
Am Fam Physician. 2016;93(3):223-224
Author disclosure: No relevant financial affiliations.
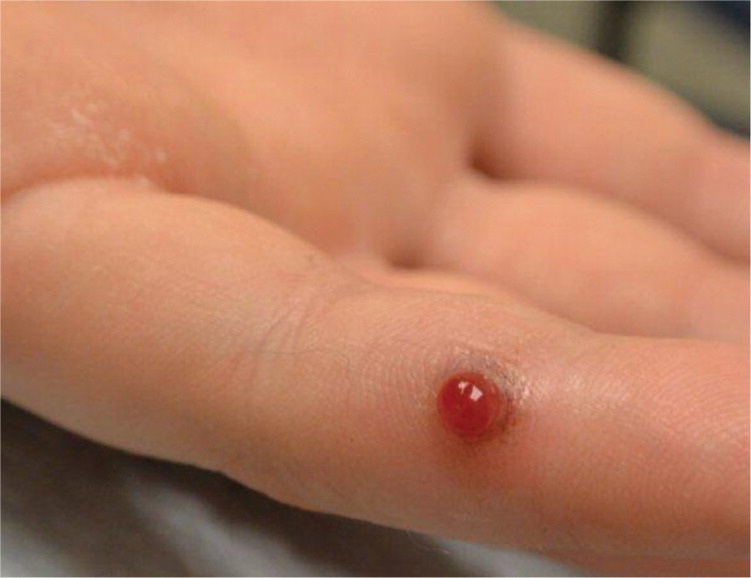
A 14-year-old boy presented with a tender red papule on his finger. He first noticed it two months earlier. It bled several times, especially when rubbed by his baseball mitt. He had no medical problems or allergies, and he was not taking any medications. He had no other similar skin lesions, and the review of systems was negative for bleeding problems, easy bruising, and frequent infections.
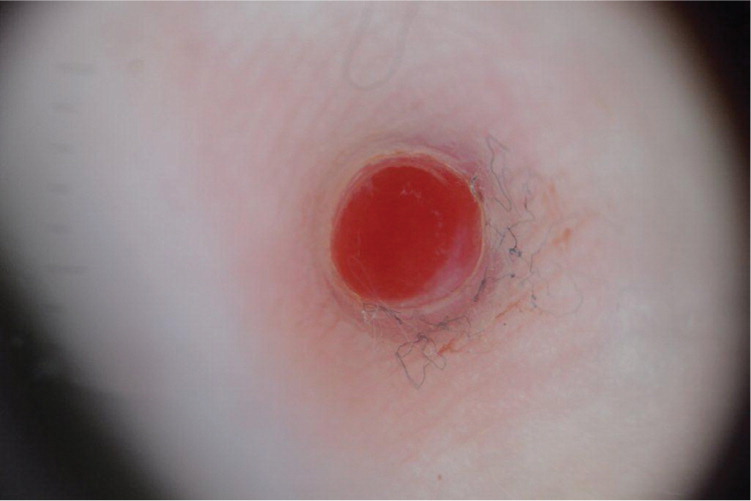
Physical examination revealed a solitary bright-red papule on the distal lateral portion of his left fifth finger (Figure 1). On dermoscopy, the lesion was homogeneously red and surrounded by a white collarette of scale (Figure 2). There was no evidence of a pigment network, pigment globules, or dotted vessels.
Question
Discussion
The answer is C: pyogenic granuloma. Pyogenic granulomas are more accurately described as lobular capillary hemangiomas because the lesions are not purulent or granulomatous. They are benign vascular tumors that typically evolve over weeks to months, rarely growing larger than 1 cm. They can occur at any age but are most common in children and young adults. Most are solitary, and they are often attributed to trauma. They are also associated with several medications, including isotretinoin, capecitabine (Xeloda), and indinavir (Crixivan).1 On dermoscopy, 92% of pyogenic granulomas have a homogeneous reddish area and 85% have a white collarette2; the combination of these two findings was found to be 100% specific for pyogenic granulomas.3
Treatment of a pyogenic granuloma is typically surgical, although spontaneous resolution has been reported.4 Shave removal is often sufficient because they are small and superficial. For smaller lesions, silver nitrate alone may be applied instead of shave removal. For larger lesions, silver nitrate may be applied after excision or curettage may be performed to remove remaining tissue. Some pyogenic granulomas have features similar to malignant lesions. In these lesions, a biopsy with histopathologic analysis should be performed. Recurrence is common, especially if the removal is too superficial and a portion of the lesion persists after the excision.
Amelanotic melanomas present as pink or skin-colored plaques, typically on sun-exposed sites. They lack the classic dark or multicolored presentation of typical melanomas. On dermoscopy, amelanotic melanomas may have milky red globules, polymorphous vessels, or dotted vessels similar to those of Spitz nevi.5 Diagnosis requires histologic analysis.
Hemangiomas are benign vascular proliferations. Most hemangiomas appear within the first few months of life and involute spontaneously. On dermoscopy, hemangiomas have red lacunae (or lagoons) of dilated blood vessels separated by white septa.6
Spitz nevi are brown, pink, or red dome-shaped papules composed of melanocytes. Spitz nevi are more common in children, whereas malignant spitzoid melanoma is more common in adults. On dermoscopy, up to 78% of Spitz nevi have dotted vessels.5 A starburst pattern, where melanocytes radiate out symmetrically from the edge of the lesion, is also seen with Spitz nevi.7 Because of the clinical similarities between Spitz nevi and spitzoid melanoma, lesions with dotted vessels or a starburst pattern on dermoscopy are typically biopsied.
Warts (verrucas) are caused by a common viral infection and often affect the hands and feet. Warts may be solitary or multiple. They are usually firm, hyperkeratotic papules with scale, and they occasionally bleed. On dermoscopy, homogeneous black to red dots (thrombosed capillaries) and globules are seen in 79% of warts.8
