
Am Fam Physician. 2015;92(8):694-699
Family physicians considering corticosteroid injections as part of a comprehensive treatment plan for musculoskeletal diagnoses will find few high-quality studies to assist with evidence-based decision making. Most studies of corticosteroid injections for the treatment of osteoarthritis, tendinopathy, bursitis, or neuropathy include only small numbers of patients and have inconsistent long-term follow-up. Corticosteroid injections for the treatment of adhesive capsulitis result in short-term improvements in pain and range of motion. For subacromial impingement syndrome, corticosteroid injections provide short-term pain relief and improvement in function. In medial and lateral epicondylitis, corticosteroid injections offer only short-term improvement of symptoms and have a high rate of symptom recurrence. Corticosteroid injections for carpal tunnel syndrome may help patients avoid or delay surgery. Trigger finger and de Quervain tenosynovitis may be treated effectively with corticosteroid injections. Patients with hip or knee osteoarthritis may have short-term symptom relief with corticosteroid injections.
Family physicians often treat patients with musculoskeletal conditions.1 In the United States, 8% of ambulatory visits are for musculoskeletal and soft tissue concerns, and more than 13% of these patients have arthritis as a comorbid chronic condition.2 Although many common musculoskeletal diagnoses can be successfully treated with conservative treatments such as rest, ice or heat, splinting, oral nonsteroidal anti-inflammatory drugs (NSAIDs), and physical therapy, almost two-thirds of family physicians use corticosteroid injections as part of a treatment plan.3 Treatment of musculoskeletal conditions by a primary care physician can improve patient satisfaction4 and help avoid costly referrals. Discussion of the diagnostic benefits, techniques, and adverse effects of corticosteroid injections is beyond the scope of this article; however, given the reported rarity of adverse effects, physicians should consider them relatively safe. This article summarizes the research on corticosteroid injections to provide family physicians with evidence-based recommendations for their use (Table 1).
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Corticosteroid injections in the shoulder have only short-term benefits in adhesive capsulitis and subacromial impingement syndrome. | B | 5, 7–9, 12, 14, 19 |
| Corticosteroid injections for lateral and medial epicondylitis lead to short-term improvement but have a high rate of recurrence and are no better than other options in the long term. | B | 21, 26–30 |
| Corticosteroid injections can be considered for patients with carpal tunnel syndrome who wish to avoid or delay surgical treatment. | B | 35, 36, 40 |
| Corticosteroid injections for de Quervain tenosynovitis and trigger finger are effective early in therapy. | B | 44, 46, 48, 50 |
| Corticosteroid injections provide short-term relief from symptoms of knee and hip osteoarthritis in patients who wish to delay surgery. | B | 57, 60–63 |
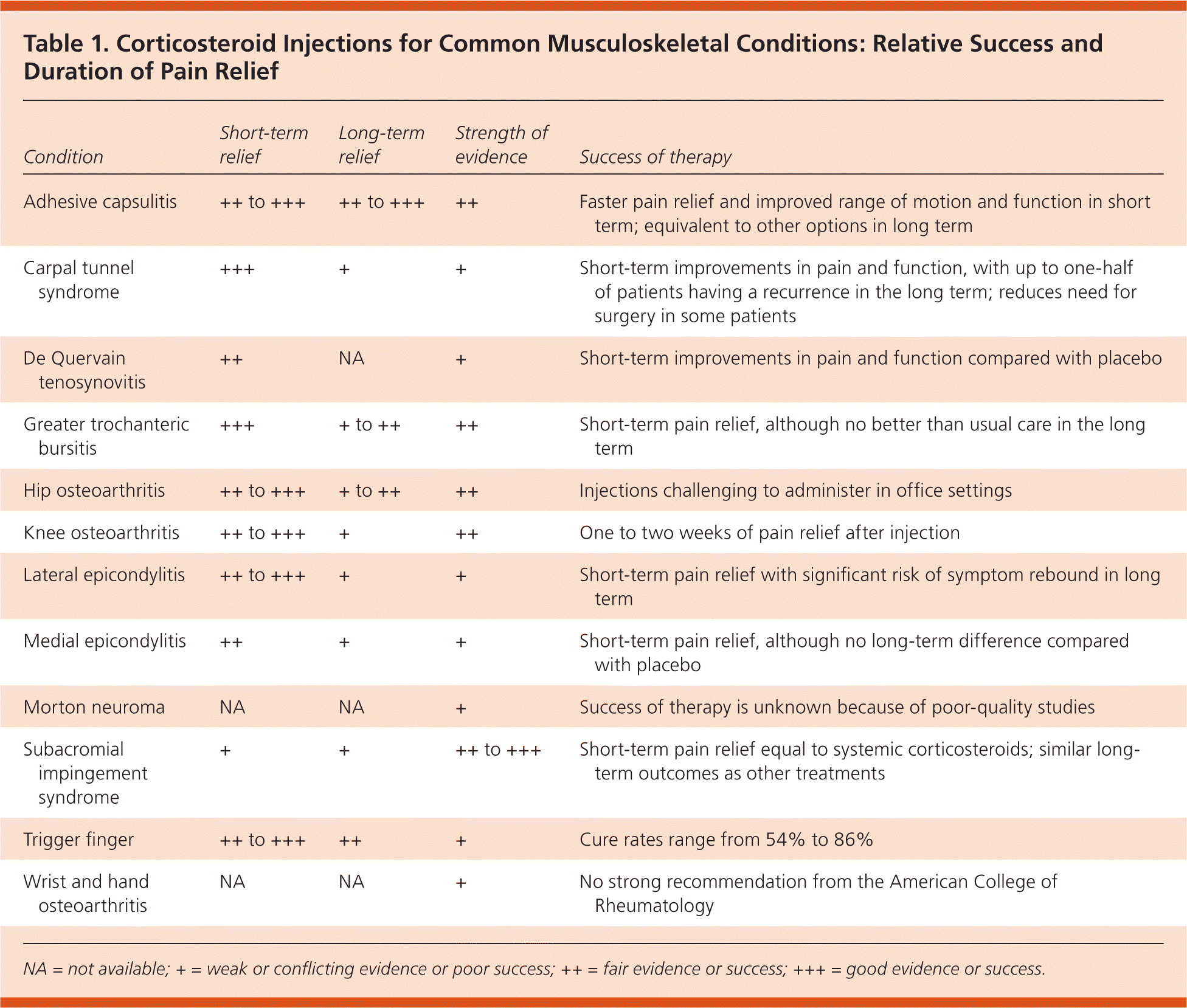
| Condition | Short-term relief | Long-term relief | Strength of evidence | Success of therapy |
|---|---|---|---|---|
| Adhesive capsulitis | ++ to +++ | ++ to +++ | ++ | Faster pain relief and improved range of motion and function in short term; equivalent to other options in long term |
| Carpal tunnel syndrome | +++ | + | + | Short-term improvements in pain and function, with up to one-half of patients having a recurrence in the long term; reduces need for surgery in some patients |
| De Quervain tenosynovitis | ++ | NA | + | Short-term improvements in pain and function compared with placebo |
| Greater trochanteric bursitis | +++ | + to ++ | ++ | Short-term pain relief, although no better than usual care in the long term |
| Hip osteoarthritis | ++ to +++ | + to ++ | ++ | Injections challenging to administer in office settings |
| Knee osteoarthritis | ++ to +++ | + | ++ | One to two weeks of pain relief after injection |
| Lateral epicondylitis | ++ to +++ | + | + | Short-term pain relief with significant risk of symptom rebound in long term |
| Medial epicondylitis | ++ | + | + | Short-term pain relief, although no long-term difference compared with placebo |
| Morton neuroma | NA | NA | + | Success of therapy is unknown because of poor-quality studies |
| Subacromial impingement syndrome | + | + | ++ to +++ | Short-term pain relief equal to systemic corticosteroids; similar long-term outcomes as other treatments |
| Trigger finger | ++ to +++ | ++ | + | Cure rates range from 54% to 86% |
| Wrist and hand osteoarthritis | NA | NA | + | No strong recommendation from the American College of Rheumatology |
Adhesive Capsulitis
Adhesive capsulitis describes a continuum of pain and stiffness in the shoulder, followed by contracture of the shoulder structures, then gradual recovery of range of motion.5–7 It is generally self-limiting, although some patients report persistent pain and limited range of motion after three years.5,7,8
Most interventions for adhesive capsulitis result in improvement. In the short term (eight to 16 weeks), intra-articular or subacromial corticosteroid injections outperform oral corticosteroids, NSAIDs, and physical therapy.5,8,9 However, the difference in outcomes between groups is not statistically significant after one year.5,8,9 Surgery (manipulation with arthroscopic arthrolysis) is superior in terms of range of motion and function by six weeks, although patients who receive intra-articular corticosteroid injections have similar gains by 12 weeks.7
Physicians should recommend conservative treatment initially, adding oral or injected corticosteroids if there is not adequate improvement in pain, range of motion, or function. Before referring a patient for manipulation under anesthesia, physicians should consider a subacromial corticosteroid injection, because it poses less risk.
Subacromial Impingement Syndrome
Subacromial impingement syndrome includes rotator cuff syndrome, tendinitis, and bursitis of the shoulder.10 It results from a combination of intrinsic and extrinsic factors that injure the bursa and rotator cuff tendons in the subacromial space.11 Subacromial impingement syndrome is the most common diagnosis in patients with shoulder pain.12,13
Corticosteroid injections provide a maximum of four weeks of pain relief.14 Intra-articular injections are no better than placebo, and subacromial injections provide only minimal pain relief.14 Ultrasound-guided injections have no benefit compared with landmark-guided injections.15 There is no difference in pain or disability at four weeks with systemic vs. subacromial injections.16
Corticosteroid injections for subacromial impingement syndrome have similar to worse outcomes compared with conservative treatments. A combination of physical therapy and corticosteroid injections provides better pain relief at six weeks compared with physical therapy alone, but by 12 and 24 weeks there is no difference between treatments.12 Subacromial injections of triamcinolone are inferior to ketorolac for short-term improvement in forward flexion strength and patient satisfaction.17 In an industry-sponsored study, application of a heated lidocaine/tetracaine patch (Synera) provided similar improvements in pain and range of motion as subacromial triamcinolone injections by six weeks.18 A Cochrane review found no difference in outcomes at four weeks between corticosteroid injections, ultrasonography, acupuncture, and oral NSAIDs.14
Physicians should recommend conservative therapies initially for treatment of subacromial impingement syndrome. The patient's preferences and duration of symptoms should also be considered, because corticosteroid injections are more effective for those with symptoms of less than 12 weeks' duration.19
Lateral Epicondylitis
In patients with symptoms of up to six weeks' duration, corticosteroid injection provides pain relief for four to six weeks.20–27 One trial showed corticosteroids to be superior to local anesthetic in terms of pain and disability at three weeks, but by 12 weeks the corticosteroid group had a 35% recurrence rate compared with no recurrences in the local anesthetic group.27
Long-term outcomes after corticosteroid injection indicate no benefit or symptom worsening.21,26 The recurrence rate one year after a single corticosteroid injection is more than 50%, compared with a 12% recurrence rate in patients receiving a placebo injection.23,26 Physical therapy also has poor long-term results, with a one-year recurrence rate of 8% to 29%.23,26 Treatment with a muscle energy technique improved pain-free grip strength and pain at 52 weeks compared with a single injection of corticosteroid.28
Corticosteroid injections can be part of a treatment plan for lateral epicondylitis, although patients should be warned that there is a high recurrence rate. Patients should be counseled that current evidence indicates that long-term outcomes are often the same, regardless of initial treatment.
Medial Epicondylitis
Medial epicondylitis (golfer's elbow) is pain over the medial epicondyle.29 Corticosteroid injection can provide short-term improvements in pain, although there is no long-term difference in outcomes between corticosteroid injections and placebo at six weeks and one year.29,30 Platelet-rich plasma injection provides greater improvements in pain and function at 52 weeks compared with corticosteroids, although it is unclear whether these outcomes are clinically meaningful to patients.31 Given the lack of evidence, physicians should look to studies of lateral epicondylitis for guidance.
Carpal Tunnel Syndrome
Carpal tunnel syndrome is caused by entrapment of the median nerve under the transverse carpal ligament at the wrist.32 Genetic predisposition and obesity are risk factors.33 Younger patients with shorter symptom duration are more likely to have spontaneous improvement compared with those who have bilateral symptoms and a positive Phalen test.34
Corticosteroid injections are beneficial in improving short-term outcomes.35–38 Triamcinolone injections result in improved symptom scores and functional status at one week compared with placebo injection.35 Methylprednisolone injection reduces symptom severity at 10 weeks compared with placebo.36 At two weeks, systemic corticosteroids and local injections provide similar improvements in symptoms; however, patients who receive injections have significantly better symptom scores by eight and 12 weeks.39 Local corticosteroid injection and oral NSAIDs with a neutral wrist splint result in similar short-term improvements in symptom severity.40 Two corticosteroid injections provide no additional improvement compared with only a single injection.41
Long-term outcomes are mixed in patients with carpal tunnel syndrome who are treated with corticosteroid injections; up to one-half have symptom recurrence.35 Ultrasonography may improve the duration of effect and other parameters, but at significant cost.42 The need for surgery at one year is reduced with corticosteroid injection, but a significant number of patients (75% in one study) eventually undergo surgical treatment.36
Physicians can tailor their treatment recommendations to the patient's preferences. Corticosteroid injection is an option as long as patients are aware that it may not prevent recurrence or the need for surgery.
De Quervain Tenosynovitis
De Quervain tenosynovitis is tendinosis of the abductor pollicis longus and extensor pollicis brevis in the first dorsal compartment of the wrist.43 Research on this condition is limited by small patient numbers, differences in the type of injectable corticosteroid used, and poor long-term follow-up.44
A 2009 Cochrane review supports the use of corticosteroid injections over splinting in patients with de Quervain tenosynovitis,44 although the study on which the recommendation is based included only pregnant and lactating women.45 A more recent study shows improvement in pain and function at one week after corticosteroid injection compared with placebo.46 Corticosteroid injection alone results in improved outcomes compared with a combination of injection and splinting, whereas treatment with rest alone or NSAIDs alone does not improve symptoms.43
Trigger Finger
Trigger finger is the triggering or locking of a finger caused by histologic changes in the A1 pulley that prevent smooth motion of the flexor digitorum profundus and superficialis tendons.47 Rheumatoid arthritis, diabetes mellitus, carpal tunnel syndrome, and de Quervain tenosynovitis are associated with trigger finger.48
Cure rates after corticosteroid injection are generally moderate, ranging from 54% to 86%.48,49 Compared with placebo injections, corticosteroids result in less triggering and improved pain at one week, and these effects persist through one year.50 In one study, corticosteroid injections resulted in less topical and joint pain at one week and one month compared with percutaneous and open releases; however, patients who underwent surgery had better outcomes at six months.48 Symptom relapse occurred in 12% of patients who received one injection, 18% of those who received a second injection, and none who underwent surgery.48 However, a Cochrane review notes that studies of corticosteroid injections for trigger finger are limited by sample size and short duration of follow-up.47
Physicians should offer a corticosteroid injection for patients with trigger finger who are seeking a nonsurgical treatment option.
Wrist and Hand Osteoarthritis
The American College of Rheumatology makes “no strong recommendation” for intra-articular corticosteroid injection in patients with hand osteoarthritis.51 A Cochrane review of intra-articular corticosteroid injections for wrist or hand rheumatoid arthritis found only one study with moderate bias that recommended against splinting or resting the wrist after intra-articular corticosteroid injection.52 Physicians are best advised to refer patients who desire such an intervention to a subspecialist.
Greater Trochanteric Bursitis
Greater trochanteric bursitis is in the differential diagnosis for pain in the lateral hip. This condition has recently been referred to as greater trochanteric pain syndrome, reflecting the results of radiologic and histopathologic studies that indicate no inflammation of the subgluteus maximus bursa.53
Compared with usual care (analgesics and physical therapy), corticosteroid injections provide greater pain relief at rest and with activity at six weeks and three months, but no differences in pain or function at six months and one year.54 Physicians may consider corticosteroid injections for patients with greater trochanteric pain who desire more prompt resolution of their symptoms.
Hip Osteoarthritis
Hip osteoarthritis affects more than one-third of patients older than 85 years.55 Treatment with intra-articular corticosteroid injections in the outpatient setting is challenging given the need for radiographic guidance.56 A small double-blind study comparing corticosteroid and placebo injections using an ultrasound-guided anterolateral approach showed improvement in pain on walking at two and four weeks for the corticosteroid group, although that improvement disappeared by three months.57 Fluoroscopically guided corticosteroid injections provide improvement in pain, stiffness, and physical function at two months compared with placebo injections.55 Most primary care physicians should consider orthopedic referral for patients who desire injection treatment for hip osteoarthritis.
Knee Osteoarthritis
Guidelines from the American College of Rheumatology conditionally recommend the use of intra-articular corticosteroid injections for treatment of knee osteoarthritis.51 The duration of pain relief is one to two weeks in most trials, with a few showing improvements lasting three to four weeks.60–63 Research uniformly supports the safety of intra-articular corticosteroid injections for treatment of knee osteoarthritis; however, these studies are limited by lack of histologic data and poor long-term follow-up.64 A Cochrane review found weak evidence for the use of corticosteroid injections for the treatment of knee rheumatoid arthritis.52
Physicians may consider intra-articular corticosteroid injections before orthopedic referral for surgical evaluation in patients with knee osteoarthritis.
Morton Neuroma
Morton neuroma refers to pain between the metatarsal heads from the plantar digital nerve, most commonly affecting the third web space.65
A Cochrane review notes that although corticosteroid injection is considered a standard treatment for Morton neuroma, few studies have investigated its safety and effectiveness, and those that are published are of poor quality.65 Physicians may consider corticosteroid injection for these patients, but should be advised there is no good-quality evidence to support it.
The authors thank Jillah Biza, Riecker Memorial Library at St. Joseph Mercy Hospital, Ann Arbor, Mich., for her assistance with literature searches and obtaining articles.
Data Sources: PubMed, SPORTDiscus (EBSCO), Cochrane, and the AHRQ databases were searched for studies published within the past 10 years. Additional searches were performed using Essential Evidence Plus. Key words were corticosteroid injections and lateral epicondylitis/tennis elbow, carpal tunnel syndrome/median neuropathy, deQuervain's tenosy-novitis/thumb tendinitis, rotator cuff tendinitis/shoulder bursitis/shoulder pain, greater trochanteric bursitis/lateral hip pain, and knee pain/knee osteoarthritis. Search dates: March 2014 through June 2015.
