
A more recent article on polyarticular joint pain in adults is available.
Am Fam Physician. 2015;92(1):35-41
Related letter: Diagnostic Tool for Gout Without Need for Joint Aspiration
Author disclosure: No relevant financial affiliations.
Polyarticular arthritis is commonly encountered in clinical settings and has multiple etiologies. The first step is to distinguish between true articular pain and nonarticular or periarticular conditions by recognizing clinical patterns through the history and physical examination. Once pain within a joint or joints is confirmed, the next step is to classify the pain as noninflammatory or inflammatory in origin. Noninflammatory arthritis, which is mostly related to osteoarthritis, has a variable onset and severity and does not have inflammatory features, such as warm or swollen joints. Osteoarthritis usually presents with less than one hour of morning stiffness and pain that is aggravated by activity and improves with rest. A review of systems is usually negative for rashes, oral ulcers, or other internal organ involvement. In contrast, inflammatory arthritis generally causes warm, swollen joints; prolonged morning stiffness; and positive findings on a review of systems. Once inflammatory arthritis is suspected, possible diagnoses are sorted by the pattern of joint involvement, which includes number and type of joints involved, symmetry, and onset. The suspicion for inflammatory arthritis should be confirmed by the appropriate serologic/tissue and/or imaging studies in the clinical setting or in consultation with a subspecialist.
When a patient presents with pain in multiple joints, the pain can originate from the joint (true arthritis); the or bursa; or from psychogenic/metabolic factors, such as depression or hypothyroidism. Once arthritis is suspected, physicians should distinguish between noninflammatory and inflammatory forms of arthritis while recognizing potentially disabling and life-threatening problems.
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Joint swelling, erythema, prolonged morning stiffness (more than one hour), and symmetric pain even at rest are suggestive of inflammatory conditions. | C | 3–6 |
| Noninflammatory and inflammatory conditions can be differentiated with C-reactive protein and erythrocyte sedimentation rate tests; however, in the acute phase, erythrocyte sedimentation rate is less reliable than C-reactive protein. | C | 7, 8 |
| In the diagnosis of gout, a high serum uric acid level has little diagnostic value. The standard of diagnosis is the presence of intracellular monosodium urate crystals on polarized microscopy. | C | 14, 15 |
| Osteoarthritis is noninflammatory; is typically pauciarticular; and often involves the spine and weight-bearing joints, such as the hips and knees. | C | 3–6 |
| Recommendation | Sponsoring organization |
|---|---|
| Do not test antinuclear antibody subserologies without a positive antinuclear antibody test result and clinical suspicion of immune-mediated disease. | American College of Rheumatology |
| Do not test for Lyme disease as a cause of musculoskeletal symptoms without an exposure history and appropriate examination findings. | American College of Rheumatology |
Conditions with polyarthritis are often accompanied by synovitis. On the other hand, conditions that cause pain outside of the joints are considered when there is no apparent joint inflammation. Nearly 50% of patients with polyarticular pain will have unclassifiable conditions; these patients may not need medications and may go into remission within one year.1 However, patients with unclassifiable conditions may benefit from medications for symptomatic relief.
Patient History
The first step in the diagnosis is to determine the onset and timing (acute vs. chronic) of symptoms. Acute symptoms last from hours to two weeks, whereas symptoms are considered chronic after two weeks. The pattern of chronic symptoms should be classified as intermittent or constant (fluctuating from mild, moderate, or severe) to help identify the behavior of the inflammatory process, possible triggers, and concurrent problems.
The pattern of joint involvement is pro-filed by assessing symmetry, and number and types of joints involved. A symmetric pattern affects both sides of the body as opposed to an asymmetric pattern, which has a spotty distribution. Possible conditions are classified based on number of joints affected: pauciarticular pattern (two to four joints) vs. polyarticular pattern (five or more joints). The spondyloarthropathies are classically pauciarticular, whereas rheumatoid arthritis (RA) is usually polyarticular. However, spondyloarthropathies, such as psoriatic arthritis, may also present in a polyarticular manner, whereas RA may initially affect just a few joints.
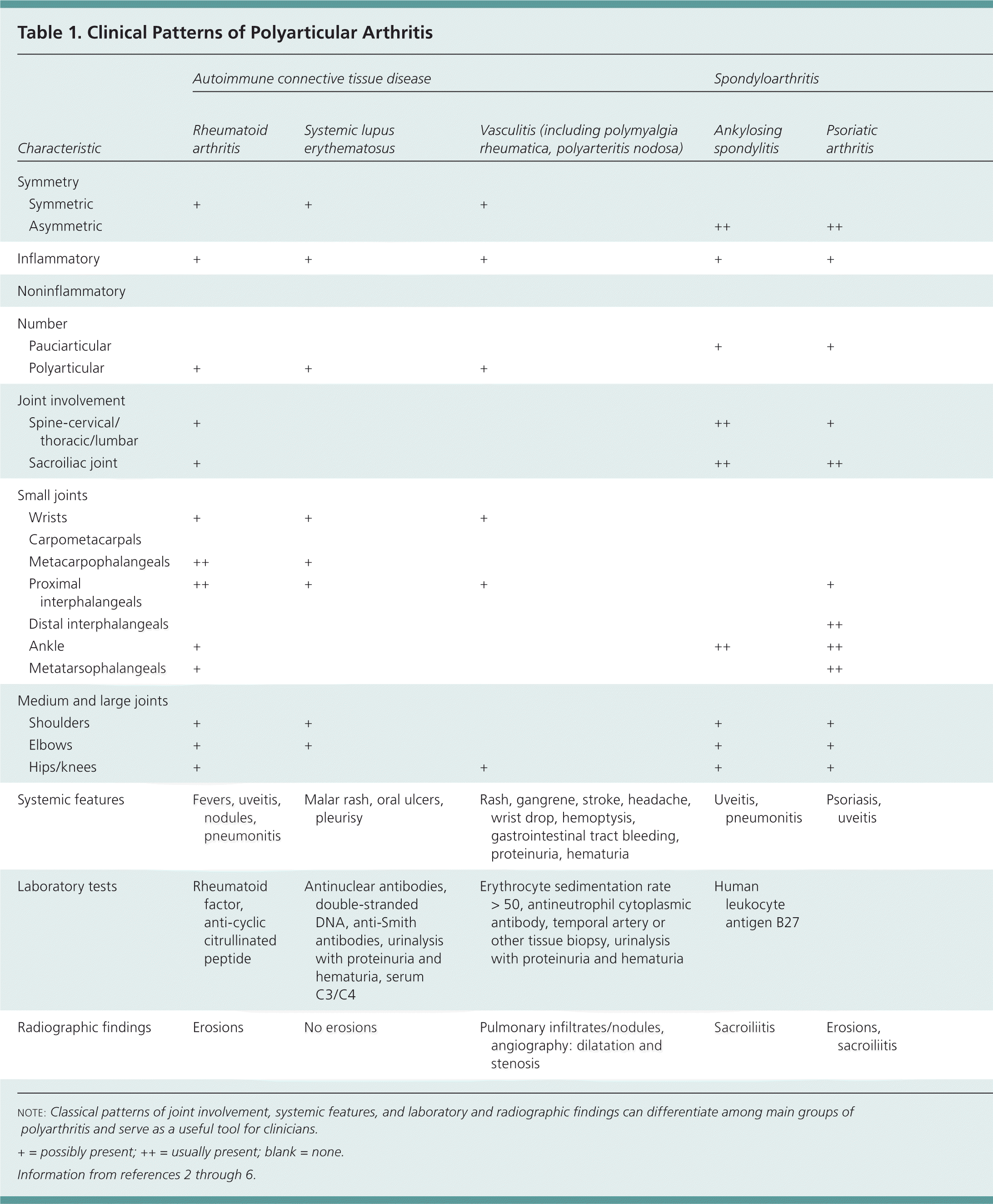
The size and kind of joints involved also provide major diagnostic clues. For instance, spondyloarthropathies often involve the spine, including sacroiliac joints and medium/large joints, such as the shoulders, hips, knees, and ankles. Smaller joint involvement, such as the wrists, fingers, and toes, is more consistent with RA and lupus. Table 1 summarizes clinical patterns that are helpful in the diagnosis of polyarticular arthritis.2–6
| Autoimmune connective tissue disease | Spondyloarthritis | Infectious arthritis | Crystal arthritis | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Characteristic | Rheumatoid arthritis | Systemic lupus erythematosus | Vasculitis (including polymyalgia rheumatica, polyarteritis nodosa) | Ankylosing spondylitis | Psoriatic arthritis | Reactive arthritis | Inflammatory bowel disease arthritis | Bacterial | Viral | Gout | Calcium pyrophosphate deposition disease | Osteoarthritis | |
| Symmetry | |||||||||||||
| Symmetric | + | + | + | + | |||||||||
| Asymmetric | ++ | ++ | + | + | + | + | + | + | |||||
| Inflammatory | + | + | + | + | + | + | + | + | + | + | + | ||
| Noninflammatory | + | ||||||||||||
| Number | |||||||||||||
| Pauciarticular | + | + | + | + | + | + | + | + | |||||
| Polyarticular | + | + | + | + | |||||||||
| Joint involvement | |||||||||||||
| Spine-cervical/thoracic/lumbar | + | ++ | + | + | + | + | + | ||||||
| Sacroiliac joint | + | ++ | ++ | + | + | + | |||||||
| Small joints | |||||||||||||
| Wrists | + | + | + | + | + | ++ | + | ||||||
| Carpometacarpals | ++ | ||||||||||||
| Metacarpophalangeals | ++ | + | + | + | |||||||||
| Proximal interphalangeals | ++ | + | + | + | + | ||||||||
| Distal interphalangeals | ++ | ++ | |||||||||||
| Ankle | + | ++ | ++ | ++ | + | + | + | + | + | ||||
| Metatarsophalangeals | + | ++ | + | + | ++ | + | |||||||
| Medium and large joints | |||||||||||||
| Shoulders | + | + | + | + | + | + | ++ | + | |||||
| Elbows | + | + | + | + | + | + | + | ||||||
| Hips/knees | + | + | + | + | + | + | ++ | ++ | ++ | ||||
| Systemic features | Fevers, uveitis, nodules, pneumonitis | Malar rash, oral ulcers, pleurisy | Rash, gangrene, stroke, headache, wrist drop, hemoptysis, gastrointestinal tract bleeding, proteinuria, hematuria | Uveitis, pneumonitis | Psoriasis, uveitis | Uveitis, urethritis, enteritis | Crohn disease, ulcerative colitis | Fever | Fever, rash | Tophi, uric acid stones | Preexisting osteoarthritis; Wilson disease, ochronosis, hemochromatosis | ||
| Laboratory tests | Rheumatoid factor, anti-cyclic citrullinated peptide | Antinuclear antibodies, double-stranded DNA, anti-Smith antibodies, urinalysis with proteinuria and hematuria, serum C3/C4 | Erythrocyte sedimentation rate > 50, antineutrophil cytoplasmic antibody, temporal artery or other tissue biopsy, urinalysis with proteinuria and hematuria | Human leukocyte antigen B27 | Testing for Chlamydia, Gonorrhea, Salmonella, and Shigella titers | Tissue biopsy | Lyme disease testing, joint/blood culture | Hepatitis B surface antigen, hepatitis C virus antibody, human immunodeficiency virus, human parvovirus B19 | Serum uric acid, uric acid crystals in joint fluid | Calcium pyrophosphate crystals in joint fluid; measurements of thyroid-stimulating hormone, parathyroid hormone, iron, magnesium, or phosphorus | |||
| Radiographic findings | Erosions | No erosions | Pulmonary infiltrates/nodules, angiography: dilatation and stenosis | Sacroiliitis | Erosions, sacroiliitis | Effusions | Erosions, overhanging edges | Chondrocalcinosis | Osteophytes, joint space narrowing | ||||
INFLAMMATORY AND NONINFLAMMATORY ARTHRITIS
Arthritis can be divided into two broad categories: inflammatory and noninflammatory (degenerative arthritis). The presence of joint swelling, erythema, prolonged morning stiffness (more than one hour), and symmetric pain even at rest is suggestive of inflammatory conditions.3–6 On the other hand, weight bearing and movement worsens the pain of noninflammatory arthritis conditions, such as osteoarthritis. Noninflammatory arthritis typically causes less than one hour of morning stiffness. Weight-bearing joints in the lower extremities are likewise more commonly involved in an asymmetric pattern. A symmetric presentation suggests an underlying inflammatory arthritis condition.2
Signs of systemic inflammation include rashes (e.g., psoriasis, photosensitivity), oral and genital ulcerations, Raynaud phenomenon, serositis with pleurisy and pericarditis, sicca symptoms of dry eyes and dry mouth, eye inflammation, bowel inflammation, neurologic symptoms, and ischemic symptoms (including stroke). These signs are integral in correctly diagnosing systemic inflammatory arthropathy.
OTHER CAUSES OF JOINT PAIN
Neurologic causes of pain may be determined by characterization; apart from numbness and burning pain, the pain is unlikely to worsen with joint movement and is likely to worsen at night. Combinations of causes might make characterization of pain difficult. For example, a neurologic cause of pain might be combined with a rheumatologic cause, leading to mixed characteristics.
Extra-articular symptoms can help narrow the diagnostic options. For example, weakness may be a sign of neuromuscular disease, whereas dry mouth, dry eyes, Raynaud phenomenon, pleuritic chest pain, nasal ulcers, oral ulcers, alopecia, adenopathy, or rash might suggest systemic inflammatory rheumatologic conditions. Constitutional symptoms such as weight loss, night sweats, fever, and fatigue are also more common with systemic illnesses.
Patient history, including social history, can provide further insight into the patient's physiologic state. This includes identifying comorbid conditions that might increase the pain burden, such as diabetes mellitus with complications of neuropathy; depression; polypharmacy and use of medications that can cause arthritis, such as in drug-induced lupus arthritis; exposure to ticks that can cause Lyme disease in an endemic area; or exposure to hepatitis C, parvovirus, or human immunodeficiency virus, which can lead to viral arthritis.3 The history should also include surgical procedures, fractures, and trauma. The patient's exercise capabilities or ability to perform activities of daily living should be assessed.
EMERGENT CONDITIONS
In general, emergent conditions involving the joints present acutely and should be recognized promptly. Septic arthritis typically involves a large joint such as the knee,3 but can affect several joints and is accompanied by malaise, weight loss, fever, and swollen and/or warm joints.3 Other conditions include neuropathies, radiculopathies, or myelopathies, which cause numbness or a burning pain, (e.g., cauda equina syndrome); compartment syndrome, with joint pain exceeding what would be expected based on physical examination findings; and sepsis or infection.
Physical Examination
The presence of the cardinal signs of inflammation on physical examination, such as erythema, warmth, swelling, and tenderness, confirms inflammatory arthritis.3,4 Noninflammatory arthritis may also present with swelling and tenderness, but does not cause erythema or warmth. Periarthritis in the contiguous structures, such as the tendons, ligaments, and bursa, should also be differentiated using physical examination findings. Nonarticular conditions, such as muscular injuries, tendinitis, or bursitis, present with a normal passive range of motion and reduced active range of motion, with the latter usually caused by pain. On the other hand, joint abnormalities, synovitis, and soft tissue contractures (e.g., frozen shoulder) present with reduced passive and active range of motion. Increased pain with active or resisted range of motion also suggests processes that involve the muscles, tendons, and bursa. During evaluation of range of motion, crepitation without warmth or erythema suggests a degenerative process, such as osteoarthritis.
Systemic autoimmune diseases are associated with organ system involvement in addition to arthritis. For instance, fine inspiratory rales suggest interstitial lung disease, a complication of RA; pleuropericardial friction rubs occur with lupus; and parotid gland enlargement accompanies Sjögren syndrome.3 Mucocutaneous disorders, sarcoidosis, cancer, pseudogout, gout, podagra, systemic lupus erythematosus (SLE), vasculitis, Still disease, post–enteric infection reactive arthritis, and infectious arthritis may all present with fever.3
Once the history and physical examination are complete, the clinician can usually establish whether the pain is truly articular and whether the condition is inflammatory or noninflammatory. Further management should be directed toward refining the specific arthritis diagnosis, instituting therapy, and possibly facilitating subspecialty consultations (i.e., orthopedic surgery, rehabilitation, neurology, or rheumatology). Rheumatology consultation may be appropriate even for nonclassifiable conditions because seronegative inflammatory arthritis is fairly common, and identifying these conditions in the primary care setting may be challenging.
Laboratory Tests
ANTINUCLEAR ANTIBODY
SLE without antinuclear antibodies comprises less than 2% of cases; therefore, SLE is unlikely in a patient with polyarthritis who tests negative for the antibodies. Conversely, many rheumatic conditions can be associated with antinuclear antibodies; therefore, a positive test result does not always correlate with SLE, especially in a patient who lacks other specific clinical criteria.2,3 The higher the titer of antinuclear antibodies, the greater the chance of autoimmune disease. A diagnosis of SLE becomes more likely when a high ANA titer is accompanied by more specific autoantibodies for lupus, such as anti–double-stranded DNA and anti-Smith antibodies. Sjögren syndrome may be present with any autoimmune illness, or it may be the primary diagnosis with dry eyes, dry mouth, and titers positive for anti–Sjögren syndrome A and B antibodies.3
ERYTHROCYTE SEDIMENTATION RATE AND C-REACTIVE PROTEIN
Noninflammatory and inflammatory conditions can be differentiated using C-reactive protein and erythrocyte sedimentation rate (ESR) tests, which are nonspecific for inflammation.7 Rheumatic, malignant, and infectious conditions, and allergic reactions might cause these levels to be elevated; therefore, these tests are not diagnostic.7 Because abnormal red cells might affect the ESR, it is less reliable in the acute phase than the C-reactive protein test.8,9 Other noninflammatory conditions, including dysproteinemia, hyperlipoproteinemia, diabetes, and kidney problems, can lead to an elevated ESR and should be considered.7 The ESR level varies between men and women, and increases with age. The normal upper limit for ESR is calculated as age plus 10 divided by two for women, and age divided by two for men.
A normal ESR also does not preclude rheumatic disease. In one series, 3% of patients with RA had normal ESR findings.10 However, when clinical presentation and physical examination findings point to a specific diagnosis, an ESR result that is compatible with that diagnosis may help support an inflammatory diagnosis. For example, a markedly increased ESR in an older individual with shoulder and hip pain might lead to a diagnosis of polymyalgia rheumatica; however, the diagnosis should not be discounted entirely if the ESR is within normal limits.
RHEUMATOID FACTOR AND ANTI–CITRULLINATED PEPTIDE ANTIBODIES
Anti–citrullinated peptide antibody levels are more specific for RA and correlate with erosive disease. Rheumatoid factor is a nonspecific immunoglobulin that is also detected in chronic infections, such as hepatitis C, tuberculosis, and infective endocarditis, and in autoimmune disorders such as paraproteinemias, vasculitis, or SLE and should prompt consideration for these entities in the absence of a typical RA joint pattern.11,12 The diagnostic value of rheumatoid factor testing may be limited by its specificity; however, it should be used when signs and symptoms of inflammatory arthritis are present. In the clinical setting of symmetric polyarthritis, a high rheumatoid factor titer is associated with poor outcomes and high predictive value for diagnosing RA.13
SERUM URIC ACID
A high serum uric acid level is commonly seen in the general population and is not diagnostic of gout.14 Gout is diagnosed by aspiration of joint fluid and demonstration of intracellular monosodium urate crystals on polarized microscopy. In most patients with gout, serum uric acid levels are elevated in the intercurrent period.15 During a gout attack, the serum uric acid level may be normal or even low, and is best measured during the intercurrent period and every three to six months to monitor response to uric acid–lowering therapy with a goal of keeping levels below 6 mg per dL (357 μmol per L).14,15
SYNOVIAL FLUID TESTS
Crystal-induced synovitis and bacterial infections should be confirmed by joint aspiration and synovial fluid tests for Gram stain and culture, cell count, and crystals. Febrile patients with a joint effusion should be treated for septic arthritis until it can be ruled out.3,16 Superimposed septic arthritis should be ruled out in patients with known arthritis who present with fever. Synovial fluid is considered noninflammatory if the white blood cell count is less than 2,000 per mm3 (2.0 × 109 per L), typically with less than 75% polymorphonuclear leukocytes. Infection is confirmed and best treated with a positive Gram stain with confirmed growth of bacteria or other pathogen on culture. Gout is confirmed by findings of intracellular negatively birefringent crystals on polarized microscopy, whereas pseudogout or calcium deposition disease is con-firmed with positively birefringent crystals.17
TESTS FOR INFECTION
Testing for the presence of Borrelia burgdorferi, hepatitis B, hepatitis C, or parvovirus antibodies can lead to the diagnosis and specific treatment. It must be noted that parvovirus immunoglobulin M (IgM) must be present to indicate acute infection; IgG indicates past exposure. However, these tests should be ordered only when there is clinical suspicion and not routinely. These tests are expensive, are unnecessary unless clinically indicated, and can result in high false-positive rates.18
Imaging
Polyarticular arthropathies require imaging if the clinician is looking for concurrent fracture, erosions, osteoarthritis, or osteomyelitis. The best approach is to evaluate the joints that are commonly affected by specific conditions. For example, radiographs of the feet, hands/wrists, and cervical spine will provide changes most useful for the diagnosis of RA by demonstrating erosions in the metatarsophalangeal, wrist, and metacarpal joints, or C1-C2 articulations suggestive of atlantoaxial instability.19
In new-onset bursitis, tendinitis, gout, SLE, or RA, radiography may not be helpful because of limited diagnostic specificity. In seronegative spondyloarthropathy, such as ankylosing spondylitis, sacroiliac joint radiographs can show early abnormalities best confirmed by magnetic resonance imaging.19,20
Small erosions are more visible on ultrasonography or magnetic resonance imaging.19 Erosions associated with RA do not have the overhanging edge caused by repair changes that may be seen on imaging in chronic gout.3 When calcified, tophaceous deposits are easily visible on radiographs. If not, an arc of crystals on the cartilaginous surface may be seen more easily on ultrasonography.21 Paget disease, infection, malignancy, and disease involving the sacroiliac and hip joints are sometimes diagnosed more easily through imaging with specific procedures or radionuclide scans.2
Biopsy
Tissue biopsies are essential for diagnosing giant cell arteritis (temporal artery biopsy), cutaneous lupus or skin vasculitis (skin biopsy), glomerulonephritis (kidney biopsy), and pulmonary vasculitis (lung biopsy). A synovial biopsy may help in elusive cases, such as granulomatous diseases (e.g., sarcoidosis, fungal infection, tuberculosis), hemochromatosis, Whipple disease, and rheumatoid nodules.2
Data Sources: A PubMed search was completed in Clinical Queries. using the key terms polyarticular, arthritis, polyarthritis, joint pain, and joint inflammation. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. Also searched were the Cochrane database, Essential Evidence Plus, UpToDate, and DynaMed. Search dates: December 2013 through March 2014.
