressing and got their wound wet within the first 12 hours (8.9% vs. 8.4%, respectively).19
When Are Prophylactic Antibiotics Appropriate?
Prophylactic antibiotics have little benefit in healthy patients with clean wounds. Topical antibiotic ointments decrease the risk of infection in minor contaminated wounds. Prophylactic antibiotic use may reduce the incidence of infection in human bite wounds. Prophylactic oral antibiotics are generally prescribed for deep puncture wounds and wounds involving the palms and fingers.
EVIDENCE SUMMARY
A meta-analysis of seven RCTs involving 1,734 patients with simple nonbite wounds found that those who received systemic antibiotics did not have a significantly lower incidence of infection compared with untreated patients.20 An RCT of 922 patients undergoing sterile surgical procedures found no increased incidence of infection and similar healing rates with topical application of white petrolatum to the wound site compared with antibiotic ointment.21 However, several studies have supported the use of prophylactic topical antibiotics for minor wounds. An RCT of 426 patients with uncomplicated wounds found significantly lower infection rates with topical bacitracin, neomycin/bacitracin/polymyxin B, or silver sulfadiazine (Silvadene) compared with topical petrolatum (5.5%, 4.5%, 12.1%, and 17.6%, respectively).22
Topical silver-containing ointments and dressings have been used to prevent wound infections. A review of 26 RCTs found insufficient evidence to support these treatments.23 A review of eight RCTs of bites from cats, dogs, and humans found that the use of prophylactic antibiotics significantly reduced infection rates after human bites (odds ratio = 0.02; 95% confidence interval, 0.00 to 0.33), but not after dog or cat bites.24 A Cochrane review found three small trials in which prophylactic antibiotics after bites to the hand reduced the risk of infection from 28% to 2%.24
When Is Tetanus Prophylaxis Needed for Minor Wounds?
The Centers for Disease Control and Prevention recommends that tetanus toxoid be administered as soon as possible to patients who have no history of tetanus immunization, who have not completed a primary series of tetanus immunization (at least three tetanus toxoid–containing vaccines), or who have not received a tetanus booster in the past 10 years.25 Tetanus immunoglobulin is also indicated for patients with puncture or contaminated wounds who have never had tetanus immunization.26
How Are Wound Infections Diagnosed and Treated?
Symptoms of infection may include redness, swelling, warmth, fever, pain, lymphangitis, lymphadenopathy, and purulent discharge.27–29 The treatment of wound infections depends on the severity of the infection, type of wound, and type of pathogen involved. Treatment may include debridement and wound dressings that promote granulation, tissue preservation, and moisture. Empiric antibiotic treatment should be based on the potentially causative organism. Superficial mild infections can be treated with topical agents, whereas mild and moderate infections involving deeper tissues should be treated with oral antibiotics. Most severe infections, and moderate infections in high-risk patients, require initial parenteral antibiotics.30,31 Cultures should be obtained for wounds that do not respond to empiric therapy, and in immunocompromised patients.30
EVIDENCE SUMMARY
Wounds often become colonized by normal skin flora (gram-positive cocci, gram-negative bacilli, and anaerobes), but most immunocompetent patients will not develop an infection. An infected wound will disrupt tissue granulation and delay healing. Superficial mild infections can be treated with topical antibiotics; other infections require oral or intravenous antibiotics. Penetrating wounds from bites or other materials may introduce other types of bacteria. The goal of treatment is to eliminate the bacteria without further damage to the underlying tissue.
Assessment and Initial Care. Evaluating the extent and severity of the infection will help determine the proper treatment course. The Infectious Diseases Society of America uses several clinical indicators to help stage the severity of wounds: those without purulence or inflammation are considered noninfected, and infected wounds are classified as mild, moderate, or severe based on their size and depth, surrounding cellulitis, tissue involvement, and presence of systemic or metabolic findings30,32 (Table 230–33 ).
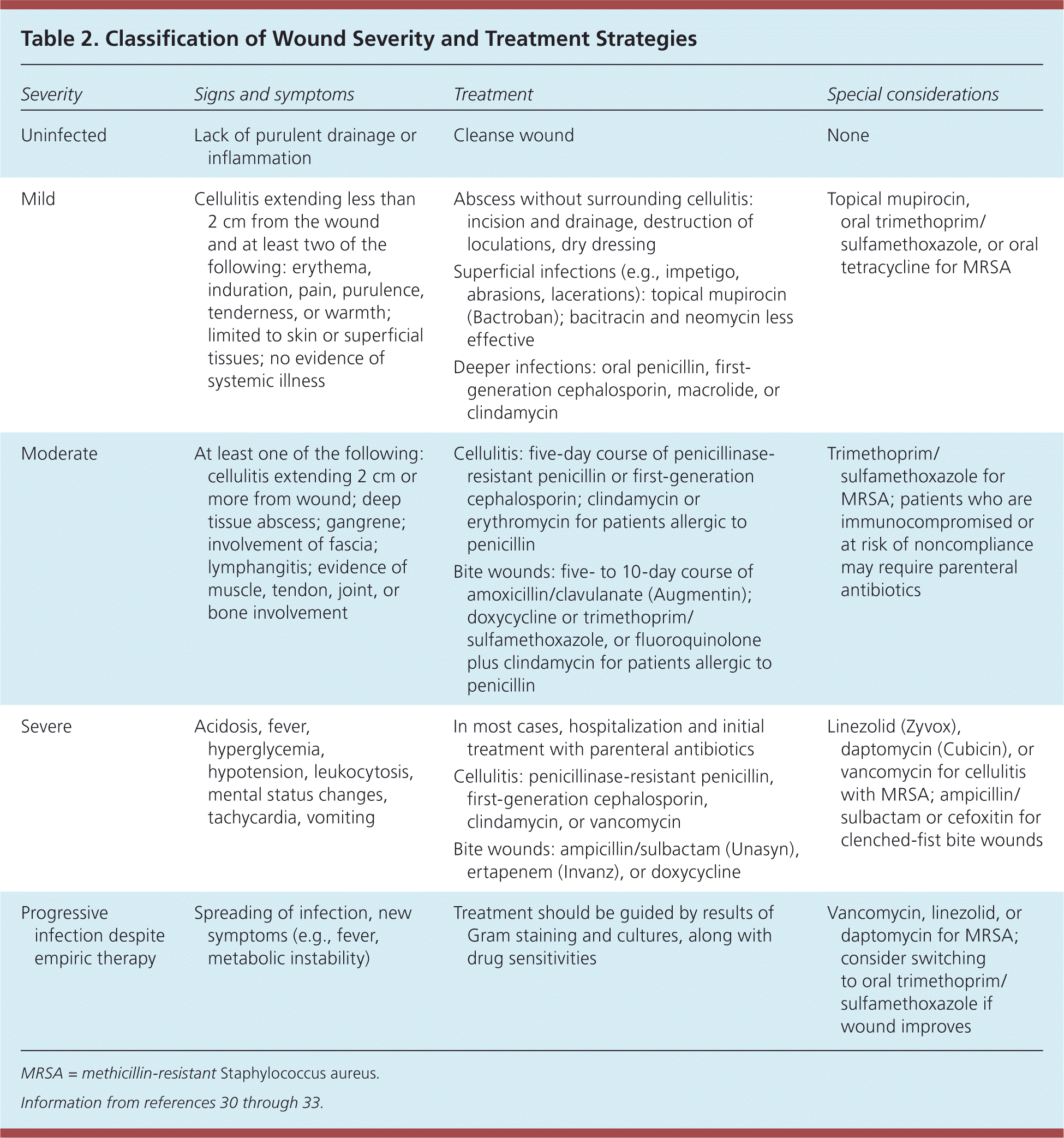
| Severity | Signs and symptoms | Treatment | Special considerations |
|---|---|---|---|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Treatment for an infected wound should begin with cleansing the area with sterile saline. Debridement can be performed using surgical techniques or topical agents that lead to enzymatic breakdown or autolysis of necrotic tissue. Five RCTs with a total of 159 patients found weak evidence that enzymatic debridement leads to faster results compared with saline-soaked dressings.34 Elevation of the affected area and optimal treatment of underlying predisposing conditions (e.g., diabetes mellitus) will help the healing process.30
Antibiotic Selection. Superficial mild infections (e.g., impetigo, mild cellulitis from abrasions or lacerations) are usually caused by staphylococci and streptococci and can be treated with topical antimicrobials, such as bacitracin, polymyxin B/bacitracin/neomycin, and mupirocin (Bactroban).31 Metronidazole gel 0.75% can be used alone or in combination with other antibiotics if anaerobes are suspected. There is limited evidence to suggest one topical agent over another, except in the case of suspected methicillin-resistant Staphylococcus aureus infection, in which mupirocin 2% cream or ointment is superior to other topical agents and certain oral antibiotics.33–35
Empiric oral antibiotics should be considered for nonsuperficial mild to moderate infections.30,31 Most infections in nonpuncture wounds are caused by staphylococci and streptococci and can be treated empirically with a five-day course of a penicillinase-resistant penicillin, first-generation cephalosporin, macrolide, or clindamycin. Consensus guidelines recommend trimethoprim/sulfamethoxazole or tetracycline if methicillin-resistant S. aureus infection is suspected,30 although a Cochrane review found insufficient evidence that one antibiotic was superior for treating methicillin-resistant S. aureus–colonized nonsurgical wounds.36
Moderate wound infections in immunocompromised patients and severe wound infections usually require parenteral antibiotics, with possible transition to oral agents.30,31 The choice of agent should be based on the potentially causative organism, history, and local antibiotic resistance patterns. For severe infections with potential methicillin-resistant S. aureus involvement, treatment should start with linezolid (Zyvox), daptomycin (Cubicin), or vancomycin.30
Puncture Wounds. Serious complications from infected animal or human bites include septic arthritis, osteomyelitis, subcutaneous abscess, tendinitis, and bacteremia.30 Common organisms in domestic animal bite wounds include Pasteurella multocida, S. aureus, Bacteroides tectum, and Fusobacterium, Capnocytophaga, and Porphyromonas species. Human bite wounds may include streptococci, S. aureus, and Eikenella corrodens, in addition to many anaerobes.30 For mild to moderate infections, a five- to 10-day course of oral amoxicillin/clavulanate (Augmentin) is preferred. Doxycycline, tri-methoprim/sulfamethoxazole, or a fluoroquinolone plus clindamycin should be used in patients who are allergic to penicillin.30 For severe infections, parenteral ampicillin/sulbactam (Unasyn), cefoxitin, or ertapenem (Invanz) should be used. Because E. corrodens is resistant to most oral antibiotics, clenched-fist bite wounds should be treated with parenteral ampicillin/sulbactam.30
Burns. Secondary infections from burns may progress rapidly because of loss of epithelial protection. These infections require broad-spectrum antibiotics that are active against gram-positive and gram-negative organisms, including S. aureus, Streptococcus pyogenes, Pseudomonas, Acinetobacter, and Klebsiella. Widespread fungal infection is a rare but serious complication of broad-spectrum antibiotic use in burns. In these cases, systemic antifungals with coverage of Candida, Aspergillus, and Zygomycetes should be considered.28,29,37
When Does a Wound Require Hospitalization or Referral to a Wound Care Specialist?

| Hospitalization |
| Failure of outpatient treatment |
| Necrotizing fasciitis |
| Nonadherence to outpatient therapy |
| Poorly controlled diabetes mellitus or peripheral vascular disease; immunocompromised |
| Severe cellulitis |
| Systemic infection |
| Worsening of wound |
| Referral |
| Severe or circumferential burns, or burns to the face or appendages |
| Wounds affecting joints, bones, tendons, or nerves |
| Wounds to large areas of the body |
| Wounds to the face |
EVIDENCE SUMMARY
Necrotizing fasciitis is a rare but life-threatening infection that may result from traumatic or surgical wounds. Immediate hospitalization for intravenous antibiotics and referral for surgical debridement are required.28
Patients with severe, full-thickness, or circumferential burns, or those that affect the appendages or face should be referred to a burn center, if available. The American Burn Association has created criteria to help determine when referral is recommended (available at https://www.aafp.org/afp/2012/0101/p25.html#afp20120101p25-t4).29
Data Sources: A PubMed search was completed in Clinical Queries using the key terms wound care, laceration, abrasion, burn, puncture wound, bite, treatment, and identification. This search included meta-analyses, randomized controlled trials, clinical trials, and reviews limited to English-language articles about human participants. Also searched were the Cochrane database, Essential Evidence Plus, and the National Guideline Clearinghouse. Search dates: February 1, 2014 to September 19, 2014.