
A more recent article on acute and chronic prostatitis is available.
Am Fam Physician. 2016;93(4):290-296
Related letter: Exercise Is Effective Therapy for Chronic Nonbacterial Prostatitis and Chronic Pelvic Pain Syndrome
Author disclosure: No relevant financial affiliations.
Chronic prostatitis is relatively common, with a lifetime prevalence of 1.8% to 8.2%. Risk factors include conditions that facilitate introduction of bacteria into the urethra and prostate (which also predispose the patient to urinary tract infections) and conditions that can lead to chronic neuropathic pain. Chronic prostatitis must be differentiated from other causes of chronic pelvic pain, such as interstitial cystitis/bladder pain syndrome and pelvic floor dysfunction; prostate and bladder cancers; benign prostatic hyperplasia; urolithiasis; and other causes of dysuria, urinary frequency, and nocturia. The National Institutes of Health divides prostatitis into four syndromes: acute bacterial prostatitis, chronic bacterial prostatitis (CBP), chronic nonbacterial prostatitis (CNP)/chronic pelvic pain syndrome (CPPS), and asymptomatic inflammatory prostatitis. CBP and CNP/CPPS both lead to pelvic pain and lower urinary tract symptoms. CBP presents as recurrent urinary tract infections with the same organism identified on repeated cultures; it responds to a prolonged course of an antibiotic that adequately penetrates the prostate, if the urine culture suggests sensitivity. If four to six weeks of antibiotic therapy is effective but symptoms recur, another course may be prescribed, perhaps in combination with alpha blockers or nonopioid analgesics. CNP/CPPS, accounting for more than 90% of chronic prostatitis cases, presents as prostatic pain lasting at least three months without consistent culture results. Weak evidence supports the use of alpha blockers, pain medications, and a four- to six-week course of antibiotics for the treatment of CNP/CPPS. Patients may also be referred to a psychologist experienced in managing chronic pain. Experts on this condition recommend a combination of treatments tailored to the patient's phenotypic presentation. Urology referral should be considered when appropriate treatment is ineffective. Additional treatments include pelvic floor physical therapy, phytotherapy, and pain management techniques. The UPOINT (urinary, psychosocial, organ-specific, infection, neurologic/systemic, tenderness) approach summarizes the various factors that may contribute to presentation and can guide treatment.
What Is Chronic Prostatitis?
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Chronic prostatitis should be considered in men with persistent pain associated with urination or ejaculation, or lower urinary tract symptoms related to voiding or storage. | C | 3 |
| CBP is recognized by multiple urine cultures positive for the same organism. These cultures can be from post-prostatic massage urine, midstream clean-catch urine, or prostate secretions. | C | 5 |
| CNP/CPPS presents similarly to CBP, but it is much more common and urine culture results are negative or inconsistent. | C | 3, 5 |
| CBP should be treated with a 4- to 6-week course of a fluoroquinolone antibiotic (preferably levofloxacin [Levaquin], but a macrolide can be used if chlamydia is suspected), and pain medication. If the patient responds, but then relapses, a second 4- to 6-week course of an antibiotic plus an alpha blocker should be considered. | B | 3, 11, 14 |
| CNP/CPPS should be treated for 4 to 6 weeks, preferably with an alpha blocker, antibiotic, and pain medication. | C | 21 |
| If CBP or CNP/CPPS does not improve significantly with initial treatment, the patient should be referred to a urologist. | C | 3 |
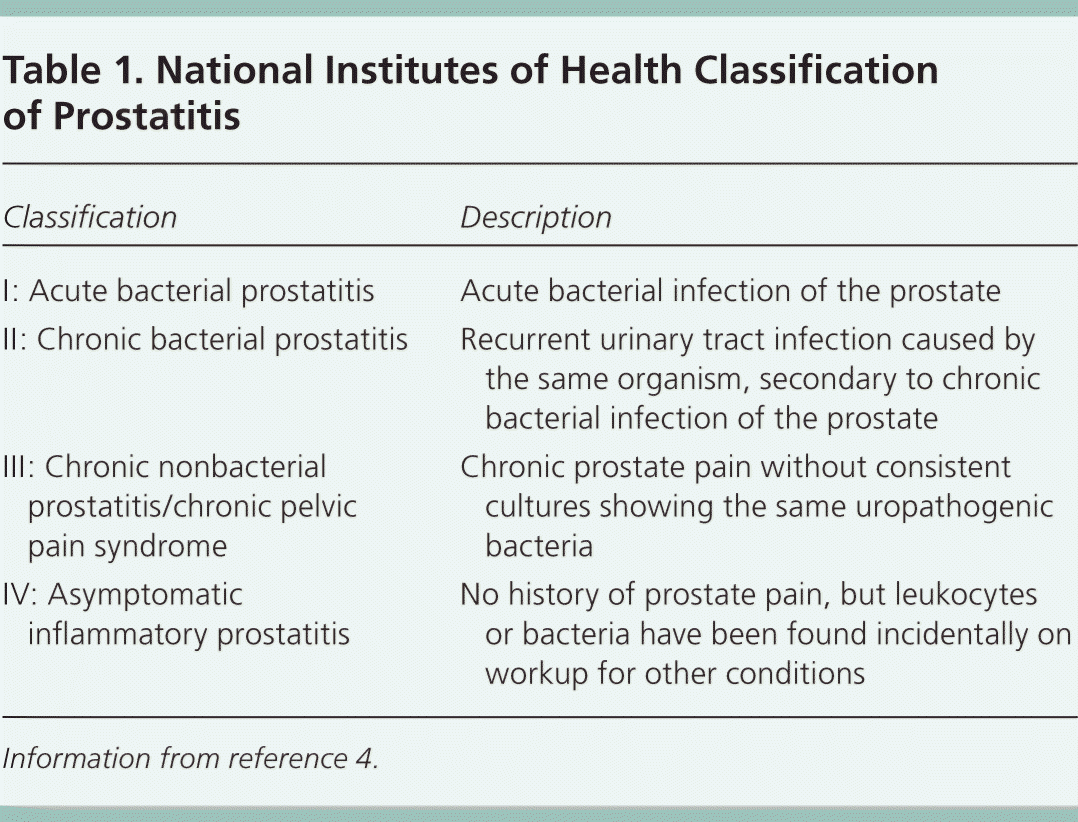
| Classification | Description |
|---|---|
| I: Acute bacterial prostatitis | Acute bacterial infection of the prostate |
| II: Chronic bacterial prostatitis | Recurrent urinary tract infection caused by the same organism, secondary to chronic bacterial infection of the prostate |
| III: Chronic nonbacterial prostatitis/chronic pelvic pain syndrome | Chronic prostate pain without consistent cultures showing the same uropathogenic bacteria |
| IV: Asymptomatic inflammatory prostatitis | No history of prostate pain, but leukocytes or bacteria have been found incidentally on workup for other conditions |
EVIDENCE SUMMARY
CBP lasts three months or longer and consistently grows the same bacterial strain on repeated cultures (using post-prostate massage urine; midstream clean-catch urine; or prostate secretions, such as expressed secretion).5 Gram-negative Escherichia coli is the most common organism followed by gram-positive Enterococcus.6 CNP/CPPS is much more common than CBP, comprising more than 90% of chronic prostatitis cases.5,7 It is defined as pelvic pain lasting three or more months without consistently positive bacterial cultures.
What Are the Known Risk Factors for Chronic Prostatitis?
Conditions that allow retrograde movement of bacteria into the urethra and the prostate are risk factors for CBP. Patients with a history of urethritis caused by sexually transmitted infections (STIs) are thought to be at risk of subsequent CBP. Risk factors for CNP/CPPS are largely unknown but may include conditions that can lead to chronic neuropathic pain.
EVIDENCE SUMMARY
CBP is thought to be caused by infection moving from the distal urethra to the prostate. Facilitating factors are the presence of foreskin, urethral stricture, benign prostatic hyperplasia, history of STI, recent instrumentation or catheterization, and retrograde ejaculation.6
The specific pathophysiology of CNP/CPPS is poorly understood. Recent research suggests that some insult to the prostate may trigger central pain sensitization leading to persistent neuropathic pain, which is similar to other chronic pain conditions such as fibromyalgia, irritable bowel syndrome, and endometriosis.8
Which Conditions Should Be Distinguished from Chronic Prostatitis?
Several disorders of the pelvic region can lead to symptoms similar to those of chronic prostatitis (Table 2). In particular, the symptoms of interstitial cystitis/bladder pain syndrome largely overlap with those of chronic prostatitis.

| Gastrointestinal: Irritable bowel syndrome, colon cancer |
| Genitourinary: Interstitial cystitis/bladder pain syndrome, benign prostatic hyperplasia, bladder/prostate cancer, calculi, sexually transmitted infections, foreign body, prostatic abscess |
| Musculoskeletal: Pelvic floor dysfunction, pelvic injury or trauma |
| Neurologic: Neurogenic bladder, pudendal neuralgia |
EVIDENCE SUMMARY
Conditions with symptoms similar to those of chronic prostatitis include acute infections, such as acute bacterial prostatitis, prostatic abscess, and STIs; and obstructive pathologies, such as benign prostatic hyperplasia, bladder cancer, calculi, and foreign body.6 Because CBP and CNP/CPPS have similar presentations, the same differential diagnosis should be considered.
Urine cytologies and/or cystoscopy to exclude bladder cancer should be performed in patients with hematuria and risk factors for bladder cancer (e.g., smoking, age older than 40 years). Bladder cancer is diagnosed in about 1% of patients referred for persistent chronic prostatitis.9
What Are the Symptoms of Chronic Prostatitis, and How Is It Evaluated?
Chronic prostatitis presents as urogenital pain, lower urinary tract symptoms, psychological symptoms, and/or sexual dysfunction.3 The initial evaluation can easily be performed in a primary care office and includes history, physical examination, and basic laboratory tests. Several validated questionnaires record baseline symptoms and their impact on quality of life, as well as monitor disease progression and success of treatment. The UPOINT (urinary, psychosocial, organ-specific, infection, neurologic/systemic, tenderness) approach summarizes the various factors that can contribute to chronic prostatitis presentation and can guide treatment.
EVIDENCE SUMMARY
Pain occurs with CBP and CNP/CPPS. The pain may present in the lower back, hypogastrium, pelvis, or genitalia. The patient may also report pain with urination or ejaculation, and lower urinary tract symptoms related to voiding (weak stream, straining, and hesitancy) or storage problems (urgency, frequency, and dysuria). Other symptoms may include sexual dysfunction and psychosocial symptoms, such as anxiety, stress, and depression.3
The initial physical examination should assess the abdomen, costovertebral angle, suprapubic area, and external genitalia, and should include a digital rectal examination. The physical examination can identify other causes of pelvic pain, such as epididymitis, genital herpes, and urolithiasis with radiation of pain into the groin. Urine should be obtained, before and after the prostatic massage, for urinalysis and culture.
The laboratory evaluation begins with urinalysis, urine culture, and screening for STIs. Prostate-specific antigen (PSA) testing should be performed in patients with prostate cancer risk factors (e.g., positive family history), abnormal digital rectal examination findings, or symptoms of obstruction. PSA testing is delayed if the patient has had a recent digital rectal examination, physical activity, or sexual activity, or has a current prostate infection; these factors can elevate the PSA level.3 Pre- and post-prostatic massage cultures that match a previously documented infection are the best way to diagnosis CBP, with a sensitivity of 44% and specificity of 100%.5 When sending the pre- and post-massage urine for culture, “report all growth” should be written on the laboratory requisition.
False-positive cultures (patients with CNP/CPPS who have a positive post-massage urine culture result) and false-negative cultures (patients with CBP who have an initial negative post-massage culture result) are possible. If the patient has previous urine cultures that were positive for the same organism as the current positive post-massage urine culture, this may suggest CBP. Cultures that are inconsistent, showing different organisms when positive, may support a diagnosis of CNP/CPPS.10 If prior records are not available, repeat digital rectal examinations and post-massage urine cultures may be necessary to clarify the diagnosis.
The NIH Chronic Prostatitis Symptom Index (http://www.prostatitis.org/symptomindex.html) is a validated tool for assessing pain, voiding symptoms, and impact on quality of life. It can also be used to track effectiveness of treatment; a decrease of at least 6 points indicates a response to treatment.6 The International Prostate Symptom Score (http://www.baus.org.uk/_userfiles/pages/files/Patients/Leaflets/IPSS.pdf) assesses urinary symptoms and impact on quality of life for all prostate diseases. It rates irritative and storage symptoms on a scale from 0 to 5, in addition to a quality-of-life question. The recently developed UPOINT approach to the evaluation highlights various symptom phenotypes and helps direct multimodal therapy.3
Which Antibiotics Are Effective for CBP, and What Other Therapies Are Beneficial?
Fluoroquinolones are the preferred first-line agents, with levofloxacin (Levaquin) showing advantages over ciprofloxacin. Azithromycin (Zithromax) may have a higher cure rate when treating Chlamydia trachomatis. Bacterial strains that are multidrug resistant or that form moderate to strong biofilms are particularly challenging to treat. Other therapies, such as uroselective alpha blockers, can be used with antibiotics in patients with lower urinary tract symptoms. Acetaminophen is generally a good first-line treatment for pain in early disease. Table 3summarizes treatment options.3
EVIDENCE SUMMARY
Treatment is based on bacterial sensitivities and takes into account the ability of the antibiotic to penetrate the prostate. Fluoroquinolones are the consensus choice for first-line treatment.3 In a comparison of oral levofloxacin, 500 mg daily, and ciprofloxacin, 500 mg twice daily, given for four weeks, levofloxacin was superior in clinical effectiveness (93.3% vs. 71.9%) and had lower recurrence rates over six months (4% vs. 19.2%).11 In another study (without subsequent follow-up) of a 28-day course of levofloxacin, 500 mg daily, the medication was well-tolerated, with a treatment adherence rate of 98.6%, a cure rate of 58.9%, and a significant decrease in patient-reported symptoms.12 The Prostatitis Expert Reference Group recommends four to six weeks of treatment.3
In a case study, an extended spectrum beta-lactamase E. coli prostatitis was successfully treated with the combination of fosfomycin (Monurol) and doxycycline.15 Bacterial strains producing moderate to strong biofilms, including E. coli, gram-negative bacteria, Staphylococci, and Enterococci,16 can be particularly difficult to treat and correlate with higher NIH Chronic Prostatitis Symptom Index scores and decreased clinical response.17 Usually, CBP responds to a four- to six-week trial of a long-acting fluoroquinolone. If symptoms recur or do not clear with the antibiotic alone, a second course of antibiotics can be combined with a uroselective alpha blocker (e.g., tamsulosin [Flomax], alfuzosin [Uroxatral], silodosin [Rapaflo]), especially in patients with significant voiding lower urinary tract symptoms or high post-void residuals.3
Research on pain management strategies for CBP is limited, but acetaminophen is first-line therapy for recent onset of pain (less than six months). Evidence suggests that nonsteroidal anti-inflammatory drugs (NSAIDs) are ineffective. If NSAIDs are used, only a four- to six-week trial should be given, and to avoid adverse effects, the therapy should be stopped if there is no response.3
There is overlap in treatment effectiveness between CBP and CNP/CPPS. For either condition, the National Institute for Health and Care Excellence guidelines recommend medications for neuropathic pain, such as gabapentin (Neurontin) or pregabalin (Lyrica), tricyclic antidepressants, and serotonin-norepinephrine reuptake inhibitors, if first-line treatments fail.18 Opioid medications are not recommended because there is no evidence that they are effective and there is potential for dependency.3
What Are First-Line Treatments for CNP/CPPS?
For newer-onset CNP/CPPS (three to six months' duration), first-line therapies are acetaminophen, uroselective alpha blockers, and possibly a four- to six-week trial of an antibiotic. For CNP/CPPS lasting more than six months, options include uroselective alpha blockers and a four- to six-week trial of an antibiotic, with a four- to six-week trial of an NSAID if inflammatory disease is suspected. Screening for trauma, prior abuse, and psychosocial factors is also reasonable, regardless of symptom duration. Table 3 summarizes treatment options.3
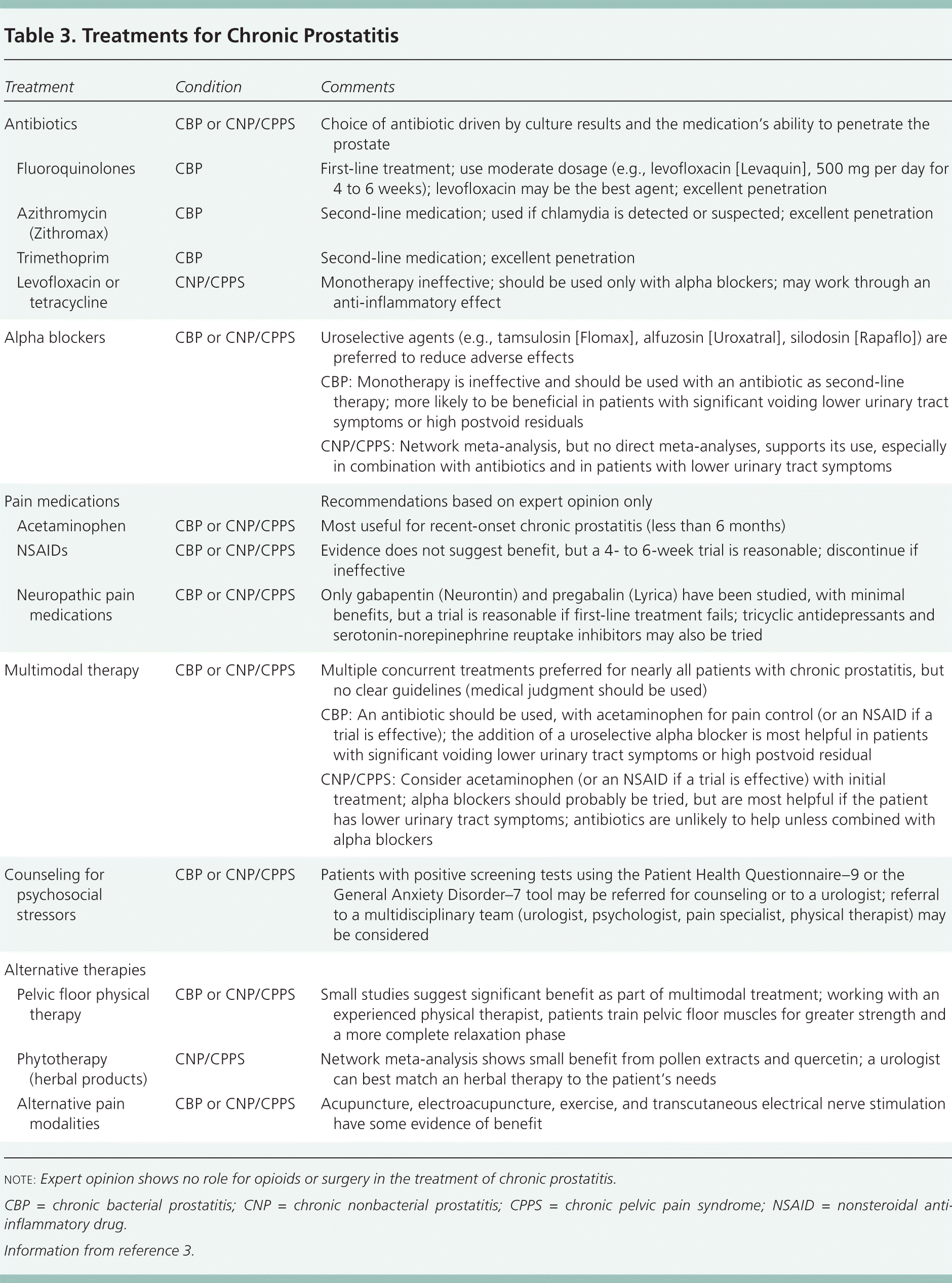
| Treatment | Condition | Comments | |
|---|---|---|---|
| Antibiotics | CBP or CNP/CPPS | Choice of antibiotic driven by culture results and the medication's ability to penetrate the prostate | |
| Fluoroquinolones | CBP | First-line treatment; use moderate dosage (e.g., levofloxacin [Levaquin], 500 mg per day for 4 to 6 weeks); levofloxacin may be the best agent; excellent penetration | |
| Azithromycin (Zithromax) | CBP | Second-line medication; used if chlamydia is detected or suspected; excellent penetration | |
| Trimethoprim | CBP | Second-line medication; excellent penetration | |
| Levofloxacin or tetracycline | CNP/CPPS | Monotherapy ineffective; should be used only with alpha blockers; may work through an anti-inflammatory effect | |
| Alpha blockers | CBP or CNP/CPPS | Uroselective agents (e.g., tamsulosin [Flomax], alfuzosin [Uroxatral], silodosin [Rapaflo]) are preferred to reduce adverse effects | |
| CBP: Monotherapy is ineffective and should be used with an antibiotic as second-line therapy; more likely to be beneficial in patients with significant voiding lower urinary tract symptoms or high postvoid residuals | |||
| CNP/CPPS: Network meta-analysis, but no direct meta-analyses, supports its use, especially in combination with antibiotics and in patients with lower urinary tract symptoms | |||
| Pain medications | Recommendations based on expert opinion only | ||
| Acetaminophen | CBP or CNP/CPPS | Most useful for recent-onset chronic prostatitis (less than 6 months) | |
| NSAIDs | CBP or CNP/CPPS | Evidence does not suggest benefit, but a 4- to 6-week trial is reasonable; discontinue if ineffective | |
| Neuropathic pain medications | CBP or CNP/CPPS | Only gabapentin (Neurontin) and pregabalin (Lyrica) have been studied, with minimal benefits, but a trial is reasonable if first-line treatment fails; tricyclic antidepressants and serotonin-norepinephrine reuptake inhibitors may also be tried | |
| Multimodal therapy | CBP or CNP/CPPS | Multiple concurrent treatments preferred for nearly all patients with chronic prostatitis, but no clear guidelines (medical judgment should be used) | |
| CBP: An antibiotic should be used, with acetaminophen for pain control (or an NSAID if a trial is effective); the addition of a uroselective alpha blocker is most helpful in patients with significant voiding lower urinary tract symptoms or high postvoid residual | |||
| CNP/CPPS: Consider acetaminophen (or an NSAID if a trial is effective) with initial treatment; alpha blockers should probably be tried, but are most helpful if the patient has lower urinary tract symptoms; antibiotics are unlikely to help unless combined with alpha blockers | |||
| Counseling for psychosocial stressors | CBP or CNP/CPPS | Patients with positive screening tests using the Patient Health Questionnaire–9 or the General Anxiety Disorder–7 tool may be referred for counseling or to a urologist; referral to a multidisciplinary team (urologist, psychologist, pain specialist, physical therapist) may be considered | |
| Alternative therapies | |||
| Pelvic floor physical therapy | CBP or CNP/CPPS | Small studies suggest significant benefit as part of multimodal treatment; working with an experienced physical therapist, patients train pelvic floor muscles for greater strength and a more complete relaxation phase | |
| Phytotherapy (herbal products) | CNP/CPPS | Network meta-analysis shows small benefit from pollen extracts and quercetin; a urologist can best match an herbal therapy to the patient's needs | |
| Alternative pain modalities | CBP or CNP/CPPS | Acupuncture, electroacupuncture, exercise, and transcutaneous electrical nerve stimulation have some evidence of benefit | |
EVIDENCE SUMMARY
The evidence for CNP/CPPS treatment is poor, with small studies showing small effects, suggesting any benefit may be a placebo effect.19,20 Direct meta-analyses have not shown benefit from any single treatment, and only a statistical method (network meta-analysis) has found significant benefit from alpha blockers and antibiotics. 5-alpha-reductase inhibitors showed a statistically significant, but probably not clinically significant, benefit. Combining alpha blockers and antibiotics had the largest benefit.21
As with CBP, alpha blockers are most likely to be beneficial in patients with CNP/CPPS and lower urinary tract symptoms. Using uroselective agents reduces adverse effects. Combining the alpha blocker with an antibiotic, typically a fluoroquinolone, for four to six weeks, is an appropriate first-line treatment. Levofloxacin and tetracycline are most commonly used in CNP. Acetaminophen may also be used for new-onset CNP/CPPS. As in CBP, NSAIDs are unlikely to be effective, and opiates are not recommended.
Patients may also be screened for trauma, prior abuse, and psychosocial contributors (e.g., depression, anxiety) with the Patient Health Questionnaire–9 or Generalized Anxiety Disorder–7 instrument. A positive screening result prompts referral to a psychologist experienced in treating chronic pain, who provides counseling concurrently with medication therapy.3
Are Alternative Treatments Beneficial as Second-Line Therapy for Chronic Prostatitis?
Beyond first-line treatments, phytotherapy/herbal products (for CNP), multiple alternative modalities for pain management, and medication for neuropathic pain may be beneficial. Alternative therapies are usually provided after referral to a urologist.
EVIDENCE SUMMARY
The evidence for some herbal therapies and for pelvic floor physical therapy is similar in strength to the evidence for alpha blockers and antibiotics.3 Pelvic floor physical therapy should be used only after any concurrent infection, cancer, or prostatic hypertrophy are treated. A pain management approach is advised when usual treatments fail. Weak evidence supports the use of neuropathic pain medications and acupuncture.3 The UPOINT approach to symptom evaluation can direct which treatments to use (e.g., in a patient with minimal neurologic and psychosocial symptoms, a trial of phytotherapy and pelvic floor physical therapy may be appropriate).
When Should the Family Physician Refer Patients with Chronic Prostatitis to a Urologist?
Indications for referral include hematuria, severe dysuria, positive results on pre-massage urine culture, presence of a prostate nodule, an elevated PSA level, and failure of medical therapy.3
EVIDENCE SUMMARY
The Prostatitis Expert Reference Group recommends referral for possibly serious conditions. Hematuria, prostate nodules, or elevated PSA levels suggest cancer; severe dysuria suggests another diagnosis; and a positive result on pre-massage culture suggests an anatomic pathology. These patients should be referred to a urologist for further diagnosis and treatment.3
Failure of medical therapy is described as persistent symptoms after two four- to six-week courses of antibiotics, with or without an alpha blocker, in patients with CBP, and persistent symptoms after one four- to six-week course of an alpha blocker combined with an antibiotic in patients with CNP/CPPS.
Recent European guidelines suggest referral to a multidisciplinary team (urologist, psychologist, pain specialist, physical therapist), although there are no published studies to support this approach.3 Also, few centers offer this multidisciplinary approach. From a practical perspective, referral to a urologist experienced in treating chronic prostatitis would be appropriate.
Data Sources: A PubMed search was completed in Clinical Queries using the key term chronic prostatitis. The search included English-language clinical trials, randomized controlled trials, meta-analyses, systematic reviews, and reviews, using the categories of etiology, diagnosis, prognosis, therapy, risk factors, and clinical prediction guides. Also searched were Essential Evidence Plus, the Cochrane Library, and DynaMed. Search dates: September 17, 2014, and November 3, 2015.
