
Am Fam Physician. 2015;92(5):358-365
Patient information: See related handout on food poisoning, written by the authors of this article.
Author disclosure: No relevant financial affiliations.
The Centers for Disease Control and Prevention estimates that each year, one in six Americans will experience a foodborne illness. The most common causes in the United States are viruses, such as norovirus; bacteria, such as Salmonella, Escherichia coli, Campylobacter, and Listeria; and parasites, such as Toxoplasma gondii and Giardia. Resources are available to educate consumers on food recalls and proper handling, storage, and cooking of foods. Diagnosis and management of a foodborne illness are based on the history and physical examination. Common symptoms of foodborne illnesses include vomiting, diarrhea (with or without blood), fever, abdominal cramping, headache, dehydration, myalgia, and arthralgias. Definitive diagnosis can be made only through stool culture or more advanced laboratory testing. However, these results should not delay empiric treatment if a foodborne illness is suspected. Empiric treatment should focus on symptom management, rehydration if the patient is clinically dehydrated, and antibiotic therapy. Foodborne illnesses should be reported to local and state health agencies; reporting requirements vary among states.
Foodborne illness can be caused by a multitude of microorganisms such as viruses, bacteria, and parasites. Foodborne illness is a worldwide problem, and U.S. outbreaks often garner media attention and result in food recalls. Foodborne illnesses are becoming a greater challenge because of new and emerging microorganisms and toxins, the growth of antibiotic resistance, increasing food contamination caused by new environments and methods of food production, and an increase in multistate outbreaks.1 There are more than 250 identified pathogens that cause foodborne illness. The Centers for Disease Control and Prevention (CDC) estimates that one in six Americans (approximately 48 million) will become sick from a foodborne pathogen each year, resulting in 128,000 hospitalizations and 3,000 deaths.2 Most foodborne illnesses, hospitalizations, and deaths are caused by one of eight common pathogens: norovirus, nontyphoidal Salmonella, Clostridium perfringens, Campylobacter, Staphylococcus aureus, Toxoplasma gondii, Listeria monocytogenes, and Shiga toxin–producing Escherichia coli2 (Table 13). E. coli is commonly divided into two broad types, Shiga toxin–producing—of which E. coli O157:H7 is the best studied—and non-Shiga toxin–producing, which includes enteropathogenic, enteroinvasive, enteroaggregative, and diffusely adherent E. coli. New pathogens emerge constantly, whereas others decrease in significance or disappear altogether. Predicting the emergence or disappearance of specific pathogens—other than in the setting of an identified outbreak—is difficult and has not significantly prevented or limited foodborne illnesses.
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Stool cultures are the diagnostic standard for bacterial foodborne illness; however, culture results are positive in less than 40% of cases. | C | 4, 5 |
| A single dose of ondansetron (Zofran) is recommended in children with clinically significant gastroenteritis-related vomiting. | A | 12–14 |
| Oral rehydration therapy is effective in preventing and treating dehydration in patients of all ages. | A | 16–19 |
| Empiric antibiotic therapy should be considered in cases of suspected foodborne illness if the patient is febrile and has signs of invasive disease, if symptoms have persisted for more than one week or are severe, or if hospitalization may be required. | C | 10, 16, 17, 19 |
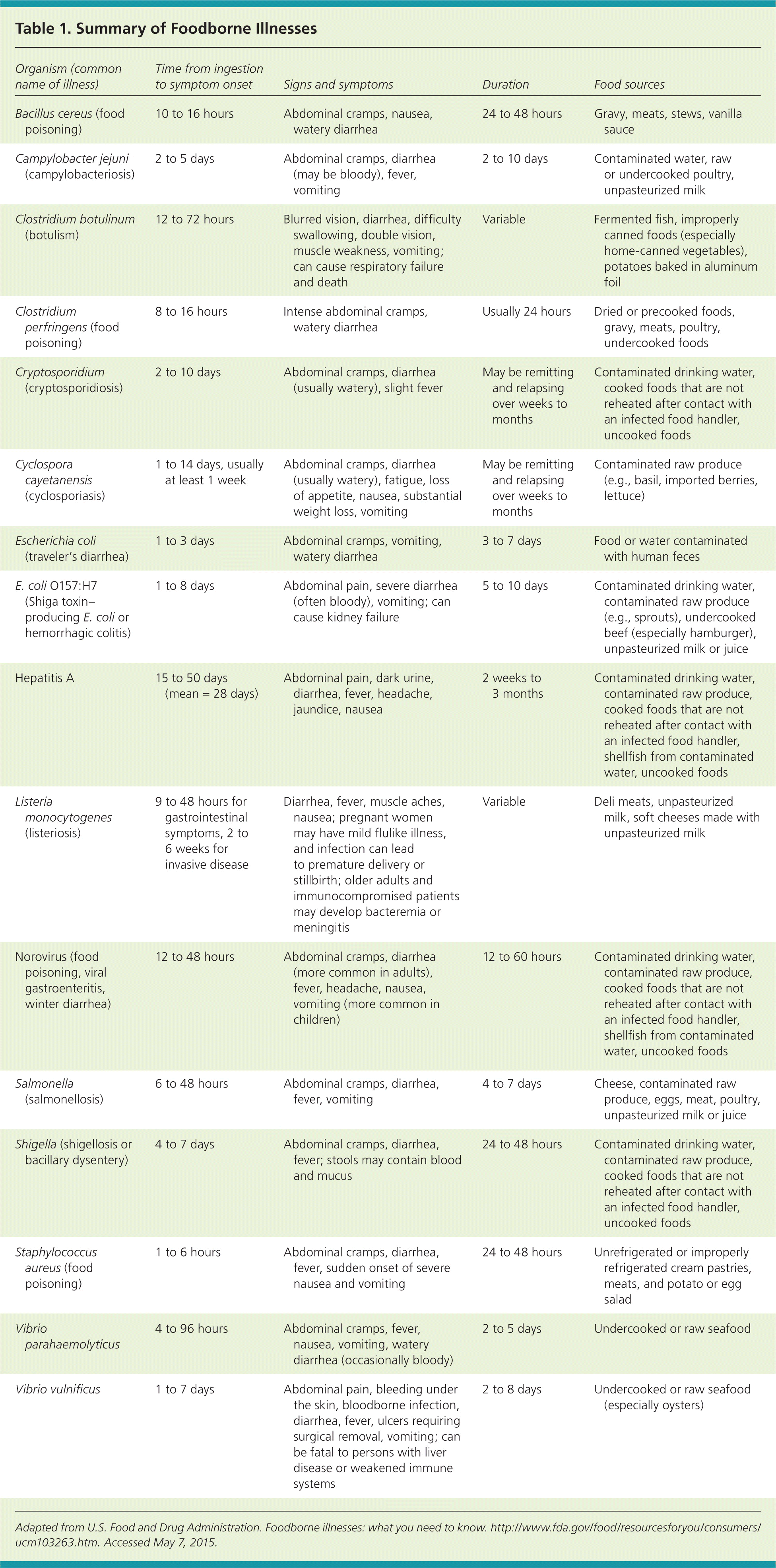
| Organism (common name of illness) | Time from ingestion to symptom onset | Signs and symptoms | Duration | Food sources |
|---|---|---|---|---|
| Bacillus cereus (food poisoning) | 10 to 16 hours | Abdominal cramps, nausea, watery diarrhea | 24 to 48 hours | Gravy, meats, stews, vanilla sauce |
| Campylobacter jejuni (campylobacteriosis) | 2 to 5 days | Abdominal cramps, diarrhea (may be bloody), fever, vomiting | 2 to 10 days | Contaminated water, raw or undercooked poultry, unpasteurized milk |
| Clostridium botulinum (botulism) | 12 to 72 hours | Blurred vision, diarrhea, difficulty swallowing, double vision, muscle weakness, vomiting; can cause respiratory failure and death | Variable | Fermented fish, improperly canned foods (especially home-canned vegetables), potatoes baked in aluminum foil |
| Clostridium perfringens (food poisoning) | 8 to 16 hours | Intense abdominal cramps, watery diarrhea | Usually 24 hours | Dried or precooked foods, gravy, meats, poultry, undercooked foods |
| Cryptosporidium (cryptosporidiosis) | 2 to 10 days | Abdominal cramps, diarrhea (usually watery), slight fever | May be remitting and relapsing over weeks to months | Contaminated drinking water, cooked foods that are not reheated after contact with an infected food handler, uncooked foods |
| Cyclospora cayetanensis (cyclosporiasis) | 1 to 14 days, usually at least 1 week | Abdominal cramps, diarrhea (usually watery), fatigue, loss of appetite, nausea, substantial weight loss, vomiting | May be remitting and relapsing over weeks to months | Contaminated raw produce (e.g., basil, imported berries, lettuce) |
| Escherichia coli (traveler's diarrhea) | 1 to 3 days | Abdominal cramps, vomiting, watery diarrhea | 3 to 7 days | Food or water contaminated with human feces |
| E. coli O157:H7 (Shiga toxin–producing E. coli or hemorrhagic colitis) | 1 to 8 days | Abdominal pain, severe diarrhea (often bloody), vomiting; can cause kidney failure | 5 to 10 days | Contaminated drinking water, contaminated raw produce (e.g., sprouts), undercooked beef (especially hamburger), unpasteurized milk or juice |
| Hepatitis A | 15 to 50 days (mean = 28 days) | Abdominal pain, dark urine, diarrhea, fever, headache, jaundice, nausea | 2 weeks to 3 months | Contaminated drinking water, contaminated raw produce, cooked foods that are not reheated after contact with an infected food handler, shellfish from contaminated water, uncooked foods |
| Listeria monocytogenes (listeriosis) | 9 to 48 hours for gastrointestinal symptoms, 2 to 6 weeks for invasive disease | Diarrhea, fever, muscle aches, nausea; pregnant women may have mild flulike illness, and infection can lead to premature delivery or stillbirth; older adults and immunocompromised patients may develop bacteremia or meningitis | Variable | Deli meats, unpasteurized milk, soft cheeses made with unpasteurized milk |
| Norovirus (food poisoning, viral gastroenteritis, winter diarrhea) | 12 to 48 hours | Abdominal cramps, diarrhea (more common in adults), fever, headache, nausea, vomiting (more common in children) | 12 to 60 hours | Contaminated drinking water, contaminated raw produce, cooked foods that are not reheated after contact with an infected food handler, shellfish from contaminated water, uncooked foods |
| Salmonella (salmonellosis) | 6 to 48 hours | Abdominal cramps, diarrhea, fever, vomiting | 4 to 7 days | Cheese, contaminated raw produce, eggs, meat, poultry, unpasteurized milk or juice |
| Shigella (shigellosis or bacillary dysentery) | 4 to 7 days | Abdominal cramps, diarrhea, fever; stools may contain blood and mucus | 24 to 48 hours | Contaminated drinking water, contaminated raw produce, cooked foods that are not reheated after contact with an infected food handler, uncooked foods |
| Staphylococcus aureus (food poisoning) | 1 to 6 hours | Abdominal cramps, diarrhea, fever, sudden onset of severe nausea and vomiting | 24 to 48 hours | Unrefrigerated or improperly refrigerated cream pastries, meats, and potato or egg salad |
| Vibrio parahaemolyticus | 4 to 96 hours | Abdominal cramps, fever, nausea, vomiting, watery diarrhea (occasionally bloody) | 2 to 5 days | Undercooked or raw seafood |
| Vibrio vulnificus | 1 to 7 days | Abdominal pain, bleeding under the skin, bloodborne infection, diarrhea, fever, ulcers requiring surgical removal, vomiting; can be fatal to persons with liver disease or weakened immune systems | 2 to 8 days | Undercooked or raw seafood (especially oysters) |
Prevention
Prevention is the first step in combatting foodborne illnesses. Consumer information on food safety is available from the CDC at http://www.cdc.gov/foodsafety/facts.html or from the U.S. Food and Drug Administration at http://www.fda.gov/Food/FoodborneIllnessContaminants/FoodborneIllnessesNeedToKnow/default.htm or http://www.foodsafety.gov, or by calling (888) SAFEFOOD ([888] 723–3366). Guidelines for safely handling and preparing food should be followed regardless of the setting in which food is consumed. Although these recommendations have been shown to reduce the risk of foodborne illness in the United States, the risk increases with travel.
Diagnosis
HISTORY
Foodborne illness can have various presentations, ranging from clinically mild illness that requires only outpatient care to severe illness that requires hospitalization. Most foodborne illnesses are associated with vomiting or diarrhea (more than three loose stools in 24 hours). Other common symptoms include fever, bloody diarrhea, abdominal cramping, headache, dehydration, myalgia, and arthralgias.4 Patients may have several symptoms or only one. The history is the most important step in evaluating a patient with diarrheal illness (Table 2).5

| Findings from patient history | Comment |
|---|---|
| Acute abdominal pain, fever, and vomiting | Together, these symptoms raise suspicion for infectious diarrhea |
| Dietary factors | Recent changes in diet and ingestion of foods included in recent recalls or undercooked foods should raise suspicion for foodborne illness |
| Duration of symptoms | Longer duration raises concern for dehydration |
| Employment history | Persons who work at child care centers or in close contact with others are at risk of viral diarrhea |
| Exposure to other persons with diarrhea | Cross-contamination and transmission of pathogens are possible; may help narrow differential if cause is known in the other person |
| Hospitalization or nursing home admission | Raises suspicion for Clostridium difficile infection |
| Immunocompromise | Raises suspicion for atypical causes of diarrhea |
| Medical history | Can help determine possible comorbidities that suggest a cause |
| Recent antibiotic use | Raises suspicion for C. difficile infection |
| Stool characteristics (bloody, foul smelling, watery) | Bloody diarrhea raises suspicion for Salmonella, Shigella, or enterohemorrhagic Escherichia coli infection (or mesenteric ischemia in at-risk populations) |
| Foul-smelling stools in patients with recent hospitalization or antibiotic use raise suspicion for C. difficile or Giardia infection | |
| Watery stools raise suspicion for viral cause or Giardia infection | |
| Travel history | Travel to foreign countries, especially non-Western countries, should raise suspicion for infectious diarrhea |
None of the symptoms of foodborne illness is specific, so the clinician must consider the history, epidemiologic features, and objective findings to make an accurate diagnosis. Symptoms and time of onset can narrow the differential diagnosis (Table 3) and help identify a likely pathogen.4 Early onset of vomiting and diarrhea results from ingestion of preformed toxins, most often S. aureus or Bacillus cereus. Diarrhea within 24 hours of ingestion is most likely caused by C. perfringens or B. cereus. Diarrhea within 24 to 48 hours of ingestion is most often caused by Campylobacter jejuni in individual cases or Salmonella in outbreaks.4 Foodborne illnesses commonly associated with fever are caused by Vibrio cholerae non-O1, Shigella, and C. jejuni (Table 4). Enterotoxins in the small bowel caused by E. coli, C. perfringens, and viruses produce excessive secretions of fluids and electrolytes that overwhelm the large bowel; therefore, they are typically associated with watery diarrhea. Bloody diarrhea with abdominal pain should prompt consideration of inflammatory damage to the intestinal mucosa or an infection (e.g., C. jejuni, Salmonella enteritidis, enteroinvasive E. coli) affecting the large bowel.
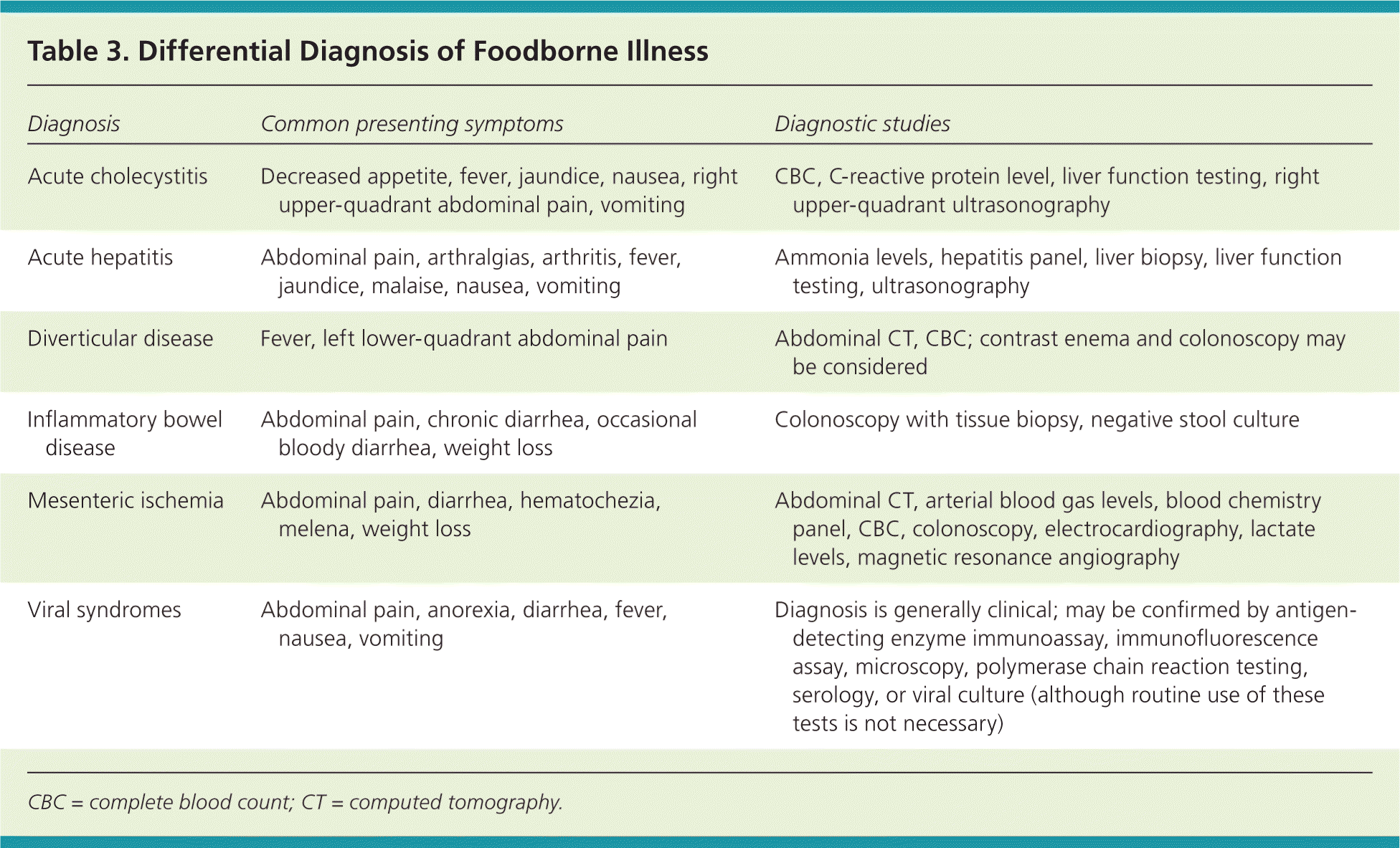
| Diagnosis | Common presenting symptoms | Diagnostic studies |
|---|---|---|
| Acute cholecystitis | Decreased appetite, fever, jaundice, nausea, right upper-quadrant abdominal pain, vomiting | CBC, C-reactive protein level, liver function testing, right upper-quadrant ultrasonography |
| Acute hepatitis | Abdominal pain, arthralgias, arthritis, fever, jaundice, malaise, nausea, vomiting | Ammonia levels, hepatitis panel, liver biopsy, liver function testing, ultrasonography |
| Diverticular disease | Fever, left lower-quadrant abdominal pain | Abdominal CT, CBC; contrast enema and colonoscopy may be considered |
| Inflammatory bowel disease | Abdominal pain, chronic diarrhea, occasional bloody diarrhea, weight loss | Colonoscopy with tissue biopsy, negative stool culture |
| Mesenteric ischemia | Abdominal pain, diarrhea, hematochezia, melena, weight loss | Abdominal CT, arterial blood gas levels, blood chemistry panel, CBC, colonoscopy, electrocardiography, lactate levels, magnetic resonance angiography |
| Viral syndromes | Abdominal pain, anorexia, diarrhea, fever, nausea, vomiting | Diagnosis is generally clinical; may be confirmed by antigen-detecting enzyme immunoassay, immunofluorescence assay, microscopy, polymerase chain reaction testing, serology, or viral culture (although routine use of these tests is not necessary) |

| Fever | |
| Characteristically associated | |
| Campylobacter jejuni | |
| Shigella | |
| Vibrio cholerae non-O1 | |
| Often associated | |
| Norwalk virus | |
| Salmonella | |
| Vibrio parahaemolyticus | |
| Vomiting | |
| Characteristically associated | |
| Bacillus cereus (emetic syndrome) | |
| Norwalk virus | |
| Staphylococcus aureus | |
| Often associated | |
| Clostridium botulinum | |
| V. cholerae O1 | |
| V. parahaemolyticus | |
PHYSICAL EXAMINATION
The physical examination can help narrow the differential diagnosis, and vital signs can help determine the severity of volume depletion. Orthostatic pulse and blood pressure changes should be noted, and a basic general physical examination should be performed, with assessment of skin turgor, the abdomen, mucous membranes, and mental status.5
ANCILLARY TESTING
Watchful waiting is often the most appropriate option in the initial diagnosis and management of foodborne illness; ancillary testing is usually not necessary. If testing is performed, stool culture can provide a definitive diagnosis of infectious diarrhea and is useful for outbreak identification. In most outpatients who have self-limiting gastroenteritis, a stool culture does not affect management.4 Bacteria are the most common cause of non–self-limiting foodborne illness; however, stool cultures are positive in less than 40% of cases.4,5 Newer techniques such as polymerase chain reaction testing have become readily available and provide more rapid, reliable determination of specific pathogens. An organism-specific diagnosis can help clinicians to narrow treatment recommendations, aid public health professionals, and prevent unnecessary procedures.
Other tests that can be considered include serum chemistry (including albumin levels), C-reactive protein levels, complete blood count, blood cultures, urinalysis, abdominal radiography, anoscopy, and endoscopy, if warranted by the severity and pattern of symptoms.5 In severe cases of infectious diarrhea, toxic megacolon should be considered, which can be identified on plain abdominal radiography.4 Severe inflammatory changes can also be seen on computed tomography. It may be reasonable to obtain blood cultures in patients with fever and diarrhea (with or without blood), because up to 1% of cases of nontyphoidal Salmonella infections are associated with bacteremia.4,5 Sigmoidoscopy or colonoscopy may be useful in hospitalized patients with bloody diarrhea to obtain tissue and histology, which could aid in the diagnosis.
Stool microscopy is rarely diagnostic, but the presence of red and white blood cells may signal a colonic source.4 Its primary use is identification of ova, cysts, and parasites, although antigen testing is more sensitive and specific for Giardia. Microscopic evaluation for fecal polymorphonuclear leukocytes or lactoferrin measurements may be useful if an inflammatory etiology is suspected. A positive stool culture is more likely when analysis indicates an inflammatory process. Compared with leukocyte examinations, lactoferrin measurements are more sensitive but more expensive, have a higher false-positive rate, and require a fresh-cup sample examined by an experienced microscopist.5
Management
SYMPTOMATIC TREATMENT
Use of antidiarrheal medications, including antimotility agents, anticholinergics, and adsorbents, is not recommended in children, especially those younger than two years, and is discouraged if infection with Shiga toxin–producing E. coli is suspected.6–8 Symptomatic treatment with loperamide (Imodium) and bismuth subsalicylate (Pepto-Bismol) is effective and may be considered in adults with uncomplicated acute or traveler's diarrhea.9–11 Although loperamide is more effective than bismuth subsalicylate, it is not recommended for patients with hematochezia and systemic symptoms because it may increase the risk of invasive disease.10
In patients with clinically significant vomiting, antiemetics can alleviate symptoms and reduce the need for hospitalization and intravenous fluid administration. Multiple studies support the use of a single dose of ondansetron (Zofran) in children with gastroenteritis-related vomiting.12–14 The use of antiemetics in adults with gastroenteritis is reasonable, but data about adverse effects are lacking.
DEHYDRATION
Many physicians are reluctant to use oral rehydration therapy, despite its proven effectiveness in the management of diarrhea-associated dehydration.6,15 It has been proven to prevent and treat dehydration in patients of all ages.5,16–19 Guidelines that recommend the use of oral rehydration therapy for mild to moderate dehydration in infants and children have been published by the World Health Organization, the American Academy of Pediatrics, and the CDC.6,7,20 Oral rehydration solutions contain a blend of electrolytes, as well as carbohydrates. Sports drinks and soft drinks have a high carbohydrate-to-sodium ratio and total osmolality, and can exacerbate diarrhea.19
Clinical assessment should be used to guide rehydration therapy. Children—especially infants—are predisposed to dehydration and require more diligence in determining hydration status. CDC guidelines recommend the initial use of oral rehydration therapy with replacement of continuing fluid losses in children with mild to moderate dehydration. Children with severe dehydration should be hospitalized and given intravenous fluids.6,7 When oral rehydration therapy or intravenous fluid administration is used in infants, care should be taken to minimize interruptions in breastfeeding or formula feeding.6,7
EMPIRIC ANTIBIOTICS
Most cases of acute infectious diarrhea are viral, and improper use of empiric antibiotics is associated with increased morbidity caused by adverse effects and Clostridium difficile colitis. Empiric antibiotics should be considered in cases of suspected foodborne illness only if the patient is febrile and has signs of invasive disease (e.g., gross hematochezia, leukocytes on fecal smear), if symptoms have persisted for more than one week or are severe (i.e., more than eight liquid stools per day), or if hospitalization may be required.10,16,17,19 A fluoroquinolone (or trimethoprim/sulfamethoxazole in children) is generally recommended for empiric antibiotic therapy.5 Stool testing should still be performed.
Empiric antibiotic therapy decreases the duration of symptoms in patients with traveler's diarrhea.5,9 Enterotoxigenic E. coli is the most common cause of traveler's diarrhea worldwide and is generally susceptible to ciprofloxacin, but azithromycin (Zithromax) is equally effective and a better choice in areas where fluoroquinolone-resistant C. jejuni is present.9,21 Patients with diarrhea of more than 10 days' duration that is associated with fatty or foul-smelling stools, cramps, bloating, and weight loss can be treated empirically for Giardia infection.22 Because of an increased risk of hemolytic uremic syndrome, patients receiving empiric antibiotic therapy should be monitored closely if Shiga toxin–producing E. coli infection is suspected.4,23
TARGETED ANTIBIOTICS
If empiric treatment has not been initiated, antibiotic therapy may be indicated once stool culture, bacterial toxin, or microscopy results are available. Antibiotic therapy can shorten the duration of symptoms and may prevent bacteremia in older adults, newborns, and immunocompromised patients.4 Recommended treatment regimens for foodborne pathogens are outlined in Table 5.8,18,19,21–24 Ciprofloxacin is no longer recommended for treatment of Campylobacter infection; a macrolide, such as erythromycin, is recommended instead.24
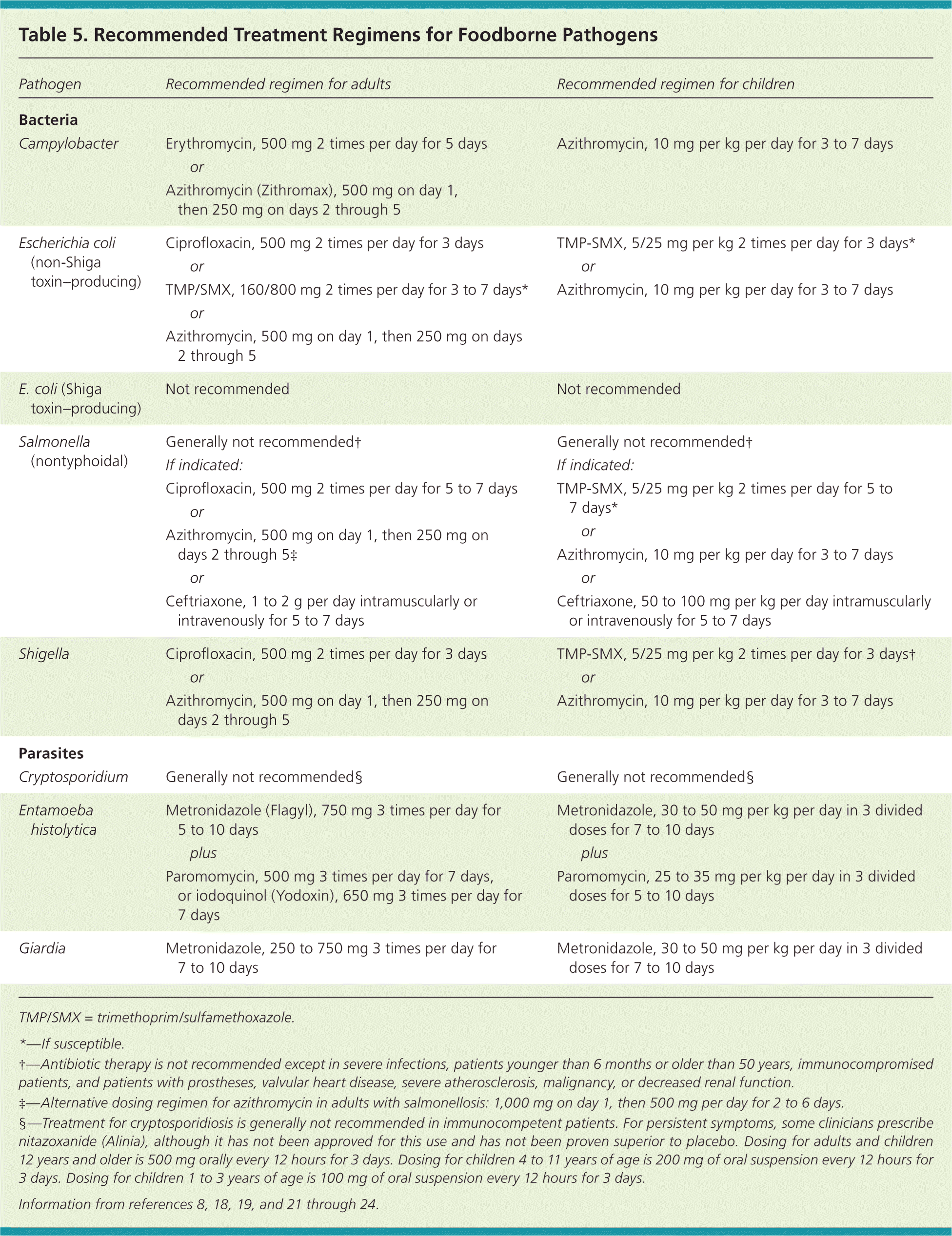
| Pathogen | Recommended regimen for adults | Recommended regimen for children | ||
|---|---|---|---|---|
| Bacteria | ||||
| Campylobacter | Erythromycin, 500 mg 2 times per day for 5 days | Azithromycin, 10 mg per kg per day for 3 to 7 days | ||
| or | ||||
| Azithromycin (Zithromax), 500 mg on day 1, then 250 mg on days 2 through 5 | ||||
| Escherichia coli (non-Shiga toxin–producing) | Ciprofloxacin, 500 mg 2 times per day for 3 days | TMP-SMX, 5/25 mg per kg 2 times per day for 3 days* | ||
| or | or | |||
| TMP/SMX, 160/800 mg 2 times per day for 3 to 7 days* | Azithromycin, 10 mg per kg per day for 3 to 7 days | |||
| or | ||||
| Azithromycin, 500 mg on day 1, then 250 mg on days 2 through 5 | ||||
| E. coli (Shiga toxin–producing) | Not recommended | Not recommended | ||
| Salmonella (nontyphoidal) | Generally not recommended† | Generally not recommended† | ||
| If indicated: | If indicated: | |||
| Ciprofloxacin, 500 mg 2 times per day for 5 to 7 days | TMP-SMX, 5/25 mg per kg 2 times per day for 5 to 7 days* | |||
| or | or | |||
| Azithromycin, 500 mg on day 1, then 250 mg on days 2 through 5‡ | Azithromycin, 10 mg per kg per day for 3 to 7 days | |||
| or | or | |||
| Ceftriaxone, 1 to 2 g per day intramuscularly or intravenously for 5 to 7 days | Ceftriaxone, 50 to 100 mg per kg per day intramuscularly or intravenously for 5 to 7 days | |||
| Shigella | Ciprofloxacin, 500 mg 2 times per day for 3 days | TMP-SMX, 5/25 mg per kg 2 times per day for 3 days† | ||
| or | or | |||
| Azithromycin, 500 mg on day 1, then 250 mg on days 2 through 5 | Azithromycin, 10 mg per kg per day for 3 to 7 days | |||
| Parasites | ||||
| Cryptosporidium | Generally not recommended§ | Generally not recommended§ | ||
| Entamoeba histolytica | Metronidazole (Flagyl), 750 mg 3 times per day for 5 to 10 days | Metronidazole, 30 to 50 mg per kg per day in 3 divided doses for 7 to 10 days | ||
| plus | plus | |||
| Paromomycin, 500 mg 3 times per day for 7 days, or iodoquinol (Yodoxin), 650 mg 3 times per day for 7 days | Paromomycin, 25 to 35 mg per kg per day in 3 divided doses for 5 to 10 days | |||
| Giardia | Metronidazole, 250 to 750 mg 3 times per day for 7 to 10 days | Metronidazole, 30 to 50 mg per kg per day in 3 divided doses for 7 to 10 days | ||
Outbreak Surveillance and Reporting
Although reporting requirements vary, most states require physicians to report cases of hepatitis A and botulism, and Salmonella, Shiga toxin–producing E. coli, Listeria, Shigella, and Vibrio infections. A definitive diagnosis is not necessary to report a suspected foodborne illness. Outbreaks can be declared by local, county, state, or national agencies; reporting outbreaks to the CDC is left to the discretion of the agency. Physicians should avoid attributing cases of foodborne illness to specific food sources without definitive testing and reporting. In cases of suspected foodborne illness or in the setting of an outbreak, stool and vomitus samples should be sent for testing. All reports of outbreaks are entered into the CDC's Foodborne Disease Outbreak Surveillance System, after which the data are analyzed to monitor and identify the root cause of the outbreak. Once an outbreak has occurred, prevention strategies should focus on educating the public through the news media and correcting the underlying cause, such as through food product recalls. Information on outbreaks, outbreak surveillance, and identified trends can be found at http://www.cdc.gov/foodsafety/fdoss/index.html or by calling the CDC at (800) CDC-INFO ([800] 232–4636).
Data Sources: A PubMed search was completed using the key terms foodborne illness, infectious diarrhea, food poisoning, salmonella, Shigella, Escherichia coli, Campylobacter, food safety, hemolyticuremic syndrome, oral rehydration solution, oral rehydration therapy, traveler's diarrhea, and bloody diarrhea. We also searched Essential Evidence Plus, UpToDate, OVID, and the Internet, specifically focusing on information contained in the CDC and FDA websites, as well as the Cochrane library. Search date: March 2014.
The views expressed in this article are those of the authors and do not necessarily reflect the official policy of the Department of Defense, the Department of the Army, or the U.S. Army Medical Department.
